Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study - PubMed (original) (raw)
. 2020 Feb 15;395(10223):507-513.
doi: 10.1016/S0140-6736(20)30211-7. Epub 2020 Jan 30.
Min Zhou 2, Xuan Dong 1, Jieming Qu 2, Fengyun Gong 3, Yang Han 4, Yang Qiu 5, Jingli Wang 3, Ying Liu 6, Yuan Wei 1, Jia'an Xia 1, Ting Yu 1, Xinxin Zhang 7, Li Zhang 8
Affiliations
- PMID: 32007143
- PMCID: PMC7135076
- DOI: 10.1016/S0140-6736(20)30211-7
Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study
Nanshan Chen et al. Lancet. 2020.
Abstract
Background: In December, 2019, a pneumonia associated with the 2019 novel coronavirus (2019-nCoV) emerged in Wuhan, China. We aimed to further clarify the epidemiological and clinical characteristics of 2019-nCoV pneumonia.
Methods: In this retrospective, single-centre study, we included all confirmed cases of 2019-nCoV in Wuhan Jinyintan Hospital from Jan 1 to Jan 20, 2020. Cases were confirmed by real-time RT-PCR and were analysed for epidemiological, demographic, clinical, and radiological features and laboratory data. Outcomes were followed up until Jan 25, 2020.
Findings: Of the 99 patients with 2019-nCoV pneumonia, 49 (49%) had a history of exposure to the Huanan seafood market. The average age of the patients was 55·5 years (SD 13·1), including 67 men and 32 women. 2019-nCoV was detected in all patients by real-time RT-PCR. 50 (51%) patients had chronic diseases. Patients had clinical manifestations of fever (82 [83%] patients), cough (81 [82%] patients), shortness of breath (31 [31%] patients), muscle ache (11 [11%] patients), confusion (nine [9%] patients), headache (eight [8%] patients), sore throat (five [5%] patients), rhinorrhoea (four [4%] patients), chest pain (two [2%] patients), diarrhoea (two [2%] patients), and nausea and vomiting (one [1%] patient). According to imaging examination, 74 (75%) patients showed bilateral pneumonia, 14 (14%) patients showed multiple mottling and ground-glass opacity, and one (1%) patient had pneumothorax. 17 (17%) patients developed acute respiratory distress syndrome and, among them, 11 (11%) patients worsened in a short period of time and died of multiple organ failure.
Interpretation: The 2019-nCoV infection was of clustering onset, is more likely to affect older males with comorbidities, and can result in severe and even fatal respiratory diseases such as acute respiratory distress syndrome. In general, characteristics of patients who died were in line with the MuLBSTA score, an early warning model for predicting mortality in viral pneumonia. Further investigation is needed to explore the applicability of the MuLBSTA score in predicting the risk of mortality in 2019-nCoV infection.
Funding: National Key R&D Program of China.
Copyright © 2020 Elsevier Ltd. All rights reserved.
Figures
Figure
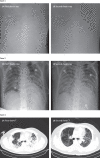
Chest x-rays and chest CTs of three patients Case 1: chest x-ray was obtained on Jan 1 (1A). The brightness of both lungs was diffusely decreased, showing a large area of patchy shadow with uneven density. Tracheal intubation was seen in the trachea and the heart shadow outline was not clear. The catheter shadow was seen from the right axilla to the mediastinum. Bilateral diaphragmatic surface and costal diaphragmatic angle were not clear, and chest x-ray on Jan 2 showed worse status (1B). Case 2: chest x-ray obtained on Jan 6 (2A). The brightness of both lungs was decreased and multiple patchy shadows were observed; edges were blurred, and large ground-glass opacity and condensation shadows were mainly on the lower right lobe. Tracheal intubation could be seen in the trachea. Heart shadow roughly presents in the normal range. On the left side, the diaphragmatic surface is not clearly displayed. The right side of the diaphragmatic surface was light and smooth and rib phrenic angle was less sharp. Chest x-ray on Jan 10 showed worse status (2B). Case 3: chest CT obtained on Jan 1 (3A) showed mass shadows of high density in both lungs. Bright bronchogram is seen in the lung tissue area of the lesion, which is also called bronchoinflation sign. Chest CT on Jan 15 showed improved status (3B).
Comment in
- High-resolution computed tomography features of 17 cases of coronavirus disease 2019 in Sichuan province, China.
Zhang S, Li H, Huang S, You W, Sun H. Zhang S, et al. Eur Respir J. 2020 Apr 30;55(4):2000334. doi: 10.1183/13993003.00334-2020. Print 2020 Apr. Eur Respir J. 2020. PMID: 32139463 Free PMC article. - Initial Experience of an Emergency Department in Shenzhen in Responding to the Emerging Wuhan Coronavirus Pneumonia.
Lu KL, Chen S, Leung LP. Lu KL, et al. Ann Emerg Med. 2020 Apr;75(4):556. doi: 10.1016/j.annemergmed.2020.02.006. Ann Emerg Med. 2020. PMID: 32216893 Free PMC article. No abstract available. - Impact of COVID-19: perspectives from gastroenterology.
Tay SW, Teh KKJ, Wang LM, Ang TL. Tay SW, et al. Singapore Med J. 2020 Sep;61(9):460-462. doi: 10.11622/smedj.2020051. Epub 2020 Apr 13. Singapore Med J. 2020. PMID: 32279480 Free PMC article. No abstract available. - Multicenter analysis of clinical characteristics and outcomes in patients with COVID-19 who develop liver injury.
Qi X, Liu C, Jiang Z, Gu Y, Zhang G, Shao C, Yue H, Chen Z, Ma B, Liu D, Zhang L, Wang J, Xu D, Lei J, Li X, Huang H, Wang Y, Liu H, Yang J, Pan H, Liu W, Wang W, Li F, Zou S, Zhang H, Dong J. Qi X, et al. J Hepatol. 2020 Aug;73(2):455-458. doi: 10.1016/j.jhep.2020.04.010. Epub 2020 Apr 17. J Hepatol. 2020. PMID: 32305291 Free PMC article. No abstract available. - Mitochondrial oxidative stress, mitochondrial ROS storms in long COVID pathogenesis.
Noonong K, Chatatikun M, Surinkaew S, Kotepui M, Hossain R, Bunluepuech K, Noothong C, Tedasen A, Klangbud WK, Imai M, Kawakami F, Kubo M, Kitagawa Y, Ichikawa H, Kanekura T, Sukati S, Somsak V, Udomwech L, Ichikawa T, Nissapatorn V, Tangpong J, Indo HP, Majima HJ. Noonong K, et al. Front Immunol. 2023 Dec 22;14:1275001. doi: 10.3389/fimmu.2023.1275001. eCollection 2023. Front Immunol. 2023. PMID: 38187378 Free PMC article. Review.
Similar articles
- Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China.
Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, Zhang L, Fan G, Xu J, Gu X, Cheng Z, Yu T, Xia J, Wei Y, Wu W, Xie X, Yin W, Li H, Liu M, Xiao Y, Gao H, Guo L, Xie J, Wang G, Jiang R, Gao Z, Jin Q, Wang J, Cao B. Huang C, et al. Lancet. 2020 Feb 15;395(10223):497-506. doi: 10.1016/S0140-6736(20)30183-5. Epub 2020 Jan 24. Lancet. 2020. PMID: 31986264 Free PMC article. - Epidemiological and clinical characteristics of coronavirus disease (COVID-19) cases at a screening clinic during the early outbreak period: a single-centre study.
Khan M, Khan H, Khan S, Nawaz M. Khan M, et al. J Med Microbiol. 2020 Aug;69(8):1114-1123. doi: 10.1099/jmm.0.001231. J Med Microbiol. 2020. PMID: 32783802 Free PMC article. - Epidemiological and clinical characteristics of 1663 hospitalized patients infected with COVID-19 in Wuhan, China: a single-center experience.
Yu C, Lei Q, Li W, Wang X, Li W, Liu W. Yu C, et al. J Infect Public Health. 2020 Sep;13(9):1202-1209. doi: 10.1016/j.jiph.2020.07.002. Epub 2020 Jul 17. J Infect Public Health. 2020. PMID: 32718894 Free PMC article. - Maternal and infant outcomes of full-term pregnancy combined with COVID-2019 in Wuhan, China: retrospective case series.
Chen Y, Bai J. Chen Y, et al. Arch Gynecol Obstet. 2020 Sep;302(3):545-551. doi: 10.1007/s00404-020-05573-8. Epub 2020 Jul 21. Arch Gynecol Obstet. 2020. PMID: 32696241 Free PMC article. Review. - Clinical Characteristics and Morbidity Associated With Coronavirus Disease 2019 in a Series of Patients in Metropolitan Detroit.
Suleyman G, Fadel RA, Malette KM, Hammond C, Abdulla H, Entz A, Demertzis Z, Hanna Z, Failla A, Dagher C, Chaudhry Z, Vahia A, Abreu Lanfranco O, Ramesh M, Zervos MJ, Alangaden G, Miller J, Brar I. Suleyman G, et al. JAMA Netw Open. 2020 Jun 1;3(6):e2012270. doi: 10.1001/jamanetworkopen.2020.12270. JAMA Netw Open. 2020. PMID: 32543702 Free PMC article. Review.
Cited by
- Isolation, identification, and challenges of extracellular vesicles: emerging players in clinical applications.
Ma X, Peng L, Zhu X, Chu T, Yang C, Zhou B, Sun X, Gao T, Zhang M, Chen P, Chen H. Ma X, et al. Apoptosis. 2024 Nov 10. doi: 10.1007/s10495-024-02036-2. Online ahead of print. Apoptosis. 2024. PMID: 39522104 Review. - Evaluation of the Relationship between Early Clinical Manifestations and Changes in Biochemical, Inflammatory, and Coagulation Parameters and the Prognosis of Pregnant Women with COVID-19 Admitted to the ICU.
Ebrahim Babai M, Kabiri A, Movahedi M, Ghahiri A, Hajhashemi M, Dehghan M. Ebrahim Babai M, et al. Adv Biomed Res. 2024 Sep 23;13:76. doi: 10.4103/abr.abr_257_23. eCollection 2024. Adv Biomed Res. 2024. PMID: 39512403 Free PMC article. - Clinical and Epidemiological Features of Pediatric COVID-19: A Retrospective Study.
Mirkarimi M, Heidari S, Shamsizadeh A, Tahouri K, Alisamir M, Fathi M, Mohammadi S. Mirkarimi M, et al. Health Sci Rep. 2024 Nov 6;7(11):e70181. doi: 10.1002/hsr2.70181. eCollection 2024 Nov. Health Sci Rep. 2024. PMID: 39512246 Free PMC article. - Risk factors affecting the development of pneumothorax in patients followed up in intensive care with a diagnosis of COVID-19.
Turan YB. Turan YB. BMC Infect Dis. 2024 Nov 5;24(1):1243. doi: 10.1186/s12879-024-10147-z. BMC Infect Dis. 2024. PMID: 39501177 Free PMC article. - Immunopathological markers and cell types linked to COVID-19 symptom manifestation.
Song HW, Jo HY, Kim SC, Choi SS. Song HW, et al. BMC Infect Dis. 2024 Nov 4;24(1):1237. doi: 10.1186/s12879-024-10139-z. BMC Infect Dis. 2024. PMID: 39497098 Free PMC article.
References
- WHO Clinical management of severe acute respiratory infection when Novel coronavirus (nCoV) infection is suspected: interim guidance. Jan 11, 2020. https://www.who.int/internal-publications-detail/clinical-management-of-...
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources