Type 2 diabetes as a disease of ectopic fat? - PubMed (original) (raw)
Review
Type 2 diabetes as a disease of ectopic fat?
Naveed Sattar et al. BMC Med. 2014.
Abstract
Background: Although obesity and diabetes commonly co-exist, the evidence base to support obesity as the major driver of type 2 diabetes mellitus (T2DM), and the mechanisms by which this occurs, are now better appreciated.
Discussion: This review briefly examines several sources of evidence - epidemiological, genetic, molecular, and clinical trial - to support obesity being a causal risk factor for T2DM. It also summarises the ectopic fat hypothesis for this condition, and lists several pieces of evidence to support this concept, extending from rare conditions and drug effects to sex- and ethnicity-related differences in T2DM prevalence. Ectopic liver fat is the best-studied example of ectopic fat, but more research on pancreatic fat as a potential cause of β-cell dysfunction seems warranted. This ectopic fat concept, in turn, broadly fits with the observation that individuals of similar ages can develop diabetes at markedly different body mass indexes (BMIs). Those with risk factors leading to more rapid ectopic fat gain - for example, men (compared with women), certain ethnicities, and potentially those with a family history of diabetes, as well as others with genes linked to a reduced subcutaneous adiposity - are more likely to develop diabetes at a younger age and/or lower BMI than those without.
Summary: Obesity is the major risk factor for T2DM and appears to drive tissue insulin resistance in part via gain of ectopic fat, with the best-studied organ being the liver. However, ectopic fat in the pancreas may contribute to β-cell dysfunction. In line with this observation, rapid resolution of diabetes linked to a preferential and rapid reduction in liver fat has been noted with significant caloric reduction. Whether these observations can help develop better cost-effective and sustainable lifestyle /medical interventions in patients with T2DM requires further study.
Figures
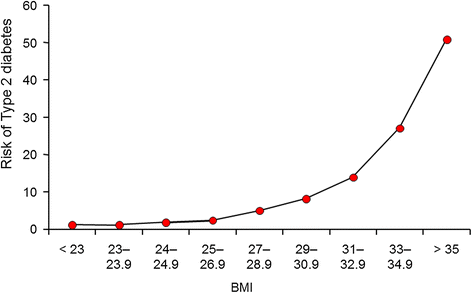
Figure 1
Relationship between body mass index (BMI) and risk for diabetes in US Health Professionals, derived from data extracted from Chan et al. [2].
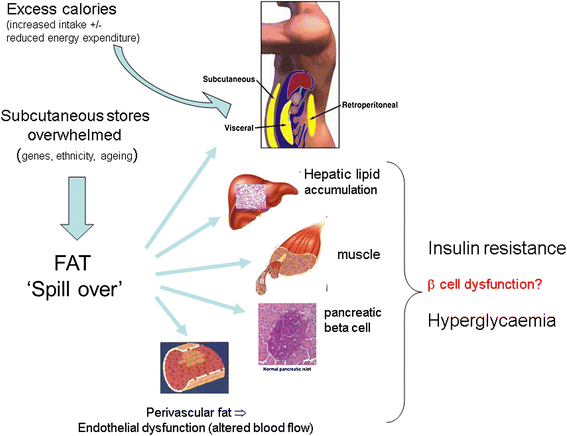
Figure 2
Simple concept of ectopic fat and development of insulin resistance and frank diabetes. A simple conceptual illustration on the development and location of ectopic fat in individuals once they have ‘overwhelmed’ their ability to store safe subcutaneous fat. Certain factors such as sex (females have greater storage capacity), genetics (with family history of type 2 diabetes mellitus (T2DM) as a broad proxy measure), ethnicity (for example, South Asians) and ageing appear to have relevance to an individual’s ability to store fat subcutaneously. Other factors, such as smoking, may also be relevant but more data are needed to examine this. In temporal terms, it may be that liver fat accumulation occurs closer to the time of development of T2DM whereas muscle insulin resistance is a more proximal development. Perivascular fat may contribute to vascular dysfunction via a process of adverse vasocrine signalling, leading in turn to impaired nutrient blood flow; that is, vascular insulin resistance. Finally, some recent evidence indicates that excess fat may also accumulate in the pancreas to contribute to β-cell dysfunction, and thus development of T2DM. Such excess pancreatic fat appears reversible, and could contribute to diabetes resolution even in some patients with T2DM who are on insulin.
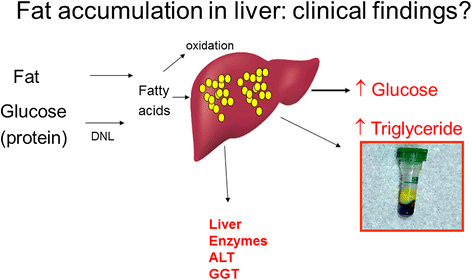
Figure 3
Biochemical findings supporting excess liver fat. This simple figure signals the link between excess calories, leading to excess liver fat and the common biochemical findings of high glucose, altered liver enzymes (alanine aminotransferase (ALT) much greater than aspartate aminotransferase (AST)) and hypertriglyceridaemia. When these three biochemical features are present in overweight or obese individuals who are not excessive alcohol drinkers, the likelihood of non-alcoholic fatty liver disease (NAFLD) is high.
Similar articles
- Plasma fibroblast growth factor 21 levels increase with ectopic fat accumulation and its receptor levels are decreased in the visceral fat of patients with type 2 diabetes.
Hong ES, Lim C, Choi HY, Lee YK, Ku EJ, Moon JH, Park KS, Jang HC, Choi SH. Hong ES, et al. BMJ Open Diabetes Res Care. 2019 Nov 17;7(1):e000776. doi: 10.1136/bmjdrc-2019-000776. eCollection 2019. BMJ Open Diabetes Res Care. 2019. PMID: 31798902 Free PMC article. - Pancreatic Fat is not significantly correlated with β-cell Dysfunction in Patients with new-onset Type 2 Diabetes Mellitus using quantitative Computed Tomography.
Li YX, Sang YQ, Sun Y, Liu XK, Geng HF, Zha M, Wang B, Teng F, Sun HJ, Wang Y, Qiu QQ, Zang X, Wang Y, Wu TT, Jones PM, Liang J, Xu W. Li YX, et al. Int J Med Sci. 2020 Jul 2;17(12):1673-1682. doi: 10.7150/ijms.46395. eCollection 2020. Int J Med Sci. 2020. PMID: 32714070 Free PMC article. - Failure of fat cell proliferation, mitochondrial function and fat oxidation results in ectopic fat storage, insulin resistance and type II diabetes mellitus.
Heilbronn L, Smith SR, Ravussin E. Heilbronn L, et al. Int J Obes Relat Metab Disord. 2004 Dec;28 Suppl 4:S12-21. doi: 10.1038/sj.ijo.0802853. Int J Obes Relat Metab Disord. 2004. PMID: 15592481 Review. - Low proliferative potential of adipose-derived stromal cells associates with hypertrophy and inflammation in subcutaneous and omental adipose tissue of patients with type 2 diabetes mellitus.
Stafeev I, Podkuychenko N, Michurina S, Sklyanik I, Panevina A, Shestakova E, Yah'yaev K, Fedenko V, Ratner E, Vorotnikov A, Menshikov M, Yashkov Y, Parfyonova Y, Shestakova M. Stafeev I, et al. J Diabetes Complications. 2019 Feb;33(2):148-159. doi: 10.1016/j.jdiacomp.2018.10.011. Epub 2018 Nov 4. J Diabetes Complications. 2019. PMID: 30482492 - Obesity, insulin resistance and comorbidities? Mechanisms of association.
Castro AV, Kolka CM, Kim SP, Bergman RN. Castro AV, et al. Arq Bras Endocrinol Metabol. 2014 Aug;58(6):600-9. doi: 10.1590/0004-2730000003223. Arq Bras Endocrinol Metabol. 2014. PMID: 25211442 Free PMC article. Review.
Cited by
- The Transcriptomic Evidence on the Role of Abdominal Visceral vs. Subcutaneous Adipose Tissue in the Pathophysiology of Diabetes in Asian Indians Indicates the Involvement of Both.
Kumar A, Tiwari P, Saxena A, Purwar N, Wahi N, Sharma B, Mathur SK. Kumar A, et al. Biomolecules. 2020 Aug 24;10(9):1230. doi: 10.3390/biom10091230. Biomolecules. 2020. PMID: 32847136 Free PMC article. - Type 2 diabetes and metabolic surgery guidelines and recommendations should urgently be unified.
Halpern B, Mancini MC. Halpern B, et al. Acta Diabetol. 2021 Apr;58(4):531-536. doi: 10.1007/s00592-020-01603-8. Epub 2020 Sep 15. Acta Diabetol. 2021. PMID: 32930887 Free PMC article. - Ectopic Fat Accumulation in Pancreas and Heart.
Kozawa J, Shimomura I. Kozawa J, et al. J Clin Med. 2021 Mar 23;10(6):1326. doi: 10.3390/jcm10061326. J Clin Med. 2021. PMID: 33806978 Free PMC article. Review. - Noninvasive fat quantification of the liver and pancreas may provide potential biomarkers of impaired glucose tolerance and type 2 diabetes.
Dong Z, Luo Y, Cai H, Zhang Z, Peng Z, Jiang M, Li Y, Li C, Li ZP, Feng ST. Dong Z, et al. Medicine (Baltimore). 2016 Jun;95(23):e3858. doi: 10.1097/MD.0000000000003858. Medicine (Baltimore). 2016. PMID: 27281097 Free PMC article. - Qizhi Jiangtang Jiaonang Improves Insulin Signaling and Reduces Inflammatory Cytokine Secretion and Reactive Oxygen Species Formation in Insulin Resistant HepG2 Cells.
Zhang XT, Yu CJ, Liu JW, Zhang YP, Zhang C, Song CX, Xie JS, Sai JY, Zheng JT, Wang F. Zhang XT, et al. Evid Based Complement Alternat Med. 2015;2015:518639. doi: 10.1155/2015/518639. Epub 2015 May 5. Evid Based Complement Alternat Med. 2015. PMID: 26074994 Free PMC article.
References
- Frayling TM, Timpson NJ, Weedon MN, Zeggini E, Freathy RM, Lindgren CM, Perry JRB, Elliott KS, Lango H, Rayner NW, Shields B, Harries LW, Barrett JC, Ellard S, Groves CJ, Knight B, Patch AM, Ness AR, Ebrahim S, Lawlor DA, Ring SM, Ben-Shlomo Y, Jarvelin MR, Sovio U, Bennett AJ, Melzer D, Ferrucci L, Loos RJF, Barroso I, Wareham NJ, et al. A common variant in the FTO gene is associated with body mass index and predisposes to childhood and adult obesity. Science. 2007;316:889–894. doi: 10.1126/science.1141634. - DOI - PMC - PubMed
- Rees SD, Islam M, Hydrie MZ, Chaudhary B, Bellary S, Hashmi S, O'Hare JP, Kumar S, Sanghera DK, Chaturvedi N, Barnett AH, Shera AS, Weedon MN, Basit A, Frayling TM, Kelly MA, Jafar TH. An FTO variant is associated with Type 2 diabetes in South Asian populations after accounting for body mass index and waist circumference. Diabet Med. 2011;28:673–680. doi: 10.1111/j.1464-5491.2011.03257.x. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical