Fertility-sparing trachelectomy for early-stage cervical cancer: A proposal of an ideal candidate - PubMed (original) (raw)
Multicenter Study
. 2020 Feb;156(2):341-348.
doi: 10.1016/j.ygyno.2019.11.021. Epub 2019 Nov 23.
Takashi Iwata 2, Kaoru Okugawa 3, Koji Matsuo 4, Tsuyoshi Saito 5, Kyoko Tanaka 2, Kenichiro Morishige 6, Hiroaki Kobayashi 7, Kiyoshi Yoshino 8, Hideki Tokunaga 9, Tomoaki Ikeda 10, Makio Shozu 11, Nobuo Yaegashi 9, Takayuki Enomoto 12, Mikio Mikami 13
Affiliations
- PMID: 31767188
- PMCID: PMC7526083
- DOI: 10.1016/j.ygyno.2019.11.021
Multicenter Study
Fertility-sparing trachelectomy for early-stage cervical cancer: A proposal of an ideal candidate
Hiroko Machida et al. Gynecol Oncol. 2020 Feb.
Abstract
Objective: To propose an ideal patient candidate with early-stage cervical cancer for undergoing fertility-sparing trachelectomy.
Methods: This nationwide, multicenter, retrospective study was conducted by the Japan Society of Obstetrics and Gynecology involving women aged <45 years with clinical stage I-II cervical cancer who had planned fertility-sparing trachelectomy and pelvic lymphadenectomy between 2009 and 2013 (n = 393). Ideal candidates were defined to have a tumor size of ≤2 cm, no lymph node metastasis, no deep stromal invasion, and no high-risk histology (n = 284, 69.6%). Less-ideal candidates were defined to have any one of these four characteristics (n = 109, 30.4%). Propensity score inverse probability of treatment weighting was used to assess survival outcomes.
Results: Less-ideal candidates were more likely to undergo hysterectomy conversion (22.9% versus 3.2%), receive postoperative radiotherapy (11.9% versus 0.4%), or chemotherapy (32.1% versus 3.2%) compared with ideal candidates (all, P < 0.05). The weighted model revealed that among those who underwent trachelectomy (ideal candidates, n = 275 and less-ideal candidates, n = 84), less-ideal candidates had significantly decreased disease-free survival (5-year rates: 85.5% versus 95.5%; HR 3.93, 95% CI 1.99-7.74; P < 0.001) and cause-specific survival (92.5% versus 98.6%; HR 5.47, 95% CI 1.68-17.8, P = 0.001) compared with ideal candidates. Similarly, less-ideal candidates were significantly associated with decreased disease-free survival compared with ideal candidates among those who were young age, had small tumors or squamous histology, and underwent surgery alone (all, P < 0.05).
Conclusion: Less-ideal candidates had approximately four-fold higher recurrence risk and cancer mortality compared with ideal candidates. Ideal candidates for fertility-sparing trachelectomy for early-stage cervical cancer proposed in our study may be useful as the future framework for developing guidelines for fertility-sparing trachelectomy in Japan.
Keywords: Cervical cancer; Deep stromal invasion; Lymph node metastasis; Survival; Trachelectomy; Tumor size.
Copyright © 2019 Elsevier Inc. All rights reserved.
Figures
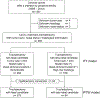
Fig. 1.
Schema for patient selection.
Fig. 2.
Survival curves: ideal candidates versus less-ideal candidates. P values were derived from IPTW-adjusted log-rank test. A) disease-free survival and B) cause-specific survival are shown between the ideal and less-ideal candidate groups. Y-axis was truncated to 50–100%. Risk-stratified survival curves are shown for C) disease-free survival and D) cause-specific survival between the ideal versus less-ideal candidate groups.
Fig. 3.
Forest plots for HR for disease-free survival (IPTW models). Cox proportional hazard regression models for analysis. In each subgroup analysis, IPTW was fitted to compare the ideal and less-ideal candidate groups. HR represents the less-ideal candidate group versus the ideal candidate group. In all the subgroups, the less-ideal group had significantly decreased disease-free survival compared with that of the ideal group. X-axis was transformed to log10 scale. Circles represent IPTW-HR, and bars represent 95% confidence intervals. Abbreviations: HR, hazard ratio; IPTW, inverse probability of treatment weighting; SCC, squamous cell carcinoma. *Trachelectomy alone without neoadjuvant chemotherapy or postoperative treatment.
References
- Projected Cancer Statistics, Cancer information service, https://ganjoho.jp/en/public/statistics/short_pred.html, 2018. Accessed date: 4 September 2019.
- Peters WA 3rd, Liu PY, Barrett RJ 2nd, Stock RJ, Monk BJ, Berek JS, et al. , Concurrent chemotherapy and pelvic radiation therapy compared with pelvic radiation therapy alone as adjuvant therapy after radical surgery in high-risk early-stage cancer of the cervix, J. Clin. Oncol. Off. J. Am. Soc. Clin. Oncol 18 (2000) 1606–1613. -PubMed
- Monk BJ, Wang J, Im S, Stock RJ, Peters WA 3rd, Liu PY, et al. , Rethinking the use of radiation and chemotherapy after radical hysterectomy: a clinical-pathologic analysis of a Gynecologic Oncology Group/Southwest Oncology Group/Radiation Therapy Oncology Group trial, Gynecol. Oncol 96 (2005) 721–728. -PubMed
- Querleu D, Morrow CP, Classification of radical hysterectomy, Lancet Oncol. 9 (2008) 297–303. -PubMed
- Cervical cancer. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines), https://www.nccn.org/professionals/physician_gls/pdf/cervical.pdf, Accessed date: 20 August 2019.