CNS immune privilege: hiding in plain sight - PubMed (original) (raw)
Review
CNS immune privilege: hiding in plain sight
Monica J Carson et al. Immunol Rev. 2006 Oct.
Abstract
Central nervous system (CNS) immune privilege is an experimentally defined phenomenon. Tissues that are rapidly rejected by the immune system when grafted in sites, such as the skin, show prolonged survival when grafted into the CNS. Initially, CNS immune privilege was construed as CNS isolation from the immune system by the blood-brain barrier (BBB), the lack of draining lymphatics, and the apparent immunoincompetence of microglia, the resident CNS macrophage. CNS autoimmunity and neurodegeneration were presumed automatic consequences of immune cell encounter with CNS antigens. Recent data have dramatically altered this viewpoint by revealing that the CNS is neither isolated nor passive in its interactions with the immune system. Peripheral immune cells can cross the intact BBB, CNS neurons and glia actively regulate macrophage and lymphocyte responses, and microglia are immunocompetent but differ from other macrophage/dendritic cells in their ability to direct neuroprotective lymphocyte responses. This newer view of CNS immune privilege is opening the door for therapies designed to harness autoreactive lymphocyte responses and also implies (i) that CNS autoimmune diseases (i.e. multiple sclerosis) may result as much from neuronal and/or glial dysfunction as from immune system dysfunctions and (ii) that the severe neuronal and glial dysfunction associated with neurodegenerative disorders (i.e. Alzheimer's disease) likely alters CNS-specific regulation of lymphocyte responses affecting the utility of immune-based therapies (i.e. vaccines).
Figures
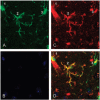
Fig. 1
Microglial morphology is an inaccurate predictor of juxtaposition with cerebrovasculature. (A) Three apparently stellate Iba-1+cells in the CNS of a healthy adult mouse are identified in green. (B) All nuclei in the same tissue section are identified in blue with DAPI. (C) All myeloid cells and blood vessels are identified in red with tomato lectin. (D) Merged images of all three panels illustrates close juxtaposition of cell 1 but not that of cells 2 and 3 with blood vessels. Confocal images were taken using a Zeiss. A rotating three-dimensional image is provided online as Supplemental Movie 1.
Fig. 2. The genotype of resident microglia and peripheral immune cells can be differentially manipulated using irradiation bone marrow chimeric methodology.
(A) Rodents receive whole-body irradiation sufficient to kill the adult bone marrow stem cell population. (B) To survive, irradiated rodents must receive bone marrow from a donor. The genotype of the donor and recipient can differ. (C) The donor bone marrow contributes to the repopulation of the peripheral immune system but not to that of most the CNS myeloid population (see text for discussion).
Similar articles
- The movers and shapers in immune privilege of the CNS.
Engelhardt B, Vajkoczy P, Weller RO. Engelhardt B, et al. Nat Immunol. 2017 Feb;18(2):123-131. doi: 10.1038/ni.3666. Epub 2017 Jan 16. Nat Immunol. 2017. PMID: 28092374 Review. - Immune privilege and HIV-1 persistence in the CNS.
Persidsky Y, Poluektova L. Persidsky Y, et al. Immunol Rev. 2006 Oct;213:180-94. doi: 10.1111/j.1600-065X.2006.00440.x. Immunol Rev. 2006. PMID: 16972904 Review. - Antigen-presenting cell diversity for T cell reactivation in central nervous system autoimmunity.
Waisman A, Johann L. Waisman A, et al. J Mol Med (Berl). 2018 Dec;96(12):1279-1292. doi: 10.1007/s00109-018-1709-7. Epub 2018 Nov 1. J Mol Med (Berl). 2018. PMID: 30386908 Review. - Balancing function vs. self defense: the CNS as an active regulator of immune responses.
Carson MJ, Sutcliffe JG. Carson MJ, et al. J Neurosci Res. 1999 Jan 1;55(1):1-8. doi: 10.1002/(SICI)1097-4547(19990101)55:1<1::AID-JNR1>3.0.CO;2-9. J Neurosci Res. 1999. PMID: 9890428 Review. - The role of microglia in central nervous system immunity and glioma immunology.
Yang I, Han SJ, Kaur G, Crane C, Parsa AT. Yang I, et al. J Clin Neurosci. 2010 Jan;17(1):6-10. doi: 10.1016/j.jocn.2009.05.006. Epub 2009 Nov 18. J Clin Neurosci. 2010. PMID: 19926287 Free PMC article. Review.
Cited by
- Computational modeling of tuberculous meningitis reveals an important role for tumor necrosis factor-α.
El-Kebir M, van der Kuip M, van Furth AM, Kirschner DE. El-Kebir M, et al. J Theor Biol. 2013 Jul 7;328:43-53. doi: 10.1016/j.jtbi.2013.03.008. Epub 2013 Mar 26. J Theor Biol. 2013. PMID: 23542051 Free PMC article. - Neuroimmune crosstalk in the central nervous system and its significance for neurological diseases.
Tian L, Ma L, Kaarela T, Li Z. Tian L, et al. J Neuroinflammation. 2012 Jul 2;9:155. doi: 10.1186/1742-2094-9-155. J Neuroinflammation. 2012. PMID: 22747919 Free PMC article. Review. - Radiotherapy and Systemic Treatment for Leptomeningeal Disease.
Frechette KM, Breen WG, Brown PD, Sener UT, Webb LM, Routman DM, Laack NN, Mahajan A, Lehrer EJ. Frechette KM, et al. Biomedicines. 2024 Aug 7;12(8):1792. doi: 10.3390/biomedicines12081792. Biomedicines. 2024. PMID: 39200256 Free PMC article. Review. - Nestin-GFP transgene labels immunoprivileged bone marrow mesenchymal stem cells in the model of ectopic foci formation.
Karpenko D, Kapranov N, Bigildeev A. Karpenko D, et al. Front Cell Dev Biol. 2022 Sep 5;10:993056. doi: 10.3389/fcell.2022.993056. eCollection 2022. Front Cell Dev Biol. 2022. PMID: 36133916 Free PMC article. - Review: microglia of the aged brain: primed to be activated and resistant to regulation.
Norden DM, Godbout JP. Norden DM, et al. Neuropathol Appl Neurobiol. 2013 Feb;39(1):19-34. doi: 10.1111/j.1365-2990.2012.01306.x. Neuropathol Appl Neurobiol. 2013. PMID: 23039106 Free PMC article. Review.
References
- Lo D, et al. Integrating innate and adaptive immunity in the whole animal. Immunol Rev. 1999;169:225–239. - PubMed
- Grigoriadis N, Grigoriadis S, Polyzoidou E, Milonas I, Karussis D. Neuroinflammation in multiple sclerosis: evidence for autoimmune dysregulation, not simple autoimmune reaction. Clin Neurol Neurosurg. 2006;108:241–244. - PubMed
- Elward K, Gasque P. “Eat me” and “don't eat me” signals govern the innate immune response and tissue repair in the CNS: emphasis on the critical role of the complement system. Mol Immunol. 2003;40:85–94. - PubMed
- Rosenberg GA. Matrix metalloproteinases in neuroinflammation. Glia. 2002;39:279–291. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources