Systemic Inflammation and Cardiovascular Comorbidity in Psoriasis Patients: Causes and Consequences - PubMed (original) (raw)
Review
Systemic Inflammation and Cardiovascular Comorbidity in Psoriasis Patients: Causes and Consequences
Wolf-Henning Boehncke. Front Immunol. 2018.
Abstract
Psoriasis is a common inflammatory skin disease characterized by the appearance of red scaly plaques that can affect any part of the body. High prevalence, chronicity, disfiguration, disability, and associated comorbidity make it a challenge for clinicians of multiple specialties. Likewise, its complex pathogenesis, comprising inflammation, hyperproliferation, and angioneogenesis, intrigues numerous scientific disciplines, namely, immunology. From a clinical perspective, the severity of psoriasis is highlighted by its increased mortality, with cardiovascular diseases contributing the highest excess risk. From a scientific point of view, psoriasis has to be considered a systemic inflammatory condition, as blood biomarkers of inflammation are elevated and imaging techniques document sites of inflammation beyond the skin. While the association of psoriasis with cardiovascular diseases is now widely accepted, causes and consequences of this association are controversially discussed. This review comments on epidemiologic, genetic, and mechanistic studies that analyzed the relation between psoriasis and cardiovascular comorbidity. The hypothesis of psoriasis potentially being an independent cardiovascular risk factor, driving atherosclerosis via inflammation-induced endothelial dysfunction, will be discussed. Finally, consequences for the management of psoriasis with the objective to reduce the patients' excess cardiovascular risk will be pointed out.
Keywords: atherosclerosis; coronary heart disease; endothelial dysfunction; insulin resistance; mortality; psoriasis; stroke.
Figures
Figure 1
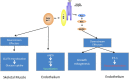
Metabolic and vascular effects of insulin. Under physiologic conditions, the activated insulin receptor on endothelial cells leads to phosphorylation of endothelial nitric oxide synthase (eNOS) via activation of insulin receptor substrate (IRS) and phosphoinositide-3-kinase (a). This results in vasodilation via NO production. This branch also regulates GLUT4 translocation and glucose uptake in muscle cells. The mitogen-activated protein kinase (MAPK) pathway controls secretion of vasoconstrictive ET-1 in endothelial cells, and cell growth and mitogenesis in cells at large. Inflammation reduces NO production via blocking insulin receptor signaling at the level of the IRS-1 (b).
Figure 2
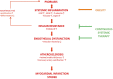
The concept of the “psoriatic march.” This hypothesis suggests that psoriasis is a systemic inflammatory condition, as numerous biomarkers of inflammation are elevated in the patients’ blood compartment. Functional consequences are insulin resistance, evidenced by an increased HOMA-IR (homeostasis assessment of insulin resistance), and endothelial dysfunction, resulting in increased vascular stiffness. This provides the basis for atherosclerosis, observable through analysis of vessel wall composition via CTs or ultrasound. Depending on the sites of atherosclerosis, major cardiovascular events such as myocardial infarction and stroke result from this. This “backbone” (red, bold) may be developed further by adding additional “modules”: insulin resistance has been shown to alter epidermal homeostasis (red, fine). Obesity, causing a state of systemic inflammation as well, is a known risk factor for psoriasis and may induce the phenotype (orange, bold). Whether systemic anti-inflammatory therapy is capable of reducing the patients’ cardiovascular risk through reducing insulin resistance and endothelial dysfunction is still a matter of debate (green).
References
- WHO. Document EB133.R2, Agenda Item 6.2. (2013).
- Mehta NN, Yu Y, Saboury B, Foroughi N, Krishnamoorthy P, Raper A, et al. Systemic and vascular inflammation in patients with moderate to severe psoriasis as measured by [18F]-fluorodeoxyglucose positron emission tomography-computed tomography (FDG-PET/CT): a pilot study. Arch Dermatol (2011) 147(9):1031–9.10.1001/archdermatol.2011.119 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical