Real-world data reveal a diagnostic gap in non-alcoholic fatty liver disease - PubMed (original) (raw)
doi: 10.1186/s12916-018-1103-x.
A Katrina Loomis 2, Jolyon Fairburn-Beech 1, Johan van der Lei 3, Talita Duarte-Salles 4, Daniel Prieto-Alhambra 5, David Ansell 6, Alessandro Pasqua 7, Francesco Lapi 7, Peter Rijnbeek 3, Mees Mosseveld 3, Paul Avillach 8, Peter Egger 1, Stuart Kendrick 1, Dawn M Waterworth 1, Naveed Sattar 9, William Alazawi 10
Affiliations
- PMID: 30099968
- PMCID: PMC6088429
- DOI: 10.1186/s12916-018-1103-x
Real-world data reveal a diagnostic gap in non-alcoholic fatty liver disease
Myriam Alexander et al. BMC Med. 2018.
Abstract
Background: Non-alcoholic fatty liver disease (NAFLD) is the most common cause of liver disease worldwide. It affects an estimated 20% of the general population, based on cohort studies of varying size and heterogeneous selection. However, the prevalence and incidence of recorded NAFLD diagnoses in unselected real-world health-care records is unknown. We harmonised health records from four major European territories and assessed age- and sex-specific point prevalence and incidence of NAFLD over the past decade.
Methods: Data were extracted from The Health Improvement Network (UK), Health Search Database (Italy), Information System for Research in Primary Care (Spain) and Integrated Primary Care Information (Netherlands). Each database uses a different coding system. Prevalence and incidence estimates were pooled across databases by random-effects meta-analysis after a log-transformation.
Results: Data were available for 17,669,973 adults, of which 176,114 had a recorded diagnosis of NAFLD. Pooled prevalence trebled from 0.60% in 2007 (95% confidence interval: 0.41-0.79) to 1.85% (0.91-2.79) in 2014. Incidence doubled from 1.32 (0.83-1.82) to 2.35 (1.29-3.40) per 1000 person-years. The FIB-4 non-invasive estimate of liver fibrosis could be calculated in 40.6% of patients, of whom 29.6-35.7% had indeterminate or high-risk scores.
Conclusions: In the largest primary-care record study of its kind to date, rates of recorded NAFLD are much lower than expected suggesting under-diagnosis and under-recording. Despite this, we have identified rising incidence and prevalence of the diagnosis. Improved recognition of NAFLD may identify people who will benefit from risk factor modification or emerging therapies to prevent progression to cardiometabolic and hepatic complications.
Keywords: Epidemiology; NAFLD; NASH; Population.
Conflict of interest statement
We followed local data laws in all four territories from which the data were obtained. In all countries, specific ethical approval was not required for this study as it used anonymised data. However, approval was sought and obtained from the scientific research committee for THIN, the IPCI Governing Board (reference 2015/18), the SIDIAP Ethics Committee (reference P15/167) and the scientific committee of the Italian College of General Practitioners and Primary Care.
Not applicable.
MA was contracted to work at, and JFB, PE, SK and DW are employees of, GlaxoSmithKline, which has conducted clinical research including trials of therapeutic agents in NAFLD. AKL is an employee of Pfizer, which is conducting clinical research including trials of therapeutic agents in NAFLD. DPA has received unrestricted research grants from UCB, Amgen and Servier, and consultancy fees (paid to his department or research group) from UCB Pharma. DA has provided consultancy and advice to many pharmaceutical companies on undertaking outcome studies using real-world evidence. FL has provided consultancy tor AlfaSigma, Bayer and Abbvie. PE and SK are employees and stockholders of GlaxoSmithKline. NS has consulted for Boehringer Ingelheim, Eli Lilly, Novo Nordisk and Janssen, and has received grants from Astrazeneca and BI. WA is a consultant and has delivered sponsored lectures to UCB Pharma, Gilead, Intercept and Medimmune. TDS has no conflicts of interest to declare.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
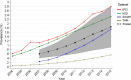
Fig. 1
Point prevalence of NAFLD (per 100 persons) by calendar year. Results are shown for each database and pooled across databases by meta-analysis. The pooled estimate is provided from 2007 only as data from SIDIAP were available only from that year onward. The pooled estimate confidence interval is shaded grey. HSD Health Search Database, IPCI Integrated Primary Care Information, NAFLD non-alcoholic fatty liver disease, SIDIAP Information System for Research in Primary Care, THIN The Health Improvement Network
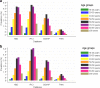
Fig. 2
Point prevalence of NAFLD (per 100 persons) by age group on 1 January 2015 in a males and b females. HSD Health Search Database, IPCI Integrated Primary Care Information, NAFLD non-alcoholic fatty liver disease, SIDIAP Information System for Research in Primary Care, THIN The Health Improvement Network
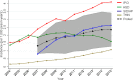
Fig. 3
Incidence of NAFLD (per 1000 person-years) by calendar year in four primary-care databases, and pooled across databases by a random effects meta-analysis. The pooled estimate is provided from 2007 only as data from SIDIAP were available only from that year onward. The pooled estimate confidence interval is shaded grey. HSD Health Search Database, IPCI Integrated Primary Care Information, NAFLD non-alcoholic fatty liver disease, SIDIAP Information System for Research in Primary Care, THIN The Health Improvement Network
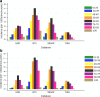
Fig. 4
Incidence of NAFLD (per 1000 person-years) by age group for the four primary care databases for 2015 in a males and b females. HSD Health Search Database, IPCI Integrated Primary Care Information, NAFLD non-alcoholic fatty liver disease, SIDIAP Information System for Research in Primary Care, THIN The Health Improvement Network
Comment in
- Putting non-alcoholic fatty liver disease on the radar for primary care physicians: how well are we doing?
Sanyal AJ. Sanyal AJ. BMC Med. 2018 Aug 24;16(1):148. doi: 10.1186/s12916-018-1149-9. BMC Med. 2018. PMID: 30139362 Free PMC article.
Similar articles
- Non-alcoholic fatty liver disease and risk of incident acute myocardial infarction and stroke: findings from matched cohort study of 18 million European adults.
Alexander M, Loomis AK, van der Lei J, Duarte-Salles T, Prieto-Alhambra D, Ansell D, Pasqua A, Lapi F, Rijnbeek P, Mosseveld M, Avillach P, Egger P, Dhalwani NN, Kendrick S, Celis-Morales C, Waterworth DM, Alazawi W, Sattar N. Alexander M, et al. BMJ. 2019 Oct 8;367:l5367. doi: 10.1136/bmj.l5367. BMJ. 2019. PMID: 31594780 Free PMC article. - Risks and clinical predictors of cirrhosis and hepatocellular carcinoma diagnoses in adults with diagnosed NAFLD: real-world study of 18 million patients in four European cohorts.
Alexander M, Loomis AK, van der Lei J, Duarte-Salles T, Prieto-Alhambra D, Ansell D, Pasqua A, Lapi F, Rijnbeek P, Mosseveld M, Waterworth DM, Kendrick S, Sattar N, Alazawi W. Alexander M, et al. BMC Med. 2019 May 20;17(1):95. doi: 10.1186/s12916-019-1321-x. BMC Med. 2019. PMID: 31104631 Free PMC article. - Estimating global prevalence, incidence, and outcomes of non-alcoholic fatty liver disease from 2000 to 2021: systematic review and meta-analysis.
Liu J, Tian Y, Fu X, Mu C, Yao M, Ni Y, Liu Y, Li Z. Liu J, et al. Chin Med J (Engl). 2022 Jul 20;135(14):1682-1691. doi: 10.1097/CM9.0000000000002277. Chin Med J (Engl). 2022. PMID: 36070463 Free PMC article. - Evolving epidemiology of non-alcoholic fatty liver disease in South Korea: incidence, prevalence, progression, and healthcare implications from 2010 to 2022.
Park JW, Yoo JJ, Lee DH, Chang Y, Jo H, Cho YY, Lee S, Kim LY, Jang JY; Korean Association for the Study of the Liver. Park JW, et al. Korean J Intern Med. 2024 Nov;39(6):931-944. doi: 10.3904/kjim.2024.164. Epub 2024 Oct 24. Korean J Intern Med. 2024. PMID: 39444335 Free PMC article. - Global prevalence of non-alcoholic fatty liver disease and non-alcoholic steatohepatitis in the overweight and obese population: a systematic review and meta-analysis.
Quek J, Chan KE, Wong ZY, Tan C, Tan B, Lim WH, Tan DJH, Tang ASP, Tay P, Xiao J, Yong JN, Zeng RW, Chew NWS, Nah B, Kulkarni A, Siddiqui MS, Dan YY, Wong VW, Sanyal AJ, Noureddin M, Muthiah M, Ng CH. Quek J, et al. Lancet Gastroenterol Hepatol. 2023 Jan;8(1):20-30. doi: 10.1016/S2468-1253(22)00317-X. Epub 2022 Nov 16. Lancet Gastroenterol Hepatol. 2023. PMID: 36400097
Cited by
- Non-alcoholic fatty liver disease and the risk of fibrosis in Italian primary care services: GPS-NAFLD Study: GPS-NAFLD Study.
Miele L, Grattagliano I, Lapi F, Dajko M, De Magistris A, Liguori A, De Matthaeis N, Rossi A, Gasbarrini A, Cricelli C, Grieco A. Miele L, et al. Liver Int. 2022 Dec;42(12):2632-2645. doi: 10.1111/liv.15443. Epub 2022 Oct 18. Liver Int. 2022. PMID: 36169605 Free PMC article. - Regulatory Networks, Management Approaches, and Emerging Treatments of Nonalcoholic Fatty Liver Disease.
Yang B, Yang X, Tan X, Lu L, Fan W, Barbier-Torres L, Steggerda J, Liu T, Yang H. Yang B, et al. Can J Gastroenterol Hepatol. 2022 Nov 8;2022:6799414. doi: 10.1155/2022/6799414. eCollection 2022. Can J Gastroenterol Hepatol. 2022. PMID: 36397950 Free PMC article. Review. - Management of nonalcoholic fatty liver disease in the Middle East.
Sanai FM, Abaalkhail F, Hasan F, Farooqi MH, Nahdi NA, Younossi ZM. Sanai FM, et al. World J Gastroenterol. 2020 Jul 7;26(25):3528-3541. doi: 10.3748/wjg.v26.i25.3528. World J Gastroenterol. 2020. PMID: 32742124 Free PMC article. Review. - Clinical and economic burden of nonalcoholic steatohepatitis in Saudi Arabia, United Arab Emirates and Kuwait.
Sanai FM, Al Khathlan A, Al Fadhli A, Jazzar AS, Hashim AM, Mansour E, Abaalkhail F, Hasan F, Al Mudaiheem H, Al Quraishi H, Bottomley J, Alswat KA, Al Ghamdi M, Farghaly M, Fathy M, Awad N, Mohamed O, Kozma S, Al-Hamoudi W, Al-Jedai A. Sanai FM, et al. Hepatol Int. 2021 Aug;15(4):912-921. doi: 10.1007/s12072-021-10182-x. Epub 2021 Apr 6. Hepatol Int. 2021. PMID: 33822317 Free PMC article. - Fatty liver index as a predictor of increased risk of cardiometabolic disease: finding from the Kuopio Ischaemic Heart Disease Risk Factor Study Cohort.
Olubamwo OO, Virtanen JK, Pihlajamaki J, Mantyselka P, Tuomainen TP. Olubamwo OO, et al. BMJ Open. 2019 Sep 5;9(9):e031420. doi: 10.1136/bmjopen-2019-031420. BMJ Open. 2019. PMID: 31492793 Free PMC article.
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous