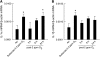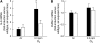Type I interleukin-1 receptor is required for pulmonary responses to subacute ozone exposure in mice - PubMed (original) (raw)
Type I interleukin-1 receptor is required for pulmonary responses to subacute ozone exposure in mice
Richard A Johnston et al. Am J Respir Cell Mol Biol. 2007 Oct.
Abstract
Interleukin (IL)-1, a proinflammatory cytokine, is expressed in the lung after ozone (O(3)) exposure. IL-1 mediates its effects through the type I IL-1 receptor (IL-1RI), the only signaling receptor for both IL-1alpha and IL-1beta. The purpose of this study was to determine the role of IL-1RI in pulmonary responses to O(3.) To that end, wild-type, C57BL/6 (IL-1RI(+/+)) mice and IL-1RI-deficient (IL-1RI(-/-)) mice were exposed to O(3) either subacutely (0.3 ppm for 72 h) or acutely (2 ppm for 3 h). Subacute O(3) exposure increased bronchoalveolar lavage fluid (BALF) protein, interferon-gamma-inducible protein (IP)-10, soluble tumor necrosis factor receptor 1 (sTNFR1), and neutrophils in IL-1RI(+/+) and IL-1RI(-/-) mice. With the exception of IP-10, all outcome indicators were reduced in IL-1RI(-/-) mice. Furthermore, subacute O(3) exposure increased IL-6 mRNA expression in IL-1RI(+/+), but not IL-1RI(-/-) mice. Acute (2 ppm) O(3) exposure increased BALF protein, IL-6, eotaxin, KC, macrophage inflammatory protein (MIP)-2, IP-10, monocyte chemotactic protein-1, sTNFR1, neutrophils, and epithelial cells in IL-1RI(+/+) and IL-1RI(-/-) mice. For IL-6, eotaxin, MIP-2, and sTNFR1, there were small but significant reductions of these outcome indicators in IL-1RI(-/-) versus IL-1RI(+/+) mice at 6 hours after exposure, but not at other time points, whereas other outcome indicators were unaffected by IL-1RI deficiency. These results suggest that IL-1RI is required for O(3)-induced pulmonary inflammation during subacute O(3) exposure, but plays a more minor role during acute O(3) exposure. In addition, these results suggest that the induction of IL-6 via IL-1RI may be important in mediating the effects of O(3) during subacute exposure.
Figures
**Figure 1.
(A) IL-1α and (B) IL-1β mRNA expression in lung tissue from room air– or O3-exposed wild-type (C57BL/6) mice. Lungs were harvested 30 minutes after cessation of exposure to 0.3 ppm O3 for 72 hours, or 3, 6, or 24 hours after cessation of exposure to 2 ppm O3 for 3 hours. Lungs from air-exposed controls were obtained at the same time. mRNA transcript copy number was normalized to β-actin transcript copy number. n = 7–13 mice for each group. *P < 0.05 compared with air-exposed controls.
**Figure 2.
The concentrations of protein, interferon-γ–inducible protein (IP)-10, soluble tumor necrosis factor receptor 1 (sTNFR1), as well as the total number of macrophages, neutrophils, and epithelial cells in the bronchoalveolar lavage fluid (BALF) of wild-type, C57BL/6 (IL-1RI+/+; solid bars) and IL-1RI–deficient (IL-1RI−/−; open bars) mice 30 minutes after the cessation of a 72-hour exposure to either room air or 0.3 ppm ozone (O3). n = 8–26 for each treatment group. *P < 0.05 compared with genotype-matched, air-exposed controls. #P < 0.05 compared with IL-1RI−/− mice within the same exposure group.
**Figure 3.
(A) IL-6 and (B) intercellular adhesion molecule (ICAM)-1 mRNA expression in lung tissue from room air– or O3-exposed, wild-type C57BL/6 (IL-1RI+/+; solid bars) and IL-1RI–deficient (IL-1RI−/−; open bars) mice. Lungs were harvested 30 minutes after cessation of exposure to 0.3 ppm O3 for 72 hours. Lungs from air-exposed controls were obtained at the same time. mRNA levels for each treatment group were normalized for 18S rRNA and expressed as the fold-induction of the values determined for air-exposed, wild-type C57BL/6 (IL-1RI+/+) mice. n = 8–10 mice for each group. *P < 0.05 compared with air-exposed controls.
**Figure 4.
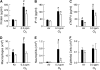
The concentrations of protein, IL-6, eotaxin, KC, macrophage inflammatory protein (MIP)-2, IP-10, MCP-1, and sTNFR1 in the BALF of wild-type, C57BL/6 (IL-1RI+/+; solid bars) and IL-1RI–deficient (IL-1RI−/−; open bars) mice 3, 6, or 24 hours after the cessation of a 3-hour exposure to either room air or 2 ppm ozone (O3). The concentrations of BALF protein, IP-10, and sTNFR1 from air-exposed mice are identical to those found in Figure 2 and are included here to demonstrate the effect of O3 on our outcome indicators. n = 5–26 for each treatment group. *P < 0.05 compared with genotype-matched, air-exposed controls. #P < 0.05 compared with IL-1RI−/− mice within the same exposure group.
**Figure 5.
The total number of macrophages, neutrophils, and epithelial cells in the BALF of wild-type, C57BL/6 (IL-1RI+/+; solid bars) and IL-1RI–deficient (IL-1RI−/−; open bars) mice 3, 6, or 24 hours after the cessation of a 3-hour exposure to either room air or 2 ppm ozone (O3). The data shown here from air-exposed mice are identical to those found in Figure 2 and are included here to demonstrate the effect of O3 on our outcome indicators. n = 8–26 for each treatment group. *P < 0.05 compared with genotype-matched, air-exposed controls. #P < 0.05 compared with IL-1RI−/− mice within the same exposure group.
References
- Goss CH, Newsom SA, Schildcrout JS, Sheppard L, Kaufman JD. Effect of ambient air pollution on pulmonary exacerbations and lung function in cystic fibrosis. Am J Respir Crit Care Med 2004;169:816–821. -PubMed
- Tolbert PE, Mulholland JA, MacIntosh DL, Xu F, Daniels D, Devine OJ, Carlin BP, Klein M, Dorley J, Butler AJ, et al. Air quality and pediatric emergency room visits for asthma in Atlanta, Georgia, USA. Am J Epidemiol 2000;151:798–810. -PubMed
- O'Neill MS, Loomis D, Borja-Aburto VH. Ozone, area social conditions, and mortality in Mexico City. Environ Res 2004;94:234–242. -PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Research Materials