Parent and Provider Perspectives on Recently Incarcerated Youths’ Access to Healthcare During Community Reentry (original) (raw)
. Author manuscript; available in PMC: 2021 May 25.
Abstract
Incarcerated youth have numerous healthcare needs, yet access to healthcare following community reentry is limited. Healthcare and juvenile justice providers, along with parents, strongly influence access to care for youth undergoing reentry. However, their perspectives are often missing from the literature. We examined parent and provider perspectives on youths’ access to healthcare during community reentry. We conducted 72 longitudinal interviews with parents of youth undergoing reentry (n= 34 parents) and cross-sectional interviews with health and juvenile justice providers (n=20 providers). We performed inductive analysis of interview transcripts to identify the major themes related to access to healthcare during reentry. Respondents identified key leverage points that influence access to healthcare along the spectrum of individual, community, and policy-level factors. Parent and provider perspectives demonstrated substantial overlap, strongly concurring on the essential role of parents in linking youth to care and the external factors that limit parents’ ability to connect youth to care. However, providers discussed parents not buying-in to treatment plans as a barrier to care, and parents uniquely described feeling powerless when their children were not motivated to receive care. Parents and providers agreed on priority solutions for improving care access during reentry. Immediate solutions centered on: 1) increasing reliability and continuity of providers, 2) providing free or low-cost transportation to healthcare visits, and 3) eliminating gaps in Medicaid coverage post-incarceration. Findings also signal the broader need to pursue strategies that increase family engagement in healthcare during reentry. In doing so, health and juvenile justice providers can partner with parents to overcome barriers to healthcare for youth during reentry.
Keywords: juvenile justice, incarcerated youth, reentry, aftercare, healthcare access
1. Background and Significance
In 2016, 66,000 youth were court mandated to United States (U.S.) juvenile justice residential facilities (National Center for Juvenile Justice, 2017), many of whom had critical medical and psychiatric needs (Barnert, Perry, & Morris, 2016). Researchers have estimated that up to seventy-five percent of incarcerated youth have at least one diagnosable psychiatric condition (Teplin, Abram, McClelland, Dulcan, & Mericle, 2002). One-third of incarcerated youth report recent suicidal thoughts, and 1 in 10 have prior suicide attempts (Abram et al., 2008). Further, the risk of death from homicide or suicide is four-times higher than non-justice-involved peers (Teplin, McClelland, Abram, & Mileusnic, 2005).
Given the high morbidity and mortality rates for incarcerated youth and the negative health impacts of incarceration (Barnert et al., 2017), timely access to community health services following release is vital. The reentry period, defined as the six-month period when incarcerated youth transition from juvenile correctional facilities back to their communities, signifies a critical juncture for justice-involved youth (Altschuler & Brash, 2004). Recidivism rates are high (Annie E. Casey Foundation, 2013) and youth with behavioral health conditions have the highest risk of re-arrest (Schubert & Mulvey, 2014). Although the prevalence and severity of behavioral health disorders predicts re-arrest and less time attending school or work (Piquero, Monahan, Glasheen, Schubert, & Mulvey, 2013), the peer-reviewed literature on youth reentry has largely overlooked health and healthcare needs.
Access to healthcare, especially behavioral and reproductive health services, may be critical for youths’ health and well-being during reentry (Burns, Schoenwald, Burchard, Faw, & Santos, 2000). For example, access to mental health services during reentry can increase success in enrolling in school and obtaining employment (Burns et al., 2000), and reproductive care can reduce unplanned pregnancies (Barnert et al., 2019). All youth, by federal law, are guaranteed access to healthcare when detained (Golzari, Hunt, & Chamberlain, 2008); however, many lack access to care once released (Golzari & Kuo, 2013). Youth may have benefited from correctional healthcare received in detention, but the extent to which benefits can be sustained require that they stay connected to care. The question remains, how can policies and practices support youths’ crucial linkages to community health systems?
The health literature has yet to hone in on the specific barriers or facilitators that influence youths’ access to healthcare during reentry. The limited research in this area has used youth surveys and identified lack of insurance or unaffordability of co-payments as the most common barrier, followed by lack of transportation, and lack of parent accompaniment to health visits (Golzari & Kuo, 2013; Barnert et al., 2019). Studies that capture youths’ perspectives have also identified youths’ lack of interest in obtaining formal healthcare support during reentry (Fields & Abrams, 2010; Golzari & Kuo, 2013). A qualitative study on barriers to community healthcare for adjudicated youth included interviews with five individual service providers. The study delineated individual-level barriers to care and similarly identified youth disinterest in healthcare as a barrier. It also highlighted youth distrust of providers or fear of healthcare, in addition to structural barriers, such as difficulties with scheduling and long wait times for appointments (Udell, Mohammed, & Breland, 2017).
Finally, another qualitative study about connections to mental healthcare during reentry examined youth-caregiver dyads and described the key barrier of parents being out of the loop about diagnoses and care plans youth received while incarcerated (Aalsma, Brown, Holloway, & Ott, 2014). This finding suggests the important role of parents in linking youth to care during reentry. To our knowledge, this is the only prior study examining barriers to care for recently incarcerated youth that includes the perspectives of service providers.
Given adolescents’ reliance on parents to facilitate healthcare access, parent perspectives may be critical to understanding solutions for overcoming barriers to care during reentry. Further, a broad array of factors influences healthcare access during reentry, and youth interface with many agencies upon release. The various types of professionals who interact with these youth possess unique insight into youths’ community healthcare access. However, the extent to which parent and provider perspectives on barriers to care during reentry converge versus diverge remains unclear. Each has a valuable vantage point that may be able to uniquely understand and influence youths’ care access during reentry. Therefore, from the perspectives of parents and providers, we sought to answer: 1) What leverage points influence youths’ healthcare access during reentry? and 2) How can we optimize youths’ access to care during reentry? Throughout these responses, we also consider the convergence and divergence of parent and provider perspectives.
2. Theoretical Frame
The Social Ecological Model (SEM) provides a framework for understanding the multilevel, interactive effects of leverage points that influence healthcare access during reentry, over five nested, hierarchical levels: the individual, interpersonal, community, organizational, and policy or enabling environment (CDC, 2015). The individual level represents the young person themself, whose behavior is affected by their own knowledge, attitude, feelings, and values. At the interpersonal level, youth are influenced by their network of friends, families, providers, and other social supports. The community level constitutes the relationships among organizations and institutions, including the youth’s neighborhood and its associations, schools, businesses, and transportation. The organizational level refers to the systems, policies, rules, and regulations of social institutions that affect how healthcare services are provided to the youth. At the policy level, youth are affected by laws and policies recognized by society and government.
3. Method
3.1. Study Purpose
The study intended to obtain a broad view of parents’ as well as health and juvenile justice providers’ perceived leverage points for influencing youth healthcare access during youth reentry, including factors acting as barriers or facilitators to care. By honing in on modifiable leverage points, we sought to develop a roadmap for policy and systems change to improve care access. We examined medical and behavioral healthcare because justice-involved youth often have health needs that span various types of providers, healthcare delivery to the youth is often scattered and difficult to navigate, and barriers across healthcare settings often overlap (Barnert, Perry, & Morris, 2016).
3.2. Design and Setting
We conducted this qualitative interview study in partnership with a large, metropolitan, southwestern juvenile justice system. Our university IRB and the county juvenile court approved all study procedures.
In this large southwestern county, a prior study (n=1,102) found that approximately 95% of incarcerated youth in the study region were racial/ethnic minorities--65% Hispanic, 30% African-American, and 5% Caucasian/other; 10% females (Herz et al., 2015). The average age at arrest for youth was 15 years, and the vast majority were from low-income families. Moreover, 92% had received behavioral health diagnoses from the county department of mental health, including 50% with diagnosed substance abuse disorders (Herz et al., 2015). Upon release, most youth are released on probation supervision and are referred to a variety of health service agencies across the county.
3.3. Participants and Data Collection
We used two separate purposive sampling frames for the parent and provider interviews, both from the same metropolitan, southwestern juvenile justice agency, between 2016-2017. Sampling approaches are described below.
3.3.1. Parent Interviews
For the parent/caregiver interviews, caregivers of youth returning home from juvenile correctional institutions in the focal county were eligible for study participation. Parents/caregivers had to be fluent in English or Spanish and able to provide verbal consent. The parent/caregiver interviews were situated in a larger mixed methods study on reentry and health, which had a youth survey response rate of 44% (Barnert et al., 2019). This response rate is consistent with prior studies involving juvenile justice-involved youth (Abrams, 2010).
Families received a study flyer with the youth’s release paperwork and were invited to contact the study team. With rigorous permissions in place, study team members also recruited parents to participate based on contact information obtained from probation of youth releases from incarceration the week prior. Consent/assent discussions occurred by telephone. Team members emphasized the confidential, voluntary nature of the study, and the independence of the study from the justice system. Caregivers were provided a $30 gift card for the completion of each interview.
At one, three, and six months after the youth’s incarceration, caregivers completed confidential, qualitative interviews about healthcare access during reentry. We initially invited all caregivers to participate and then purposively oversampled fathers to obtain fathers’ perspectives because we more readily encountered mothers in our recruitment efforts. All caregivers who we reached and invited to participate agreed to be interviewed.
Semi-structured interviews examined caregiver views about youths’ health and experiences accessing (or not accessing) care since returning home from incarceration (see Appendix A: Parent Interview Guide). We conducted interviews at the timing and location of participants’ preferences; 20% of the interviews occurred in person and 80% via telephone. Youth were not present during the parent interviews. Interviews lasted 30-60 minutes and were digitally recorded.
In total, 34 caregivers participated in 52 longitudinal interviews at 1, 3, and 6 months following the youth’s release from a county juvenile correctional facility. Caregivers identified their race/ethnicity as follows: 32% African-American, 62% Latino, and 6% Mixed. Most (85%) were female. Approximately half (53%) of the interviews were conducted in Spanish. Spanish interviews were conducted by a native Spanish speaker and then transcribed and coded in Spanish. Caregivers were 82% mothers, 15% fathers, and 3% grandmothers. We will henceforth use the term “parent” for simplicity as the vast majority of caregivers were mothers or fathers.
3.3.2. Provider Interviews
For provider interviews, we used purposive sampling to identify key stakeholders with expertise in juvenile justice and healthcare. We primarily focused on community and correctional healthcare providers and healthcare leaders. The sampling was expanded to include providers in the juvenile justice system with knowledge and experiences in the additional fields known to impact health for all youth during reentry--the education, probation, and judicial systems. In addition to clinicians, we sought individuals with leadership roles who could provide a broad perspective. Categories included: 1) mental health and physical correctional health leaders; 2) leadership and health providers in community pediatrics, reproductive health-focused, mental health, and substance use treatment centers known to serve a high proportion of justice-involved youth; 3) leadership in the correctional education system and the large county public school district; and 4) leadership in the juvenile probation and court system.
To achieve the purposive sampling goals, the research team generated a list of potential nominees for interviews through contacts with correctional medical and mental health leadership within the juvenile justice system that the lead author developed through prior research. We supplemented the list with snowball sampling to include two probation leaders, one judge, and one correctional education leader, each with identified expertise on reentry. Participating juvenile justice and correctional health leaders then nominated community healthcare providers known to take care of a high volume of youth undergoing reentry. We looked for the division heads or, in the case of large entities, sought leaders overseeing reentry activities.
Potential participants received an email inviting them to participate in the study. All invited individuals agreed to participate and/or referred us to another individual within their agency; thus, 100% of the invited agencies agreed to participate. Several participants had both administrative leadership and direct provider roles. In total, 20 individuals participated. The breakdown of participants, by stakeholder group was: six community healthcare professionals (including at least one representative from a medical, behavioral health, and reproductive health clinic); four correctional mental healthcare professionals; four correctional medical professionals; two judicial professionals; two education professionals (one from the probation school system and one from the public school district); one probation representative; and one health professional from a national entity overseeing quality of correctional healthcare.
Participants completed a confidential, semi-structured interview over the telephone, each lasting approximately 30-45 minutes. The semi-structured interview guide probed providers’ perspectives on leverage points that influence healthcare access during reentry and recommendations for improving care access (see Appendix B: Provider Interview Guide). Interviews were audio-recorded and transcribed by a professional transcription service.
3.4. Data Analysis
We used six-step thematic analysis for the parent and provider interviews. We applied the Social Ecological Model to guide the conceptualization and organization of themes (CDC, 2015). First, the research team met several times to develop an initial codebook for the parent interviews. We then refined the codebook using iterative thematic analysis, following the advice of Braun and Clarke (2006). Once the team reached consensus on the codebook, two team members independently coded the parent transcripts using Atlas.Ti software. A third coder resolved coding disagreements. We discussed emergent themes in regular research meetings, during which we organized the codes into themes and applied definitions to the themes. We paid specific attention to whether participants viewed the current operation of each identified lever as “open” (i.e., facilitating access to care) or “closed” (i.e., creating a barrier to care), as well as the extent to which respondents viewed levers as modifiable. We then repeated this process with the provider interview transcripts, allowing for comparisons between the parent and provider perspectives. We continued interviews until we reached and surpassed saturation of themes about barriers to care (Bowen, 2008).
4. Results
4.1. Concordance between Parent and Provider Perspectives
Overall, parents and providers agreed that parents play a crucial role in influencing whether or not youth connect to care during reentry (“It’s really up to the parents”). One parent stated, “When parents fall short… it’s kind of hopeless for the kids.” Providers and parents described external factors that influence the extent to which parents can support youth with accessing care, such as parents facing competing demands (“Our families are struggling and have a lot of stuff going on”) in the context of difficult-to-navigate healthcare settings.
Both providers and parents attributed some blame to parents for their role when healthcare falls through the cracks. One provider commented, “Many times, the parents don’t really understand or prioritize [healthcare].” Although parents did not blame themselves as individuals for youth not connecting to care, they mirrored the perspectives of the providers in that they spoke generally about other parents who fail to link youth to care during reentry. For example, parents stated, “Some parents really don’t care” or, because of life stressors, “they forget to engage in their children’s lives.” Thus, both parents and providers described a degree of failed responsibility on the part of some parents with regards to linking youth to care during reentry.
Parents and providers diverged on the issue of treatment engagement, referring to acceptance and buy-in of a treatment plan. Providers, as compared to parents, tended to blame parents for sometimes not buying-in to treatment plans, which they believed caused youth to disengage from treatment. Whereas providers discussed the perceived problem of parents not buying-in to mental health treatment plans, especially regarding the use of psychotropic medications, parents did not view lack of parental buy-in to mental health treatment as a barrier to care.
Additionally, both parents and providers discussed the importance of youth motivation to receive care for promoting successful linkages and engagement during reentry. As one provider stated, “Some parents do want to help their child, but the child’s not letting them help them.” Parents, as compared to providers, uniquely described feeling powerless when their children did not want to receive care. As one parent stated, “If he’s not willing to accept the fact that he has ADHD, he’s not willing to take the medication, then how can anything that’s at his disposal help him?”
Parents, as compared to providers, generally had a deeper insight into the competing priorities and mindset of the youth when making decisions regarding healthcare access during reentry. Additionally, while parents and providers agreed on the importance of minimizing fragmentation of care, in addition to continuity of providers, parents highlighted the importance of reliable providers who show up to scheduled clinic or home therapy sessions. Although parents were interviewed longitudinally during the reentry period (and providers interviewed only once), parents’ perspectives towards the leverage points remained consistent across interviews.
The themes below summarize the parent and providers perspectives on leverage points that influence access to healthcare during youth reentry. Parents and providers demonstrated agreement about solutions to prioritize for improving youths’ linkages to care during reentry, which are also summarized below.
4.2. Leverage Points that Influence Youths’ Access to Care (Figure 1)
Figure 1:
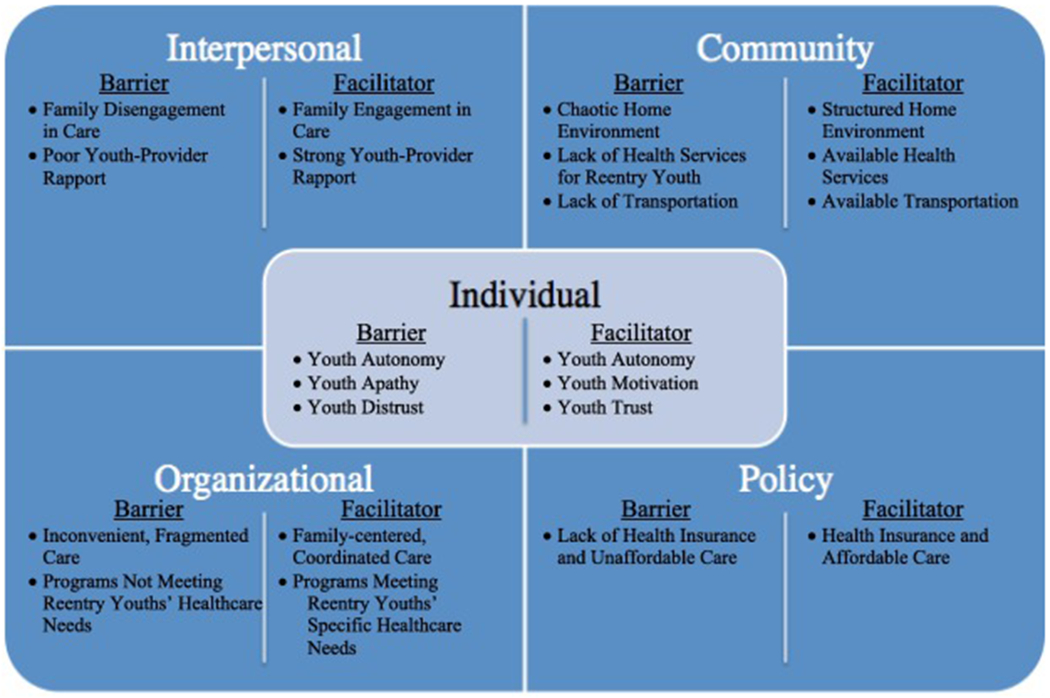
Leverage Points Operating as Facilitators or Barriers for Youths’ Access to Care During Community Reentry
At each level of the SEM, leverage points that influence access to care emerged from the interviews and were analyzed in terms of the factors at play as well as the extent to which that lever created a gateway that was open (i.e., functioning as a facilitator) versus closed (i.e., functioning as a barrier). Table 1 summarizes the leverage points across the SEM model.
Table 1.
Leverage Points for Youths’ Access to Care During Community Reentry
| Leverage Point | Quotes | |
|---|---|---|
| INDIVIDUAL LEVEL | ||
| Youtha Autonomy | Parent | (+) “She’ll definitely remind me of an appointment. To me, that’s like being…that’s the adult in [Youth]. She’s responsible in those areas.” |
| Provider | (+) “There are some teens that are very aware that they need help and are willing to do it and so, they come in asking for it.”(−) “Ultimately, we said, ‘This is your choice.’ So, she chose to leave.” | |
| Youth Motivation/Apathy | Parent | (−) “Well, they told him it’s best that he gets on the medication…Something may not work, something may work but you won’t know until you try. But [Youth] doesn’t care.” |
| Provider | (+) “We have one kid who was a… transgender female taking hormones. She AWOLed her facility and managed to take a bus, I believe, all the way to the clinic in [this] county to make sure she made it to her appointment on time.”(−) “.They [youth] tend not to necessarily be as interested in getting healthcare.” | |
| Youth Trust/Distrust | Parent | (−) “No. No. No. Because for one, [Youth] wasn’t honest about a lot of stuff. I can just see it. So therefore you’re not honest with everything then nothing works.” |
| Provider | (+) “The rapport and the trust is built while they’re still incarcerated.”(−) “They [reentry youth] don’t trust people right away, for the most part.” | |
| INTERPERSONAL LEVEL | ||
| Family Engagement/Disengagement | Parent | (+) “Having parents who are engaged. Parents who actually care about the wellbeing of their kids are the ones who are going to make sure that their kids are healthy and came move on in life.”(−) “I think it [Zoloft & Trazadone] helps. But it would be best if he stops the medicine because I think that when one takes, takes too much medicine, you become addicted to the medicine.” |
| Provider | (+) “The whole family system needs to change in order for there to be impactful improvement on the kid’s behavior.”(−) “One of the top challenges that we face is to engage the parents in treatment.” | |
| Youth-Provider Rapport | Parent | (+) “So that depends on the doctor and the relationship that that particular doctor has with that kid. You know, like I know [Youth’s] doctor has a good relationship with him. He’s been with him since he was 6 weeks old. So it’s a little bit different because he will talk to his doctor. Preferably and not talk to me. Which is fine with me. But he has that type of relationship. So I would say give them a doctor that they trust.”(−) “She would manipulate the psychologist. She knew how to control her and she didn’t feel she had the trust to tell her things.” |
| Provider | (+) “We had the time, we had the energy, and the motivation to really make it a priority to connect with them.”(−) “I think a lot of times people haven’t had any experience living the kind of lives that our kids come from and they haven’t really made an effort to try to figure out what it’s like for the child.” | |
| COMMUNITY LEVEL | ||
| Chaotic vs Structured Home Environments | Parent | (−) “The neighborhood is very bad…lots of shootings.” |
| Provider | (−) “Many of them go back to gang-infested neighborhoods and crime-ridden neighborhoods where many of their peers are involved in gangs, crime, anti-social acts. It makes it difficult to engage them in services.” | |
| Availability of Health Services | Parent | (+) “We simply arrive, sign-in, and they see us instantly.”(−) “I made the appointment, but the clinic told me they didn’t have anything closer, until September. |
| Provider | (+) “The focus is on helping them to reintegrate back into the community by providing evidence-based therapy services to the youth and the families.”(−) “It’s really difficult. The resources that are available are minimal.” | |
| Transportation for Clinic Visits | Parent | (+) “No, it hasn’t been difficult because the doctor isn’t very far, so there is a way for me to take her to the doctor.”(−) “It’s been hard trying to get back and forth constantly down there, because we don’t always have transportation.” |
| Provider | (−) “There’s transportation, which can be a problem… Parents may work all day and night, and so they may not be able to physically get to an office.” | |
| ORGANIZATIONAL LEVEL | ||
| Family-Centered, Coordinated Healthcare | Parent | (+) “Everything was already set up by the time he got home, so they already had found someone that was available to come.”(−) “Usually they will call and give me an appointment or they would have someone coming out to my house but they haven’t done any of this type of stuff this trip. So I don’t know really what’s going on with the mental health.” |
| Provider | (+) “We have great collaboration… It’s not just the clinician and the family, but it’s also working with the other community providers, such as probation or child welfare.”(−) “I think the problem is that the system is not very coordinated and there’s multiple models of care, multiple kinds of insurance.” | |
| Reentry Care Programs | Parent | (+) “So, if they had some kind of program that made the kids, at least make sure they get to their appointments, made sure they see who they need to see. I think that would work. …” |
| Provider | (−) “It is the fear that adults have, but also they tend to not believe that our [youth] can be successful because they have been incarcerated.” | |
| POLICY LEVEL | ||
| Health Insurance | Parent | (−) “Well, they sent me a letter telling me that they were going to discontinue his MediCal because he was in custody. I got a letter from probation letting them know that he’s on longer in custody. So I gave that to the social worker. So now I’m kind of getting the runaround about who his doctor is, if the MediCal’s any good or onto it’s just a mess. He really hasn’t seen any doctors since he’s been home even though he needs to.” |
| Provider | (−) “Medicaid is not automatically reactivated and the family has a hard time getting their insurance reestablished and then they can’t fill their prescriptions. They can’t keep their follow-up appointments.” |
4.2.1. Individual level.
Individual-level leverage points included: autonomy, motivation/apathy, and trust/distrust. Autonomy had the dual function of facilitating access to care as well as inhibiting it; the remaining leverage points all functioned as barriers or “closed” gateways.
The concept of youth autonomy referred to the perception of youth feeling able to take care of themselves. Parents and providers agreed that this sense of autonomy sometimes enhanced youths’ willingness and ability to seek healthcare, while other times it contributed to a sense that they do not need health professionals. Parents described varying levels of youth autonomy in healthcare seeking behaviors; older adolescents were more often expected to schedule their own healthcare appointments. As one parent stated, “I really want them to learn to take care of themselves ‘cause I’m a be outta here in a minute.” Parents and providers expressed that youth often had an independent and “rebellious nature” that lead them to forego healthcare interventions. Embedded within the concept of autonomy was the notion of resiliency, which enhanced youths’ abilities to seek out needed care. Unlike the parents, who did not discuss youths’ household challenges, providers explained that many youth had undergone “trauma and so much issues in the families.” Providers described the youth as “incredibly strong,” fostering an autonomy that, at times, could drive youth to access care. However, the strength and autonomy resulting from prior trauma and life challenges also functioned as a barrier to care.
The leverage point youth motivation/apathy referred to the degree that parents and providers perceived youth had internal drive to seek care. They expressed that youth often seemed apathetic towards seeking care during reentry and that providers tend to view the youth as “lazy.” Parents and providers believed that apathy among youth led to them prioritizing care or disliking receiving care. For example, one provider explained that previous negative interactions with providers resulting from frequent systems contact caused youth to be “burnt out from their own treatment.” Likewise, as one parent stated when referring to repeated healthcare experiences, “We are all tired.” Parents also provided additional insight into the perceived apathy of youth towards care. Reasons shared only by parents included youth preferring to be with friends upon returning home (rather than attending health appointments) and youths’ fears of “bad” diagnoses. Contrasting the notion of apathy, both parents and providers described examples of youth demonstrating motivation to access care such as by riding the bus to clinic or requesting to attend clinic visits.
Youth trust/distrust emerged as another individual-level barrier. Parents and providers viewed trust--especially of health providers and probation officers--as pivotal. However, parents and providers emphasized youth mistrust towards providers; not trust. Parents related observing their children not trusting providers, especially mental health professionals, and “manipulating” therapists or not being honest with them about their life circumstances. Similarly, as one provider expressed, youth undergoing reentry tend to not “trust people right away.” Parents and providers explained that a component of the distrust towards providers related to youths’ fear of being negatively judged by providers for their justice-involvement or risky health behaviors, which caused youth to avoid seeking care.
4.2.2. Interpersonal level.
Interpersonal leverage points influencing youths’ care access during reentry centered on: family engagement/disengagement in care and youth-provider rapport.
Family engagement/disengagement in care referred to the extent to which families were supportive and involved in youths’ care during reentry. Engagement referred both to utilizing healthcare services and buying-in to treatment plans. Both parents and providers viewed family engagement as a critical lever for influencing youths’ access to care, especially for the delivery of psychiatric care. As one parent stated, ensuring youth attend all their health appointments is “the best thing a parent can do.” The engagement/disengagement lever mainly functioned as a closed gateway. Parents and providers agreed that lack of parent engagement in youths’ healthcare during reentry, most often attributed to parents being busy or overwhelmed, was a key factor limiting youths’ access to care during reentry. Nearly all provider interviewees spoke about the potency of family engagement to transform access and healthcare experiences. As one provider stated, “The biggest obstacle is probably just the parents…and having them buy into it.” Providers felt that many parents had “ambivalence about psychotropic medications,” which decreased youths’ likelihood of medication adherence. Parents emphasized families, especially the youth, not understanding or being “in denial” of youths’ psychiatric diagnoses.
In addition to parent/caregiver buy-in to care plans, parents and providers explained that many parents lack the availability or knowledge to help youth form healthcare linkages during reentry. Lack of caregiver availability was most often attributed to caregivers’ demanding work schedules or parental incarceration. Parents, in particular, highlighted the potential for probation officers to link youth to care and also to educate the families on the importance of accessing care.
Youth-provider rapport referred to the quality of the interaction and relationship between the youth and health provider. Parents and providers viewed this leverage point as frequently functioning in the closed position; however, interviewees cited several instances and aspects of positive patient-provider rapport that motivated youth to access care. Providers expressed that provider involvement of youth in developing care plans enhanced youths’ motivation to engage in care. Providers cited shared decision-making over healthcare decisions, such as when to initiate medication use, as particularly useful with older adolescents.
Although providers highlighted some positive examples, they felt that many community providers were apathetic about this population, which mirrored the parents’ descriptions of their children not connecting with providers during clinical encounters. As one provider stated, clinicians were “not putting the 100 percent that they should be.” Several provider interviewees attributed the clinician apathy towards youth to provider burn out or providers not relating to the youth. As one provider explained, it can be difficult for providers to empathize and understand the perspectives of youth undergoing reentry because most providers have not “had any experience living the kind of lives that [they] come from.” Lack of empathy towards the youth decreased the quality of care youth received, which, in turn, decreases youths’ motivation to access care and makes providers less motivated to help.
In contrast to providers, parents emphasized continuity and accountability of providers even just showing up for scheduled in-home appointments as an important means to improve rapport. Providers themselves disagreed on how to enhance rapport; some providers felt clinicians needed to be more compassionate towards the youth, while others attributed the main source of the disconnect to family disengagement.
4.2.3. Community Level.
Community-level leverage points included: chaotic vs. structured environments, availability of health services for youth undergoing reentry, and transportation.
Chaotic vs. structured environments referred to the extent to which youth returned to stable, regimented environments. Parents and providers readily discussed the challenges of youth returning to their home, school, and neighborhood. As one provider stated, many youth return to largely unchanged, chaotic environments--to “the same community and the same home where the initial issues were.” While providers frequently discussed challenges in the home, parents did not talk about their own family challenges, although some cited problems in other homes, such as parental drug use. Parents and providers agreed that implementation of structured activities following release mitigated this challenge by keeping youth “out of trouble.” Many youth were returning to dangerous neighborhoods and schools described as “gang-infested,” “crime-ridden,” and “with a lot of violence,” including, as expressed by parents, “brown” versus “black” violence, making it difficult for youth to prioritize their health or even to attend school.
Availability of health services for youth undergoing reentry was viewed as both functioning to facilitate access and as creating a barrier to care, depending on youths’ location and needs. Geographic proximity to primary care and specialty clinics was variable in the county and greatly influenced the logistic feasibility of attending clinic. Parents emphasized the value of “in-home” therapy programs, as these programs minimized transportation and childcare burdens; however, parents cited lack of privacy and inconsistency of provider attendance as concerns. Parents and providers viewed mental health and substance use treatment services as insufficiently available in the county.
Transportation referred to the youths’ access to transportation to health visits. Parents and providers viewed transportation as an obstacle to care because many youth live far from clinics, have unreliable transportation, or rely on caregivers who are unavailable to provide rides to health visits. Transportation was viewed as more modifiable than the other leverage points. Several providers spontaneously stated that it is cheaper to provide transportation than to have the youth fail to access care and become incarcerated again.
4.2.4. Organizational level.
Organizational-level leverage points were: family-centered, coordinated healthcare and programs that meet the youths’ specific healthcare needs.
Family-centered, coordinated healthcare referred to the degree to which the healthcare system was able to deliver coordinated care that met families’ needs. Parents and providers agreed on the importance of coordinated care and emphasized the important role of probation in linking youth to care during reentry. They described fragmented care in transitions between correctional and community settings, and fragmented care across community agencies. Lack of coordination within the community healthcare system, with its “multiple models of care, multiple kinds of insurance,” made it difficult for the youth and their families to access recommended services. Families had difficulty obtaining appointment times that were feasible to attend, requiring that families miss work and youth miss school to attend health visits.
Parents and providers explained that families had to meet multiple requirements to access mental healthcare. There were often “long wait [times]” to see a child psychiatrist. Multiple health system visits, “up to five, six, or seven”, were sometimes needed to see a child psychiatrist and obtain psychotropic medication. Providers explained that many families experience multiple systems involvement (e.g., criminal justice, child welfare, immigration). The high level of systems involvement created an overwhelming burden of requirements and appointments for families. While families described their individual experiences, providers explained uncoordinated care as a common pattern of youth reentry. Thus, the delivery of family-centered, coordinated care was viewed as necessary but largely lacking in the county.
Programs that meet the youths’ specific healthcare needs referred to the extent to which programs existed that met the unique needs of youth undergoing reentry. Parents shared firsthand accounts of utilizing reentry programs that were helpful. Providers agreed that programs geared towards reintegration of youth back into their communities were valuable. Linkages from healthcare providers to comprehensive social services resources in the community, such as housing, employment, and mentoring programs were viewed as critical. Even when programs were capable of meeting the unique needs of these youth, limitations of health providers within healthcare systems created barriers to care. Permeating healthcare experiences, unlike parents who did not discuss prejudices against the youth, providers reported that biases against justice-involved youth existed across care and agency settings. According to providers, youth faced systemic prejudice on the basis of their incarceration history. They reported encounters with providers who “tended to not believe that our [justice-involved youth] can be successful because they have been incarcerated.” Overall, in terms of influencing access to care, the leverage point of reentry-specific programs was viewed as open in some ways, but also closed in many other ways.
4.2.5. Policy level.
Policy-level leverage points centered on health insurance and cost. Parents frequently mentioned challenges related to gaps in Medicaid coverage post-release. Parents and providers both discussed the enhanced difficulties facing families with undocumented status, particularly regarding insurance status. An open gateway within insurance status arose from employee-based health insurance benefits.
Key issues with Medicaid policy reported by parents and providers related primarily to Medicaid suspension during incarceration causing gaps in Medicaid coverage after release. Medicaid lapsed for many youth because the law dictates the suspension of Medicaid while youth are incarcerated but not reinstatement upon release. Parents and providers noted that youth were sometimes unable to fill their prescriptions or keep their follow-up appointments upon reentry due to lapses in Medicaid coverage. Challenges also arose from clinicians in the community declining Medicaid, making care unaffordable for families. Parents explained that care was often unaffordable even when youth had insurance and access to care covered by their insurance because of co-pays, which parents described as ranging from 25−25-25−30. Immigration status and, in particular, undocumented status, either of youth or their caregivers, was reported as limiting care access for some youth during reentry as concerns about insurance coverage and cost were heightened.
Within the health insurance leverage point, health benefits associated with employment, including through jobs gained through reentry vocational programs, opened the gateway to care.
4.3. Parent and Provider Recommendations
At each level of the SEM, recommendations for improving access to community care for youth during reentry emerged (Table 2).
Table 2.
Leverage Points and Recommendations for Improving Access to Care for Youth During Community Reentry
| LEVERAGE POINTS | RECOMMENDATION |
|---|---|
| INDIVIDUALYouth autonomyYouth motivation/apathyYouth trust/distrust | • Cultivate health education and awareness of healthcare needs |
| INTERPERSONALFamily engagement/disengagement in careYouth-provider rapport | • Increase reliability and continuity of providers • Enhance emotional support from providers • Normalize mental health services |
| COMMUNITYChaotic vs. structured home environments; Availability of health services for the youthTransportation | • Foster structure and stability in home environments • Offer free or low-cost transportation • Increase availability of community substance use treatment services |
| ORGANIZATIONALFamily centered, coordinated healthcarePrograms that meet youths’ specific care needs during reentry | • Increase ease of sharing medical records across agencies • Refrain from associating healthcare with punishment • Cidtivate families’ ability to navigate large complex systems • Increase efficiency of care delivery |
| POLICYHealth insurance | • Maintain Medicaid eligibility and coverage • Increase utilization of social services and benefits |
4.3.1. Individual.
Youth-level leverage points were viewed as relatively immutable. However, to better drive youth to seek care, participants recommended programs and practices that cultivate health education and awareness of healthcare needs. Parents and providers explained that fostering education and awareness about the value of care could facilitate family engagement and motivate youth to seek care. One provider stated that preventive care is something “that needs to be talked about more often with youth” because youth tend to feel “indestructible.”
4.3.2. Interpersonal.
Parents and providers viewed the interpersonal-level leverage points as multifaceted. Recommendations to address these interrelated issues included: increase reliability and continuity of providers, increase emotional support from providers, and normalize mental health services. The recommendation increase reliability and continuity of providers emerged most strongly from the parent interviews; notably, in addition to promoting care continuity, parents were asking that providers show up to appointments and in-home therapy visits when expected. Parents expressed that this would facilitate trust in providers, thereby promoting positive rapport and family engagement in care. The recommendation to enhance emotional support from providers referred to giving emotional support during the transitional process back to the youth’s home environment. Rather than a simple “hand-off,” providers recommended that clinicians invest the time and energy to establish sincere emotional connections with youth, which can be used as a platform to encourage youth to engage in healthcare during reentry. The recommendation to normalize mental health services referred to reducing youths’ and caregivers’ stigma around mental healthcare as a means to encourage youth to seek the care they need.
4.3.3. Community.
Interviewees had mixed levels of optimism for improving the community-level leverage points. Most viewed the leverage point of home environments as largely immutable and beyond the scope of health providers, except as a downstream benefit from improved mental health status. Programs that foster structure and stability in home environments were viewed as useful but difficult to implement. In contrast, transportation was viewed as highly mutable and perhaps the highest yield gateway for counties to improve access to care during reentry. Parents and providers suggested that counties offer free or low-cost transportation to health appointments as a cost-effective means to improve health outcomes. Parents and providers also generally agreed that lack of availability of health services was a concern. Providers specifically suggested that the county increase availability of community substance use treatment services in the community.
4.3.4. Organizational.
Parents and providers felt that steps were needed to improve interagency collaboration. Many felt that the degree of change required to achieve actual benefit for families seemed insurmountable. Others felt that progress was underway and improvement inevitable.
Specific recommendations at the organizational level were: increase ease of sharing medical records across agencies, refrain from associating healthcare with punishment, cultivate youths’ ability to navigate large complex systems, and increase efficiency of care delivery. Increase ease of sharing medical records across agencies referred to the recommendation from providers to improve electronic data sharing across community health systems and between community and correctional health providers. Refrain from associating healthcare with punishment referred to providers suggesting moving away from the punitive approach of punishing youth when they break healthcare-related terms of their probation, such as not attending court-mandated substance use treatment services. Cultivate families’ ability to navigate large complex systems referred to the need to know how to navigate large health systems such as the county mental health clinics; parents wanted probation officers to assist with this. The recommendation increase efficiency of care delivery referred to the suggestion to improve pragmatic aspects of care delivery, such as ease of scheduling, as scheduling challenges were viewed as unnecessarily burdensome for families. This would prevent families from becoming discouraged and instead help families to maintain confidence in the systems of care.
4.3.5. Policy.
Parents and providers identified health insurance and cost as the most important policy-level leverage point. Reforming practices and policies related to Medicaid was viewed as high-yield for improving access to care for the youth. Specifically, maintain Medicaid eligibility and coverage was recommended to overcome gaps in care related to Medicaid suspension during incarceration. Another suggestion was to increase utilization of social services and benefits in order to overcome the poor integration of social services and under-utilization of public benefits.
5. Discussion
Overall, parents and providers agreed that youth undergoing community reentry have high healthcare needs, access to healthcare is important for reducing risky health behaviors and preventing recidivism, and parents play a pivotal role in linking youth to care during reentry. Parents and providers demonstrated substantial agreement about the identified barriers to care during reentry. Their perspectives diverged in that providers blamed parents for sometimes not buying into recommended treatment plans for reentry, especially with regards to mental healthcare, while parents uniquely described feeling powerless when their children were not motivated to receive care. Notably, parents and providers agreed about priority solutions for improving youths’ linkages to care during the crucial reentry period. They also identified leverage points for improving youths’ healthcare access during reentry that spanned all levels of the SEM (CDC, 2015). Findings suggest that solutions to optimize these leverage points exist at every hierarchical level--from individual youth, to families, providers, and to the policies that govern the health systems and community settings youth return home to.
5.1. High-Yield Solutions
Parents and providers identified three leverage points as highest yield for change: transportation, provider reliability and continuity, and health insurance. Solutions included: 1) offering free or lost cost transportation for health visits, 2) ensuring reliability and continuity of providers, and 3) ensuring maintenance of Medicaid insurance coverage.
Other researchers have previously described transportation as a major barrier to care for youth during reentry (Golzari & Kuo, 2013). Providing transportation to health services may be cost-effective and might serve to activate an emotional gateway to care--youth realize that society wants them to be healthy and succeed. Feeling supported and having the logistical means to access care could have great impact in helping youth to overcome barriers to care.
Ensuring reliability and continuity of care aligns with the leverage point that parents and providers emphasized: the importance of family engagement in care, especially in regards to psychiatric care. Interviewees indicated that some aspects of the fragmentation are inherent to reentry, suggesting an opportunity for health and justice systems to improve care continuity during the crucial reentry period. Overcoming care fragmentation would address most, if not all, the identified individual and interpersonal-level leverage points identified. To overcome fragmentation, health systems solutions, such as payment reform, can decrease healthcare costs and improve quality of care for young undergoing reentry (Hyman, 2010). Simultaneously, community-based programs, such as community health worker interventions designed for reentry populations, can help youth and parents navigate fragmented health systems, thereby promoting continuous access to insurance coverage, medications, and providers (Wang et al, 2010). Additionally, cultural shifts that identify continuity of care as a priority goal amongst juvenile justice and health leaders can play an important role in promoting seamless transitions of care during reentry.
The disconnect between parent and provider perspectives, which centered on the extent to which youth and parents demonstrated buy-in to treatment plans during reentry, further signals a need to pursue strategies that enhance families’ engagement in treatment during reentry period. These strategies could address the underlying issue of providers blaming parents for youths’ lack of treatment engagement. In addition to promoting provider reliability and continuity, successful approaches may entail involving families in pre-release planning and keeping parents informed about diagnoses and treatment delivered in the detention setting. This can minimize parents feeling “out of the loop” about care received in detention, and reduce confusion and thus increase buy-in for reentry treatment plans (Aalsma et al., 2014). Additionally, shared-decision making throughout the healthcare process and providing greater health education to parents and youth, especially about psychotropic medications, when indicated, is a promising strategy identified for justice-involved girls and offers a sound approach for increasing families’ engagement in treatment (Barnert, Kelly, Godoy, Abrams, & Bath, 2019). Shared-decision making can help youth, parents, and providers develop an authentic partnership that enhances treatment engagement, reduces blame, and increases youths’ chances of success.
The most pressing policy issue seems to be problems related to lack of or insufficient health insurance. Medicaid is not automatically reinstated upon release from detention, too often leading to gaps in Medicaid insurance coverage, and ultimately, inability for youth to access healthcare. Time to Medicaid de-enrollment differs by youth age, gender, race/ethnicity, and degree of justice involvement, creating inequities in access to care during reentry (Anderson et al, 2019). Ensuring that programs and policies are in place to prevent gaps in Medicaid coverage during reentry was viewed as the second key for improving access to care. Currently, federal law requires that Medicaid be suspended or terminated for youth in detention (Acoca, Stephens, & Van Vleet, 2014). Until this practice ceases, policy interventions and local practices are needed that: delay disenrollment, ensure re-enrollment in Medicaid prior to release, release youth with an identification card in hand, promote follow-up of youth to confirm Medicaid reinstatement in the aftercare period, and ensure adequate coverage consistent with families’ financial means (Gupta, Kelleher, Pajer, Stevens, & Cuellar, 2005). Findings also indicate that developing mechanisms to provide insurance coverage for undocumented families is an important policy focus.
6. Limitations
Our study design includes several key limitations. Selection bias was a concern as parents more involved in their children’s healthcare were more likely to participate in the study. Also, the analysis did not include the perspectives of youth; having their buy-in and perspective is critical to developing and implementing programs and policies for youth during reentry. Additionally, some barriers identified may not be specific to the youth undergoing reentry, but instead may relate more broadly to youth from low-income families or youth of color who are navigating healthcare access and decisions. Many families in our study struggled with poverty and racial injustices while navigating the challenges of their children’s detention and subsequent reentry. The backdrop of poverty and institutionalized racism likely impacted youths’ experiences of obtaining care. Further attention to the unique aspects of reentry is warranted. Moreover, although participants were knowledgeable and experienced, each spoke from their own vantage points--speaking together in a roundtable discussion may have yielded different insights. The study considered both medical and behavioral healthcare, but unique field-specific facilitators and barriers to care likely exist and warrants further investigation. Nevertheless, the parents and providers offered valuable insight on solutions for overcoming identified barriers and facilitators to healthcare for youth undergoing reentry.
7. Conclusion
A priority goal for overcoming barriers to care during reentry is to provide transportation for community health services and to ensure continuity of providers. Policymakers should focus on the immediate goal of solving the logistical barrier created by gaps in Medicaid insurance coverage. Achieving these priority goals can help increase family engagement in care. Findings also suggest that additional strategies, such as increasing youth and parent psychoeducation about medications, are worthwhile for increasing families’ treatment engagement--or treatment “buy-in”--during reentry. Although the parents and providers perspectives had substantial congruences, the divergences identified in this study regarding youth and parent “buy-in” to treatment may reflect a broader schism in providers’ versus parents’ understanding and approach regarding how to achieve the shared goal of promoting youths’ health and success during reentry. One interesting angle of this research is to potentially challenge the sterotype that parents are uninvolved or do not care. Overcoming this schism and these stereotpyes offers a pathway for parents and providers to become collaborative partners in supporting youths’ healthy transitions during reentry.
Supplementary Material
1
2
Highlights.
- Parents and providers agreed on solutions for increasing care access during reentry
- Systems priorities include care continuity and overcoming transportation barriers
- Eliminating Medicaid coverage gaps during reentry was viewed as a policy priority
- Overall, parents play an essential role in linking youth to care during reentry
- Longer-term strategies to enhance family engagement in care are also needed
Acknowledgments
We thank students Marisela Aguilar, Bria Pettway, and Christopher Bondoc for their intellectual contributions. We also thank our study participants
Funding: This work was supported by the National Institutes of Health – National Institute on Drug Abuse [UL1TR000124], the UCLA CTSI [KL2, UL1TR000124], and the California Community Foundation [BAPP-16-125450].
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
Declaration of Interest: The authors have no conflicts of interest to disclose.
Declaration of interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
WE DECLARE THAT WE HAVE NO COMPETING INTERESTS.
References
- Aalsma MC, Brown JR, Holloway ED, & Ott MA (2014). Connection to mental health care upon community reentry for detained youth: A qualitative study. BMC Public Health, 14, 117. 10.1186/1471-2458-14-117 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Abram KM, Choe JY, Washburn JJ, Teplin LA, King DC, & Dulcan MK (2008). Suicidal ideation and behaviors among youths in juvenile detention. Journal of the American Academy of Child & Adolescent Psychiatry, 47(3), 291–300. 10.1097/CHI.0b013e318160b3ce [DOI] [PMC free article] [PubMed] [Google Scholar]
- Abrams LS (2010). Sampling ‘hard to reach’ populations in qualitative research: The case of incarcerated youth. Qualitative Social Work, 9(4), 536–550. https://doi.org/10.1177%2F1473325010367821 [Google Scholar]
- Acoca L, Stephens J, & Van Vleet A (2014). Health coverage and care for youth in the juvenile justice system: The role of Medicaid and CHIP. Washington DC: The Henry J. Kaiser Family Foundation. [Google Scholar]
- Altschuler DM, & Brash R (2004). Adolescent and teenage offenders confronting the challenges and opportunities of reentry. Youth Violence and Juvenile Justice, 2(1), 72–87. https://doi.org/10.1177%2F1541204003260048 [Google Scholar]
- Anderson VR, Ouyang F, Tu W, Rosenman MB, Wiehe SH, Aalsma MC (2019). Medicaid Coverage and Continuity for Juvenile Justice-Involved Youth. Journal of Correctional Health Care, 25(1), 45–54. [DOI] [PubMed] [Google Scholar]
- Annie E Casey Foundation. (2013). Reducing youth incarceration in the United States. Baltimore, MD: Annie E. Casey Foundation. [Google Scholar]
- Barnert ES, Perry R, & Morris RE (2016). Juvenile incarceration and health. Academic Pediatrics, 16(2), 99–109. 10.1016/j.acap.2015.09.004 [DOI] [PubMed] [Google Scholar]
- Barnert ES, Dudovitz R, Nelson BB, Coker TR, Biely C, Li N, & Chung PJ (2017). How does incarcerating young people affect their adult health outcomes? Pediatrics, 139(2), e20162624. 10.1542/peds.2016-2624 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Barnert ES, Kelly M, Godoy S, Abrams LS, & Bath E (2019). Behavioral health treatment “Buy-in” among adolescent females with histories of commercial sexual exploitation. Child Abuse & Neglect, 104042. 10.1016/j.chiabu.2019.104042 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Barnert ES, Lopez N, Pettway B, Keshav N, Abrams LS, Zima B, Chung PJ (2019). The role of parent engagement in overcoming barriers to care for youth after incarceration. Journal of Community Health, Epub. https://doi.10.1007/s10900-019-00747-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bowen GA (2008). Naturalistic inquiry and the saturation concept: A research note. Qualitative Research, 8(1), 137–152. https://doi.org/10.1177%2F1468794107085301 [Google Scholar]
- Braun V, & Clarke V (2006). Using thematic analysis in psychology. Qualitative Research in Psychology, 3(2), 77–101. 10.1191/1478088706qp063oa [DOI] [Google Scholar]
- Burns BJ, Schoenwald SK, Burchard JD, Faw L, & Santos AB (2000). Comprehensive community-based interventions for youth with severe emotional disorders: Multisystemic therapy and the wraparound process. Journal of Child and Family Studies, 9(3), 238–314. 10.1023/A:1026440406435 [DOI] [Google Scholar]
- Centers for Disease Control and Prevention. (2015). Colorectal cancer control program: social ecological model. Retrieved October 24, 2019, from https://www.cdc.gov/cancer/crccp/index.htm?CDC_AA_refVal=https%3A%2F%2Fwww.cdc.gov%2Fcancer%2Fcrccp%2Fsem.htm. [Google Scholar]
- Fields D, & Abrams LS (2010). Gender differences in the perceived needs and barriers of youth offenders preparing for community reentry. Child & Youth Care Forum, 39(4), 253–269. 10.1007/s10566-010-9102-x [DOI] [PMC free article] [PubMed] [Google Scholar]
- Golzari M, Hunt SJ, & Chamberlain LJ (2008). Role of pediatricians as advocates for incarcerated youth. Pediatrics, 121(2), e397–398. 10.1542/peds.2007-0780 [DOI] [PubMed] [Google Scholar]
- Golzari M, & Kuo A (2013). Healthcare utilization and barriers for youth post-detention. International Journal of Adolescent Medicine and Health, 25(1), 65–67. 10.1515/ijamh-2013-0008 [DOI] [PubMed] [Google Scholar]
- Gupta RA, Kelleher KJ, Pajer K, Stevens J, & Cuellar A (2005). Delinquent youth in corrections: Medicaid and reentry into the community. Pediatrics, 115(4), 1077–1083. 10.1542/peds.2004-0776 [DOI] [PubMed] [Google Scholar]
- Herz D, Chan K, Lee S, Ross M, McCroskey J, Newell M, & Fraser C (2015). The Los Angeles County juvenile probation outcomes study. Los Angeles, CA: Advancement Project. [Google Scholar]
- Hyman DA (2010). Health Care Fragmentation. In The Fragmetnation of U.S. Health Care: Causes and Solutions. Oxford University Press. 10.1093/acprof:oso/9780195390131.003.002 [DOI] [Google Scholar]
- Mears DP, Cochran JC, Greenman SJ, Bhati AS, & Greenwald MA (2011). Evidence on the effectiveness of juvenile court sanctions. Journal of Criminal Justice, 39(6), 509–520. 10.1016/j.jcrimjus.2011.09.006 [DOI] [Google Scholar]
- National Center for Juvenile Justice (2017). Easy access to juvenile court statistics: 1997-2017. Retrieved October 24, 2019, from https://www.ojjdp.gov/ojstatbb/ezajcs/. [Google Scholar]
- Piquero AR, Monahan KC, Glasheen C, Schubert CA, & Mulvey EP (2013). Does time matter? Comparing trajectory concordance and covariate association using time-based and age-based assessments. Crime & Delinquency, 59(5), 738–763. https://doi.org/10.1177%2F0011128712459491 [Google Scholar]
- Schubert CA, & Mulvey EP (2014). Behavioral health problems, treatment, and outcomes in serious youthful offenders. US Department of Justice, Office of Juvenile Justice and Delinquency Prevention. [Google Scholar]
- Teplin LA, Abram KM, McClelland GM, Dulcan MK, & Mericle AA (2002). Psychiatric disorders in youth in juvenile detention. Archives of General Psychiatry, 59(12), 1133–1143. 10.1001/archpsyc.59.12.1133 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Teplin LA, McClelland GM, Abram KM, & Mileusnic D (2005). Early violent death among delinquent youth: A prospective longitudinal study. Pediatrics, 115(6), 1586–1593. 10.1542/peds.2004-1459 [DOI] [PMC free article] [PubMed] [Google Scholar]
- Udell W, Mohammed S, & Breland D (2017). Barriers to independently accessing care among detention youth. Journal of Adolescent Research, 32(4), 433–455. https://doi.org/10.1177%2F0743558416653219 [Google Scholar]
- Wang EA, Hong CS, Samuels L, Shavit S, Sanders R, Kushel M (2010). Transitions clinic: creating a community-based model of health care for recently released California prisoners. Public Health Reports, 125(2):171–177. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
1
2