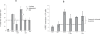Homologous recombination repair is essential for repair of vosaroxin-induced DNA double-strand breaks - PubMed (original) (raw)
Homologous recombination repair is essential for repair of vosaroxin-induced DNA double-strand breaks
Rachael Elizabeth Hawtin et al. Oncotarget. 2010 Nov.
Abstract
Vosaroxin (formerly voreloxin) is a first-in-class anticancer quinolone derivative that intercalates DNA and inhibits topoisomerase II, inducing site-selective double-strand breaks (DSB), G2 arrest and apoptosis. Objective responses and complete remissions were observed in phase 2 studies of vosaroxin in patients with solid and hematologic malignancies, and responses were seen in patients whose cancers were resistant to anthracyclines. The quinolone-based scaffold differentiates vosaroxin from the anthracyclines and anthracenediones, broadly used DNA intercalating topoisomerase II poisons. Here we report that vosaroxin induces a cell cycle specific pattern of DNA damage and repair that is distinct from the anthracycline, doxorubicin. Both drugs stall replication and preferentially induce DNA damage in replicating cells, with damage in G2 / M > S >> G1. However, detectable replication fork collapse, as evidenced by DNA fragmentation and long tract recombination during S phase, is induced only by doxorubicin. Furthermore, vosaroxin induces less overall DNA fragmentation. Homologous recombination repair (HRR) is critical for recovery from DNA damage induced by both agents, identifying the potential to clinically exploit synthetic lethality.
Conflict of interest statement
T. Helleday and C. Lundin received support from Sunesis Pharmaceuticals
R Hawtin, D. Stockett, O Wong, and J Fox were / are employees of Sunesis Pharmaceuticals.
Figures
Figure 1. Vosaroxin- and doxorubicin -induced DNA DSB are increased in replicating cells
The cell cycle dependence of vosaroxin-induced DNA damage was investigated using MO59K glioma cells which are large and highly adherent, and thus amenable to centrosome staining and analysis via immunofluorescence. Cells were treated for 6 hours with 1 or 9 μM vosaroxin (A) or 1 μM vosaroxin or 0.1 μM doxorubicin (B). Average γH2AX fluorescence intensity is displayed, with each symbol representing one cell. Cell cycle phases were established by analysis of centrosome size and number, and representative images are shown in Figure S1. The number of cells counted per phase is shown (n). Mean intensity is represented by horizontal line on the graph and listed below with standard error of the mean (SEM). Data are representative of three (vosaroxin) and two (doxorubicin) independent experiments.
Figure 2. Vosaroxin induces DNA fragmentation independent of DNA synthesis, in contrast with doxorubicin which induces S phase dependent and independent fragmentation
SPD8 cells were treated for 4 hr with 20 μM vosaroxin (V), 3 μM doxorubicin (DOX), 3 μM aphidicolin (Aph) or to vosaroxin or doxorubicin plus aphidicolin (+Aph) to arrest cells in S phase. Controls included 50 Gy of γ-irradiation (50 Gy) or DMSO only (Con). A) PFGE following 24 hr run. M = molecular markers. DNA fragment size is shown in Mbp. B) Luminescence intensity plots, in arbitrary units, showing data from vosaroxin treated cells +/− aphidicolin, doxorubicin treated cells +/− aphidicolin or an overlay of vosaroxin and doxorubicin treated cells with 50 Gy data included as positive control reference. A shift in the presence of aphidicolin indicates S phase dependent fragmentation. No difference was detected for vosaroxin +/− aphidicolin.
Figure 3. Vosaroxin and doxorubicin are cytotoxic both during and independent of DNA synthesis
SPD8 cells were exposed for 4 hr to 2 μM vosaroxin (V), 0.3 μM doxorubicin (DOX), 0.5 μM aphidicolin (Aph), or with vosaroxin or doxorubicin plus aphidicolin (+Aph) to arrest cells in S phase. Controls were treated with DMSO only (Con). Colony growth was evaluated after 7 days. Cloning efficiency is plotted as percent of untreated control. The graphic outlines the experimental approach, which is designed to identify S phase dependent and independent cytotoxicity. S phase independent toxicity (dotted bracket) is identified by the growth inhibition that occurred in the presence of S phase block. The S phase dependent toxicity (solid bracket) is determined by subtraction of S phase independent toxicity from overall toxicity. Both drugs demonstrate a component of S phase toxicity, however the majority of cytotoxicity is S phase independent. Data represent the mean of 3 independent experiments, error bars represent SEM.
Figure 4. Vosaroxin and doxorubicin induce HRR during and independent of DNA synthesis
A) Vosaroxin and doxorubicin trigger HRR during S phase. SPD8 cells were exposed for 4 hr to 2 μM vosaroxin (V), 0.3 μM doxorubicin (DOX), 0.5 μM aphidicolin (Aph), or with vosaroxin or doxorubicin plus aphidicolin (+Aph) to arrest cells in S phase. Controls were treated with DMSO only (C). The percent of cells with >9 RAD51 foci, representative of HRR activation, is plotted. The dashed horizontal line represents RAD51 foci induced by aphidicolin alone. Brackets represent the differential between vosaroxin or doxorubicin +/− aphidicolin (ie; vosaroxin alone minus vosaroxin + Aph). A decrease in the presence of Aph for both drugs indicates S phase dependent induction of RAD 51 foci. Data represent the mean of 3 independent experiments, error bars represent SEM. B) S phase block reduces doxorubicin-induced but not vosaroxin-induced long tract recombination. SPD8 cells were exposed for 4 hr to 2 μM vosaroxin (V), 0.3 μM doxorubicin (DOX), 0.5 μM aphidicolin (Aph), or with vosaroxin or doxorubicin plus aphidicolin (+Aph) to arrest cells in S phase. Controls were treated with DMSO only (C). The same population of treated cells were plated for cloning efficiency (Figure 3). Revertants / recombinants were selected by growth for 7 days in the presence of HAsT. The horizontal dashed line denotes reversion / recombination in the presence of aphicicolin control. To determine S phase dependent recombination events that are induced by each drug, the number of recombination events in the presence of drug + Aph are subtracted from the number of events with drug alone (ie; revertants with vosaroxin alone minus vosaroxin + Aph). No significant difference was detected for vosaroxin. A modest but significant difference was detected for doxorubicin (p=0.04). Data are plotted as revertants / 105 cells, and represent the mean of 3 independent experiments. Error bars represent SEM.
Figure 5. HRR compromised cells are sensitized to vosaroxin and doxorubicin
A) Vosaroxin and doxorubicin are more cytotoxic for RAD51D null cells. The matched cell lines RAD51D1 (RAD51D null) and RAD51D1.3 (matched, RAD51D reconstituted) were exposed to a dose-titration of vosaroxin, doxorubicin or DMSO control for 72 hr. Inhibition of proliferation is plotted as the percent of control. The mean IC50's for each drug in both cell lines, and the fold difference in sensitivity between lines, is tabulated. Loss of RAD51D increased sensitivity to both drugs. Data represent the mean of two independent experiments, error bars represent SEM. B) HRR compromised cells are unable to completely repair vosaroxin- and doxorubicin-induced DNA damage. RAD51D1 and RAD51D1.3 cells were treated for 6 hr with 0.11 μM vosaroxin, 1 μM doxorubicin, or with DMSO control, followed by washout and temporal evaluation of recovery from DNA damage, via quantification of γH2AX foci. DNA damage was evaluated upon compound removal (at 6 hr) and 16, 24 and 40 hr after washout. The graphs show the percent of cells at each time point with >5 γH2AX foci. Repair of DNA damage was compromised following treatment with each drug. Data represent the mean of 2 independent experiments, error bars represent SEM. Representative images are shown for each cell line at the time of compound removal and 24 hr following washout.
Figure 6. BRCA2 loss sensitizes cells to vosaroxin and doxorubicin
A) Cells expressing truncated BRCA2 are sensitized to vosaroxin more than doxorubicin. VC8 (mutant BRCA2) and VC8-B2 (restored BRCA2) cells were treated for 4 hr with a dose-titration of vosaroxin, doxorubicin, or with DMSO control. Inhibition of proliferation was evaluated following 5 days incubation and is represented as percent of DMSO control. Graphs represent the mean of 2 independent experiments and error bars represent SEM. The shift in IC50 between cell lines is shown for each compound. B) BRCA2 knockdown sensitizes cells equally to vosaroxin and doxorubicin. siRNA knockdown of BRCA2 was performed in U20S human sarcoma cells, followed by treatment with a dose-titration of vosaroxin or doxorubicin, or with DMSO control. Colony growth inhibition was evaluated following 14 days incubation and is graphed relative to DMSO control. Error bars represent SEM. The efficiency of knockdown at 24 and 48 hr post transfection, with BRCA2 siRNA or transfection agent alone (-) is shown. The shift in IC50 between conditions is shown for each compound.
Figure 7. Model for induction of differential, cell cycle phase specific DNA damage and HRR processes following exposure to vosaroxin or doxorubicin
DNA in G2 / M phase is shown on the left, with the replication fork advancing during S phase to the right. Points of homologous recombination are depicted by X, with the region exchanged depicted by the horizontal arrow. These regions also represent potential DNA fragments in the absence of DNA repair. A) Vosaroxin-induced DNA damage is depicted in the upper model, where the replication fork is stalled due to topologic stress in DNA, resulting in a prolonged S phase and the induction of RAD51 foci. Replication fork collapse is either below detectable levels or is absent, evidenced by undetectable DNA fragmentation or HRR-mediated long tract recombination during S phase. The toxicity of S phase induced lesions is low. In G2 / M phase, DNA DSB induction is maximal, inducing detectable DNA fragmentation, HRR-mediated long tract recombination and maximal toxicity. B) Doxorubicin-induced DNA damage is depicted in the lower model, where in addition to cleavable complexes base mutations, DNA cross-linking and DNA adducts are also generated. The advancing replication fork encounters torsional stress in the DNA and RAD51 foci are induced. A proportion of active replication forks collide with DNA lesions (shown here as a DNA adduct), inducing DNA fragmentation (represented by the horizontal arrows) and long tract recombination, indicating replication fork collapse. Sites for additional potential fork collapse are shown by the X, in regions of doxorubicin-DNA cross links and adducts. Fewer DNA DSB are formed in S phase than in G2 / M and cytotoxicity of the lesions is lower. In G2 / M phase, DNA DSB induction is maximal, resulting in increased DNA fragmentation, HRR-mediated long tract recombination and maximal toxicity. Because of the increased number and / or diversity of DNA interactions, DNA DSB induction and fragmentation is greater than that induced by vosaroxin, so generating an increased number of smaller (1.6 – 0.2 Mbp) fragments. This is represented by the increased number of, and smaller size of, the horizontal arrows.
Similar articles
- Voreloxin is an anticancer quinolone derivative that intercalates DNA and poisons topoisomerase II.
Hawtin RE, Stockett DE, Byl JA, McDowell RS, Nguyen T, Arkin MR, Conroy A, Yang W, Osheroff N, Fox JA. Hawtin RE, et al. PLoS One. 2010 Apr 15;5(4):e10186. doi: 10.1371/journal.pone.0010186. PLoS One. 2010. PMID: 20419121 Free PMC article. - The preclinical discovery of vosaroxin for the treatment of acute myeloid leukemia.
Paubelle E, Zylbersztejn F, Thomas X. Paubelle E, et al. Expert Opin Drug Discov. 2017 Jul;12(7):747-753. doi: 10.1080/17460441.2017.1331215. Epub 2017 May 22. Expert Opin Drug Discov. 2017. PMID: 28504025 Review. - Radiosensitization by the novel DNA intercalating agent vosaroxin.
Gordon IK, Graves C, Kil WJ, Kramp T, Tofilon P, Camphausen K. Gordon IK, et al. Radiat Oncol. 2012 Feb 27;7:26. doi: 10.1186/1748-717X-7-26. Radiat Oncol. 2012. PMID: 22369205 Free PMC article. - Homologous recombination is the principal pathway for the repair of DNA damage induced by tirapazamine in mammalian cells.
Evans JW, Chernikova SB, Kachnic LA, Banath JP, Sordet O, Delahoussaye YM, Treszezamsky A, Chon BH, Feng Z, Gu Y, Wilson WR, Pommier Y, Olive PL, Powell SN, Brown JM. Evans JW, et al. Cancer Res. 2008 Jan 1;68(1):257-65. doi: 10.1158/0008-5472.CAN-06-4497. Cancer Res. 2008. PMID: 18172318 - Molecular and Pharmacologic Properties of the Anticancer Quinolone Derivative Vosaroxin: A New Therapeutic Agent for Acute Myeloid Leukemia.
Jamieson GC, Fox JA, Poi M, Strickland SA. Jamieson GC, et al. Drugs. 2016 Sep;76(13):1245-1255. doi: 10.1007/s40265-016-0614-z. Drugs. 2016. PMID: 27484675 Free PMC article. Review.
Cited by
- Pleiotropic functions of EAPII/TTRAP/TDP2: cancer development, chemoresistance and beyond.
Li C, Sun SY, Khuri FR, Li R. Li C, et al. Cell Cycle. 2011 Oct 1;10(19):3274-83. doi: 10.4161/cc.10.19.17763. Epub 2011 Oct 1. Cell Cycle. 2011. PMID: 21926483 Free PMC article. Review. - Recent progress in targeting cancer.
Demidenko ZN, McCubrey JA. Demidenko ZN, et al. Aging (Albany NY). 2011 Dec;3(12):1154-62. doi: 10.18632/aging.100421. Aging (Albany NY). 2011. PMID: 22228887 Free PMC article. Review. - Effects of conditional depletion of topoisomerase II on cell cycle progression in mammalian cells.
Gonzalez RE, Lim CU, Cole K, Bianchini CH, Schools GP, Davis BE, Wada I, Roninson IB, Broude EV. Gonzalez RE, et al. Cell Cycle. 2011 Oct 15;10(20):3505-14. doi: 10.4161/cc.10.20.17778. Cell Cycle. 2011. PMID: 22067657 Free PMC article. - A dual role for A-type lamins in DNA double-strand break repair.
Redwood AB, Perkins SM, Vanderwaal RP, Feng Z, Biehl KJ, Gonzalez-Suarez I, Morgado-Palacin L, Shi W, Sage J, Roti-Roti JL, Stewart CL, Zhang J, Gonzalo S. Redwood AB, et al. Cell Cycle. 2011 Aug 1;10(15):2549-60. doi: 10.4161/cc.10.15.16531. Epub 2011 Aug 1. Cell Cycle. 2011. PMID: 21701264 Free PMC article. - Antiproliferative Activities of Lipophililic Fluoroquinolones- Based Scaffold Against a Panel of Solid and Liquid Cancer Cell Lines.
Qashou E, Al-Hiari Y, Kasabri V, AlBashiti R, AlAlawi S, Telfah A, AlHadid A. Qashou E, et al. Asian Pac J Cancer Prev. 2022 May 1;23(5):1529-1537. doi: 10.31557/APJCP.2022.23.5.1529. Asian Pac J Cancer Prev. 2022. PMID: 35633535 Free PMC article.
References
- Tomita K, Tsuzuki Y, Shibamori K, Tashima M, Kajikawa F, Sato Y, Kashimoto S, Chiba K, Katsuhiko H. Synthesis and Structure-Activity Relationships of Novel 7-Substituted 1,4-Dihydro-4-oxo-1-(2thiazolyl)-1,8-naphthyridine-3-carboxylic Acids as Antitumor Agents. Part1. J Med Chem. 2002;45:5564–75. - PubMed
- Tsuzuki Y, Tomita K, Shibamori K, Sato Y, Kashimoto S, Chiba K. Synthesis and structure-activity relationships of novel 7-substituted 1,4-dihydro-4-oxo-1-(2-thiazolyl)-1,8-naphthyridine-3-carboxylic acids as antitumor agents. Part 2. J Med Chem. 2004;47:2097–109. - PubMed
- Hoch U, Lynch J, Sato Y, Kashimoto S, Kajikawa F, Furutani Y, Silverman J. Voreloxin, formerly SNS-595, has potent activity against a broad panel of cancer cell lines and in vivo tumor models. Cancer Chemother Pharmacol. 2009;64:53–65. - PubMed
- Scatena C, Kumer J, Arbitrario J, Howlett A, Hawtin R, Fox J, Silverman J. Voreloxin, a first-in-class anticancer quinolone derivative, acts synergistically with cytarabine in vitro and induces bone marrow aplasia in vivo. Cancer Chemotherapy and Pharmaology. 2010 January 07 epub ahead of print. - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources