Ten-year course of borderline personality disorder: psychopathology and function from the Collaborative Longitudinal Personality Disorders study - PubMed (original) (raw)
Comparative Study
doi: 10.1001/archgenpsychiatry.2011.37. Epub 2011 Apr 4.
Robert L Stout, Thomas H McGlashan, M Tracie Shea, Leslie C Morey, Carlos M Grilo, Mary C Zanarini, Shirley Yen, John C Markowitz, Charles Sanislow, Emily Ansell, Anthony Pinto, Andrew E Skodol
Affiliations
- PMID: 21464343
- PMCID: PMC3158489
- DOI: 10.1001/archgenpsychiatry.2011.37
Comparative Study
Ten-year course of borderline personality disorder: psychopathology and function from the Collaborative Longitudinal Personality Disorders study
John G Gunderson et al. Arch Gen Psychiatry. 2011 Aug.
Abstract
Context: Borderline personality disorder (BPD) is traditionally considered chronic and intractable.
Objective: To compare the course of BPD's psychopathology and social function with that of other personality disorders and with major depressive disorder (MDD) over 10 years.
Design: A collaborative study of treatment-seeking, 18- to 45-year-old patients followed up with standardized, reliable, and repeated measures of diagnostic remission and relapse and of both global social functioning and subtypes of social functioning.
Setting: Nineteen clinical settings (hospital and outpatient) in 4 northeastern US cities.
Participants: Three study groups, including 175 patients with BPD, 312 with cluster C personality disorders, and 95 with MDD but no personality disorder.
Main outcome measures: The Diagnostic Interview for DSM-IV Personality Disorders and its follow-along version (the Diagnostic Interview for DSM-IV Personality Disorders-Follow-Along Version) were used to diagnose personality disorders and assess changes in them. The Structured Clinical Interview for DSM-IV Axis I Disorders and the Longitudinal Interval Follow-up Evaluation were used to diagnose MDD and assess changes in MDD and in social function.
Results: Eighty-five percent of patients with BPD remitted. Remission of BPD was slower than for MDD (P < .001) and minimally slower than for other personality disorders (P < .03). Twelve percent of patients with BPD relapsed, a rate less frequent and slower than for patients with MDD (P < .001) and other personality disorders (P = .008). All BPD criteria declined at similar rates. Social function scores showed severe impairment with only modest albeit statistically significant improvement; patients with BPD remained persistently more dysfunctional than the other 2 groups (P < .001). Reductions in criteria predicted subsequent improvements in DSM-IV Axis V Global Assessment of Functioning scores (P < .001).
Conclusions: The 10-year course of BPD is characterized by high rates of remission, low rates of relapse, and severe and persistent impairment in social functioning. These results inform expectations of patients, families, and clinicians and document the severe public health burden of this disorder.
Figures
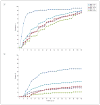
Figure 1
Diagnostic remission (A) and diagnostic relapse (B) of major depressive disorder (MDD), other personality disorders (OPD; either avoidant personality disorder [AVPD] or obsessive-compulsive personality disorder [OCPD]), and borderline personality disorder (BPD). Remission of MDD was based on a Psychiatric Status Rating of less than 2 for 2 consecutive months, and MDD relapse was based on a Psychiatric Status Rating of 5 or 6 for 2 consecutive months. Remission of OPD was defined as either fewer than 2 AVPD criteria for AVPD cases or fewer than 2 OCPD criteria for OCPD cases for 2 or 12 consecutive months, and OPD relapse was defined as returning to more than 4 criteria for 2 months or for either AVPD or OCPD cases separately. Remission of BPD was defined as fewer than 2 criteria for 2 or 12 consecutive months, and BPD relapse was defined as returning to more than 5 criteria for 2 months. Analyses were based on lifetest survival estimates.
Figure 2
Prevalence of borderline personality disorder criteria. Positive indicates the cases with a score of 2 (definitely present and clinically significant) for each of the 9 borderline personality disorder criteria on the Diagnostic Interview for DSM-IV Personality Disorders, assessed for the 2 years prior to the follow-up point.
Figure 3
Scores on the Global Assessment of Functioning (GAF) (A) and the Global Social Adjustment (GSA) scale (B). A, A score of 100 represents the best level of overall functioning, and a score of 0 represents the lowest level. B, A score of 0 represents the highest level of social functioning, and a score of 5 represents the lowest level. MDD indicates major depressive disorder; OPD, other personality disorders; and BPD, borderline personality disorder.
Figure 4
Functional remission, defined as a Global Assessment of Functioning score greater than 70 sustained for 2 months. Analyses were conducted using lifetest survival estimates. MDD indicates major depressive disorder; OPD, other personality disorders; and BPD, borderline personality disorder.
References
- Grilo CM, McGlashan TH, Oldham JM. Course and stability of personality disorders. J Pract Psychiatry Behav Health. 1998;1(4):61–75.
- Robins E, Guze SB. Establishment of diagnostic validity in psychiatric illness: its application to schizophrenia. Am J Psychiatry. 1970;126(7):983–987. -PubMed
- Gunderson JG, Shea MT, Skodol AE, McGlashan TH, Morey LC, Stout RL, Zanarini MC, Grilo CM, Oldham JM, Keller MB. The Collaborative Longitudinal Personality Disorders Study: development, aims, design, and sample characteristics. J Pers Disord. 2000;14(4):300–315. -PubMed
Publication types
MeSH terms
Grants and funding
- K05 MH001654/MH/NIMH NIH HHS/United States
- K23 MH080221/MH/NIMH NIH HHS/United States
- R01 MH 01654/MH/NIMH NIH HHS/United States
- R01 MH050838/MH/NIMH NIH HHS/United States
- K23 MH073708/MH/NIMH NIH HHS/United States
- R01 MH050837/MH/NIMH NIH HHS/United States
- R01 MH050850/MH/NIMH NIH HHS/United States
- R01MH50850/MH/NIMH NIH HHS/United States
- R01 MH050840/MH/NIMH NIH HHS/United States
- R01MH50840/MH/NIMH NIH HHS/United States
- R01 MH 69904/MH/NIMH NIH HHS/United States
- R01 MH050839/MH/NIMH NIH HHS/United States
- R01 MH 080221/MH/NIMH NIH HHS/United States
- R01MH50839/MH/NIMH NIH HHS/United States
- R01 MH 50838/MH/NIMH NIH HHS/United States
- K23 MH069904/MH/NIMH NIH HHS/United States
- R01 MH 50837/MH/NIMH NIH HHS/United States
- R01 MH 73708/MH/NIMH NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources