Circulating omega-6 polyunsaturated fatty acids and total and cause-specific mortality: the Cardiovascular Health Study - PubMed (original) (raw)
Multicenter Study
Circulating omega-6 polyunsaturated fatty acids and total and cause-specific mortality: the Cardiovascular Health Study
Jason H Y Wu et al. Circulation. 2014.
Abstract
Background: Although omega-6 polyunsaturated fatty acids (n-6 PUFA) have been recommended to reduce coronary heart disease (CHD), controversy remains about benefits versus harms, including concerns over theorized proinflammatory effects of n-6 PUFA. We investigated associations of circulating n-6 PUFA including linoleic acid (the major dietary PUFA), γ-linolenic acid, dihomo-γ-linolenic acid, and arachidonic acid, with total and cause-specific mortality in the Cardiovascular Health Study, a community-based U.S. cohort.
Methods and results: Among 2792 participants(aged ≥65 years) free of cardiovascular disease at baseline, plasma phospholipid n-6 PUFA were measured at baseline using standardized methods. All-cause and cause-specific mortality, and total incident CHD and stroke, were assessed and adjudicated centrally. Associations of PUFA with risk were assessed by Cox regression. During 34 291 person-years of follow-up (1992-2010), 1994 deaths occurred (678 cardiovascular deaths), with 427 fatal and 418 nonfatal CHD, and 154 fatal and 399 nonfatal strokes. In multivariable models, higher linoleic acid was associated with lower total mortality, with extreme-quintile hazard ratio =0.87 (P trend=0.005). Lower death was largely attributable to cardiovascular disease causes, especially nonarrhythmic CHD mortality (hazard ratio, 0.51; 95% confidence interval, 0.32-0.82; P trend=0.001). Circulating γ-linolenic acid, dihomo-γ-linolenic acid, and arachidonic acid were not significantly associated with total or cause-specific mortality (eg, for arachidonic acid and CHD death, the extreme-quintile hazard ratio was 0.97; 95% confidence interval, 0.70-1.34; P trend=0.87). Evaluated semiparametrically, linoleic acid showed graded inverse associations with total mortality (P=0.005). There was little evidence that associations of n-6 PUFA with total mortality varied by age, sex, race, or plasma n-3 PUFA. Evaluating both n-6 and n-3 PUFA, lowest risk was evident with highest levels of both.
Conclusions: High circulating linoleic acid, but not other n-6 PUFA, was inversely associated with total and CHD mortality in older adults.
Keywords: cardiovascular diseases; epidemiology; fatty acids, omega-6; mortality.
© 2014 American Heart Association, Inc.
Conflict of interest statement
Conflict of Interest Disclosures: Dr. Mozaffarian reports ad hoc travel reimbursement or honoraria from Bunge, Pollock Institute, Quaker Oats, and Life Sciences Research Organization; ad hoc consulting fees from McKinsey Health Systems Institute, Foodminds, Nutrition Impact, Amarin, Omthera, and Winston and Strawn LLP; membership, Unilever North America Scientific Advisory Board; royalties from UpToDate; and research grants from GlaxoSmithKline, Sigma Tau, Pronova, the Gates Foundation, the Sackler Institute of Nutrition, and the National Institutes of Health. The other authors report no conflicts.
Figures
Figure 1
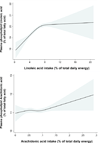
Relationship between estimated dietary consumption of linoleic acid and arachidonic acid and their circulating concentrations in plasma phospholipids, evaluated using restricted cubic splines and adjusted for age, gender, race, BMI, and use of lipid lowering medications. The solid lines and shaded areas represent the central risk estimates and 95% CIs, respectively. Median intakes of linoleic acid and arachidonic acid were 6% of total energy (14.1g/day) and 0.08% of total energy (0.17g/day), respectively. Strong evidence was seen for both overall positive association (P < 0.001) and nonlinearity (P < 0.001) of the relationship between dietary and circulating linoleic acid. In contrast, little evidence of either an overall relationship (P = 0.24) or nonlinearity (P = 0.40) was evident for dietary and circulating arachidonic acid.
Figure 2
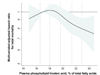
Multivariable hazard ratios of plasma phospholipid linoleic acid with risk of total mortality, evaluated by restricted cubic splines from Cox models adjusted for age, gender, race, enrollment site, education, smoking status, prevalent diabetes, atrial fibrillation, and hypertension, leisure-time physical activity, body mass index, waist circumference, alcohol use, and plasma phospholipid long-chain n-3 PUFA levels. The solid lines and shaded areas represent the central risk estimates and 95% CIs, respectively, relative to the reference level (12.5th percentile). The dotted vertical lines correspond to the 10th, 25th, 50th, 75th, and 90th percentiles of linoleic acid levels. A significant inverse association was evident (P=0.005), with little evidence for nonlinearity (P nonlinearity=0.16).
Figure 3
Multivariable hazard ratios for total mortality by joint levels of plasma phospholipid linoleic acid and long-chain n-3 PUFA, adjusted for age, gender, race, enrollment site, education, smoking status, prevalent diabetes, atrial fibrillation, and hypertension, leisure-time physical activity, body mass index, waist circumference, and alcohol use, *P<0.05 compared with the referent category. Associations appeared independent, with little evidence for significant interaction between linoleic acid and long-chain n-3 PUFA (Wald test for multiplicative interaction: _P_=0.54).
Comment in
- Letter by Sertoglu et al Regarding Article, "Circulating Omega-6 Polyunsaturated Fatty Acids and Total and Cause-Specific Mortality: The Cardiovascular Health Study".
Sertoglu E, Kayadibi H, Uyanik M. Sertoglu E, et al. Circulation. 2015 Jul 21;132(3):e22. doi: 10.1161/CIRCULATIONAHA.114.013853. Circulation. 2015. PMID: 26195493 No abstract available.
Similar articles
- Plasma phospholipid long-chain ω-3 fatty acids and total and cause-specific mortality in older adults: a cohort study.
Mozaffarian D, Lemaitre RN, King IB, Song X, Huang H, Sacks FM, Rimm EB, Wang M, Siscovick DS. Mozaffarian D, et al. Ann Intern Med. 2013 Apr 2;158(7):515-25. doi: 10.7326/0003-4819-158-7-201304020-00003. Ann Intern Med. 2013. PMID: 23546563 Free PMC article. - Circulating and dietary omega-3 and omega-6 polyunsaturated fatty acids and incidence of CVD in the Multi-Ethnic Study of Atherosclerosis.
de Oliveira Otto MC, Wu JH, Baylin A, Vaidya D, Rich SS, Tsai MY, Jacobs DR Jr, Mozaffarian D. de Oliveira Otto MC, et al. J Am Heart Assoc. 2013 Dec 18;2(6):e000506. doi: 10.1161/JAHA.113.000506. J Am Heart Assoc. 2013. PMID: 24351702 Free PMC article. - N-6 and N-3 fatty acid cholesteryl esters in relation to fatal CHD in a Dutch adult population: a nested case-control study and meta-analysis.
de Goede J, Verschuren WM, Boer JM, Verberne LD, Kromhout D, Geleijnse JM. de Goede J, et al. PLoS One. 2013 May 31;8(5):e59408. doi: 10.1371/journal.pone.0059408. Print 2013. PLoS One. 2013. PMID: 23741290 Free PMC article. - Gestational diabetes mellitus decreased umbilical cord blood polyunsaturated fatty acids: a meta-analysis of observational studies.
Hai-Tao Y, Zhi-Heng G, Yi-Ru C, Yue-Ting L, Hai-Ying Z, Ya-Juan L, Lin X. Hai-Tao Y, et al. Prostaglandins Leukot Essent Fatty Acids. 2021 Aug;171:102318. doi: 10.1016/j.plefa.2021.102318. Epub 2021 Jul 2. Prostaglandins Leukot Essent Fatty Acids. 2021. PMID: 34246926 Review. - Plasma free fatty acid and lipoproteins as sources of polyunsaturated fatty acid for the brain.
Spector AA. Spector AA. J Mol Neurosci. 2001 Apr-Jun;16(2-3):159-65; discussion 215-21. doi: 10.1385/JMN:16:2-3:159. J Mol Neurosci. 2001. PMID: 11478370 Review.
Cited by
- Associations of serum n-3 and n-6 polyunsaturated fatty acids with plasma natriuretic peptides.
Daneshmand R, Kurl S, Tuomainen TP, Virtanen JK. Daneshmand R, et al. Eur J Clin Nutr. 2016 Aug;70(8):963-9. doi: 10.1038/ejcn.2016.58. Epub 2016 Apr 13. Eur J Clin Nutr. 2016. PMID: 27071511 - Re-evaluation of the traditional diet-heart hypothesis: analysis of recovered data from Minnesota Coronary Experiment (1968-73).
Ramsden CE, Zamora D, Majchrzak-Hong S, Faurot KR, Broste SK, Frantz RP, Davis JM, Ringel A, Suchindran CM, Hibbeln JR. Ramsden CE, et al. BMJ. 2016 Apr 12;353:i1246. doi: 10.1136/bmj.i1246. BMJ. 2016. PMID: 27071971 Free PMC article. Review. - Plasma Cholesterol- and Body Fat-Lowering Effects of Chicken Protein Hydrolysate and Oil in High-Fat Fed Male Wistar Rats.
Aloysius TA, Tillander V, Pedrelli M, Dankel SN, Berge RK, Bjørndal B. Aloysius TA, et al. Nutrients. 2022 Dec 16;14(24):5364. doi: 10.3390/nu14245364. Nutrients. 2022. PMID: 36558523 Free PMC article. - Update of the Brazilian Guideline for Familial Hypercholesterolemia - 2021.
Izar MCO, Giraldez VZR, Bertolami A, Santos Filho RDD, Lottenberg AM, Assad MHV, Saraiva JFK, Chacra APM, Martinez TLR, Bahia LR, Fonseca FAH, Faludi AA, Sposito AC, Chagas ACP, Jannes CE, Amaral CK, Araújo DB, Cintra DE, Coutinho EDR, Cesena F, Xavier HT, Mota ICP, Giuliano ICB, Faria Neto JR, Kato JT, Bertolami MC, Miname MH, Castelo MHCG, Lavrador MSF, Machado RM, Souza PG, Alves RJ, Machado VA, Salgado Filho W. Izar MCO, et al. Arq Bras Cardiol. 2021 Oct;117(4):782-844. doi: 10.36660/abc.20210788. Arq Bras Cardiol. 2021. PMID: 34709306 Free PMC article. English, Portuguese. No abstract available.
References
- Dietary Guidelines for Americans. 7th ed. Washington DC: UC Government Printing Office; 2010. US Department of Agriculture, US Department of Health and Human Services. - PubMed
- Harris WS, Mozaffarian D, Rimm E, Kris-Etherton P, Rudel LL, Appel LJ, Engler MM, Engler MB, Sacks F. Omega-6 fatty acids and risk for cardiovascular disease: a science advisory from the American Heart Association Nutrition Subcommittee of the Council on Nutrition, Physical Activity, and Metabolism; Council on Cardiovascular Nursing; and Council on Epidemiology and Prevention. Circulation. 2009;119:902–907. - PubMed
- Mensink RP, Zock PL, Kester AD, Katan MB. Effects of dietary fatty acids and carbohydrates on the ratio of serum total to HDL cholesterol and on serum lipids and apolipoproteins: a meta-analysis of 60 controlled trials. Am J Clin Nutr. 2003;77:1146–1155. - PubMed
- Jakobsen MU, O'Reilly EJ, Heitmann BL, Pereira MA, Balter K, Fraser GE, Goldbourt U, Hallmans G, Knekt P, Liu S, Pietinen P, Spiegelman D, Stevens J, Virtamo J, Willett WC, Ascherio A. Major types of dietary fat and risk of coronary heart disease: a pooled analysis of 11 cohort studies. Am J Clin Nutr. 2009;89:1425–1432. - PMC - PubMed
- Chowdhury R, Warnakula S, Kunutsor S, Crowe F, Ward HA, Johnson L, Franco OH, Butterworth AS, Forouhi NG, Thompson SG, Khaw K, Mozaffarian D, Danesh J, Di Angelantonio E. Association of Dietary, Circulating, and Supplement Fatty Acids With Coronary Risk: A Systematic Review and Meta-analysis. Ann Intern Med. 2014;160:398–406. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- HHSN268200800007C/HL/NHLBI NIH HHS/United States
- N01HC55222/HL/NHLBI NIH HHS/United States
- N01HC85086/HL/NHLBI NIH HHS/United States
- HHSN268201200036C/HL/NHLBI NIH HHS/United States
- R01 HL080295/HL/NHLBI NIH HHS/United States
- N01HC85082/HL/NHLBI NIH HHS/United States
- N01HC85083/HL/NHLBI NIH HHS/United States
- HL080295/HL/NHLBI NIH HHS/United States
- N01HC85080/HL/NHLBI NIH HHS/United States
- N01HC85081/HL/NHLBI NIH HHS/United States
- R01 HL085710/HL/NHLBI NIH HHS/United States
- U01 HL080295/HL/NHLBI NIH HHS/United States
- N01HC85079/HL/NHLBI NIH HHS/United States
- R01 AG023629/AG/NIA NIH HHS/United States
- AG023629/AG/NIA NIH HHS/United States
- R56 AG023629/AG/NIA NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical