Clinical outcome of patients with epistaxis treated with nasal packing after hospital discharge - PubMed (original) (raw)
Clinical outcome of patients with epistaxis treated with nasal packing after hospital discharge
Marina Faistauer et al. Braz J Otorhinolaryngol. 2009 Nov-Dec.
Abstract
Epistaxis is a common clinical condition and in most public hospitals these patients received nasal packing and were admitted to the hospital as initial management strategies. However, little is known about the follow-up of these patients after they leave the hospital.
Aim: To identify the clinical outcome of patients treated for epistaxis following discharge.
Materials and methods: We analyzed the results of questionnaires from patients hospitalized for non-traumatic epistaxis between March 2006 and March 2007.
Study design: Cohort longitudinal.
Results: Fifty-four of eighty-seven patients answered (62%). Epistaxis recurred in 37% of the patients. Of the patients who had recurrent bleeding, 70% were hypertensive, 35% were chronic users of acetylsalicylic acid, and 55% used tobacco. Forty per cent of the recurrences occurred in the first week after discharge, and fifty per cent needed to return to the emergency room. Seventy per cent of those who returned to the emergency room required a second treatment.
Conclusions: Recurrence after epistaxis treatment is common and may occur soon after the initial discharge. Although our sample was small, this data suggests the need for a reevaluation of the current treatment mode of patients with epistaxis in the emergency rooms of public hospitals.
Figures
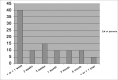
Graph 1
Time span between hospital discharge and the first episode of recurrence in the sample patients.
Similar articles
- Clinical Practice Guideline: Nosebleed (Epistaxis).
Tunkel DE, Anne S, Payne SC, Ishman SL, Rosenfeld RM, Abramson PJ, Alikhaani JD, Benoit MM, Bercovitz RS, Brown MD, Chernobilsky B, Feldstein DA, Hackell JM, Holbrook EH, Holdsworth SM, Lin KW, Lind MM, Poetker DM, Riley CA, Schneider JS, Seidman MD, Vadlamudi V, Valdez TA, Nnacheta LC, Monjur TM. Tunkel DE, et al. Otolaryngol Head Neck Surg. 2020 Jan;162(1_suppl):S1-S38. doi: 10.1177/0194599819890327. Otolaryngol Head Neck Surg. 2020. PMID: 31910111 - Recent trends in epistaxis management in the United States: 2008-2010.
Villwock JA, Jones K. Villwock JA, et al. JAMA Otolaryngol Head Neck Surg. 2013 Dec;139(12):1279-84. doi: 10.1001/jamaoto.2013.5220. JAMA Otolaryngol Head Neck Surg. 2013. PMID: 24136624 Review. - Clinical Practice Guideline: Nosebleed (Epistaxis) Executive Summary.
Tunkel DE, Anne S, Payne SC, Ishman SL, Rosenfeld RM, Abramson PJ, Alikhaani JD, Benoit MM, Bercovitz RS, Brown MD, Chernobilsky B, Feldstein DA, Hackell JM, Holbrook EH, Holdsworth SM, Lin KW, Lind MM, Poetker DM, Riley CA, Schneider JS, Seidman MD, Vadlamudi V, Valdez TA, Nnacheta LC, Monjur TM. Tunkel DE, et al. Otolaryngol Head Neck Surg. 2020 Jan;162(1):8-25. doi: 10.1177/0194599819889955. Otolaryngol Head Neck Surg. 2020. PMID: 31910122 Review. - The role of surgical audit in improving patient management; nasal haemorrhage: an audit study.
Upile T, Jerjes W, Sipaul F, El Maaytah M, Nouraei SA, Singh S, Hopper C, Wright A. Upile T, et al. BMC Surg. 2007 Sep 13;7:19. doi: 10.1186/1471-2482-7-19. BMC Surg. 2007. PMID: 17854499 Free PMC article. - Do all epistaxis patients with a nasal pack need admission? A retrospective study of 116 patients managed in accident and emergency according to a peer reviewed protocol.
Van Wyk FC, Massey S, Worley G, Brady S. Van Wyk FC, et al. J Laryngol Otol. 2007 Mar;121(3):222-7. doi: 10.1017/S0022215106003148. Epub 2006 Oct 11. J Laryngol Otol. 2007. PMID: 17040607
Cited by
- Parents' knowledge regarding first-aid management of epistaxis in children in Taif, Saudi Arabia.
Alam BS, Jawhari AM, Aljuaid AS, Althomali MA, AlMutairi BS, Alobaylan HA, Alosaimi SM. Alam BS, et al. J Family Med Prim Care. 2023 May;12(5):940-945. doi: 10.4103/jfmpc.jfmpc_1925_22. Epub 2023 May 31. J Family Med Prim Care. 2023. PMID: 37448931 Free PMC article. - Knowledge and awareness of the Saudi general public toward epistaxis: a cross-sectional study.
Assiri AM. Assiri AM. Front Public Health. 2024 May 27;12:1269559. doi: 10.3389/fpubh.2024.1269559. eCollection 2024. Front Public Health. 2024. PMID: 38859901 Free PMC article. - [Clinical management of epistaxis].
Uhler L, Knipping S. Uhler L, et al. HNO. 2019 May;67(5):366-372. doi: 10.1007/s00106-018-0526-1. HNO. 2019. PMID: 29915939 German. - A Systematic Review and Meta-Analysis of the Awareness of and Attitudes Toward Epistaxis.
Alkhalifah KM, Alhumaidan NI, Alotaibi TA, Almnjwami RFM, Alzelfawi LA, Almughamsi RH, Alqahtani RK, Aldossari MH, Fageeh YA. Alkhalifah KM, et al. Cureus. 2023 Oct 6;15(10):e46590. doi: 10.7759/cureus.46590. eCollection 2023 Oct. Cureus. 2023. PMID: 37933345 Free PMC article. Review. - Awareness of First-Aid Management of Epistaxis Among Individuals in Al-Ahsa Region.
Alkhalaf HA, Alshoug ST, Memon AQ. Alkhalaf HA, et al. Cureus. 2024 Feb 21;16(2):e54625. doi: 10.7759/cureus.54625. eCollection 2024 Feb. Cureus. 2024. PMID: 38524033 Free PMC article.
References
- Santos R, Leonhardt F, Ferri R, Gregório L. Ligadura endoscópica endonasal da artéria esfenopalatina para epistaxe severa. Rev Bras Otorrinolaringol. 2002;68:511–514.
- Roithmann R. Rotinas em pronto socorro. Artmed; Porto Alegre: 2006. Epistaxe; pp. 557–563.
- Santos R, Cedin AC. Epistaxe em Pediatria. Sociedade Brasileira de Rinologia e Cirurgia Plástica da Face 2005.
- Herkner H, Havel C, Müllner M, Gamper G, Bur A, Temmel A, et al. Active epistaxis at ED presentation is associated with arterial hypertension. Am J Emerg Med. 2002;20:92–95. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources