Determinants and consequences of adherence to the dietary approaches to stop hypertension diet in African-American and white adults with high blood pressure: results from the ENCORE trial - PubMed (original) (raw)
Randomized Controlled Trial
. 2012 Nov;112(11):1763-73.
doi: 10.1016/j.jand.2012.07.007. Epub 2012 Sep 19.
Affiliations
- PMID: 23000025
- PMCID: PMC3483427
- DOI: 10.1016/j.jand.2012.07.007
Randomized Controlled Trial
Determinants and consequences of adherence to the dietary approaches to stop hypertension diet in African-American and white adults with high blood pressure: results from the ENCORE trial
Dawn E Epstein et al. J Acad Nutr Diet. 2012 Nov.
Abstract
Background: Although the Dietary Approaches to Stop Hypertension (DASH) diet is an accepted nonpharmacologic treatment for hypertension, little is known about what patient characteristics affect dietary adherence and what level of adherence is needed to reduce blood pressure (BP).
Objective: Our aim was to determine what factors predict dietary adherence and the extent to which dietary adherence is necessary to produce clinically meaningful BP reductions.
Design: Ancillary study of the ENCORE (Exercise and Nutrition Interventions for Cardiovascular Health) trial--a 16-week randomized clinical trial of diet and exercise.
Participants/setting: Participants included 144 sedentary, overweight, or obese adults (body mass index 25 to 39.9) with high BP (systolic 130 to 159 mm Hg and/or diastolic 85 to 99 mm Hg).
Intervention: Patients were randomized to one of three groups: DASH diet alone, DASH diet plus weight management, and Usual Diet Controls.
Main outcomes measures: Our primary outcomes were a composite index of adherence to the DASH diet and clinic BP.
Statistical analyses performed: General linear models were used to compare treatment groups on post-treatment adherence to the DASH diet. Linear regression was used to examine potential predictors of post-treatment DASH adherence. Analysis of covariance was used to examine the relation of adherence to the DASH diet and BP.
Results: Participants in the DASH diet plus weight management (16.1 systolic BP [SBP]; 95% CI 13.0 to 19.2 mm Hg and 9.9 diastolic BP [DBP]; 95% CI 8.1 to 11.6 mm Hg) and DASH diet alone (11.2 SBP; 95% CI 8.1 to 14.3 mm Hg and 7.5 DBP; 95% CI 5.8 to 9.3 mm Hg) groups showed significant reductions in BP in comparison with Usual Diet Controls participants (3.4 SBP; 95% CI 0.4 to 6.4 mm Hg and DBP 3.8; 95% CI 2.2 to 5.5 mm Hg). Greater post-treatment consumption of DASH foods was noted in both the DASH diet alone (mean = 6.20; 95% CI 5.83 to 6.57) and DASH diet plus weight management groups (mean = 6.23; 95% CI 5.88 to 6.59) compared with Usual Diet Controls (mean = 3.66; 95% CI 3.30 to 4.01; P<0.0001), and greater adherence to the DASH diet was associated with larger reductions in clinic SBP and DBP (P ≤ 0.01). Only ethnicity predicted dietary adherence, with African Americans less adherent to the DASH diet compared with whites (4.68; 95% CI 4.34 to 5.03 vs 5.83; 95% CI 5.50 to 6.11; P<0.001).
Conclusions: Greater adherence to the DASH diet was associated with larger BP reductions independent of weight loss. African Americans were less likely to be adherent to the DASH dietary eating plan compared with whites, suggesting that culturally sensitive dietary strategies might be needed to improve adherence to the DASH diet.
Trial registration: ClinicalTrials.gov NCT00571844.
Copyright © 2012 Academy of Nutrition and Dietetics. Published by Elsevier Inc. All rights reserved.
Figures
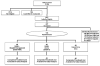
Figure 1
Participant flow in the ENCORE clinical trial. Note: BP- blood pressure; BMI- body mass index (weight in kilograms divided by height in meters squared); and DASH- Dietary Approaches to Stop Hypertension.
Similar articles
- Effects of the DASH diet alone and in combination with exercise and weight loss on blood pressure and cardiovascular biomarkers in men and women with high blood pressure: the ENCORE study.
Blumenthal JA, Babyak MA, Hinderliter A, Watkins LL, Craighead L, Lin PH, Caccia C, Johnson J, Waugh R, Sherwood A. Blumenthal JA, et al. Arch Intern Med. 2010 Jan 25;170(2):126-35. doi: 10.1001/archinternmed.2009.470. Arch Intern Med. 2010. PMID: 20101007 Free PMC article. Clinical Trial. - Optimizing Blood Pressure in African-American Women with Dietary Approaches to Stop Hypertension (DASH).
Divens LL, Carter-Holmes DV. Divens LL, et al. J Natl Black Nurses Assoc. 2019 Jul;30(1):1-6. J Natl Black Nurses Assoc. 2019. PMID: 31465678 - The PREMIER intervention helps participants follow the Dietary Approaches to Stop Hypertension dietary pattern and the current Dietary Reference Intakes recommendations.
Lin PH, Appel LJ, Funk K, Craddick S, Chen C, Elmer P, McBurnie MA, Champagne C. Lin PH, et al. J Am Diet Assoc. 2007 Sep;107(9):1541-51. doi: 10.1016/j.jada.2007.06.019. J Am Diet Assoc. 2007. PMID: 17761231 Clinical Trial. - Dietary Approaches to Stop Hypertension (DASH) Diet and Blood Pressure Reduction in Adults with and without Hypertension: A Systematic Review and Meta-Analysis of Randomized Controlled Trials.
Filippou CD, Tsioufis CP, Thomopoulos CG, Mihas CC, Dimitriadis KS, Sotiropoulou LI, Chrysochoou CA, Nihoyannopoulos PI, Tousoulis DM. Filippou CD, et al. Adv Nutr. 2020 Sep 1;11(5):1150-1160. doi: 10.1093/advances/nmaa041. Adv Nutr. 2020. PMID: 32330233 Free PMC article. - Effects of exercise, diet and weight loss on high blood pressure.
Bacon SL, Sherwood A, Hinderliter A, Blumenthal JA. Bacon SL, et al. Sports Med. 2004;34(5):307-16. doi: 10.2165/00007256-200434050-00003. Sports Med. 2004. PMID: 15107009 Review.
Cited by
- Predictors of Long-Term Adherence to Multiple Health Behavior Recommendations for Weight Management.
Fitzpatrick SL, Appel LJ, Bray B, Brooks N, Stevens VJ. Fitzpatrick SL, et al. Health Educ Behav. 2018 Dec;45(6):997-1007. doi: 10.1177/1090198118757823. Epub 2018 Feb 24. Health Educ Behav. 2018. PMID: 29478353 Free PMC article. - Self-care management strategies used by Black women who self-report consistent adherence to antihypertensive medication.
Abel WM, Joyner JS, Cornelius JB, Greer DB. Abel WM, et al. Patient Prefer Adherence. 2017 Aug 16;11:1401-1412. doi: 10.2147/PPA.S138162. eCollection 2017. Patient Prefer Adherence. 2017. PMID: 28860723 Free PMC article. - Intuitive eating practices among African-American women living with type 2 diabetes: a qualitative study.
Willig AL, Richardson BS, Agne A, Cherrington A. Willig AL, et al. J Acad Nutr Diet. 2014 Jun;114(6):889-896. doi: 10.1016/j.jand.2014.02.004. Epub 2014 Apr 1. J Acad Nutr Diet. 2014. PMID: 24699138 Free PMC article. - Longer Term Effects of Diet and Exercise on Neurocognition: 1-Year Follow-up of the ENLIGHTEN Trial.
Blumenthal JA, Smith PJ, Mabe S, Hinderliter A, Welsh-Bohmer K, Browndyke JN, Doraiswamy PM, Lin PH, Kraus WE, Burke JR, Sherwood A. Blumenthal JA, et al. J Am Geriatr Soc. 2020 Mar;68(3):559-568. doi: 10.1111/jgs.16252. Epub 2019 Nov 22. J Am Geriatr Soc. 2020. PMID: 31755550 Free PMC article. Clinical Trial. - Dietary Management of Heart Failure: DASH Diet and Precision Nutrition Perspectives.
Wickman BE, Enkhmaa B, Ridberg R, Romero E, Cadeiras M, Meyers F, Steinberg F. Wickman BE, et al. Nutrients. 2021 Dec 10;13(12):4424. doi: 10.3390/nu13124424. Nutrients. 2021. PMID: 34959976 Free PMC article. Review.
References
- Joint National Committee on Prevention. Evaluation, and Treatment of High Blood Pressure The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Archives of Internal Medicine. 2003;157:2413–2446. - PubMed
- Appel LJ, Moore TJ, Obarzanek E, et al. A clinical trial of the effects of dietary patterns on blood pressure. DASH Collaborative Research Group. New EngJ Med. 1997;336(16):1117–1124. - PubMed
- Sacks FM, Svetkey LP, Vollmer WM, et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. DASH-Sodium Collaborative Research Group. Nee Eng J Med. 2001;344(1):3–10. - PubMed
- Appel LJ. Lifestyle modification as a means to prevent and treat high blood pressure. J Am Soc Nephrol: JASN. 2003;14(7 Suppl 2):S99–S102. - PubMed
- Appel LJ, Champagne CM, Harsha DW, et al. Effects of comprehensive lifestyle modification on blood pressure control: main results of the PREMIER clinical trial. JAMA. 2003 Apr 23-30;289(16):2083–2093. - PubMed
Publication types
MeSH terms
Grants and funding
- M01-RR-30/RR/NCRR NIH HHS/United States
- 5UL1RR024128-03/RR/NCRR NIH HHS/United States
- UL1 RR024128/RR/NCRR NIH HHS/United States
- M01 RR000030/RR/NCRR NIH HHS/United States
- HL074103/HL/NHLBI NIH HHS/United States
- R01 HL074103/HL/NHLBI NIH HHS/United States
LinkOut - more resources
Full Text Sources
Medical