Albumin: Reference Range, Interpretation, Collection and Panels (original) (raw)
Reference Range
The reference range for albumin testing is as follows: [1, 2]
- The normal range is 3.5 to 5.5 g/dL or 35-55 g/liter. This range may vary slightly in different laboratories.
- Albumin composes 50%-60% of blood plasma proteins.
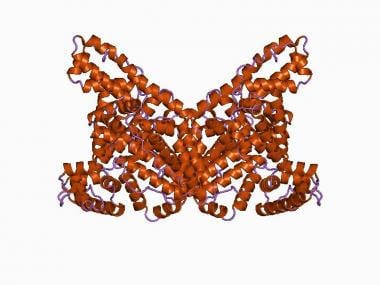
An image depicting human serum albumin can be seen below.
The structure of human serum albumin.

Interpretation
The albumin test measures the amount of albumin in the clear liquid portion of blood.
Dehydration is associated with "high" levels of albumin.
Conditions associated with "low" levels of albumin are as follows:
- Burns
Other states are as follows:
- Nephropathy
- Hepatic encephalopathy
- Hepatorenal syndrome

Collection and Panels
Methods
Details are as follows:
- Specimen type: Blood
- Container: Vacuum tubes
- Collection method: Venipuncture
- Albumin tester: A digital sensing platform running on a smart phone. [4]
Panels
Albumin testing is part of a comprehensive metabolic panel. The liver panel is a related test.

Background
Description
Albumin is a blood plasma protein synthesized in the liver. It is the single most abundant protein in plasma and constitutes about two-thirds of total protein content. Because it is the main protein in human blood, decreases in albumin due to decreased synthesis or losses result in impaired regulation of intravascular oncotic pressure and manifests as edema. As such, it transports certain hormones (eg, thyroid, estrogen, cortisol) when their specific binding globulins are saturated, as well as unconjugated bilirubin and other organic anions and many drugs (eg, penicillin, warfarin). Albumin is soluble in water, precipitated by acid, and coagulated by heat. The chief functions of albumin are to transport a wide variety of ligands, to maintain plasma oncotic pressure, and to serve as a source for endogenous amino acids. [1, 2]
Several methods exist for determining albumin levels, including dye-binding methods, electrophoresis, and immunochemical methods, as well as dipstick methods for urinary albumin.
For the determination of albumin in serum/plasma, the patient should stop taking drugs that affect albumin measurements, such as anabolic steroids, androgens, growth hormones, [5] and insulin.
A blood sample is put in a centrifuge, which spins and separates the cells from the serum.
Indications/applications
The albumin test helps to determine if the patient has liver or kidney disease or if the body is not absorbing enough protein.
Indications for the albumin test are as follows:
- Jaundice [6]
- Fatigue
- Weight loss
Causes of changes in albumin levels are as follows:
- Decreased production (low protein diet or malnutrition, malabsorption)
- Cirrhosis of the liver
- Excess excretion by the kidneys (ascites or protein-losing nephropathy or enteropathy) [7]
- Prolonged diarrhea
- Loss from skin through burns
A study by Kawaguchi et al indicated that in patients with nonalcoholic fatty liver disease (NAFLD), reductions in serum albumin are predictive of serious complications. While in study patients without serious complications, the serum albumin level declined by 0.04 g/dL/year, in, for example, those who suffered hepatic failure, the level was reduced by 0.38 g/dL/year, and in patients with gastroesophageal varices, by 0.25 g/dL/year. [8]
Limitations
See the list below:
- Albumin production is decreased during pregnancy.
- Patients taking large amounts of intravenous fluids may have inaccurate results.
- The test may need to be performed with creatinine and blood urea nitrogen tests to evaluate kidney function. [9]
- This test may need to be performed with a prealbumin test to evaluate nutritional status.
- Marked lipemia can interfere with albumin measurement.

- Burtis CA, Ashwood MD. Tietz Textbook of Clinical Chemistry. 3rd ed. Saunders; 1999.
- McPherson RA, Pincus MR. Henry's Clinical Diagnosis and Management by Laboratory Methods: Expert Consult - Online and Print. 22nd ed. Saunders; 2011.
- Kirac Y, Bilen S, Duranay M. Comparison of laboratory findings in patients with glomerulonephritis classified according to histopathologic diagnosis. Minerva Med. 2014 Apr. 105(2):149-56. [QxMD MEDLINE Link].
- Coskun AF, Nagi R, Sadeghi K, Phillips S, Ozcan A. Albumin testing in urine using a smart-phone. Lab Chip. 2013 Nov 7. 13(21):4231-8. [QxMD MEDLINE Link]. [Full Text].
- Rasmussen MH, Brændholt Olsen MW, Alifrangis L, Klim S, Suntum M. A Reversible Albumin-binding Growth Hormone Derivative is Well-tolerated and Possesses a Potential Once-weekly Treatment Profile. J Clin Endocrinol Metab. 2014 Jul 11. jc20141702. [QxMD MEDLINE Link].
- Xu B, Yu HB, Hui W, He JL, Wei LL, Wang Z, et al. Clinical features and risk factors of acute hepatitis E with severe jaundice. World J Gastroenterol. 2012 Dec 28. 18(48):7279-84. [QxMD MEDLINE Link]. [Full Text].
- Ni Z, Yuan Y, Wang Q, Cao L, Che X, Zhang M, et al. Time-averaged albumin predicts the long-term prognosis of IgA nephropathy patients who achieved remission. J Transl Med. 2014 Jul 10. 12(1):194. [QxMD MEDLINE Link]. [Full Text].
- Kawaguchi K, Sakai Y, Terashima T, et al. Decline in serum albumin concentration is a predictor of serious events in nonalcoholic fatty liver disease. Medicine (Baltimore). 2021 Aug 6. 100 (31):e26835. [QxMD MEDLINE Link]. [Full Text].
- Robb A, Ffrench-Constant A, Morris R, Denison F, Stock S. PMM.43 The Predictive Value of Urinary Albumin: Creatinine Ratio In Pregnancy. Arch Dis Child Fetal Neonatal Ed. 2014 Jun. 99 Suppl 1:A137. [QxMD MEDLINE Link].
- The structure of human serum albumin.


Author
Sridevi Devaraj, PhD, DABCC, FAACC, FRSC, CCRP Medical Director of Clinical Chemistry and Point of Care Technology (POCT), Texas Children’s Hospital and Clearlake Health Center; Director of Laboratories, TCH Centers for Women and Children; Professor of Pathology and Immunology, Director, Clinical Chemistry Fellowship and Clinical Chemistry Resident Rotation, Baylor College of Medicine; Associate Director, Texas Children’s Microbiome Center
Disclosure: Nothing to disclose.
Chief Editor
Jun Teruya, MD, DSc, FCAP Professor of Pathology and Immunology, Professor of Pediatrics, Professor of Medicine, Vice Chairman for Education, Director, Tranfusion Medicine/Blood Banking Fellowship Program, Baylor College of Medicine; Chief, Division of Transfusion Medicine and Coagulation, Texas Children's Hospital
Jun Teruya, MD, DSc, FCAP is a member of the following medical societies: American Association of Blood Banks, American Society for Clinical Pathology, American Society of Hematology, College of American Pathologists, International Society on Thrombosis and Haemostasis, Massachusetts Medical Society
Disclosure: Nothing to disclose.