Ex Vivo Drug Susceptibility Testing and Molecular Profiling of Clinical Plasmodium falciparum Isolates from Cambodia from 2008 to 2013 Suggest Emerging Piperaquine Resistance - PubMed (original) (raw)
. 2015 Aug;59(8):4631-43.
doi: 10.1128/AAC.00366-15. Epub 2015 May 26.
David L Saunders 1, Darapiseth Sea 1, Nitima Chanarat 1, Kritsanai Yingyuen 1, Siratchana Sundrakes 1, Piyaporn Saingam 1, Nillawan Buathong 1, Sabaithip Sriwichai 1, Soklyda Chann 1, Youry Se 1, You Yom 2, Thay Kheng Heng 2, Nareth Kong 2, Worachet Kuntawunginn 1, Kuntida Tangthongchaiwiriya 1, Christopher Jacob 3, Shannon Takala-Harrison 3, Christopher Plowe 3, Jessica T Lin 4, Char Meng Chuor 2, Satharath Prom 5, Stuart D Tyner 1, Panita Gosi 1, Paktiya Teja-Isavadharm 1, Chanthap Lon 1, Charlotte A Lanteri 6
Affiliations
- PMID: 26014942
- PMCID: PMC4505231
- DOI: 10.1128/AAC.00366-15
Ex Vivo Drug Susceptibility Testing and Molecular Profiling of Clinical Plasmodium falciparum Isolates from Cambodia from 2008 to 2013 Suggest Emerging Piperaquine Resistance
Suwanna Chaorattanakawee et al. Antimicrob Agents Chemother. 2015 Aug.
Abstract
Cambodia's first-line artemisinin combination therapy, dihydroartemisinin-piperaquine (DHA-PPQ), is no longer sufficiently curative against multidrug-resistant Plasmodium falciparum malaria at some Thai-Cambodian border regions. We report recent (2008 to 2013) drug resistance trends in 753 isolates from northern, western, and southern Cambodia by surveying for ex vivo drug susceptibility and molecular drug resistance markers to guide the selection of an effective alternative to DHA-PPQ. Over the last 3 study years, PPQ susceptibility declined dramatically (geomean 50% inhibitory concentration [IC50] increased from 12.8 to 29.6 nM), while mefloquine (MQ) sensitivity doubled (67.1 to 26 nM) in northern Cambodia. These changes in drug susceptibility were significantly associated with a decreased prevalence of P. falciparum multidrug resistance 1 gene (Pfmdr1) multiple copy isolates and coincided with the timing of replacing artesunate-mefloquine (AS-MQ) with DHA-PPQ as the first-line therapy. Widespread chloroquine resistance was suggested by all isolates being of the P. falciparum chloroquine resistance transporter gene CVIET haplotype. Nearly all isolates collected from the most recent years had P. falciparum kelch13 mutations, indicative of artemisinin resistance. Ex vivo bioassay measurements of antimalarial activity in plasma indicated 20% of patients recently took antimalarials, and their plasma had activity (median of 49.8 nM DHA equivalents) suggestive of substantial in vivo drug pressure. Overall, our findings suggest DHA-PPQ failures are associated with emerging PPQ resistance in a background of artemisinin resistance. The observed connection between drug policy changes and significant reduction in PPQ susceptibility with mitigation of MQ resistance supports reintroduction of AS-MQ, in conjunction with monitoring of the P. falciparum mdr1 copy number, as a stop-gap measure in areas of DHA-PPQ failure.
Copyright © 2015, American Society for Microbiology. All Rights Reserved.
Figures
FIG 1
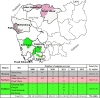
Cambodian field sites and numbers of P. falciparum isolates by region collected from malaria patients during 2008 to 2013. The map shows the locations of isolate collection sites (dot patterns denote collection provinces; gray, pink, and green shading indicate western, northern, and southern regional district areas, respectively; a plus sign indicates health centers). The table presents numbers of isolates collected per site per year and totals by region.
FIG 2
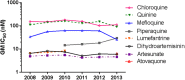
Overall trends in ex vivo drug susceptibility of P. falciparum isolates collected during 2008 to 2013 in Cambodia. GM IC50s (in nanomolars) are shown for each drug by year.
FIG 3
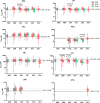
Ex vivo drug susceptibility of P. falciparum isolates from Cambodia by year and region. Box-whisker plots of IC50s (in nanomolars) are shown for each drug stratified by collection year and region: west (gray), north (pink), and south (green). Dashed lines denote median IC50s against the P. falciparum W2 reference clone and interquartile ranges. Significant P values by Mann-Whitney U test indicate differences in IC50s between regions within the same year. A significant progressive decline in MQ IC50s and rise in PPQ IC50s during 2009 to 2013 in northern isolates is denoted by an asterisk (P < 0.001 by Kruskal-Wallis test).
FIG 4
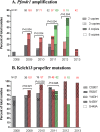
Frequency of Pf_mdr1_ amplification and Kelch13 propeller mutations by region and year. Isolate collection regions are indicated by colored bars as western (gray), northern (pink), and southern (green) Cambodia. Numbers of isolates analyzed for each region/year are indicated above each bar graph. Significant P values are shown for differences in frequency of Pf_mdr1_ amplification and Pf_kelch13_ R539T or C580Y among regions within the same year by χ2 test.
FIG 5
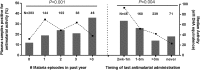
Associations between percent plasma samples positive for ex vivo antimalarial activity and patient-reported history of malaria episodes and treatment. P values of χ2 association tests are noted. Dotted lines indicate median DHA equivalents, in nanomolars, for bioassay-positive patients in each self-reported category. Numbers of isolates analyzed for each category are indicated above each bar graph.
Similar articles
- Efficacy of three anti-malarial regimens for uncomplicated Plasmodium falciparum malaria in Cambodia, 2009-2011: a randomized controlled trial and brief review.
Lek D, Rachmat A, Harrison D, Chin G, Chaoratanakawee S, Saunders D, Menard D, Rogers WO. Lek D, et al. Malar J. 2022 Sep 7;21(1):259. doi: 10.1186/s12936-022-04279-3. Malar J. 2022. PMID: 36071520 Free PMC article. Review. - Ex vivo susceptibility of Plasmodium falciparum to antimalarial drugs in western, northern, and eastern Cambodia, 2011-2012: association with molecular markers.
Lim P, Dek D, Try V, Eastman RT, Chy S, Sreng S, Suon S, Mao S, Sopha C, Sam B, Ashley EA, Miotto O, Dondorp AM, White NJ, Su XZ, Char MC, Anderson JM, Amaratunga C, Menard D, Fairhurst RM. Lim P, et al. Antimicrob Agents Chemother. 2013 Nov;57(11):5277-83. doi: 10.1128/AAC.00687-13. Epub 2013 Aug 12. Antimicrob Agents Chemother. 2013. PMID: 23939897 Free PMC article. - Ex vivo piperaquine resistance developed rapidly in Plasmodium falciparum isolates in northern Cambodia compared to Thailand.
Chaorattanakawee S, Lon C, Jongsakul K, Gawee J, Sok S, Sundrakes S, Kong N, Thamnurak C, Chann S, Chattrakarn S, Praditpol C, Buathong N, Uthaimongkol N, Smith P, Sirisopana N, Huy R, Prom S, Fukuda MM, Bethell D, Walsh DS, Lanteri C, Saunders D. Chaorattanakawee S, et al. Malar J. 2016 Oct 21;15(1):519. doi: 10.1186/s12936-016-1569-y. Malar J. 2016. PMID: 27769299 Free PMC article. Clinical Trial. - Piperaquine resistant Cambodian Plasmodium falciparum clinical isolates: in vitro genotypic and phenotypic characterization.
Boonyalai N, Vesely BA, Thamnurak C, Praditpol C, Fagnark W, Kirativanich K, Saingam P, Chaisatit C, Lertsethtakarn P, Gosi P, Kuntawunginn W, Vanachayangkul P, Spring MD, Fukuda MM, Lon C, Smith PL, Waters NC, Saunders DL, Wojnarski M. Boonyalai N, et al. Malar J. 2020 Jul 25;19(1):269. doi: 10.1186/s12936-020-03339-w. Malar J. 2020. PMID: 32711538 Free PMC article. - Monitoring antimalarial drug efficacy in the Greater Mekong Subregion: an overview of in vivo results from 2008 to 2010.
Bustos MD, Wongsrichanalai C, Delacollette C, Burkholder B. Bustos MD, et al. Southeast Asian J Trop Med Public Health. 2013;44 Suppl 1:201-30; discussion 306-7. Southeast Asian J Trop Med Public Health. 2013. PMID: 24159833 Review.
Cited by
- Rapid detection of mutations in the suspected piperaquine resistance gene E415G-exo in Plasmodium falciparum exonuclease via AS‒PCR and RAA with CRISPR/Cas12a.
Zhu H, Zhu D, Li Y, Li Y, Song X, Mo J, Liu L, Liu Z, Wang S, Yao Y, Yan H, Wu K, Wang W, Yin J, Lin M, Li J. Zhu H, et al. Int J Parasitol Drugs Drug Resist. 2024 Dec;26:100568. doi: 10.1016/j.ijpddr.2024.100568. Epub 2024 Oct 28. Int J Parasitol Drugs Drug Resist. 2024. PMID: 39476461 Free PMC article. - Progressive heterogeneity of enlarged and irregularly shaped apicoplasts in Plasmodium falciparum persister blood stages after drug treatment.
Micchelli CE, Percopo C, Traver M, Brzostowski J, Amin SN, Prigge ST, Sá JM, Wellems TE. Micchelli CE, et al. PNAS Nexus. 2024 Sep 24;3(10):pgae424. doi: 10.1093/pnasnexus/pgae424. eCollection 2024 Oct. PNAS Nexus. 2024. PMID: 39381646 Free PMC article. - Progressive heterogeneity of enlarged and irregularly shaped apicoplasts in P. falciparum persister blood stages after drug treatment.
Micchelli CE, Percopo C, Traver M, Brzostowski J, Amin SN, Prigge ST, Sá JM, Wellems TE. Micchelli CE, et al. bioRxiv [Preprint]. 2024 Aug 29:2024.01.03.574077. doi: 10.1101/2024.01.03.574077. bioRxiv. 2024. PMID: 38410435 Free PMC article. Updated. Preprint. - In vitro activity of rhinacanthin analogues against drug resistant Plasmodium falciparum isolates from Northeast Thailand.
Chaorattanakawee S, Kosaisavee V, Bunsermyos W, Aonsri C, Imaram W, Suwannasin K, Kunasol C, Thamnurak C, Boonyalai N, Saunders D, Dondorp AM, Mungthin M, Imwong M. Chaorattanakawee S, et al. Malar J. 2023 Mar 23;22(1):105. doi: 10.1186/s12936-023-04532-3. Malar J. 2023. PMID: 36959593 Free PMC article. - Efficacy of three anti-malarial regimens for uncomplicated Plasmodium falciparum malaria in Cambodia, 2009-2011: a randomized controlled trial and brief review.
Lek D, Rachmat A, Harrison D, Chin G, Chaoratanakawee S, Saunders D, Menard D, Rogers WO. Lek D, et al. Malar J. 2022 Sep 7;21(1):259. doi: 10.1186/s12936-022-04279-3. Malar J. 2022. PMID: 36071520 Free PMC article. Review.
References
- Wongsrichanalai C, Sirichaisinthop J, Karwacki JJ, Congpuong K, Miller RS, Pang L, Thimasarn K. 2001. Drug resistant malaria on the Thai-Myanmar and Thai-Cambodian borders. Southeast Asian J Trop Med Public Health 32:41–49. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous