Blood Cell - The Definitive Guide | (original) (raw)
Definition
Any blood cell definition involves a variety of cell types, each with specific functions. The primary components of blood are plasma, leukocytes, erythrocytes, and platelets; the latter three are all blood cell examples. Without them, no oxygen transportation through the circulatory system would occur, our blood would not clot, and we would have a severely compromised immune system. Blood cell production begins in the red bone marrow.
Blood Cell Types
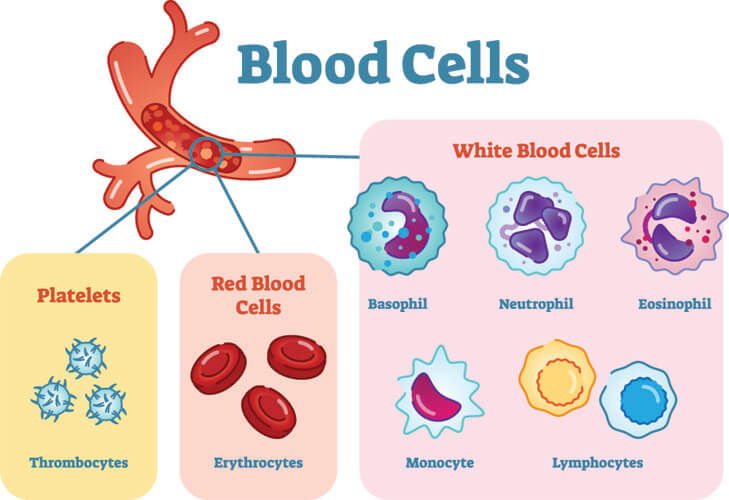
There are three main blood cell types: white (leukocytes), red (erythrocytes), and platelets (thrombocytes).
Leukocytes come in a variety of forms. The original cell – the hematopoietic blood cell – is a multipotent stem cell that differentiates into the precursors of all blood cells.
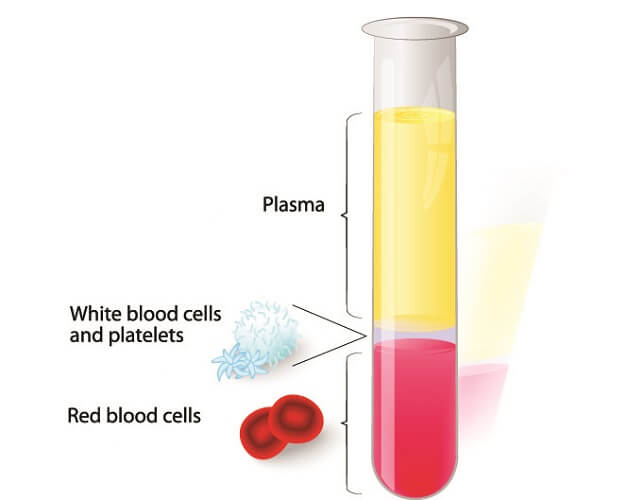
Blood cells are heavier than blood plasma and sink in a sample.
If you leave a blood sample to stand for thirty minutes, you will notice that the different components separate. Heavier erythrocytes sink to the bottom; these make up around 45% of the total blood sample. In the middle of the tube a thin, pale line constitutes the leukocyte and platelet populations. Leukocytes make up around 0.7% of the total blood volume (TBV) in a healthy person; platelets also form less than 1% of the TBV.
Plasma, at the top of the sample, helps transport the different cells through the body as well as a range of molecules. This fluid contains around 92% water; the rest is composed of important proteins (albumin, gamma globulin, and clotting factors) and a small proportion of sugars, fats, hormones, vitamins, and mineral salts.
Fresh frozen plasma does not contain blood cells.
There is only one type of red blood cell in the body; the same applies to the thrombocyte. The white blood cell, however, is found in several forms.
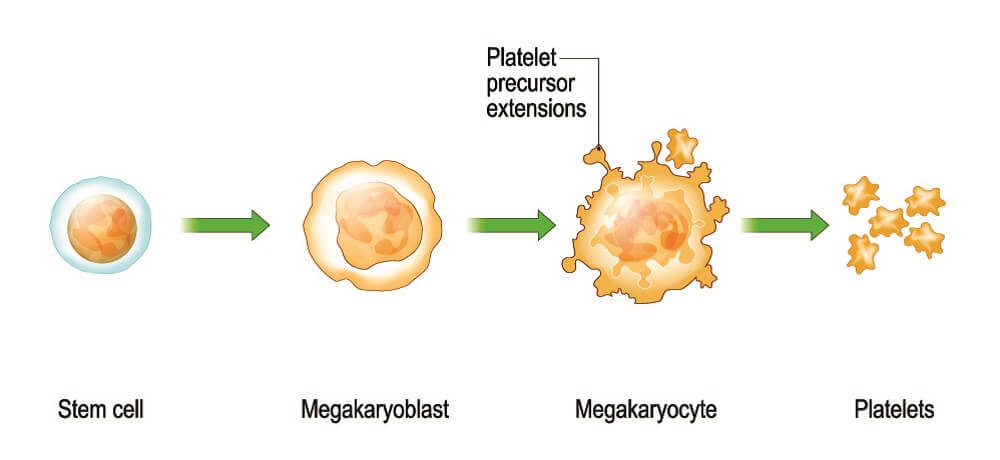
The smallest of the three types is the thrombocyte. It measures between five to seven micrometers in diameter – about 350 platelets would fit on the head of a pin. Plate-like in shape (hence the name), these cells are fragments of a larger cell called a megakaryocyte. Each megakaryocyte can produce one to three thousand platelets. Every day, a healthy human produces circa ten billion platelets; blood vessel trauma can increase this production rate twenty-fold.
Platelets are functional fragments of larger cells.
The erythrocyte measures between six to eight micrometers – 250 could fit on the head of a pin. It is a circular disc with concave centers on both sides. This shape increases the surface area of the cell for efficient oxygen uptake and release. Every day, a healthy human produces circa 200 billion of these important cells.
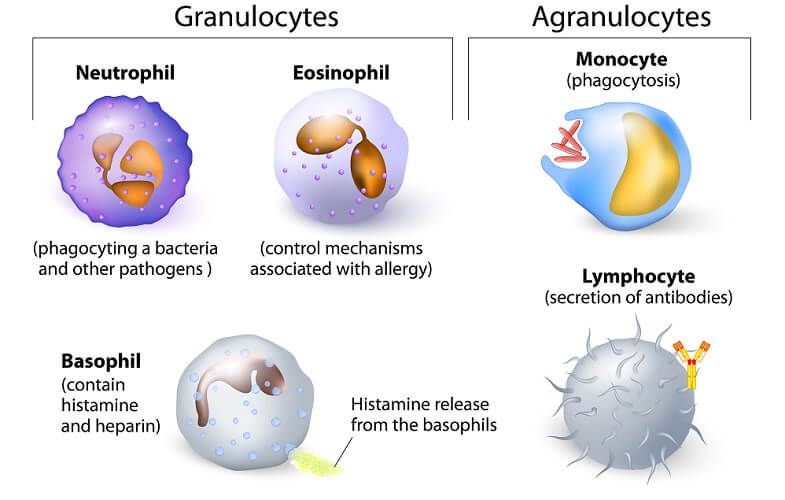
The white blood cell (WBC) comes in a variety of forms. These are primarily produced in the red bone marrow and differentiate at different stages and in different tissues such as the lymphatic organs. The main white blood cell types are:
- Monocytes: the largest WBC with an amoeba-like form that differentiates into macrophages.
- Lymphocytes: T cells and B cells that mature in the lymphatic organs after which they are named.
- Neutrophils: the most prolific WBC.
- Eosinophils: make up less than 6% of total blood cell counts, sometimes as low as 0.1%.
- Basophils: the least common WBC, but the second-largest.
WBC types
Blood Cell Lineage
Scientific ideas about blood cell linage are going through many changes. The earlier understanding of blood cell formation from stem cells – hematopoiesis – is becoming outdated as researchers discover anomalies in the classic theory. Dendritic cells, for example, were formerly thought to originate from the leukocyte line but now appear to have their own, unique branch.
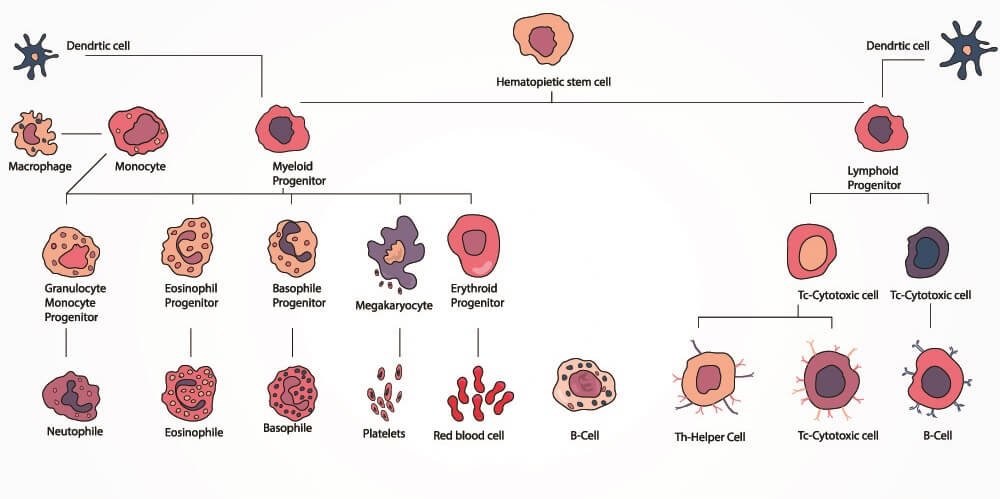
The classic hematopoietic blood cell diagram below shows the main lineages. A single multipotent hematopoietic stem cell is the origin of all blood cells. From this, two progenitor cells – common myeloid and common lymphoid – split the production process of lymphocytes from the other blood cell groups.
The common myeloid progenitor cell can differentiate into the megakaryocyte that will fragment to produce thrombocytes, erythrocyte progenitors, mast cells (of connective tissue), and myeloid leukocyte progenitors.
Hematopoiesis – blood cell differentiation from a single stem cell.
The above example has become outdated. Theories include the differentiation of a long-term hematopoietic stem cell that can self-renew to a short-term cell that must differentiate. The short-term stem cell either produces:
- Megakaryocyte-erythroid progenitor (MEP) cells that become platelets or erythrocytes;
- Common myeloid progenitor cells that form MEPs or granulocyte-macrophage progenitor (GMP) cells;
- Lymphoid-primed multipotential progenitor cells that differentiate into GMPs or common lymphocyte progenitors (CLPs);
- CLPs that become the lymphocyte group of leukocytes.
With this theory, blood cell lineages intertwine. A dendritic cell can be formed either by a GMP or a CLP. A GMP can be formed from a CMP or a lymphoid-primed multipotential progenitor cell. A CLP is the result of differentiation either in a short-term hematopoietic stem cell or a lymphoid-primed progenitor.
As yet, scientists have not agreed on a standard lineage process as they are still learning about the complex stages of blood cell production.
Blood Cell Function
Blood cell functions can be split into three main groups according to type: oxygen transportation, immunity, and the blood clotting process. These functions are the result of the erythrocyte, leukocyte, and thrombocyte respectively.
Red Blood Cell Function
Red blood cells (RBCs) transport oxygen and some nutrients through the circulatory system, although recent advances tell us that they also help to:
- Regulate redox reactions that help determine the lifespan of different cells. This involves the balance between reactive oxygen species (ROS), reactive nitrogen species (RNS), and the antioxidants that make these species less harmful;
- Increase or reduce tissue perfusion through the uptake and release of nitrous oxide. Nitrous oxide has a direct effect on vasodilation;
- Affect blood viscosity through RBC form and movement through the bloodstream – erythrocytes can elongate, tank-tread, swing, or tumble through the blood according to how much hemoglobin they contain, how much water they have, and whether the cells brush against the blood vessel wall or move through its center.
Red blood cells collect and drop off oxygen.
The primary role of erythrocytes – the transport of gases from the lungs to the tissues – gives two results: oxygen supply to the cells of tissues and partial maintenance of the acid/base equilibrium.
RBCs contain a protein called hemoglobin wrapped around iron atoms. Oxygen attaches readily to the iron and is released when the cell arrives at an area where the oxygen concentration is lower.
Carbon dioxide in the blood acts as an acid; although only a small percentage of this gas is taken up in RBCs, the system that controls body pH is extremely sensitive.
White Blood Cell Function
This article will not discuss the different functions of WBC groups. Leukocytes are immune cells that work in different ways to remove foreign particles such as microbes and pollutants, and waste products that include dead cells and toxins.
The responsibility of the leukocytes.
Humans rely on three types of immunity:
- Innate immunity: natural barriers that include the skin, stomach acid, and innate leukocytes that directly identify and eliminate pathogens (harmful molecules and microorganisms). These include natural killer cells and phagocytic cells like macrophages.
- Adaptive or acquired immunity: primarily the domain of lymphocytes that produce antibodies (humoral immune response) during a later or recurring stage of infection.
- Passive immunity: immunity taken from another source, usually in the form of antibodies in the mother’s breast milk or the infusion of antibodies.
Platelet Function
Platelets circulate in the blood and go through three different stages when they detect blood vessel wall damage. Thrombocytes are part of the hemostasis mechanism that helps prevent blood from leaking out of damaged capillaries, veins, and arteries.
The coagulation cascade – a complex but life-saving mechanism.
The following steps occur:
- Receptors on the platelet membrane detect vessel wall damage. When damage occurs, the endothelium releases chemicals that are recognized by platelet receptors. Early-arriving platelets that pick up these chemicals via their receptors change shape and begin to stick to exposed collagen within the affected area. This primary part of the hemostatic process is called adhesion or tethering.
- Upon adhesion, the next step – thrombocyte activation – occurs. With the shape change, various cytoplasmic granules and chemokines are released. Shape changes include pseudopods – false feet – that help the adhesion layer stick to the endothelium and also to newly arriving thrombocytes. The released chemicals are involved in the activation of extrinsic and intrinsic blood clotting pathways – the coagulation cascade (see above image).
- More and more platelets arrive to form a clot on top of the adhered layer. This process is called aggregation. The platelet cytoskeleton shrinks to reduce the clot size once no more damage signals are produced. Over time, the clot breaks down.
Blood Cell Count
Blood tests always include cell counts to detect abnormalities. Elevated or low cell numbers can mean the presence of disease.
When all blood cell counts are low, for example, this could indicate a problem in the bone marrow. If only one type of WBC is elevated this could show the presence of a specific pathogen – people with asthma usually have high eosinophil counts, for example.
The complete blood count is a routine test.
Normal Blood Cell Count
In the average, healthy human, the following numbers apply:
- Normal red blood cell count: 4.2 million to 6.1 million cells per microliter (cells/mcL)
- Normal white blood cell count: 4.5 thousand to 11 thousand cells/mcL
- Normal platelet count: 150 thousand to 450 thousand cells/mcL
Elevated Blood Cell Count Causes
Higher numbers than usual indicate a problem:
- High red blood cell count causes: low oxygen levels in the blood (respiratory or cardiovascular disorders), dehydration, kidney disease, bone marrow overproduction (polycythemia vera).
- High white blood cell count causes: the presence of infection or inflammation, physical and emotional stress, immune disorders, polycythemia vera.
- High platelet count causes: polycythemia vera, infection, and inflammation, some forms of anemia, problems with the spleen (a reservoir for platelets), cancer.
Low Blood Cell Count Causes
Low numbers also indicate a health problem:
- Low red blood cell count causes: anemia, bone marrow failure, kidney disease, bleeding, low iron, copper, folate, or B vitamin levels, pregnancy, thyroid disorders, cancer.
- Low white blood cell count causes: severe infections, antibiotic use, sarcoidosis, bone marrow failure, cancer and cancer therapy, autoimmune disorders.
- Low platelet count causes: bone marrow failure, bacterial blood infection, alcohol abuse, cancer therapy, viral infections, nutritional deficiency, idiopathic or thrombotic thrombocytopenic purpura, organ failure.
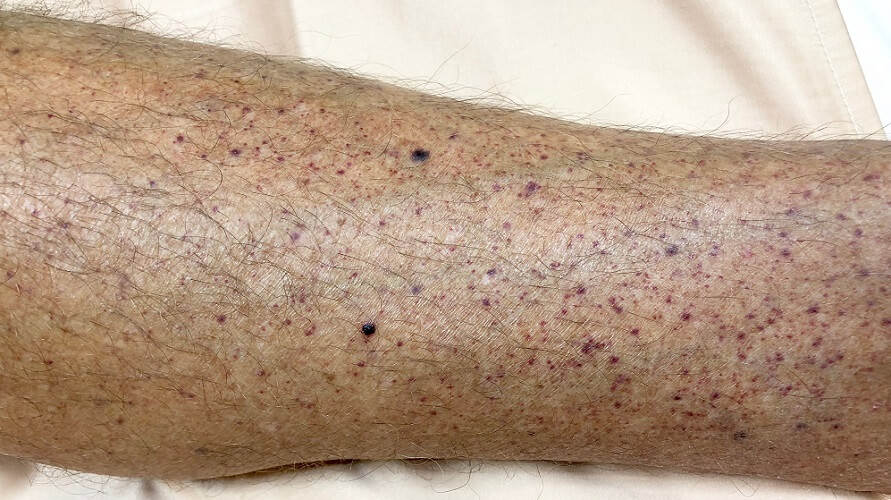
Thrombocytopenic purpura – low platelet count.
Bibliography
Show/Hide
- Dean L. Blood Groups and Red Cell Antigens [Internet]. Bethesda (MD): National Center for Biotechnology Information (US); 2005. Chapter 1, Blood and the Cells it Contains. Retrieved from: https://www.ncbi.nlm.nih.gov/books/NBK2263/
- Rogers K (Ed). (2011). Blood: Physiology and Circulation. New York, Britannica Educational Publishing.
- El-Badri N (Ed.). (2019). Regenerative Medicine and Stem Cell Biology. Cham, Springer Nature Switzerland.