Center use of technical variant grafts varies widely and impacts pediatric liver transplant waitlist and recipient outcomes in the United States - PubMed (original) (raw)
Center use of technical variant grafts varies widely and impacts pediatric liver transplant waitlist and recipient outcomes in the United States
George V Mazariegos et al. Liver Transpl. 2023.
Abstract
To assess the impact of technical variant grafts (TVGs) [including living donor (LD) and deceased donor split/partial grafts] on waitlist (WL) and transplant outcomes for pediatric liver transplant (LT) candidates, we performed a retrospective analysis of Organ Procurement and Transplantation Network (OPTN) data on first-time LT or liver-kidney pediatric candidates listed at centers that performed >10 LTs during the study period, 2004-2020. Center variance was plotted for LT volume, TVG usage, and survival. A composite center metric of TVG usage and WL mortality was developed to demonstrate the existing variation and potential for improvement. Sixty-four centers performed 7842 LTs; 657 children died on the WL. Proportions of WL mortality by center ranged from 0% to 31% and those of TVG usage from 0% to 76%. Higher TVG usage, from deceased donor or LD, independently or in combination, significantly correlated with lower WL mortality. In multivariable analyses, death from listing was significantly lower with increased center TVG usage (HR = 0.611, CI: 0.40-0.92) and LT volume (HR = 0.995, CI: 0.99-1.0). Recipients of LD transplants (HR = 0.637, CI: 0.51-0.79) had significantly increased survival from transplant compared with other graft types, and recipients of deceased donor TVGs (HR = 1.066, CI: 0.93-1.22) had statistically similar outcomes compared with whole graft recipients. Increased TVG utilization may decrease WL mortality in the US. Hence, policy and training to increase TVG usage, availability, and expertise are critical.
Copyright © 2023 The Author(s). Published by Wolters Kluwer Health, Inc.
Conflict of interest statement
Emily R. Perito consults with BridgeBio and received grants from Albireo and Mirum. The remaining authors have no conflicts to report.
Figures
FIGURE 1
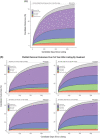
Centers plotted in terciles spanning the minimum and maximum of center metrics: LT volume, TVG volume, WL mortality, and proportions of technical variants (TV, deceased and living donor), and of graft and recipient death within 1-year post-LT. [1Q, median (IQR)].
FIGURE 2
Ranking of proportional noncensored waitlist outcomes and graft types by center WL mortality.
FIGURE 3
Center performance by proportion of waitlist mortality (WLM) and of technical variant graft usage (TVU). There was a significant linear relationship between an increase in TVU and reduction in WLM. Performance quadrants were defined by median values of WLM (6.9%) and TVU (38.7%%) observed in per-candidate analyses. The scatterplot shows 1 dot per center with size related to pediatric liver transplant volume during the study.
FIGURE 4
(A) Overall-center waitlist removal outcomes within 1 year of listing. (B) Waitlist removal outcomes within one of listing by center performance quadrant. Candidate waitlist outcomes were categorized as censored if they were removed from list due to administrative reasons or got better, received a whole graft liver transplant, deceased donor technical variant (“DDTV”) transplant, living donor technical variant (“LDTV”) transplant, or removal if they died or became too sick (“Death/Too Sick”).
FIGURE 5
Centers by performance quadrant and OPTN Region.
FIGURE 6
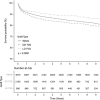
Kaplan-Meier analysis for recipient survival from time of transplant to graft failure or death or last follow-up, stratified by transplant graft type.
FIGURE 7
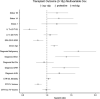
Multivariable Cox analysis of factors associated with recipient graft failure. See Supplemental Table S2 (
) for additional details.
FIGURE 8
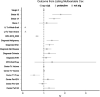
Multivariable Cox analysis of factors associated with patient survival from listing. See Supplemental Table S4 (
) for additional details.
Comment in
- Insufficient use of technical variant grafts: An unfulfilled promise in pediatric liver transplantation.
Sayed BA, Cattral M, Ghanekar A, Ng VL. Sayed BA, et al. Liver Transpl. 2023 Jul 1;29(7):663-664. doi: 10.1097/LVT.0000000000000158. Epub 2023 Apr 18. Liver Transpl. 2023. PMID: 37067384 No abstract available.
References
- Kwong AJ, Kim WR, Lake JR, Smith JM, Schladt DP, Skeans MA, et al. OPTN/SRTR 2019 Annual Data Report: Liver. Am J Transplant. 2021;21(suppl 2):208–315. -PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials