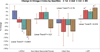Effect of Omega-3 Acid Ethyl Esters on Left Ventricular Remodeling After Acute Myocardial Infarction: The OMEGA-REMODEL Randomized Clinical Trial - PubMed (original) (raw)
Randomized Controlled Trial
. 2016 Aug 2;134(5):378-91.
doi: 10.1161/CIRCULATIONAHA.115.019949.
Shuaib Abdullah 1, James V Pottala 1, Ravi Shah 1, Siddique Abbasi 1, Damien Mandry 1, Sanjeev A Francis 1, Heidi Lumish 1, Brian B Ghoshhajra 1, Udo Hoffmann 1, Evan Appelbaum 1, Jiazhuo H Feng 1, Ron Blankstein 1, Michael Steigner 1, Joseph P McConnell 1, William Harris 1, Elliott M Antman 1, Michael Jerosch-Herold 1, Raymond Y Kwong 2
Affiliations
- PMID: 27482002
- PMCID: PMC4973577
- DOI: 10.1161/CIRCULATIONAHA.115.019949
Randomized Controlled Trial
Effect of Omega-3 Acid Ethyl Esters on Left Ventricular Remodeling After Acute Myocardial Infarction: The OMEGA-REMODEL Randomized Clinical Trial
Bobak Heydari et al. Circulation. 2016.
Abstract
Background: Omega-3 fatty acids from fish oil have been associated with beneficial cardiovascular effects, but their role in modifying cardiac structures and tissue characteristics in patients who have had an acute myocardial infarction while receiving current guideline-based therapy remains unknown.
Methods: In a multicenter, double-blind, placebo-controlled trial, participants presenting with an acute myocardial infarction were randomly assigned 1:1 to 6 months of high-dose omega-3 fatty acids (n=180) or placebo (n=178). Cardiac magnetic resonance imaging was used to assess cardiac structure and tissue characteristics at baseline and after study therapy. The primary study endpoint was change in left ventricular systolic volume index. Secondary endpoints included change in noninfarct myocardial fibrosis, left ventricular ejection fraction, and infarct size.
Results: By intention-to-treat analysis, patients randomly assigned to omega-3 fatty acids experienced a significant reduction of left ventricular systolic volume index (-5.8%, P=0.017), and noninfarct myocardial fibrosis (-5.6%, P=0.026) in comparison with placebo. Per-protocol analysis revealed that those patients who achieved the highest quartile increase in red blood cell omega-3 index experienced a 13% reduction in left ventricular systolic volume index in comparison with the lowest quartile. In addition, patients in the omega-3 fatty acid arm underwent significant reductions in serum biomarkers of systemic and vascular inflammation and myocardial fibrosis. There were no adverse events associated with high-dose omega-3 fatty acid therapy.
Conclusions: Treatment of patients with acute myocardial infarction with high-dose omega-3 fatty acids was associated with reduction of adverse left ventricular remodeling, noninfarct myocardial fibrosis, and serum biomarkers of systemic inflammation beyond current guideline-based standard of care.
Clinical trial registration: URL: http://www.clinicaltrials.gov. Unique identifier: NCT00729430.
Keywords: endomyocardial fibrosis; fatty acids, omega-3; infarction; magnetic resonance imaging; ventricular remodeling.
© 2016 American Heart Association, Inc.
Figures
Figure 1. Enrollment and Randomization
The treatment duration was 6 months for both randomized arms (between study visit 1 and 2). CMR denotes cardiac magnetic resonance imaging, ICD implantable cardioverter-defibrillator, O-3FA omega-3 fatty acids from fish oil.
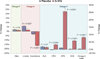
Figure 2. Percent Change of Fatty Acid Levels from Baseline to Post Treatment
Percent changes from baseline to post treatment levels of red blood cell omega-3 fatty acid are shown for the omega-3 fatty acid treated group (red bars) and placebo arm (blue bars). P values are for comparisons of percent change in red blood cell fatty acid levels between the randomized treatment arms. ALA denoted α-Linolenic acid, DHA docosahexanoic acid, DPA docosapentaenoic acid, EPA eicosapentanoic acid, and O-3FA omega-3 fatty acids from fish oil.
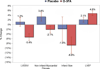
Figure 3. Percent Change of Primary and Secondary Endpoints Post Treatment
Percent changes from baseline to post treatment of the primary and secondary endpoints are shown for the omega-3 fatty acid treated group (red bars) and placebo arm (blue bars). LVESVI denotes left ventricular end-systolic volume index, and LVEF left ventricular ejection fraction.
Figure 4. Comparison of Percent Change in Study Endpoints with Quartiles of Change in Omega-3-Index Post Treatment for Patients that Completed Both Study Visits
Percent changes from pre-treatment to post-treatment of LVESVI, non-infarct myocardial fibrosis, and LVEF versus quartile changes of the red blood cell omega-3 index levels for all patients who completed both study visits (n=227). The quartiles for change in the red blood cell omega-3 index were −0.6% to 0.5%, 0.5 to 2.6%, 2.6 to 5.8%, and > 5.8%. The 5th and 95th percentiles for change in the omega-3 index were −1.0% and 6.8%, respectively. * indicate p-value < 0.05 compared to first quartile (reference), linear trend p-values are also reported.
Figure 5. Comparison of Percent Change in Systemic Biomarkers with Quartiles of Change in Omega-3-Index Post Treatment for Patients that Completed Both Study Visits
Percent changes from pre-treatment to post-treatment of systemic biomarkers versus quartile changes of the red blood cell omega-3 index levels for all patients who completed both study visits (n=227). The quartiles for change in the red blood cell omega-3 index were −0.6% to 0.5%, 0.5 to 2.6%, 2.6 to 5.8%, and > 5.8%. The 5th and 95th percentiles for change in the omega-3 index were −1.0% and 6.8%, respectively. * indicate p-value < 0.05 compared to first quartile (reference), linear trend p-values are also reported. CRP denotes high sensitivity C-reactive protein, Lp-PLA2 lipoprotein-associated phospholipase A2, and NT-proBNP N-terminal of the prohormone brain natriuretic peptide.
Figure 6. Scatter Plot of Percent Change in Serum Biomarker ST2 versus Percent Change of Non-Infarct Myocardial Fibrosis Post Treatment
Percent change from baseline to post treatment of the serum biomarker ST2 correlated against percent change in non-infarct myocardial fibrosis following 6 months of treatment with high dose omega-3 fatty acids from fish oil. P-value is for Pearson correlation coefficient.
Comment in
- Response by Heydari et al to Letter Regarding Article, "Effect of Omega-3 Acid Ethyl Esters on Left Ventricular Remodeling After Acute Myocardial Infarction: The OMEGA-REMODEL Randomized Clinical Trial".
Heydari B, Harris WS, Kwong RY. Heydari B, et al. Circulation. 2017 Jan 10;135(2):e13-e14. doi: 10.1161/CIRCULATIONAHA.116.025704. Circulation. 2017. PMID: 28069718 Free PMC article. No abstract available.
Similar articles
- Genetic profiling of fatty acid desaturase polymorphisms identifies patients who may benefit from high-dose omega-3 fatty acids in cardiac remodeling after acute myocardial infarction-Post-hoc analysis from the OMEGA-REMODEL randomized controlled trial.
Kwong RY, Heydari B, Ge Y, Abdullah S, Fujikura K, Kaneko K, Harris WS, Jerosch-Herold M, Antman EM, Seidman JG, Pfeffer MA. Kwong RY, et al. PLoS One. 2019 Sep 18;14(9):e0222061. doi: 10.1371/journal.pone.0222061. eCollection 2019. PLoS One. 2019. PMID: 31532795 Free PMC article. Clinical Trial. - OMEGA, a randomized, placebo-controlled trial to test the effect of highly purified omega-3 fatty acids on top of modern guideline-adjusted therapy after myocardial infarction.
Rauch B, Schiele R, Schneider S, Diller F, Victor N, Gohlke H, Gottwik M, Steinbeck G, Del Castillo U, Sack R, Worth H, Katus H, Spitzer W, Sabin G, Senges J; OMEGA Study Group. Rauch B, et al. Circulation. 2010 Nov 23;122(21):2152-9. doi: 10.1161/CIRCULATIONAHA.110.948562. Epub 2010 Nov 8. Circulation. 2010. PMID: 21060071 Clinical Trial. - Isosorbide Dinitrate, With or Without Hydralazine, Does Not Reduce Wave Reflections, Left Ventricular Hypertrophy, or Myocardial Fibrosis in Patients With Heart Failure With Preserved Ejection Fraction.
Zamani P, Akers S, Soto-Calderon H, Beraun M, Koppula MR, Varakantam S, Rawat D, Shiva-Kumar P, Haines PG, Chittams J, Townsend RR, Witschey WR, Segers P, Chirinos JA. Zamani P, et al. J Am Heart Assoc. 2017 Feb 20;6(2):e004262. doi: 10.1161/JAHA.116.004262. J Am Heart Assoc. 2017. PMID: 28219917 Free PMC article. Clinical Trial. - [Rationale, characteristics and study design of PREAMI (Perindopril and Remodelling in the Elderly with Acute Myocardial Infraction)].
Magrini G, Nicolosi GL, Chiariello M, Ferrari R, Remme P, Tavazzi L. Magrini G, et al. Ital Heart J. 2005 Nov;6 Suppl 7:14S-23S. Ital Heart J. 2005. PMID: 16485513 Review. Italian. - Myocardial infarction and left ventricular remodeling: results of the CEDIM trial. Carnitine Ecocardiografia Digitalizzata Infarto Miocardico.
Colonna P, Iliceto S. Colonna P, et al. Am Heart J. 2000 Feb;139(2 Pt 3):S124-30. doi: 10.1067/mhj.2000.103918. Am Heart J. 2000. PMID: 10650326 Review.
Cited by
- Fabry Disease: Cardiac Implications and Molecular Mechanisms.
Weissman D, Dudek J, Sequeira V, Maack C. Weissman D, et al. Curr Heart Fail Rep. 2024 Apr;21(2):81-100. doi: 10.1007/s11897-024-00645-1. Epub 2024 Jan 30. Curr Heart Fail Rep. 2024. PMID: 38289538 Free PMC article. Review. - The effect of omega-3 polyunsaturated fatty acid intake on blood levels of omega-3s in people with chronic atherosclerotic disease: a systematic review.
Nayda NC, Thomas JM, Delaney CL, Miller MD. Nayda NC, et al. Nutr Rev. 2023 Oct 10;81(11):1447-1461. doi: 10.1093/nutrit/nuad020. Nutr Rev. 2023. PMID: 36882117 Free PMC article. - Genetic profiling of fatty acid desaturase polymorphisms identifies patients who may benefit from high-dose omega-3 fatty acids in cardiac remodeling after acute myocardial infarction-Post-hoc analysis from the OMEGA-REMODEL randomized controlled trial.
Kwong RY, Heydari B, Ge Y, Abdullah S, Fujikura K, Kaneko K, Harris WS, Jerosch-Herold M, Antman EM, Seidman JG, Pfeffer MA. Kwong RY, et al. PLoS One. 2019 Sep 18;14(9):e0222061. doi: 10.1371/journal.pone.0222061. eCollection 2019. PLoS One. 2019. PMID: 31532795 Free PMC article. Clinical Trial. - Is Grassfed Meat and Dairy Better for Human and Environmental Health?
Provenza FD, Kronberg SL, Gregorini P. Provenza FD, et al. Front Nutr. 2019 Mar 19;6:26. doi: 10.3389/fnut.2019.00026. eCollection 2019. Front Nutr. 2019. PMID: 30941351 Free PMC article. - Inflammation in Human Heart Failure: Major Mediators and Therapeutic Targets.
Reina-Couto M, Pereira-Terra P, Quelhas-Santos J, Silva-Pereira C, Albino-Teixeira A, Sousa T. Reina-Couto M, et al. Front Physiol. 2021 Oct 11;12:746494. doi: 10.3389/fphys.2021.746494. eCollection 2021. Front Physiol. 2021. PMID: 34707513 Free PMC article. Review.
References
- Mozaffarian D, Rimm EB. Fish intake, contaminants, and human health: evaluating the risks and the benefits. JAMA. 2006;296:1885–1899. - PubMed
- De Caterina R. n-3 fatty acids in cardiovascular disease. N Engl J Med. 2011;364:2439–2450. - PubMed
- Marchioli R, Barzi F, Bomba E, Chieffo C, Di Gregorio D, Di Mascio R, Franzosi MG, Geraci E, Levantesi G, Maggioni AP, Mantini L, Marfisi RM, Mastrogiuseppe G, Mininni N, Nicolosi GL, Santini M, Schweiger C, Tavazzi L, Tognoni G, Tucci C, Valagussa F, Investigators GI-P. Early protection against sudden death by n-3 polyunsaturated fatty acids after myocardial infarction: time-course analysis of the results of the Gruppo Italiano per lo Studio della Sopravvivenza nell’Infarto Miocardico (GISSI)-Prevenzione. Circulation. 2002;105:1897–1903. - PubMed
- Rauch B, Schiele R, Schneider S, Diller F, Victor N, Gohlke H, Gottwik M, Steinbeck G, Del Castillo U, Sack R, Worth H, Katus H, Spitzer W, Sabin G, Senges J, Group OS. OMEGA, a randomized, placebo-controlled trial to test the effect of highly purified omega-3 fatty acids on top of modern guideline-adjusted therapy after myocardial infarction. Circulation. 2010;122:2152–2159. - PubMed
- Chan W, Duffy SJ, White DA, Gao XM, Du XJ, Ellims AH, Dart AM, Taylor AJ. Acute left ventricular remodeling following myocardial infarction: coupling of regional healing with remote extracellular matrix expansion. JACC Cardiovasc Imaging. 2012;5:884–893. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical