Self-collected and clinician-collected anal swabs show modest agreement for HPV genotyping - PubMed (original) (raw)
Self-collected and clinician-collected anal swabs show modest agreement for HPV genotyping
Racheal S Dube Mandishora et al. PLoS One. 2021.
Erratum in
- Correction: Self-collected and clinician-collected anal swabs show modest agreement for HPV genotyping.
Dube Mandishora RS, Rounge TB, Fitzpatrick M, Christiansen IK, Ambur OH, Lagström S, Stray-Pedersen B, Tommasino M, Palefsky J, Chirenje ZM. Dube Mandishora RS, et al. PLoS One. 2023 Jul 7;18(7):e0288418. doi: 10.1371/journal.pone.0288418. eCollection 2023. PLoS One. 2023. PMID: 37418482 Free PMC article.
Abstract
Background & aim: Women with HIV/HPV coinfection and cervical lesions are at increased risk of developing HPV related anal cancer. Self-collection of anal swabs may facilitate HPV molecular testing in anal cancer screening, especially in high-risk groups, and yet it is not adequately studied. We evaluated level of agreement between self-collected anal swabs (SCAS) and clinician-collected anal swabs (CCAS) when used for HPV genotyping. We also described the anal HPV genotype distribution and HIV/HPV coinfection.
Methods: We performed a cross sectional study with participants from a visual-inspection-with-acetic-acid and cervicography (VIAC) clinic, in Harare, Zimbabwe. In a clinic setting, the women aged ≥18 years provided anal swabs in duplicate; first CCAS and then SCAS immediately after. HPV detection and genotyping were performed using next generation amplicon sequencing of a 450bp region of the HPV L1 gene. Level of agreement of HPV genotypes between CCAS and SCAS was calculated using the kappa statistic. McNemar tests were used to evaluate agreement in the proportion of genotypes detected by either method.
Results: Three-hundred women provided 600 samples for HPV genotyping. HPV genotypes were detected in 25% of SCAS and in 22% of CCAS. The most common genotypes with CCAS were HPV52, HPV62 and HPV70 and with SCAS were HPV62, HPV44, HPV52, HPV53 and HPV68. Total HPV genotypes detected in CCAS were more than those detected in SCAS, 32 versus 27. The agreement of HPV genotypes between the two methods was 0.55 in kappa value (k). The test of proportions using McNemar gave a Chi-square value of 0.75 (p = 0.39). Multiple HPV infections were detected in 28/75 and 29/67 women for CCAS and SCAS respectively.
Conclusions: SCAS and CCAS anal swabs showed moderate agreement, with no statistically significant difference in the proportion of genotypes detected by either methods. Although the differences between the two methods were not statistically significant, CCAS detected more HPV genotypes than SCAS and more HPV infections were detected in SCAS than in CCAS. Our data suggest that self-collected anal swabs can be used as an alternative to clinician-collected anal swabs for HPV genotyping.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
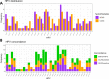
Fig 1
A) HPV genotypes detected in self-collected (SCAS) and clinician-collected (CCAS) anal swabs from women reporting for routine cervical cancer screening. B) Genotype concordance between SCAS and CCAS.
References
- Wagner M, Bennetts L, Patel H, Welner S, de Sanjose S, Weiss TW. Global availability of data on HPV genotype-distribution in cervical, vulvar and vaginal disease and genotype-specific prevalence and incidence of HPV infection in females. Infectious Agents and Cancer. 2015;10:13. 10.1186/s13027-015-0008-y -DOI -PMC -PubMed
- Cervical cancer statistics. World Cancer Research Fund. 2018. https://www.wcrf.org/dietandcancer/cancer-trends/cervical-cancer-statistics. Accessed 20 Aug 2020.