ACE Inhibitor Benefit to Kidney and Cardiovascular Outcomes for Patients with Non-Dialysis Chronic Kidney Disease Stages 3-5: A Network Meta-Analysis of Randomised Clinical Trials - PubMed (original) (raw)
ACE Inhibitor Benefit to Kidney and Cardiovascular Outcomes for Patients with Non-Dialysis Chronic Kidney Disease Stages 3-5: A Network Meta-Analysis of Randomised Clinical Trials
Yaru Zhang et al. Drugs. 2020 Jun.
Abstract
Background: The advantages of angiotensin-converting enzyme inhibitors (ACEIs) or angiotensin II receptor blockers (ARBs) in reducing risk of cardiovascular events (CVEs) and delaying end-stage kidney disease (ESKD) in patients with chronic kidney disease (CKD) is well-known. However, the efficacy and safety of these agents in non-dialysis CKD stages 3-5 patients are still a controversial issue.
Methods: Two investigators (Yaru Zhang and Dandan He) independently searched and identified relevant studies from MEDLINE (from 1950 to October 2018), EMBASE (from 1970 to October 2018), and the Cochrane Library database. Randomised clinical trials in non-dialysis CKD3-5 patients treated with renin-angiotensin system (RAS) inhibitors were included. We used standard criteria (Cochrane risk of bias tool) to assess the inherent risk of bias of trials. We calculated the odds ratio (OR) and 95% confidence interval (CI) for each outcome by random-effects model. A 2-sided p value < 0.05 was considered statistically significant, and all statistical analyses were performed using STATA, version 15.0. This network meta-analysis was undertaken by the frequency model.
Results: Forty-four randomised clinical trials with 42,319 patients were included in our network meta-analysis. ACEIs monotherapy significantly decreased the odds of kidney events (OR 0.54, 95% CI 0.41-0.73), cardiovascular events (OR 0.73, 95% CI 0.64-0.84), cardiovascular death (OR 0.73, 95% CI 0.63-0.86) and all-cause death (OR 0.77, 95% CI 0.66-0.91) when compared to placebo. According to the cumulative ranking area (SUCRA), ACEI monotherapy had the highest probabilities of their protective effects on outcomes of kidney events (SUCRA 93.3%), cardiovascular events (SUCRA 77.2%), cardiovascular death (SUCRA 86%), and all-cause death (SUCRA 94.1%), even if there were no significant differences between ACEIs and other antihypertensive drugs, including calcium channel blockers (CCBs), β-blockers and diuretics on above outcomes except for kidney events. ARB monotherapy and combination therapy of an ACEI plus an ARB showed no more advantage than CCBs, β-blockers and diuretics in all primary outcomes. In the subgroup of non-dialysis diabetic kidney disease patients, no drugs, including ACEIs or ARBs, significantly lowered the odds of cardiovascular events and all-cause death. However, ACEIs were still better than other antihypertensive drugs including ARBs in all-cause death but not ARBs in cardiovascular events according to the SUCRA. Only ARBs had significant differences in preventing the occurrence of kidney events compared with placebo (OR 0.82, 95% CI 0.72-0.95). Both ACEI/ARB monotherapy and combination therapy had higher odds of hyperkalaemia. ACEIs had 3.81 times higher odds than CCBs (95% CI 1.58-9.20), ARBs had 2.08-5.10 times higher odds than placebo and CCBs and combination therapy of an ACEI and an ARB had 4.80-24.5 times higher odds than all other treatments. Compared with placebo, CCBs and β blockers, ACEI therapy significantly increased the odds of cough (OR 2.90, 95% CI 1.76-4.77; OR 8.21, 95% CI 3.13-21.54 and OR 1.80, 95% CI 1.08-3.00). There were no statistical differences in hypotension among all comparisons except ACEIs versus placebo.
Conclusions: Although ACEIs increased the odds of hyperkalaemia, cough and hypotension, they were still superior to ARBs and other antihypertensive drugs and had the highest benefits for the prevention of kidney events, cardiovascular outcomes, cardiovascular death and all-cause mortality in non-dialysis CKD3-5 patients. In patients with advanced diabetic kidney disease, ACEIs were superior to ARBs in lowering risk of all-cause death but not in kidney events and cardiovascular events.
Conflict of interest statement
Yaru Zhang, Dandan He, Wei Zhang, Yue Xing, Yipeng Guo, Fuzhen Wang, Junya Jia, Tiekun Yan, Youxia Liu and Shan Lin declare no conflict of interest.
Figures
Fig. 1
Process for identifying studies eligible for the meta-analysis
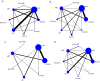
Fig. 2
Network of eligible treatment comparisons for a kidney events, b cardiovascular events, c cardiovascular death, and d all-cause death
Fig. 3
Network of adverse events comparisons: a hyperkalaemia b cough c oedema d hypotension
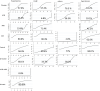
Fig. 4
Forest plot for results of primary outcomes: a kidney events, b cardiovascular events, c cardiovascular death, and d all-cause death
Fig. 5
Summary of results from network meta-analysis (on the upper triangle) and traditional pairwise meta-analysis (on the lower triangle) on primary outcomes: a kidney events, b cardiovascular events, c cardiovascular death, and d all-cause death. On the lower triangle and upper triangle, the row-defining treatment is compared with the column-defining treatment, and ORs of < 1 favour the row-defining treatment. Significant results are shown in boldface type
Fig. 6
Ranking of treatment strategies based on probability of their protective effects on outcomes of kidney events, cardiovascular events, cardiovascular death, and all-cause death according to the cumulative ranking area (SUCRA). Larger probability, stronger protective effects
Fig. 7
Forest plot for results of adverse events comparisons: a hyperkalaemia b cough c hypotension d oedema
Fig. 8
Ranking of treatment strategies based on probability of their protective effects on outcomes of for hyperkalaemia, cough, oedema and hypotension according to the cumulative ranking area (SUCRA). Larger probability, stronger protective effects
References
- Weiner DE, Tighiouart H, Amin MG, et al. Chronic kidney disease as a risk factor for cardiovascular disease and all-cause mortality: a pooled analysis of community-based studies. J Am Soc Nephrol. 2004;15(5):1307–1315. - PubMed
- Tonelli M, Wiebe N, Culleton B, et al. Chronic kidney disease and mortality risk: a systematic review. J Am Soc Nephrol. 2006;17(7):2034–2047. - PubMed
- Go AS, Chertow GM, Fan D, McCulloch CE, Hsu CY. Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Engl J Med. 2004;351(13):1296–1305. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
- 81600553/the National Natural Science Foundation
- 81270791/the National Natural Science Foundation
- 30800529/the National Natural Science Foundation
- 14JCYBJC27900/Tianjin Municipal Science and Technology Commission Foundation
- 2014KR16/Tianjin Public Health Bureau Foundation
- No. 2011BAI10B02/National Science and Technology Program during the Twelfth Five-year Plan Period
- 201302051/Shanxi Public Health Bureau Foundation
- ZYYFY2015001/General Hospital of Tianjin Medical University Youth Incubation Foundation
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous