Immunomodulation by dietary long chain omega-3 fatty acids and the potential for adverse health outcomes - PubMed (original) (raw)
Review
Immunomodulation by dietary long chain omega-3 fatty acids and the potential for adverse health outcomes
Jenifer I Fenton et al. Prostaglandins Leukot Essent Fatty Acids. 2013 Nov-Dec.
Abstract
Recommendations to consume fish for prevention of cardiovascular disease (CVD), along with the U.S. Food and Drug Administration-approved generally recognized as safe (GRAS) status for long chain omega-3 fatty acids, may have had the unanticipated consequence of encouraging long-chain omega-3 (ω-3) fatty acid [(eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA)] supplementation and fortification practices. While there is evidence supporting a protective role for EPA/DHA supplementation in reducing sudden cardiac events, the safety and efficacy of supplementation with LCω-3PUFA in the context of other disease outcomes is unclear. Recent studies of bacterial, viral, and fungal infections in animal models of infectious disease demonstrate that LCω-3PUFA intake dampens immunity and alters pathogen clearance and can result in reduced survival. The same physiological properties of EPA/DHA that are responsible for the amelioration of inflammation associated with chronic cardiovascular pathology or autoimmune states, may impair pathogen clearance during acute infections by decreasing host resistance or interfere with tumor surveillance resulting in adverse health outcomes. Recent observations that high serum LCω-3PUFA levels are associated with higher risk of prostate cancer and atrial fibrillation raise concern for adverse outcomes. Given the widespread use of supplements and fortification of common food items with LCω-3PUFA, this review focuses on the immunomodulatory effects of the dietary LCω-3PUFAs, EPA and DHA, the mechanistic basis for potential negative health outcomes, and calls for biomarker development and validation as rational first steps towards setting recommended dietary intake levels.
Keywords: B cell; CHD; Cancer; Colitis; Coronary heart disease; Fish oil; Immune function; RA; Rheumatoid arthritis; TLR; Toll-like receptor.
© 2013 Published by Elsevier Ltd.
Figures
Figure 1
The model shows a proposed mechanism by which DHA acyl chains disrupt the physical clustering of lipid rafts and associated proteins. Upon LCω-3PUFA incorporation into the membrane, and possibly through changes in lipid raft organization the following could result. LCω-3PUFAs disrupt the molecular organization of the plasma membrane, which initiates changes downstream on generation of bioactive lipids, cell signaling, and gene expression. A disruption in raft domains with n-3 PUFAs will have downstream effects on immune cell function. To date, the function of several immune cells (i.e. CD4+ T, B, dendritic cells, macrophages) in addition to other cells are disrupted by incorporation of LCω-3PUFAs into the plasma membrane. Suppression of function would have utility for treatment of symptoms associated with chronic inflammation. However, a suppression of immune cell function, perhaps at high doses of LCω-3PUFAs, could have negative side effects on susceptibility to infection and targeting of cancer cells by specific immune cells. LCω-3PUFA feeding may also influence microbial community structure and risk of inflammation. It is not known whether dietary fatty acids affect microbial cell wall structure directly, whether these changes influence eukaryotic-prokaryotic signaling or whether fatty acid-induced changes in the overall balance of microbial populations contribute to increased risk of inflammation.
Figure 2
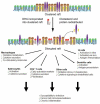
Observations associated with very low and high dietary intake of the LCω-3PUFA fatty acids, EPA and DHA. Deficiency of LCω-3PUFA intakes are associated with negative neurological, cardiovascular and reproductive outcomes. Excess LCω-3PUFA intakes are associated with an immune anergic phenotype in antigen-driven models of pathologies. Cell membrane phospholipid content has been proposed as a potential biomarker of dietary fatty acid intake and associated phenotypes. These require validation in support of the calls for Dietary Reference Intakes for these proposed nutrients.
Similar articles
- Omega-3 Fatty Acid Formulations in Cardiovascular Disease: Dietary Supplements are Not Substitutes for Prescription Products.
Fialkow J. Fialkow J. Am J Cardiovasc Drugs. 2016 Aug;16(4):229-239. doi: 10.1007/s40256-016-0170-7. Am J Cardiovasc Drugs. 2016. PMID: 27138439 Free PMC article. Review. - Pros and Cons of Long-Chain Omega-3 Polyunsaturated Fatty Acids in Cardiovascular Health.
Djuricic I, Calder PC. Djuricic I, et al. Annu Rev Pharmacol Toxicol. 2023 Jan 20;63:383-406. doi: 10.1146/annurev-pharmtox-051921-090208. Annu Rev Pharmacol Toxicol. 2023. PMID: 36662586 Review. - Risk stratification by the "EPA+DHA level" and the "EPA/AA ratio" focus on anti-inflammatory and antiarrhythmogenic effects of long-chain omega-3 fatty acids.
Rupp H, Wagner D, Rupp T, Schulte LM, Maisch B. Rupp H, et al. Herz. 2004 Nov;29(7):673-85. doi: 10.1007/s00059-004-2602-4. Herz. 2004. PMID: 15580322 Review. - Omega-3 fatty acids for nutrition and medicine: considering microalgae oil as a vegetarian source of EPA and DHA.
Doughman SD, Krupanidhi S, Sanjeevi CB. Doughman SD, et al. Curr Diabetes Rev. 2007 Aug;3(3):198-203. doi: 10.2174/157339907781368968. Curr Diabetes Rev. 2007. PMID: 18220672 Review. - Associations of erythrocyte ω-3 fatty acids with biomarkers of ω-3 fatty acids and inflammation in breast tissue.
Roy S, Brasky TM, Belury MA, Krishnan S, Cole RM, Marian C, Yee LD, Llanos AA, Freudenheim JL, Shields PG. Roy S, et al. Int J Cancer. 2015 Dec 15;137(12):2934-46. doi: 10.1002/ijc.29675. Epub 2015 Jul 28. Int J Cancer. 2015. PMID: 26137879
Cited by
- Reducing the burden of obesity-associated cancers with anti-inflammatory long-chain omega-3 polyunsaturated fatty acids.
Khatib SA, Rossi EL, Bowers LW, Hursting SD. Khatib SA, et al. Prostaglandins Other Lipid Mediat. 2016 Sep;125:100-7. doi: 10.1016/j.prostaglandins.2016.07.011. Epub 2016 Jul 19. Prostaglandins Other Lipid Mediat. 2016. PMID: 27448716 Free PMC article. Review. - Association of dietary patterns and endoscopic gastric mucosal atrophy in an adult Chinese population.
Lin S, Gao T, Sun C, Jia M, Liu C, Ma X, Ma A. Lin S, et al. Sci Rep. 2019 Nov 12;9(1):16567. doi: 10.1038/s41598-019-52951-7. Sci Rep. 2019. PMID: 31719557 Free PMC article. - Omega-3 PUFA vs. NSAIDs for Preventing Cardiac Inflammation.
Ye J, Ghosh S. Ye J, et al. Front Cardiovasc Med. 2018 Oct 23;5:146. doi: 10.3389/fcvm.2018.00146. eCollection 2018. Front Cardiovasc Med. 2018. PMID: 30406113 Free PMC article. No abstract available. - Nuclear Factor of Activated T Cells-dependent Down-regulation of the Transcription Factor Glioma-associated Protein 1 (GLI1) Underlies the Growth Inhibitory Properties of Arachidonic Acid.
Comba A, Almada LL, Tolosa EJ, Iguchi E, Marks DL, Vara Messler M, Silva R, Fernandez-Barrena MG, Enriquez-Hesles E, Vrabel AL, Botta B, Di Marcotulio L, Ellenrieder V, Eynard AR, Pasqualini ME, Fernandez-Zapico ME. Comba A, et al. J Biol Chem. 2016 Jan 22;291(4):1933-1947. doi: 10.1074/jbc.M115.691972. Epub 2015 Nov 24. J Biol Chem. 2016. PMID: 26601952 Free PMC article. - New Insights into the Pathogenesis of Non-Alcoholic Fatty Liver Disease: Gut-Derived Lipopolysaccharides and Oxidative Stress.
Ferro D, Baratta F, Pastori D, Cocomello N, Colantoni A, Angelico F, Del Ben M. Ferro D, et al. Nutrients. 2020 Sep 10;12(9):2762. doi: 10.3390/nu12092762. Nutrients. 2020. PMID: 32927776 Free PMC article. Review.
References
- Burr ML, Fehily AM, Gilbert JF, Rogers S, Holliday RM, Sweetnam PM, Elwood PC, Deadman NM. Effects of changes in fat, fish, and fibre intakes on death and myocardial reinfarction: diet and reinfarction trial (DART) Lancet. 1989;2:757–761. - PubMed
- Marchioli R, Barzi F, Bomba E, Chieffo C, Di Gregorio D, Di Mascio R, Franzosi MG, Geraci E, Levantesi G, Maggioni AP, Mantini L, Marfisi RM, Mastrogiuseppe G, Mininni N, Nicolosi GL, Santini M, Schweiger C, Tavazzi L, Tognoni G, Tucci C, Valagussa F. Early protection against sudden death by n-3 polyunsaturated fatty acids after myocardial infarction: time-course analysis of the results of the Gruppo Italiano per lo Studio della Sopravvivenza nell'Infarto Miocardico (GISSI)-Prevenzione. Circulation. 2002;105:1897–1903. - PubMed
- Dietary supplementation with n-3 polyunsaturated fatty acids and vitamin E after myocardial infarction: results of the GISSI-Prevenzione trial. Gruppo Italiano per lo Studio della Sopravvivenza nell'Infarto miocardico. Lancet. 1999;354:447–455. - PubMed
- Lowther A, editor. Fisheries of the United States 2011. National Oceanic and Atmospheric Organization; Silverspring, MD: 2012.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Research Materials