Characterizing abdominal pain in IBS: guidance for study inclusion criteria, outcome measurement and clinical practice - PubMed (original) (raw)
. 2010 Nov;32(9):1192-202.
doi: 10.1111/j.1365-2036.2010.04443.x. Epub 2010 Aug 30.
R Bolus, L A Harris, S Lucak, W D Chey, G Sayuk, E Esrailian, A Lembo, H Karsan, K Tillisch, J Talley, L Chang
Affiliations
- PMID: 20807217
- PMCID: PMC4118306
- DOI: 10.1111/j.1365-2036.2010.04443.x
Characterizing abdominal pain in IBS: guidance for study inclusion criteria, outcome measurement and clinical practice
B M R Spiegel et al. Aliment Pharmacol Ther. 2010 Nov.
Abstract
Background: Although irritable bowel syndrome (IBS) is a multisymptom disorder, abdominal pain drives illness severity more than other symptoms. Despite consensus that IBS trials should measure pain to define study entry and determine efficacy, the optimal method of measuring pain remains uncertain.
Aim: To determine whether combining information from multiple pain dimensions may capture the IBS illness experience more effectively than the approach of measuring 'pain predominance' or pain intensity alone.
Methods: Irritable bowel syndrome patients rated dimensions of pain, including intensity, frequency, constancy, predominance, predictability, duration, speed of onset and relationship to bowel movements. We evaluated the impact of each dimension on illness severity using multivariable regression techniques.
Results: Among the pain dimensions, intensity, frequency, constancy and predictability were strongly and independently associated with illness severity; the other dimensions had weaker associations. The clinical definition of 'pain predominance', in which patients define pain as their most bothersome symptom, was insufficient to categorize patients by illness severity.
Conclusions: Irritable bowel disease pain is multifaceted; some pain dimensions drive illness more than others. IBS trials should measure various pain dimensions, including intensity, constancy, frequency and predictability; this may improve upon the customary use of measuring pain as a unidimensional symptom in IBS.
© 2010 Blackwell Publishing Ltd.
Figures
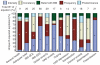
Figure 1
Independent contribution of individual dimensions of overall pain experience to illness severity metrics. Pain intensity captured 5–85% of the explained variance across metrics. Pain frequency and constancy accounted for most of the remaining explained variance across metrics. Pain bothersomeness and relief with bowel movements (BM) contributed small amounts to understanding the various metrics. Bars with asterisks indicate statistically significant associations. The models explained between 6% and 80% of the overall variance of each outcome; the lowest and highest explained variance were for generalized anxiety (overall _R_2 = 6%) and IBS-SSS severity scores (overall _R_2 = 80%) respectively. For ease of interpretation, the bars compartmentalize the relative proportion of each metric explained by the pain dimensions; for reference, the total absolute explained variance is provided above each bar.
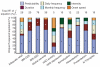
Figure 2
Independent contribution of individual dimensions of acute pain episodes to illness severity metrics. The data indicated that pain episode predictability captured at least one-third of the explained variance for all metrics except HAD anxiety. Episode duration and frequency added an additional 25%, on average, across metrics (with exception of perceived control index, in which frequency was predominant). Pain episode severity and onset speed captured only small amount of the explained variance across metrics. Bars with asterisks indicate statistically significant associations. The absolute proportion of variance explained by each model is listed atop each bar.
Figure 3
Distribution of Patient Ability to Predict Pain Episodes. Patients were posed the following question: `Some people with IBS can predict when a pain episode is about to come on while others cannot. In thinking about your IBS pain episodes, how reliably can you predict, in advance, that an episode is about to happen on a scale from 0 (IBS episodes are totally unpredictable) to 10 (IBS episodes are totally predictable)?' The data reveal a right skewed distribution with <3% able to `totally' predict their pain episodes. In contrast, the most common response was that pain episodes were `totally unpredictable'.
References
- Longstreth GF, Thompson WG, Chey WD, Houghton LA, Mearin F, Spiller RC. Functional bowel disorders. Gastroenterology. 2006;130:1480–91. -PubMed
- Whitehead WE, Crowell MD, Bosmajian L, et al. Existence of irritable bowel syndrome supported by factor analysis of symptoms in two community samples. Gastroenterology. 1990;98:336–40. -PubMed
- Taub E, Cuevas JL, Cook EW, III, Crowell M, Whitehead WE. Irritable bowel syndrome defined by factor analysis. Gender and race comparisons. Dig Dis Sci. 1995;40:2647–55. -PubMed
- Spiegel BM, Gralnek IM, Bolus R, et al. Clinical determinants of health-related quality of life in patients with irritable bowel syndrome. Arch Intern Med. 2004;164:1773–80. -PubMed
Publication types
MeSH terms
Grants and funding
- P50 DK064539/DK/NIDDK NIH HHS/United States
- U01 AR057936/AR/NIAMS NIH HHS/United States
- U01 AR057936A/AR/NIAMS NIH HHS/United States
- P50 DK64539/DK/NIDDK NIH HHS/United States