Empiric broad-spectrum antibiotic therapy of nosocomial pneumonia in the intensive care unit: a prospective observational study - PubMed (original) (raw)
Comparative Study
doi: 10.1186/cc4919. Epub 2006 May 16.
Affiliations
- PMID: 16704742
- PMCID: PMC1550932
- DOI: 10.1186/cc4919
Comparative Study
Empiric broad-spectrum antibiotic therapy of nosocomial pneumonia in the intensive care unit: a prospective observational study
Francisco Alvarez-Lerma et al. Crit Care. 2006.
Abstract
Introduction: Antibiotic de-escalation, which consists of the initial institution of empiric broad-spectrum antibiotics followed by antibiotic streamlining driven by microbiological documentation, is thought to provide maximum benefit for the individual patient, while reducing the selection pressure for resistance.
Methods: To assess a carbapenem-based de-escalating strategy in nosocomial pneumonia (NP), a prospective observational study was conducted in critically ill patients with NP treated empirically with imipenem +/- aminoglycoside/glycopeptide in 24 intensive care units of Spanish general hospitals. Overall, 244 patients were assessable (91% with late-onset NP). The primary outcome was therapeutic success 7-9 days post therapy.
Results: Microbial identification--based on cultures of tracheal aspirates in 82% of patients, cultures of protected specimen brush in 33%, and cultures of bronchoalveolar lavage in 4%--was only available for 131 (54%) patients. Initial antibiotics were inadequate for 23 (9%) patients. Of the remaining patients, antibiotics were streamlined in 56 (23%) patients and remained unchanged in 14 (6%) patients based on microbiology data, in 38 (16%) patients despite microbiology data favouring de-escalation, and in 113 (46%) patients due to unknown aetiology. Overall, de-escalation was implemented in only 23% of patients with potentially multiresistant pathogens, compared with 68% of patients with the remaining pathogens (P < 0.001). Response rates were 53% for patients continuously treated with imipenem-based regimens and 50% for the de-escalated patients. Higher Acute Physiology, Age, and Chronic Health Evaluation II scores were associated with greater mortality, whereas adequate empiric antibiotic therapy protected against fatal outcomes. No increase of superinfection rates caused by emerging pathogens was observed. The costs associated with de-escalation were mainly dependent on the duration of hospitalization.
Conclusion: This study mainly highlights the current practice of a specific algorithm of de-escalation solely based on the available microbiological data, and highlights the barriers to using it more widely. In this setting, de-escalation was less likely to occur in the presence of potentially multiresistant pathogens. Prior antibiotic administration and the low use of bronchoscopic techniques may have influenced negatively the implementation of de-escalation. Optimization of de-escalation strategies for NP should rely on a correct choice of empiric antibiotics, on appropriate microbiological investigations, and on a balanced interpretation of microbiological and clinical data.
Figures
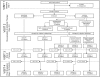
Figure 1
Study overview: flow chart representing the patient flow throughout the different study visits. Visit 1, onset of study therapy; visit 2 (3–5 days later), investigators streamlined antibiotics if favourable microbiological data were available; visit 3, patients were re-evaluated after discontinuation of therapy, visit 4, patients were re-evaluated 7–9 days later. MITT, modified intention-to-treat; D, dead; LFU, lost to follow-up.
Similar articles
- De-escalation therapy in ventilator-associated pneumonia.
Niederman MS. Niederman MS. Curr Opin Crit Care. 2006 Oct;12(5):452-7. doi: 10.1097/01.ccx.0000244126.84989.a2. Curr Opin Crit Care. 2006. PMID: 16943725 Review. - De-escalation therapy in ventilator-associated pneumonia.
Rello J, Vidaur L, Sandiumenge A, Rodríguez A, Gualis B, Boque C, Diaz E. Rello J, et al. Crit Care Med. 2004 Nov;32(11):2183-90. doi: 10.1097/01.ccm.0000145997.10438.28. Crit Care Med. 2004. PMID: 15640629 - Current guidelines for the treatment of severe pneumonia and sepsis.
Bodmann KF. Bodmann KF. Chemotherapy. 2005 Aug;51(5):227-33. doi: 10.1159/000087452. Chemotherapy. 2005. PMID: 16103664 Review.
Cited by
- Evaluation to Determine Antibiotic Resistance Reduction in Gram-Negative Bacteria from 2019 to 2021 by the Saudi Arabia National Plan.
Alrehaili JA. Alrehaili JA. J Pharm Bioallied Sci. 2024 Feb;16(Suppl 1):S393-S398. doi: 10.4103/jpbs.jpbs_616_23. Epub 2024 Feb 29. J Pharm Bioallied Sci. 2024. PMID: 38595413 Free PMC article. - Empirical Antibiotic Therapy for Ventilator-Associated Pneumonia.
Swanson JM, Wells DL. Swanson JM, et al. Antibiotics (Basel). 2013 Jul 4;2(3):339-51. doi: 10.3390/antibiotics2030339. Antibiotics (Basel). 2013. PMID: 27029307 Free PMC article. Review. - De-escalation, adequacy of antibiotic therapy and culture positivity in septic patients: an observational study.
Moraes RB, Guillén JA, Zabaleta WJ, Borges FK. Moraes RB, et al. Rev Bras Ter Intensiva. 2016 Sep;28(3):315-322. doi: 10.5935/0103-507X.20160044. Epub 2016 Sep 9. Rev Bras Ter Intensiva. 2016. PMID: 27626951 Free PMC article. - Assessment of De-Escalation of Empirical Antimicrobial Therapy in Medical Wards with Recognized Prevalence of Multi-Drug-Resistant Pathogens: A Multicenter Prospective Cohort Study in Non-ICU Patients with Microbiologically Documented Infection.
Rapti V, Poulakou G, Mousouli A, Kakasis A, Pagoni S, Pechlivanidou E, Masgala A, Sympardi S, Apostolopoulos V, Giannopoulos C, Alexiou N, Arvaniti K, Trakatelli C, Prionas A, Samarkos M, Daikos GL, Giamarellou H. Rapti V, et al. Antibiotics (Basel). 2024 Aug 27;13(9):812. doi: 10.3390/antibiotics13090812. Antibiotics (Basel). 2024. PMID: 39334987 Free PMC article.
References
- Rello J, Gallego M, Mariscal D, Sonora R, Valles J. The value of routine microbial investigation in ventilator-associated pneumonia. Am J Respir Crit Care Med. 1997;156:196–200. - PubMed
- Luna CM, Vujacich P, Niederman MS, Vay C, Gherardi C, Matera J, Jolly EC. Impact of BAL data on the therapy and outcome of ventilator-associated pneumonia. Chest. 1997;111:676–685. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous