2019 Focused Update of the Guidelines of the Taiwan Society of Cardiology for the Diagnosis and Treatment of Heart Failure - PubMed (original) (raw)
Review
. 2019 May;35(3):244-283.
doi: 10.6515/ACS.201905_35(3).20190422A.
Cho-Kai Wu 2, Ming-Lung Tsai 1, Chii-Ming Lee 2, Wei-Chun Huang 3, Hsin-Hua Chou 4, Jin-Long Huang 5, Nai-Hsin Chi 6, Hsueh-Wei Yen 7, Bing-Hsiean Tzeng 8, Wei-Ting Chang 9, Hung-Yu Chang 10, Chao-Hung Wang 11, Yen-Yu Lu 12, Jui-Peng Tsai 13, Chun-Hung Su 14, Wen-Jin Cherng 1, Wei-Hsian Yin 10, Chia-Ti Tsai 2, Yen-Wen Wu 8, Jiunn-Lee Lin 2 15, Juey-Jen Hwang 2 16
Affiliations
- PMID: 31249457
- PMCID: PMC6533577
- DOI: 10.6515/ACS.201905_35(3).20190422A
Review
2019 Focused Update of the Guidelines of the Taiwan Society of Cardiology for the Diagnosis and Treatment of Heart Failure
Chun-Chieh Wang et al. Acta Cardiol Sin. 2019 May.
Abstract
Heart failure is a growing epidemic, especially in Taiwan because of the aging population. The 2016 Taiwan Society of Cardiology - Heart Failure with reduced Ejection Fraction (TSOC-HFrEF) registry showed that the guideline-recommended therapies were prescribed suboptimally both at the time of hospital discharge and during follow-up. We, therefore, conducted this 2019 focused update of the guidelines of the Taiwan Society of Cardiology for the diagnosis and treatment of heart failure to reinforce the importance of new diagnostic and therapeutic modalities of heart failure. The 2019 focused update discusses new diagnostic criteria, pharmacotherapy, non-pharmacological management, and certain co-morbidities of heart failure. Angiotensin receptor neprilysin inhibitor and If channel inhibitor is introduced as new and recommended medical therapies. Latest criteria of cardiac resynchronization therapy, implantable cardioverter-defibrillator, heart transplantation, and ventricular assist device therapy are reviewed in the non-pharmacological management chapter. Co-morbidities in heart failure are discussed including chronic kidney disease, diabetes, chronic obstructive pulmonary disease, and sleep-disordered breathing. We also explain the adequate use of oxygen therapy and non-invasive ventilation in heart failure management. A particular chapter for chemotherapy-induced cardiac toxicity is incorporated in the focused update to emphasize the importance of its recognition and management. Lastly, implications from the TSOC-HFrEF registry and post-acute care of heart failure are discussed to highlight the importance of guideline-directed medical therapy and the benefits of multidisciplinary disease management programs. With guideline recommendations, we hope that the management of heart failure can be improved in our society.
Keywords: Biomarkers; Cardiac resynchronization therapy; Cardio-oncology; Co-morbidities; Guidelines; Heart failure; Pharmacotherapy; Post-acute care; Transplantation; Ventricular assist device.
Figures
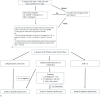
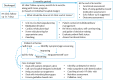
Figure 1
(A) Diagnosis of heart failure with preserved ejection fraction. (B) Grading of diastolic dysfunction. BNP, B-type natriuretic peptide; HF, heart failure; HFpEF, heart failure with preserved ejection fraction; LVEF, left ventricular ejection fraction; NT-proBNP, N-terminal pro B-type natriuretic peptide.
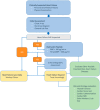
Figure 2
Algorithm of B-type natriuretic peptide (BNP) or N-terminal proB-type natriuretic peptide (NT-proBNP) to assist in the differential diagnosis of HF. HF, heart failure; MRI, magnetic resonance imaging.
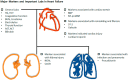
Figure 3
Key biomarkers and necessary laboratory parameters in the differential diagnosis of HF. ALT, alanine aminotransaminase; AST, aspartate aminotransaminase; BNP, B-type natriuretic peptide; BUN, blood urea nitrogen; Hb, hemoglobin; HCT, hematocrit; HF, heart failure; NGAL, neutrophil gelatinase-associated lipocalin; NT-proBNP, N-terminal proB-type natriuretic peptide; UACR, urinary albumin to creatinine ratio.
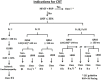
Figure 4
Indications for cardiac resynchronization therapy. AF, atrial fibrillation; CLBBB, complete left bundle branch block; CRT, cardiac resynchronization therapy; Fc, functional class; HFrEF, heart failure with reduced ejection fraction; LBBB, left bundle branch block; LVEF, left ventricular ejection fraction; QRSd, QRS duration; RVP, right ventricular pacing.
Figure 5
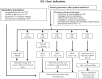
ICD class I indications. CABG, coronary artery bypass graft; CAD, coronary artery disease; CLBBB, complete left bundle branch block; CRT, cardiac resynchronization therapy; CRT-D, cardiac resynchronization therapy defibrillator; EPS, electrophysiologic study; ICD, implantable cardioverter-defibrillator; LVEF left ventricular ejection fraction; MI, myocardial infarction; NIDCM, non-ischemic dilated cardiomyopathy; NSVT, non-sustained ventricular tachycardia; NYHA, New York heart association; PTCA, percutaneous transluminal coronary angioplasty; tx, treatment; VF, ventricular fibrillation; VT, ventricular tachycardia.
Figure 6
Algorithm changes for stage D heart failure. DT, destination therapy; IABP, intra-aortic balloon pump; IV, intravenous; LVAD, left ventricular assist device; LVEF, left ventricular ejection fraction; VO2, oxygen uptake.
Figure 7
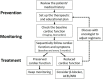
Strategies to reduce chemotherapy-induced cardiotoxicity. ACEI, angiotensin converting enzyme inhibitor; ARB, angiotensin receptor blocker.
Figure 8
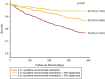
Kaplan-Meier survival curves in registry patients presenting with different types and dosages of guideline-recommended medications. Adapted from “Gap between guidelines and clinical practice in heart failure with reduced ejection fraction: results from TSOC-HFrEF registry”, by Chang HY, Wang CC, Wei J, et al., J Chin Med Assoc 2017;80: 750-7. Adapted with permission.
Figure 9
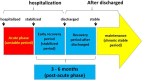
Periods from acute, post-acute to chronic phases.
Figure 10
Programs before discharge. Cath, cardiac catheterization; COPD, chronic obstructive pulmonary disease; ED, emergency department; EF, ejection fraction; HF, heart failure; ICU, intensive care unit; Lab, laboratory tests; PT, physical therapist; rehab, rehabilitation.
Figure 11
Programs after discharge. Echo, echocardiograms; HF, heart failure; rehab, rehabilitation.
References
- Lang RM, Badano LP, Mor-Avi V, et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging. 2015;16:233–270. -PubMed
- Voigt JU, Pedrizzetti G, Lysyansky P, et al. Definitions for a common standard for 2D speckle tracking echocardiography: consensus document of the EACVI/ASE/Industry Task Force to standardize deformation imaging. Eur Heart J Cardiovasc Imaging. 2015;16:1–11. -PubMed
- Lang RM, Badano LP, Tsang W, et al. American Society of E; European Association of E. EAE/ASE recommendations for image acquisition and display using three-dimensional echocardiography. J Am Soc Echocardiogr. 2012;25:3–46. -PubMed
- Chan YH, Lee HF, Wu LS, et al. Ratio of transmitral early filling velocity to early diastolic strain rate predicts outcomes in patients with systolic heart failure. Eur Heart J Cardiovasc Imaging. 2017;18:79–85. -PubMed
- Wang TJ, Larson MG, Levy D, et al. Impact of age and sex on plasma natriuretic peptide levels in healthy adults. Am J Cardiol. 2002;90:254–258. -PubMed
Publication types
LinkOut - more resources
Full Text Sources