Prevalence and temporal pattern of hospital readmissions for patients with type I and type II diabetes - PubMed (original) (raw)
Prevalence and temporal pattern of hospital readmissions for patients with type I and type II diabetes
Xiaoqian Liu et al. BMJ Open. 2015.
Abstract
Objective: Repeated hospitalisation for patients is common and costly, yet partly preventable. However, we know little about readmissions for patients with diabetes in China. The current study aims to assess the frequency and temporal pattern of and risk factors for all-cause readmission among hospitalised patients with diabetes in Tianjin, China.
Method: This retrospective, cohort analysis used the Tianjin Basic Medical Insurance Register System data of 2011. The patterns of and the reasons for all-cause readmissions for patients with diabetes were described. The differences of readmission-free survival (RFS) between newly and previously diagnosed patients were compared. Time-dependent Cox models were established to identify the risk factors for readmission at different time intervals after discharge.
Results: Readmission rates were approximately 30%, with the most common diagnoses of cerebral infarction (for type I) or diabetes (for type II) for patients with diabetes. The majority of patients were readmitted to the hospital after more than 90 days, followed by 8-30 days (all p=0.002). Approximately 37.2% and 42.8% of readmitted patients with type I and type II diabetes were diagnosed previously, and the RFS rates for previously diagnosed patients were significantly lower than for newly diagnosed patients at any time interval after discharge. Prior history of diabetes (all p<0.05), length of stay (all p<0.01) and reimbursement ratio (90% vs >92%, all p<0.0002) were consistently associated with the RFS for patients readmitted to the hospital at <7, 8-30, 31-60 and 61-90 days.
Conclusions: Hospital readmissions among patients with diabetes were affected by the diagnosis status. Patient characteristics and the quality of healthcare might regulate short-interval and long-interval hospital readmission, respectively, after discharge.
Keywords: hospital readmission.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://www.bmj.com/company/products-services/rights-and-licensing/
Figures
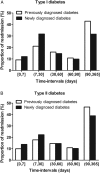
Figure 1
The proportions of readmission for newly and previously diagnosed patients with diabetes showed that, for both type of diabetes, the proportions of readmission for previously diagnosed patients with diabetes were higher than for newly diagnosed patients at intervals of 31–60, 61–90 and >90 days (p=0.002).
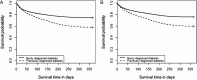
Figure 2
Kaplan–Meier (KM)-survival curves for readmission-free survival (RFS) of patients with (A) type I and (B) type II diabetes by diagnosis status. The 1-year RFS rate of patients with previously diagnosed type I or type II diabetes was significantly lower than that of newly diagnosed patients (p<0.0001).
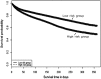
Figure 3
KM-survival curves for readmission-free survival (RFS) of patients with diabetes by predicted risk groups. The KM-survival curves for RFS as predicted in baseline 1-year readmission model from the HRs. Two curves represented low-risk group (upper) and high-risk group (lower) for readmission, respectively, and were well separated, confirming our model has good discrimination.
Similar articles
- The prevalence and long-term variation of hospital readmission for patients with diabetes in Tianjin, China: A cross-sectional study.
Liu X, Guo Y, Li D, Cui Z, Liu Y, Li C, Ma J. Liu X, et al. Medicine (Baltimore). 2017 Oct;96(42):e7953. doi: 10.1097/MD.0000000000007953. Medicine (Baltimore). 2017. PMID: 29049189 Free PMC article. - Risk Factors for 30-Day Readmissions of Individuals with Decompensated Cirrhosis.
Agrawal K, Kumar P, Markert R, Agrawal S. Agrawal K, et al. South Med J. 2015 Nov;108(11):682-7. doi: 10.14423/SMJ.0000000000000371. South Med J. 2015. PMID: 26539950 - Readmission to the Intensive Care Unit: Incidence, Risk Factors, Resource Use, and Outcomes. A Retrospective Cohort Study.
Ponzoni CR, Corrêa TD, Filho RR, Serpa Neto A, Assunção MSC, Pardini A, Schettino GPP. Ponzoni CR, et al. Ann Am Thorac Soc. 2017 Aug;14(8):1312-1319. doi: 10.1513/AnnalsATS.201611-851OC. Ann Am Thorac Soc. 2017. PMID: 28530118 - A Systematic Review of Recent Studies on Hospital Readmissions of Patients With Diabetes.
Kukde RD, Chakraborty A, Shah J. Kukde RD, et al. Cureus. 2024 Aug 22;16(8):e67513. doi: 10.7759/cureus.67513. eCollection 2024 Aug. Cureus. 2024. PMID: 39310630 Free PMC article. Review.
Cited by
- Impact of capitation on outpatient expenses among patients with diabetes mellitus in Tianjin, China: a natural experiment.
Dong Y, Chen J, Jing X, Shi X, Chen Y, Deng X, Li C, Ma J. Dong Y, et al. BMJ Open. 2019 Jun 21;9(6):e024807. doi: 10.1136/bmjopen-2018-024807. BMJ Open. 2019. PMID: 31229998 Free PMC article. - The effects of patient cost sharing on inpatient utilization, cost, and outcome.
Xu Y, Li N, Lu M, Dixon E, Myers RP, Jolley RJ, Quan H. Xu Y, et al. PLoS One. 2017 Oct 26;12(10):e0187096. doi: 10.1371/journal.pone.0187096. eCollection 2017. PLoS One. 2017. PMID: 29073234 Free PMC article. - Prevalence of cardiovascular disease in type 2 diabetes: a systematic literature review of scientific evidence from across the world in 2007-2017.
Einarson TR, Acs A, Ludwig C, Panton UH. Einarson TR, et al. Cardiovasc Diabetol. 2018 Jun 8;17(1):83. doi: 10.1186/s12933-018-0728-6. Cardiovasc Diabetol. 2018. PMID: 29884191 Free PMC article. - Analysing repeated hospital readmissions using data mining techniques.
Ben-Assuli O, Padman R. Ben-Assuli O, et al. Health Syst (Basingstoke). 2018 Nov 9;7(3):166-180. doi: 10.1080/20476965.2018.1510040. eCollection 2018. Health Syst (Basingstoke). 2018. PMID: 31215903 Free PMC article. - Emergency department visits of older adults within 30 days of discharge: analysis from the pharmacotherapy perspective.
Santos FSD, Dias BM, Reis AMM. Santos FSD, et al. Einstein (Sao Paulo). 2019 Oct 24;18:eAO4871. doi: 10.31744/einstein_journal/2020AO4871. eCollection 2019. Einstein (Sao Paulo). 2019. PMID: 31664324 Free PMC article.
References
- Wang W, McGreevey WP, Fu C et al. . Type 2 diabetes mellitus in China: a preventable economic burden. Am J Manag Care 2009;15:593–601. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical