Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies - PubMed (original) (raw)
Review
Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies
M R Law et al. BMJ. 2009.
Abstract
Objectives: To determine the quantitative efficacy of different classes of blood pressure lowering drugs in preventing coronary heart disease (CHD) and stroke, and who should receive treatment.
Design: Meta-analysis. Data source Medline (1966-2007).
Study selection: Randomised trials of blood pressure lowering drugs recording CHD events and strokes. 108 trials studied differences in blood pressure between study drug and placebo (or control group not receiving the study drug) ("blood pressure difference trials"), and 46 trials compared drugs ("drug comparison trials"). Seven trials with three randomised groups fell into both categories. The results were interpreted in the context of those expected from the largest published meta-analysis of cohort studies, totalling 958 000 people.
Participants: 464 000 people defined into three mutually exclusive categories: participants with no history of vascular disease, a history of CHD, or a history of stroke.
Results: In the blood pressure difference trials beta blockers had a special effect over and above that due to blood pressure reduction in preventing recurrent CHD events in people with a history of CHD: risk reduction 29% (95% confidence interval 22% to 34%) compared with 15% (11% to 19%) in trials of other drugs. The extra effect was limited to a few years after myocardial infarction, with a risk reduction of 31% compared with 13% in people with CHD with no recent infarct (P=0.04). In the other blood pressure difference trials (excluding CHD events in trials of beta blockers in people with CHD), there was a 22% reduction in CHD events (17% to 27%) and a 41% (33% to 48%) reduction in stroke for a blood pressure reduction of 10 mm Hg systolic or 5 mm Hg diastolic, similar to the reductions of 25% (CHD) and 36% (stroke) expected for the same difference in blood pressure from the cohort study meta-analysis, indicating that the benefit is explained by blood pressure reduction itself. The five main classes of blood pressure lowering drugs (thiazides, beta blockers, angiotensin converting enzyme inhibitors, angiotensin receptor blockers, and calcium channel blockers) were similarly effective (within a few percentage points) in preventing CHD events and strokes, with the exception that calcium channel blockers had a greater preventive effect on stroke (relative risk 0.92, 95% confidence interval 0.85 to 0.98). The percentage reductions in CHD events and stroke were similar in people with and without cardiovascular disease and regardless of blood pressure before treatment (down to 110 mm Hg systolic and 70 mm Hg diastolic). Combining our results with those from two other studies (the meta-analyses of blood pressure cohort studies and of trials determining the blood pressure lowering effects of drugs according to dose) showed that in people aged 60-69 with a diastolic blood pressure before treatment of 90 mm Hg, three drugs at half standard dose in combination reduced the risk of CHD by an estimated 46% and of stroke by 62%; one drug at standard dose had about half this effect. The present meta-analysis also showed that drugs other than calcium channel blockers (with the exception of non-cardioselective beta blockers) reduced the incidence of heart failure by 24% (19% to 28%) and calcium channel blockers by 19% (6% to 31%).
Conclusions: With the exception of the extra protective effect of beta blockers given shortly after a myocardial infarction and the minor additional effect of calcium channel blockers in preventing stroke, all the classes of blood pressure lowering drugs have a similar effect in reducing CHD events and stroke for a given reduction in blood pressure so excluding material pleiotropic effects. The proportional reduction in cardiovascular disease events was the same or similar regardless of pretreatment blood pressure and the presence or absence of existing cardiovascular disease. Guidelines on the use of blood pressure lowering drugs can be simplified so that drugs are offered to people with all levels of blood pressure. Our results indicate the importance of lowering blood pressure in everyone over a certain age, rather than measuring it in everyone and treating it in some.
Conflict of interest statement
Competing interests: MRL and NJW hold patents (granted and pending) on the formulation of a combined pill to simultaneously reduce four cardiovascular risk factors, including blood pressure.
Figures
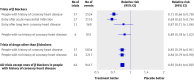
Fig 1 Relative risk estimates of coronary heart disease events in single drug blood pressure difference trials according to drug (β blockers or other), presence of CHD, and for β blockers according to acute myocardial infarction on entry. (Totals are less than the sum of the individual categories because some trials include more than one category; see web extra figures 1a-e for individual trial results and summary estimates)
Fig 2 Relative risk estimates of coronary heart disease events and stroke for a blood pressure reduction of 10 mm Hg systolic or 5 mm Hg diastolic in the blood pressure difference trials and in epidemiological cohort studies. (Total number of trials is fewer than the sum of the three categories as five included participants with and without vascular disease; see web extra figures 2a-f for individual trial results and summary estimates)
Fig 3 Relative risk estimates of coronary heart disease events and stroke in single drug blood pressure difference trials according to class of drug (excluding CHD events in trials of β blockers in people with history of coronary heart disease). (Totals are less than the sum of the individual categories because some trials include more than one category; see web extra figures 3a-i for individual trial results and summary estimates)
Fig 4 Relative risk estimates of coronary heart disease events and stroke in 46 drug comparison trials comparing each of the five classes of blood pressure lowering drug with any other class of drug (excluding CHD events in trials of β blockers in people with a history of coronary heart disease; see web extra figures 4a-j for individual trial results and summary estimates)
Fig 5 Relative risk estimates of coronary heart disease events and stroke in blood pressure difference trials according to pretreatment diastolic and systolic blood pressures (taken as average in placebo group over course of trial). (Totals are less than the sum of the individual categories because some trials include more than one category; see web extra figures 5a-l and 6a-m for individual trial results and summary estimates)
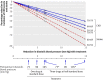
Fig 6 Reduction in incidence of coronary heart disease (CHD) events and stroke in relation to reduction in diastolic blood pressure according to drug dose, number of drugs, pretreatment diastolic blood pressure, and age. *Blood pressure reductions are more uncertain and hence also reductions in disease incidence
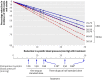
Fig 7 Reduction in incidence of coronary heart disease (CHD) events and stroke in relation to reduction in systolic blood pressure according to dose and combination of drugs, pretreatment systolic blood pressure, and age. *Blood pressure reductions are more uncertain and hence also reductions in disease incidence
Comment in
- Management of blood pressure in primary care.
McManus RJ, Mant J. McManus RJ, et al. BMJ. 2009 May 19;338:b940. doi: 10.1136/bmj.b940. BMJ. 2009. PMID: 19454748 No abstract available. - Drug prevention of hypertension. Law's flaw?
Lewis LS. Lewis LS. BMJ. 2009 Jun 29;338:b2596. doi: 10.1136/bmj.b2596. BMJ. 2009. PMID: 19564181 No abstract available. - Drug prevention of hypertension. All cause absolute benefit?
Bower P. Bower P. BMJ. 2009 Jun 29;338:b2597. doi: 10.1136/bmj.b2597. BMJ. 2009. PMID: 19564182 No abstract available. - Drug prevention of hypertension. Assumptions and extrapolation.
Bangalore S, Messerli FH. Bangalore S, et al. BMJ. 2009 Jun 29;338:b2600. doi: 10.1136/bmj.b2600. BMJ. 2009. PMID: 19564184 No abstract available. - Drug prevention of hypertension. Up to a point.
Schachter M. Schachter M. BMJ. 2009 Jun 29;338:b2601. doi: 10.1136/bmj.b2601. BMJ. 2009. PMID: 19564185 No abstract available. - Blood pressure in primary care. Home monitoring, a way to go?
Calinas-Correia J. Calinas-Correia J. BMJ. 2009 Jun 29;338:b2623. doi: 10.1136/bmj.b2623. BMJ. 2009. PMID: 19564186 No abstract available. - Drug prevention of hypertension. Contradicting Cochrane.
O'Connor RF, Moloney R. O'Connor RF, et al. BMJ. 2009 Sep 29;339:b3997. doi: 10.1136/bmj.b3997. BMJ. 2009. PMID: 19808827 No abstract available. - Blood pressure-lowering drugs in preventing cardiovascular disease.
Giles TD. Giles TD. Curr Cardiol Rep. 2009 Nov;11(6):399-400. doi: 10.1007/s11886-009-0057-1. Curr Cardiol Rep. 2009. PMID: 19863862 No abstract available. - [Are blood-pressure lowering drugs useful for preventing cardiovascular disease, and if so, in whom?].
Delgado Córdoba M, García López F. Delgado Córdoba M, et al. Nefrologia. 2009;29(6 Suppl):27-9. doi: 10.3265/NEFROLOGIA.2009.29.S.E.noID.36.free. Nefrologia. 2009. PMID: 20221220 Spanish. No abstract available.
Similar articles
- First-line diuretics versus other classes of antihypertensive drugs for hypertension.
Reinhart M, Puil L, Salzwedel DM, Wright JM. Reinhart M, et al. Cochrane Database Syst Rev. 2023 Jul 13;7(7):CD008161. doi: 10.1002/14651858.CD008161.pub3. Cochrane Database Syst Rev. 2023. PMID: 37439548 Free PMC article. Review. - Lowering blood pressure to prevent myocardial infarction and stroke: a new preventive strategy.
Law M, Wald N, Morris J. Law M, et al. Health Technol Assess. 2003;7(31):1-94. doi: 10.3310/hta7310. Health Technol Assess. 2003. PMID: 14604498 Review. - Value of low dose combination treatment with blood pressure lowering drugs: analysis of 354 randomised trials.
Law MR, Wald NJ, Morris JK, Jordan RE. Law MR, et al. BMJ. 2003 Jun 28;326(7404):1427. doi: 10.1136/bmj.326.7404.1427. BMJ. 2003. PMID: 12829555 Free PMC article. - Pharmacological interventions for hypertension in children.
Chaturvedi S, Lipszyc DH, Licht C, Craig JC, Parekh R. Chaturvedi S, et al. Evid Based Child Health. 2014 Sep;9(3):498-580. doi: 10.1002/ebch.1974. Evid Based Child Health. 2014. PMID: 25236305 Review. - Cochrane in context: pharmacological interventions for hypertension in children.
Chaturvedi S, Lipszyc DH, Licht C, Craig JC, Parekh RS. Chaturvedi S, et al. Evid Based Child Health. 2014 Sep;9(3):581-3. doi: 10.1002/ebch.1975. Evid Based Child Health. 2014. PMID: 25236306 Review.
Cited by
- Association between blood pressure multi-trajectory and cardiovascular disease among a Chinese elderly medical examination population.
Chen Q, Du J, Hong X. Chen Q, et al. Front Cardiovasc Med. 2024 Jul 24;11:1363266. doi: 10.3389/fcvm.2024.1363266. eCollection 2024. Front Cardiovasc Med. 2024. PMID: 39114559 Free PMC article. - Blood pressure evaluation and review of antihypertensive medication in patients with life limiting illness.
Dewhurst F, Baker L, Andrew I, Todd A. Dewhurst F, et al. Int J Clin Pharm. 2016 Oct;38(5):1044-7. doi: 10.1007/s11096-016-0327-0. Epub 2016 Jun 24. Int J Clin Pharm. 2016. PMID: 27343121 - Efficacy of Exercise Intervention for Weight Loss in Overweight and Obese Adolescents: Meta-Analysis and Implications.
Stoner L, Rowlands D, Morrison A, Credeur D, Hamlin M, Gaffney K, Lambrick D, Matheson A. Stoner L, et al. Sports Med. 2016 Nov;46(11):1737-1751. doi: 10.1007/s40279-016-0537-6. Sports Med. 2016. PMID: 27139723 Review. - Simulating Strategies for Improving Control of Hypertension Among Patients with Usual Source of Care in the United States: The Blood Pressure Control Model.
Fontil V, Bibbins-Domingo K, Kazi DS, Sidney S, Coxson PG, Khanna R, Victor RG, Pletcher MJ. Fontil V, et al. J Gen Intern Med. 2015 Aug;30(8):1147-55. doi: 10.1007/s11606-015-3231-8. Epub 2015 Mar 7. J Gen Intern Med. 2015. PMID: 25749880 Free PMC article. - Olmesartan/amlodipine/hydrochlorothiazide in participants with hypertension and diabetes, chronic kidney disease, or chronic cardiovascular disease: a subanalysis of the multicenter, randomized, double-blind, parallel-group TRINITY study.
Kereiakes DJ, Chrysant SG, Izzo JL Jr, Littlejohn T 3rd, Melino M, Lee J, Fernandez V, Heyrman R. Kereiakes DJ, et al. Cardiovasc Diabetol. 2012 Oct 30;11:134. doi: 10.1186/1475-2840-11-134. Cardiovasc Diabetol. 2012. PMID: 23110471 Free PMC article. Clinical Trial.
References
- Psaty BM, Lumley T, Furberg CD, Schellenbaum G, Pahor M, Alderman MH, et al. Health outcomes associated with various antihypertensive therapies used as first-line agents: a network meta-analysis. JAMA 2003;289:2534-44. - PubMed
- Kendall MJ, Lynch KP, Hjalmarson Å, Kjekshus J. β-blockers and sudden cardiac death. Ann Intern Med 1995;123:358-67. - PubMed
- Blood Pressure Lowering Treatment Trialists’ Collaboration. Effects of different blood pressure-lowering regimens on major cardiovascular events in individuals with and without diabetes mellitus. Arch Intern Med 2005;165:1410-9. - PubMed
- Blood Pressure Lowering Treatment Trialists’ Collaboration. Effects of different blood-pressure-lowering regimens on major cardiovascular events: results of prospectively-designed overviews of randomised trials. Lancet 2003;362:1527-35. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical