Alveolar Dead Space Fraction Discriminates Mortality in Pediatric Acute Respiratory Distress Syndrome - PubMed (original) (raw)
Observational Study
Alveolar Dead Space Fraction Discriminates Mortality in Pediatric Acute Respiratory Distress Syndrome
Nadir Yehya et al. Pediatr Crit Care Med. 2016 Feb.
Abstract
Objectives: Physiologic dead space is associated with mortality in acute respiratory distress syndrome, but its measurement is cumbersome. Alveolar dead space fraction relies on the difference between arterial and end-tidal carbon dioxide (alveolar dead space fraction = (PaCO2 - PetCO2) / PaCO2). We aimed to assess the relationship between alveolar dead space fraction and mortality in a cohort of children meeting criteria for acute respiratory distress syndrome (both the Berlin 2012 and the American-European Consensus Conference 1994 acute lung injury) and pediatric acute respiratory distress syndrome (as defined by the Pediatric Acute Lung Injury Consensus Conference in 2015).
Design: Secondary analysis of a prospective, observational cohort.
Setting: Tertiary care, university affiliated PICU.
Patients: Invasively ventilated children with pediatric acute respiratory distress syndrome.
Interventions: None.
Measurements and main results: Of the 283 children with pediatric acute respiratory distress syndrome, 266 had available PetCO2. Alveolar dead space fraction was lower in survivors (median 0.13; interquartile range, 0.06-0.23) than nonsurvivors (0.31; 0.19-0.42; p < 0.001) at pediatric acute respiratory distress syndrome onset, but not 24 hours after (survivors 0.12 [0.06-0.18], nonsurvivors 0.14 [0.06-0.25], p = 0.430). Alveolar dead space fraction at pediatric acute respiratory distress syndrome onset discriminated mortality with an area under receiver operating characteristic curve of 0.76 (95% CI, 0.66-0.85; p < 0.001), better than either initial oxygenation index or PaO2/FIO2. In multivariate analysis, alveolar dead space fraction at pediatric acute respiratory distress syndrome onset was independently associated with mortality, after adjustment for severity of illness, immunocompromised status, and organ failures.
Conclusions: Alveolar dead space fraction at pediatric acute respiratory distress syndrome onset discriminates mortality and is independently associated with nonsurvival. Alveolar dead space fraction represents a single, useful, readily obtained clinical biomarker reflective of pulmonary and nonpulmonary variables associated with mortality.
Figures
Figure 1
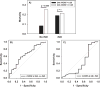
(A) AVDSf at PARDS onset and at 24 hours in survivors and non-survivors. Data is presented as medians and IQR. _P_-value represents Wilcoxon rank sum tests. (B) ROC curves for AVDSf at PARDS onset (AUROC 0.76, 95% CI 0.66 to 0.85, p < 0.001) and 24 hours after PARDS onset (AUROC 0.55, 95% CI 0.42 to 0.68, p = 0.429).
Figure 2
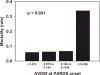
Mortality stratified by quartiles of AVDSf at PARDS onset. _P_-value represents Fisher exact test.
Figure 3
AVDSf at PARDS onset and at 24 hours in patients (A) not exposed and (B) exposed to iNO.
Figure 4
(A) AVDSf at 24 hours in patients not exposed and exposed to iNO. (B) ROC curve for discriminating mortality in patients not exposed to iNO (AUROC 0.64 (95% CI 0.50 to 0.78, p = 0.060). (C) ROC curve for discriminating mortality in patients exposed to iNO (AUROC 0.42 (95% CI 0.19 to 0.64, p = 0.386).
Comment in
- Pediatric Acute Respiratory Distress Syndrome: Which Child Is Destined to Die?
Anas NG. Anas NG. Pediatr Crit Care Med. 2016 Feb;17(2):165-7. doi: 10.1097/PCC.0000000000000632. Pediatr Crit Care Med. 2016. PMID: 26841026 No abstract available. - Generalizability Concern of Alveolar Dead Space Fraction of Yehya et al.
Koomen E, Wösten-van Asperen RM. Koomen E, et al. Pediatr Crit Care Med. 2017 Feb;18(2):204. doi: 10.1097/PCC.0000000000001041. Pediatr Crit Care Med. 2017. PMID: 28157805 No abstract available. - The authors reply.
Yehya N, Bhalla AK, Thomas NJ, Khemani RG. Yehya N, et al. Pediatr Crit Care Med. 2017 Feb;18(2):204-205. doi: 10.1097/PCC.0000000000001043. Pediatr Crit Care Med. 2017. PMID: 28157806 No abstract available.
References
- Ranieri VM, Rubenfeld GD, Thompson BT, et al. Acute respiratory distress syndrome: the Berlin Definition. JAMA. 2012;307(23):2526–2533. -PubMed
- Bernard GR, Artigas A, Brigham KL, et al. The American-European Consensus Conference on ARDS. Definitions, mechanisms, relevant outcomes, and clinical trial coordination. Am J Respir Crit Care Med. 1994;149(3 Pt 1):818–824. -PubMed
- Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. The Acute Respiratory Distress Syndrome Network. N Engl J Med. 2000;342(18):1301–1308. -PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources