Oral antihyperglycemic therapy for type 2 diabetes mellitus - PubMed (original) (raw)
Review
Oral antihyperglycemic therapy for type 2 diabetes mellitus
Alice Y Y Cheng et al. CMAJ. 2005.
Abstract
Diabetes mellitus is a chronic disease that is growing in prevalence worldwide. Pharmacologic therapy is often necessary to achieve optimal glycemic control in the management of diabetes. Orally administered antihyperglycemic agents (OHAs) can be used either alone or in combination with other OHAs or insulin. The number of available OHAs has increased significantly in the last decade, which translates into more therapeutic options and complex decision-making for physicians. This review article is designed to help with these decisions. We review the mechanism of action, efficacy and side effects of the different classes of OHAs (alpha-glucosidase inhibitors, biguanides, insulin secretagogues, insulin sensitizers and intestinal lipase inhibitor) and discuss the current recommendations for their use.
Figures
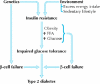
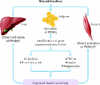
Fig. 1: Overview of the pathogenesis of type 2 diabetes mellitus. FFA = free fatty acids. Photo: Lianne Friesen and Nicholas Woolridge
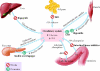
Fig. 2: Major target organs and actions of orally administered antihyperglycemic agents in type 2 diabetes mellitus. TZD = thiazolidinedione; FFA = free fatty acid; AGI = α-glucosidase inhibitor. Photo: Lianne Friesen and Nicholas Woolridge
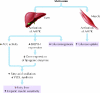
Fig. 3: Metformin activates AMPK in liver and muscle to improve glucose and lipid metabolism in type 2 diabetes. (A) shows the ion channel in a resting pancreatic β cell. (B) shows the action of insulin secretagogues on the cell. AMPK = adenosine monophosphate-activated protein kinase; ACC = acetyl-CoA carboxylase; SREPB-1 = sterol-regulatory-element-binding-protein-1; VLDL = very low density lipoprotein. Photo: Lianne Friesen and Nicholas Woolridge
Box 1
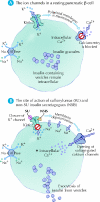
Fig. 4: Insulin secretagogues mimic glucose to close adenosine triphosphate-sensitive potassium channels (kir6.2) and stimulate insulin secretion. Photo: Lianne Friesen and Nicholas Woolridge
Fig. 5: Mechanism of action of thiazolidinediones. PPARγ = peroxisome proliferator-activated receptor-gamma; TNF-α = tumour necrosis factor-α. *There is recent evidence in rodents that skeletal muscle PPARγis an important mediator of the beneficial effects of TZDs on insulin sensitivity. Photo: Lianne Friesen and Nicholas Woolridge
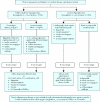
Fig. 6: Management of hyperglycemia in type 2 diabetes. BMI = body mass index. *When used in combination with insulin, insulin sensitizers may increase the risk of edema of congestive heart failure. The combination of an insulin sensitizer and insulin is currently not an approved indication in Canada. †If using preprandial insulin, do not add an insulin secretagogue. Reprinted with permission from Can J Diabetes 2003;27(Suppl 2):S39.
Comment in
- Effect of thiazolidinediones on lipid profile.
Madan P. Madan P. CMAJ. 2005 Aug 16;173(4):344; author reply 344-5. doi: 10.1503/cmaj.1050034. CMAJ. 2005. PMID: 16103495 Free PMC article. No abstract available.
Similar articles
- [Efficacy of combination therapy of alpha-glucosidase inhibitor and insulin sensitizer in patients with type 2 diabetes].
Kitaoka H. Kitaoka H. Nihon Rinsho. 2002 Sep;60 Suppl 9:464-9. Nihon Rinsho. 2002. PMID: 12387035 Review. Japanese. No abstract available. - Oral antidiabetic agents: current role in type 2 diabetes mellitus.
Krentz AJ, Bailey CJ. Krentz AJ, et al. Drugs. 2005;65(3):385-411. doi: 10.2165/00003495-200565030-00005. Drugs. 2005. PMID: 15669880 Review. - Type 2 diabetes and oral antihyperglycemic drugs.
Mizuno CS, Chittiboyina AG, Kurtz TW, Pershadsingh HA, Avery MA. Mizuno CS, et al. Curr Med Chem. 2008;15(1):61-74. doi: 10.2174/092986708783330656. Curr Med Chem. 2008. PMID: 18220763 Review. - [Combination therapy with biguanides].
Sakura H. Sakura H. Nihon Rinsho. 2002 Oct;60 Suppl 10:724-8. Nihon Rinsho. 2002. PMID: 12430309 Review. Japanese. No abstract available. - Oral antihyperglycemic therapy for type 2 diabetes: clinical applications.
Holmboe ES. Holmboe ES. JAMA. 2002 Jan 16;287(3):373-6. doi: 10.1001/jama.287.3.373. JAMA. 2002. PMID: 11790217
Cited by
- Antidiabetic effects of pterosin A, a small-molecular-weight natural product, on diabetic mouse models.
Hsu FL, Huang CF, Chen YW, Yen YP, Wu CT, Uang BJ, Yang RS, Liu SH. Hsu FL, et al. Diabetes. 2013 Feb;62(2):628-38. doi: 10.2337/db12-0585. Epub 2012 Oct 15. Diabetes. 2013. PMID: 23069626 Free PMC article. - Elucidation of the Mechanisms and Molecular Targets of Sanhuang Xiexin Decoction for Type 2 Diabetes Mellitus Based on Network Pharmacology.
Xu M, Li Z, Yang L, Zhai W, Wei N, Zhang Q, Chao B, Huang S, Cui H. Xu M, et al. Biomed Res Int. 2020 Aug 10;2020:5848497. doi: 10.1155/2020/5848497. eCollection 2020. Biomed Res Int. 2020. PMID: 32851081 Free PMC article. - The inhibitory activities of the edible green alga Capsosiphon fulvescens on rat lens aldose reductase and advanced glycation end products formation.
Islam MN, Choi SH, Moon HE, Park JJ, Jung HA, Woo MH, Woo HC, Choi JS. Islam MN, et al. Eur J Nutr. 2014 Feb;53(1):233-42. doi: 10.1007/s00394-013-0521-y. Epub 2013 Apr 11. Eur J Nutr. 2014. PMID: 23575770 - Autonomic modulation by SGLT2i or DPP4i in patients with diabetes favors cardiovascular outcomes as revealed by skin sympathetic nerve activity.
Chen JJ, Lin C, Lo MT, Lin LY, Chang HC, Liu GC. Chen JJ, et al. Front Pharmacol. 2024 Jul 30;15:1424544. doi: 10.3389/fphar.2024.1424544. eCollection 2024. Front Pharmacol. 2024. PMID: 39139635 Free PMC article. - In vitro and in silico interaction of porcine α-amylase with Vicia faba crude seed extract and evaluation of antidiabetic activity.
Choudhary DK, Mishra A. Choudhary DK, et al. Bioengineered. 2017 Jul 4;8(4):393-403. doi: 10.1080/21655979.2016.1235102. Epub 2016 Oct 28. Bioengineered. 2017. PMID: 27791455 Free PMC article.
References
- Zimmet P, Alberti KG, Shaw J. Global and societal implications of the diabetes epidemic. Nature 2001;414:782-7. - PubMed
- Health Canada. Diabetes in Canada. 2nd ed. Ottawa: Centre for Chronic Disease Prevention and Control, Population and Public Health Branch; 2002. Available at: www.hc-sc.gc.ca/pphb-dgspsp/publicat/dic-dac2/english/01cover_e.html (accessed 2004 Nov 22).
- The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993;329:977-86. - PubMed
- UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet 1998;352:837-53. - PubMed
- Ohkubo Y, Kishikawa H, Araki E, Miyata T, Isami S, Motoyoshi S, et al. Intensive insulin therapy prevents the progression of diabetic microvascular complications in Japanese patients with non-insulin dependent diabetes mellitus: a randomized prospective 6-year study. Diabetes Res Clin Pract 1995; 28 (2): 103 -17. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical