Heart Failure: Practice Essentials, Background, Pathophysiology (original) (raw)
Practice Essentials
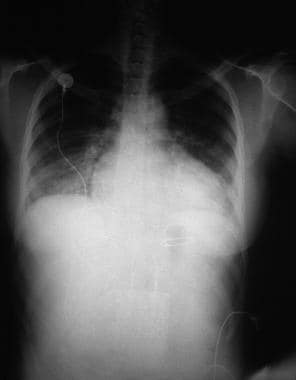
Heart failure develops when the heart, via an abnormality of cardiac function (detectable or not), fails to pump blood at a rate commensurate with the requirements of the metabolizing tissues or is able to do so only with an elevated diastolic filling pressure. See the image below.
Heart Failure. This chest radiograph shows an enlarged cardiac silhouette and edema at the lung bases, signs of acute heart failure.
Signs and symptoms
Signs and symptoms of heart failure include the following:
- Exertional dyspnea and/or dyspnea at rest
- Orthopnea
- Acute pulmonary edema
- Chest pain/pressure and palpitations
- Tachycardia
- Fatigue and weakness
- Nocturia and oliguria
- Anorexia, weight loss, nausea
- Exophthalmos and/or visible pulsation of eyes
- Distention of neck veins
- Weak, rapid, and thready pulse
- Rales, wheezing
- S3 gallop and/or pulsus alternans
- Increased intensity of P2 heart sound
- Hepatojugular reflux
- Ascites, hepatomegaly, and/or anasarca
- Central or peripheral cyanosis, pallor
See Presentation for more detail.
Diagnosis
Heart failure criteria, classification, and staging
The Framingham criteria for the diagnosis of heart failure consists of the concurrent presence of either two major criteria or one major and two minor criteria. [1]
Major criteria comprise the following:
- Paroxysmal nocturnal dyspnea
- Weight loss of 4.5 kg in 5 days in response to treatment
- Neck vein distention
- Rales
- Acute pulmonary edema
- Hepatojugular reflux
- S3 gallop
- Central venous pressure greater than 16 cm water
- Circulation time of 25 seconds or longer
- Radiographic cardiomegaly
- Pulmonary edema, visceral congestion, or cardiomegaly at autopsy
Minor criteria (accepted only if they cannot be attributed to another medical condition) are as follows:
- Nocturnal cough
- Dyspnea on ordinary exertion
- A decrease in vital capacity by one third the maximal value recorded
- Pleural effusion
- Tachycardia (rate of 120 bpm)
- Hepatomegaly
- Bilateral ankle edema
The New York Heart Association (NYHA) classification system categorizes heart failure on a scale of I to IV, [2] as follows:
- Class I: No limitation of physical activity
- Class II: Slight limitation of physical activity
- Class III: Marked limitation of physical activity
- Class IV: Symptoms occur even at rest; discomfort with any physical activity
The American College of Cardiology/American Heart Association (ACC/AHA) staging system is defined by the following four stages [3] :
- Stage A: High risk of heart failure but no structural heart disease or symptoms of heart failure
- Stage B: Structural heart disease but no symptoms of heart failure
- Stage C: Structural heart disease and symptoms of heart failure
- Stage D: Refractory heart failure requiring specialized interventions
Additional ACC/AHA/ and Heart Failure Society of America (HFSA) disease-staging terminology characterizes the syndrome as a continuum [4, 5, 6, 7] :
- "At risk for HF" for stage A: Applied to asymptomatic patients with risk factors such as diabetes or hypertension but no known cardiac changes
- "Pre-HF" for stage B: Adds cardiac structural changes or elevated natriuretic peptides, still in the absence of symptoms
- "Symptomatic HF" for stage C: Structural disease with current or previous symptoms
- "Advanced HF" for stage D: Characterized by severe debilitating symptoms or repeated hospitalizations even with guideline-directed medical therapy (GDMT)
Testing
The following tests may be useful in the initial evaluation for suspected heart failure [3, 8, 9] :
- Complete blood cell (CBC) count
- Iron studies
- Urinalysis
- Electrolyte levels
- Renal and liver function studies
- Fasting blood glucose levels
- Lipid profile
- Thyroid stimulating hormone (TSH) levels
- B-type natriuretic peptide levels
- N-terminal pro-B-type natriuretic peptide levels
- Electrocardiography
- Chest radiography
- Two-dimensional (2-D) echocardiography
- Nuclear imaging [10]
- Maximal exercise testing
- Pulse oximetry or arterial blood gas
- Noninvasive stress testing.
See Workup for more detail.
Management
Treatment includes the following:
- Nonpharmacologic therapy: Oxygen and noninvasive positive pressure ventilation, dietary sodium and fluid restriction, physical activity as appropriate, and attention to weight gain
- Pharmacotherapy: Diuretics, vasodilators, inotropic agents, anticoagulants, beta blockers, ACEIs, ARBs, CCBs, digoxin, nitrates, B-type natriuretic peptids, I(f) inhibitors, ARNIs, soluble guanylate cyclase stimulators, SGLT2Is, and MRAs
Surgical options
Surgical treatment options include the following:
- Electrophysiologic intervention
- Revascularization procedures
- Valve replacement/repair
- Ventricular restoration
- Extracorporeal membrane oxygenation
- Ventricular assist devices
- Heart transplantation
- Total artificial heart
See Treatment and Medication for more detail.

Background
Heart failure is the pathophysiologic state in which the heart, via an abnormality of cardiac function (detectable or not), fails to pump blood at a rate commensurate with the requirements of the metabolizing tissues or is able to do so only with an elevated diastolic filling pressure.
Heart failure (see the images below) may be caused by myocardial failure but may also occur in the presence of near-normal cardiac function under conditions of high demand. Heart failure always causes circulatory failure, but the converse is not necessarily the case, because various noncardiac conditions (eg, hypovolemic shock, septic shock) can produce circulatory failure in the presence of normal, modestly impaired, or even supranormal cardiac function. To maintain the pumping function of the heart, compensatory mechanisms increase blood volume, cardiac filling pressure, heart rate, and cardiac muscle mass. However, despite these mechanisms, there is a progressive decline in the ability of the heart to contract and relax, resulting in worsening heart failure.
Heart Failure. This chest radiograph shows an enlarged cardiac silhouette and edema at the lung bases, signs of acute heart failure.
Heart Failure. A 28-year-old woman presented with acute heart failure secondary to chronic hypertension. The enlarged cardiac silhouette on this anteroposterior (AP) radiograph is caused by acute heart failure due to the effects of chronic high blood pressure on the left ventricle. The heart then becomes enlarged, and fluid accumulates in the lungs (ie, pulmonary congestion).
Signs and symptoms of heart failure include tachycardia and manifestations of venous congestion (eg, edema) and low cardiac output (eg, fatigue). Breathlessness is a cardinal symptom of left ventricular (LV) failure that may manifest with progressively increasing severity.
Heart failure can be classified according to a variety of factors (see Heart Failure Criteria, Classification, and Staging). The New York Heart Association (NYHA) classification for heart failure comprises four classes, based on the relationship between symptoms and the amount of effort required to provoke them, as follows [2] :
- Class I patients have no limitation of physical activity
- Class II patients have slight limitation of physical activity
- Class III patients have marked limitation of physical activity
- Class IV patients have symptoms even at rest and are unable to carry on any physical activity without discomfort
The American College of Cardiology/American Heart Association (ACC/AHA) heart failure guidelines complements the NYHA classification to reflect the progression of disease, divided into four stages, as follows [3] :
- Stage A patients are at high risk for heart failure but have no structural heart disease or symptoms of heart failure
- Stage B patients have structural heart disease but have no symptoms of heart failure
- Stage C patients have structural heart disease and have symptoms of heart failure
- Stage D patients have refractory heart failure requiring specialized interventions
More recently, the ACC/AHA and Heart Failure Society of America (HFSA) introduced additional disease-staging terminology to characterize the syndrome of heart failure as a continuum, as follows [4, 5, 6, 7] :
- "At risk for HF" for stage A: Applied to asymptomatic patients with risk factors such as diabetes or hypertension but no known cardiac changes
- "Pre-HF" for stage B: Adds cardiac structural changes or elevated natriuretic peptides, still in the absence of symptoms
- "Symptomatic HF" for stage C: Structural disease with current or previous symptoms
- "Advanced HF" for stage D: Characterized by severe debilitating symptoms or repeated hospitalizations even with guideline-directed medical therapy (GDMT)
Laboratory studies for heart failure should include a complete blood count (CBC), electrolyte levels, and hepatorenal function studies. Imaging studies such as chest radiography and two-dimensional echocardiography are recommended in the initial evaluation of patients with known or suspected heart failure. B-type natriuretic peptide (BNP) and N-terminal pro-B-type natriuretic peptide (NT-proBNP) levels can be useful in differentiating cardiac and noncardiac causes of dyspnea. (See Workup for more information.)
In acute heart failure, patient care consists of stabilizing the patient's clinical condition; establishing the diagnosis, etiology, and precipitating factors; and initiating therapies to provide rapid symptom relief and survival benefit. Surgical options for heart failure include revascularization procedures, electrophysiologic intervention, cardiac resynchronization therapy (CRT), implantable cardioverter-defibrillators (ICDs), valve replacement or repair, ventricular restoration, heart transplantation, and ventricular assist devices (VADs). (See Treatment for more information.)
The goals of pharmacotherapy are to increase survival and to prevent complications. Along with oxygen, medications assisting with symptom relief include diuretics, digoxin, inotropes, and morphine. Drugs that can exacerbate heart failure should be avoided (nonsteroidal anti-inflammatory drugs [NSAIDs], calcium channel blockers [CCBs], and most antiarrhythmic drugs). (See Medication for more information.)
For further information, see the Medscape Drugs & Diseases articles Pediatric Congestive Heart Failure, Congestive Heart Failure Imaging, Heart Transplantation, Pediatric Heart Transplantation, Coronary Artery Bypass Grafting, and Implantable Cardioverter-Defibrillators.

Pathophysiology
The common pathophysiologic state that perpetuates the progression of heart failure is extremely complex, regardless of the precipitating event. Compensatory mechanisms exist on every level of organization, from the subcellular all the way through to organ-to-organ interactions. Only when this network of adaptations becomes overwhelmed does heart failure ensue. [11, 12, 13, 14, 15]
Adaptations
Most important among the adaptations are the following [16] :
- The Frank-Starling mechanism, in which an increased preload helps to sustain cardiac performance
- Alterations in myocyte regeneration and death
- Myocardial hypertrophy with or without cardiac chamber dilatation, in which the mass of contractile tissue is augmented
- Activation of neurohumoral systems
The release of norepinephrine by adrenergic cardiac nerves augments myocardial contractility and includes activation of the renin-angiotensin-aldosterone system [RAAS], the sympathetic nervous system [SNS], and other neurohumoral adjustments that act to maintain arterial pressure and perfusion of vital organs.
In acute heart failure, the finite adaptive mechanisms that may be adequate to maintain the overall contractile performance of the heart at relatively normal levels become maladaptive when trying to sustain adequate cardiac performance. [17]
The primary myocardial response to chronic increased wall stress is myocyte hypertrophy, death/apoptosis, and regeneration. [18] This process eventually leads to remodeling, usually the eccentric type. Eccentric remodeling further worsens the loading conditions on the remaining myocytes and perpetuates the deleterious cycle. The idea of lowering wall stress to slow the process of remodeling has long been exploited in treating heart failure patients. [19]
The reduction of cardiac output following myocardial injury sets into motion a cascade of hemodynamic and neurohormonal derangements that provoke activation of neuroendocrine systems, most notably the above-mentioned adrenergic systems and RAAS. [20]
The release of epinephrine and norepinephrine, along with the vasoactive substances endothelin-1 (ET-1) and vasopressin, causes vasoconstriction, which increases calcium afterload and, via an increase in cyclic adenosine monophosphate (cAMP), causes an increase in cytosolic calcium entry. The increased calcium entry into the myocytes augments myocardial contractility and impairs myocardial relaxation (lusitropy).
The calcium overload may induce arrhythmias and lead to sudden death. The increase in afterload and myocardial contractility (known as inotropy) and the impairment in myocardial lusitropy lead to an increase in myocardial energy expenditure and a further decrease in cardiac output. The increase in myocardial energy expenditure leads to myocardial cell death/apoptosis, which results in heart failure and further reduction in cardiac output, perpetuating a cycle of further increased neurohumoral stimulation and further adverse hemodynamic and myocardial responses.
In addition, the activation of the RAAS leads to salt and water retention, resulting in increased preload and further increases in myocardial energy expenditure. Increases in renin, mediated by a decreased stretch of the glomerular afferent arteriole, reduce delivery of chloride to the macula densa and increase beta1-adrenergic activity as a response to decreased cardiac output. This results in an increase in angiotensin II (Ang II) levels and, in turn, aldosterone levels, causing stimulation of the release of aldosterone. Ang II, along with ET-1, is crucial in maintaining effective intravascular homeostasis as mediated by vasoconstriction and aldosterone-induced salt and water retention.
The concept of the heart as a self-renewing organ is a relatively recent development. [21] This paradigm for myocyte biology created an entire field of research aimed directly at augmenting myocardial regeneration. The rate of myocyte turnover has been shown to increase during times of pathologic stress. [18] In heart failure, this mechanism for replacement becomes overwhelmed by an even faster increase in the rate of myocyte loss. This imbalance of hypertrophy and death over regeneration is the final common pathway at the cellular level for the progression of remodeling and heart failure.
Angiotensin II
Research indicates that local cardiac Ang II production (which decreases lusitropy, increases inotropy, and increases afterload) leads to increased myocardial energy expenditure. Ang II has also been shown in vitro and in vivo to increase the rate of myocyte apoptosis. [22] In this fashion, Ang II has similar actions to norepinephrine in heart failure.
Ang II also mediates myocardial cellular hypertrophy and may promote progressive loss of myocardial function. The neurohumoral factors above lead to myocyte hypertrophy and interstitial fibrosis, resulting in increased myocardial volume and increased myocardial mass, as well as myocyte loss. As a result, the cardiac architecture changes which, in turn, leads to further increase in myocardial volume and mass.
Myocytes and myocardial remodeling
In the failing heart, increased myocardial volume is characterized by larger myocytes approaching the end of their life cycle. [23] As more myocytes drop out, an increased load is placed on the remaining myocardium, and this unfavorable environment is transmitted to the progenitor cells responsible for replacing lost myocytes.
Progenitor cells become progressively less effective as the underlying pathologic process worsens and myocardial failure accelerates. These features—namely, the increased myocardial volume and mass, along with a net loss of myocytes—are the hallmark of myocardial remodeling. This remodeling process leads to early adaptive mechanisms, such as augmentation of stroke volume (Frank-Starling mechanism) and decreased wall stress (Laplace law) and, later, to maladaptive mechanisms such as increased myocardial oxygen demand, myocardial ischemia, impaired contractility, and arrhythmogenesis.
As heart failure advances, there is a relative decline in the counterregulatory effects of endogenous vasodilators, including nitric oxide (NO), prostaglandins (PGs), bradykinin (BK), atrial natriuretic peptide (ANP), and B-type natriuretic peptide (BNP). This decline occurs simultaneously with the increase in vasoconstrictor substances from the RAAS and the adrenergic system, which fosters further increases in vasoconstriction and thus preload and afterload. This results in cellular proliferation, adverse myocardial remodeling, and antinatriuresis, with total body fluid excess and worsening of heart failure symptoms.
Systolic and diastolic failure
Systolic and diastolic heart failure each result in a decrease in stroke volume. [24, 25] This leads to activation of peripheral and central baroreflexes and chemoreflexes that are capable of eliciting marked increases in sympathetic nerve traffic.
Although there are commonalities in the neurohormonal responses to decreased stroke volume, the neurohormone-mediated events that follow have been most clearly elucidated for individuals with systolic heart failure. The ensuing elevation in plasma norepinephrine directly correlates with the degree of cardiac dysfunction and has significant prognostic implications. Norepinephrine, while directly toxic to cardiac myocytes, is also responsible for a variety of signal-transduction abnormalities, such as downregulation of beta1-adrenergic receptors, uncoupling of beta2-adrenergic receptors, and increased activity of inhibitory G-protein. Changes in beta1-adrenergic receptors result in overexpression and promote myocardial hypertrophy.
Atrial natriuretic peptide and B-type natriuretic peptide
ANP and BNP are endogenously generated peptides activated in response to atrial and ventricular volume/pressure expansion. ANP and BNP are released from the atria and ventricles, respectively, and both promote vasodilation and natriuresis. Their hemodynamic effects are mediated by decreases in ventricular filling pressures, owing to reductions in cardiac preload and afterload. BNP, in particular, produces selective afferent arteriolar vasodilation and inhibits sodium reabsorption in the proximal convoluted tubule. It also inhibits renin and aldosterone release and, therefore, adrenergic activation. ANP and BNP are elevated in chronic heart failure. BNP especially has potentially important diagnostic, therapeutic, and prognostic implications.
For more information, see the Medscape Drugs & Diseases article Natriuretic Peptides in Congestive Heart Failure.
Other vasoactive systems
Other vasoactive systems that play a role in the pathogenesis of heart failure include the ET receptor system, the adenosine receptor system, vasopressin, and tumor necrosis factor-alpha (TNF-alpha). [26] ET, a substance produced by the vascular endothelium, may contribute to the regulation of myocardial function, vascular tone, and peripheral resistance in heart failure. Elevated levels of ET-1 closely correlate with the severity of heart failure. ET-1 is a potent vasoconstrictor and has exaggerated vasoconstrictor effects in the renal vasculature, reducing renal plasma blood flow, glomerular filtration rate (GFR), and sodium excretion.
TNF-alpha has been implicated in response to various infectious and inflammatory conditions. Elevations in TNF-alpha levels have been consistently observed in heart failure and seem to correlate with the degree of myocardial dysfunction. Some studies suggest that local production of TNF-alpha may have toxic effects on the myocardium, thus worsening myocardial systolic and diastolic function.
In individuals with systolic dysfunction, therefore, the neurohormonal responses to decreased stroke volume result in temporary improvement in systolic blood pressure and tissue perfusion. However, in all circumstances, the existing data support the notion that these neurohormonal responses contribute to the progression of myocardial dysfunction in the long term.
Heart failure with preserved ejection fraction
In diastolic heart failure (heart failure with preserved ejection fraction [HFpEF]), the same pathophysiologic processes occur that lead to decreased cardiac output in systolic heart failure, but they do so in response to a different set of hemodynamic and circulatory environmental factors that depress cardiac output. [27]
In HFpEF, altered relaxation and increased stiffness of the ventricle (due to delayed calcium uptake by the myocyte sarcoplasmic reticulum and delayed calcium efflux from the myocyte) occur in response to an increase in ventricular afterload (pressure overload). The impaired relaxation of the ventricle then leads to impaired diastolic filling of the left ventricle (LV).
Morris et al found that right venticular (RV) subendocardial systolic dysfunction and diastolic dysfunction, as detected by echocardiographic strain rate imaging, are common in patients with HFpEF. This dysfunction is potentially associated with the same fibrotic processes that affect the subendocardial layer of the LV and, to a lesser extent, with RV pressure overload. It may play a role in the symptomatology of patients with HFpEF. [28]
LV chamber stiffness
An increase in LV chamber stiffness occurs secondary to any one, or any combination, of the following three mechanisms:
- Rise in filling pressure
- Shift to a steeper ventricular pressure-volume curve
- Decrease in ventricular distensibility
A rise in filling pressure is the movement of the ventricle up along its pressure-volume curve to a steeper portion, as may occur in conditions such as volume overload secondary to acute valvular regurgitation or acute LV failure due to myocarditis.
A shift to a steeper ventricular pressure-volume curve results, most commonly, not only from increased ventricular mass and wall thickness (as observed in aortic stenosis and long-standing hypertension) but also from infiltrative disorders (eg, amyloidosis), endomyocardial fibrosis, and myocardial ischemia.
Parallel upward displacement of the diastolic pressure-volume curve is generally referred to as a decrease in ventricular distensibility. This is usually caused by extrinsic compression of the ventricles.
Concentric LV hypertrophy
Pressure overload that leads to concentric LV hypertrophy (LVH), as occurs in aortic stenosis, hypertension, and hypertrophic cardiomyopathy, shifts the diastolic pressure-volume curve to the left along its volume axis. As a result, ventricular diastolic pressure is abnormally elevated, although chamber stiffness may or may not be altered.
Increases in diastolic pressure lead to an increased myocardial energy expenditure, remodeling of the ventricle, increased myocardial oxygen demand, myocardial ischemia, and eventual progression of the maladaptive mechanisms of the heart that lead to decompensated heart failure.
Arrhythmias
Although life-threatening rhythms are more common in ischemic cardiomyopathy, arrhythmia imparts a significant burden in all forms of heart failure. In fact, some arrhythmias even perpetuate heart failure. The most significant of all rhythms associated with heart failure are the life-threatening ventricular arrhythmias. Structural substrates for ventricular arrhythmias that are common in heart failure, regardless of the underlying cause, include ventricular dilatatation, myocardial hypertrophy, and myocardial fibrosis.
At the cellular level, myocytes may be exposed to increased stretch, wall tension, catecholamines, ischemia, and electrolyte imbalance. The combination of these factors contributes to an increased incidence of arrhythmogenic sudden cardiac death in patients with heart failure.

Etiology
Most patients who present with significant heart failure do so because of an inability to provide adequate cardiac output in that scenario. This is often a combination of the causes listed below in the setting of an abnormal myocardium. The list of causes responsible for presentation of a patient with heart failure exacerbation is very long, and searching for the proximate cause to optimize therapeutic interventions is important.
From a clinical standpoint, classifying the causes of heart failure into the following four broad categories is useful:
- Underlying causes: Underlying causes of heart failure include structural abnormalities (congenital or acquired) that affect the peripheral and coronary arterial circulation, pericardium, myocardium, or cardiac valves, thus leading to increased hemodynamic burden or myocardial or coronary insufficiency
- Fundamental causes: Fundamental causes include biochemical and physiologic mechanisms, through which either an increased hemodynamic burden or a reduction in oxygen delivery to the myocardium results in impairment of myocardial contraction
- Precipitating causes: Overt heart failure may be precipitated by progression of the underlying heart disease (eg, further narrowing of a stenotic aortic valve or mitral valve) or various conditions (fever, anemia, infection) or medications (chemotherapy, nonsteroidal anti-inflammatory drugs [NSAIDs]) that alter the homeostasis of heart failure patients
- Genetics of cardiomyopathy: Dilated, arrhythmic right ventricular and restrictive cardiomyopathies are known genetic causes of heart failure
Underlying causes
Specific underlying factors cause various forms of heart failure, such as systolic heart failure (most commonly, left vetricular [LV] systolic dysfunction), heart failure with preserved LV ejection fraction (LVEF), acute heart failure, high-output heart failure, and right heart failure.
Underlying causes of systolic heart failure include the following:
- Coronary artery disease
- Diabetes mellitus
- Hypertension
- Valvular heart disease (stenosis or regurgitant lesions)
- Arrhythmia (supraventricular or ventricular)
- Infections and inflammation (myocarditis)
- Peripartum cardiomyopathy
- Congenital heart disease
- Drugs (either recreational, such as alcohol and cocaine, or therapeutic drugs with cardiac side effects, such as doxorubicin)
- Idiopathic cardiomyopathy
- Rare conditions (endocrine abnormalities, rheumatologic disease, neuromuscular conditions)
Underlying causes of diastolic heart failure include the following:
- Coronary artery disease
- Diabetes mellitus
- Hypertension
- Valvular heart disease (aortic stenosis)
- Hypertrophic cardiomyopathy
- Restrictive cardiomyopathy (amyloidosis, sarcoidosis)
- Constrictive pericarditis
Underlying causes of acute heart failure include the following:
- Acute valvular (mitral or aortic) regurgitation
- Myocardial infarction (MI)
- Myocarditis
- Arrhythmia
- Drugs (eg, cocaine, calcium channel blockers, or beta-blocker overdose)
- Sepsis
Underlying causes of high-output heart failure include the following:
- Anemia
- Systemic arteriovenous fistulas
- Hyperthyroidism
- Beriberi heart disease
- Paget disease of bone
- Albright syndrome (fibrous dysplasia)
- Multiple myeloma
- Pregnancy
- Glomerulonephritis
- Polycythemia vera
- Carcinoid syndrome
Underlying causes of right heart failure include the following:
- LV failure
- Coronary artery disease (ischemia)
- Pulmonary hypertension
- Pulmonary valve stenosis
- Pulmonary embolism
- Chronic pulmonary disease
- Neuromuscular disease
Precipitating causes of heart failure
A previously stable, compensated patient may develop heart failure that is clinically apparent for the first time when the intrinsic process has advanced to a critical point, such as with further narrowing of a stenotic aortic valve or mitral valve. Alternatively, decompensation may occur as a result of the failure or exhaustion of the compensatory mechanisms but without any change in the load on the heart in patients with persistent, severe pressure or volume overload. In particular, consider whether the patient has underlying coronary artery disease or valvular heart disease.
The most common cause of decompensation in a previously compensated patient with heart failure is inappropriate reduction in the intensity of treatment, such as dietary sodium restriction, physical activity reduction, or drug regimen reduction. Uncontrolled hypertension is the second most common cause of decompensation, followed closely by cardiac arrhythmias (most commonly, atrial fibrillation). Arrhythmias, particularly ventricular arrhythmias, can be life threatening. Also, patients with one form of underlying heart disease that may be well compensated can develop heart failure when a second form of heart disease ensues. For example, a patient with chronic hypertension and asymptomatic LV hypertrophy (LVH) may be asymptomatic until an MI develops and precipitates heart failure.
Systemic infection or the development of unrelated illness can also lead to heart failure. Systemic infection precipitates heart failure by increasing total metabolism as a consequence of fever, discomfort, and cough, increasing the hemodynamic burden on the heart. Septic shock, in particular, can precipitate heart failure by the release of endotoxin-induced factors that can depress myocardial contractility.
Cardiac infection and inflammation can also endanger the heart. Myocarditis or infective endocarditis may directly impair myocardial function and exacerbate existing heart disease. The anemia, fever, and tachycardia that frequently accompany these processes are also deleterious. In the case of infective endocarditis, the additional valvular damage that ensues may precipitate cardiac decompensation.
Patients with heart failure, particularly when confined to bed, are at high risk of developing pulmonary emboli, which can increase the hemodynamic burden on the right ventricle (RV) by further elevating RV systolic pressure, possibly causing fever, tachypnea, and tachycardia.
Intense, prolonged physical exertion or severe fatigue, such as may result from prolonged travel or emotional crisis, is a relatively common precipitant of cardiac decompensation. The same is true of exposure to severe climate change (ie, the individual comes in contact with a hot, humid environment or a bitterly cold one).
Excessive intake of water and/or salt and the administration of cardiac depressants or drugs that cause salt retention are other factors that can lead to heart failure. At the European Society of Cardiology 2017 Congress, investigators presented a study comprising more than 4630 people that indicated high daily salt intake (>13.7 g) is associated with a substantial increased risk of developing heart failure, independent of other risk factors. [29, 30]
Because of increased myocardial oxygen consumption and demand beyond a critical level, the following high-output states can precipitate the clinical presentation of heart failure:
- Profound anemia
- Thyrotoxicosis
- Myxedema
- Paget disease of bone
- Albright syndrome
- Multiple myeloma
- Glomerulonephritis
- Cor pulmonale
- Polycythemia vera
- Obesity
- Carcinoid syndrome
- Pregnancy
- Nutritional deficiencies (eg, thiamine deficiency, beriberi)
Longitudinal data from the Framingham Heart Study has suggested that antecedent subclinical LV systolic or diastolic dysfunction is associated with an increased incidence of heart failure, supporting the notion that heart failure is a progressive syndrome. [31, 32] Another analysis of over 36,000 patients undergoing outpatient echocardiography reported that moderate or severe diastolic dysfunction, but not mild diastolic dysfunction, is an independent predictor of mortality. [33]
Genetics of cardiomyopathy
Autosomal dominant inheritance has been demonstrated in dilated cardiomyopathy and in arrhythmic right ventricular cardiomyopathy. Restrictive cardiomyopathies are usually sporadic and associated with the gene for cardiac troponin I. Genetic tests are available at major genetic centers for cardiomyopathies. [34]
In families with a first-degree relative who has been diagnosed with a cardiomyopathy leading to heart failure, the at-risk patient should be screened and followed. [34] The recommended screening consists of an electrocardiogram and an echocardiogram. If the patient has an asymptomatic LV dysfunction, it should be documented and treated. [34]

Epidemiology
United States statistics
According to 2017 American Heart Association (AHA) data, heart failure affects an estimated 6.5 million Americans aged 20 years and older. [35] With improved survival of patients with acute myocardial infarction and with a population that continues to age, heart failure will continue to increase in prominence as a major health problem in the United States. The AHA projects a 46% increase of heart failure prevalence from year 2012 to year 2030, resulting in 8 million or more Americans aged 18 years or older with heart failure. [35]
Despite a more than decade-long decrease (2000-2012) in the the incidence of heart failure–related deaths in the United States, such deaths are on the rise again, particularly among men and non-Hispanic black populations, according to 2000-2014 data (the most recent data available) released by the Centers for Disease Control and Prevention (CDC) in December 2015. [36, 37] The crude rate for heart failure-related deaths decreased from 103.1 deaths per 100,000 population in 2000 to 89.5 in 2009; it then increased to 96.9 in 2014. The age-adjusted rate for heart failure-related deaths decreased from 105.4 deaths per 100,000 standard population in 2000 to 81.4 in 2012; it then increased to 83.4 in 2013 and to 84.0 in 2014. [36] The trend appears to represent a shift from coronary heart disease as the underlying cause of heart failure deaths toward other cardiovascular and noncardiovascular causes, including malignancies, diabetes, chronic lower respiratory diseases, and renal disease.
Analysis of national and regional trends in hospitalization and mortality among Medicare beneficiaries from 1998-2008 showed a relative decline of 29.5% in heart failure hospitalizations [35, 38] ; however, wide variations were noted between states and races, with black men having the slowest rate of decline. A relative decline of 6.6% in mortality was also observed, although the rate was uneven across states. The length of stay decreased from 6.8 days to 6.4 days, despite an overall increase in the comorbid conditions. [38]
Heart failure statistics for the United States are as follows [35] :
- Heart failure is the primary cause of hospitalization in the elderly. [39, 40]
- An estimated one in eight deaths is from heart failure (about 309,000 deaths caused by heart failure each year)
- Heart failure accounts for 8.5% of cardiovascular-related deaths
- Approximately 960,000 new cases of heart failure are diagnosed each year
- The annual incidence of heart failure in patients older than 65 years is 21 per 1,000 population
- Rehospitalization rates during the 6 months following discharge are as much as 50% [41]
- In 2012, the estimated total cost of heart failure in the United States was 30.7billion(6830.7 billion (68% of which were direct medical costs); by 2030, the total cost is projected to rise to 30.7billion(6869.7 billion, a nearly 127% increase.
The incidence and prevalence of heart failure are higher in black persons, Hispanics, Native Americans, and recent immigrants from developing nations, Russia, and the former Soviet republics. The higher prevalence of heart failure in blacks, Hispanics, and Native Americans is directly related to the higher incidence and prevalence of hypertension and diabetes. This problem is particularly exacerbated by a lack of access to health care and by substandard preventive health care available to the most indigent of individuals in these and other groups; in addition, many persons in these groups do not have adequate health insurance.
The higher incidence and prevalence of heart failure in recent immigrants from developing nations are largely due to a lack of prior preventive health care, a lack of treatment, or substandard treatment for common conditions, such as hypertension, diabetes, rheumatic fever, and ischemic heart disease.
Men and women have a similar incidence and prevalence of heart failure. However, many differences remain between men and women with heart failure, such as the following:
- Whereas the incidence of heart failure in men approximately doubles with each 10-year age increase between 65 and 85 years, it triples for women between ages 65 to 74 years and 75 to 85 years [35]
- Women tend to develop heart failure later in life than men do
- Women are more likely than men to have preserved systolic function
- Women develop depression more commonly than men do
- Women have signs and symptoms of heart failure similar to those of men, but they are more pronounced in women
- Women survive longer with heart failure than men do
The prevalence of heart failure increases with age. [40] The prevalence is 1-2% of the population younger than 55 years and increases to a rate of 10% for persons older than 75 years. Nonetheless, heart failure can occur at any age, depending on the cause.
International statistics
Heart failure is a worldwide problem. The most common cause of heart failure in industrialized countries is ischemic cardiomyopathy, with other causes, including Chagas disease and valvular cardiomyopathy, assuming a more important role in developing countries. However, in developing nations that have become more urbanized and more affluent, eating a more processed diet and leading a more sedentary lifestyle have resulted in an increased rate of heart failure, along with increased rates of diabetes and hypertension. This change was illustrated in a population study in Soweto, South Africa, where the community transformed into a more urban and westernized city, followed by an increase in diabetes, hypertension, and heart failure. [42]
In terms of treatment, one study showed few important differences in uptake of key therapies in European countries with widely differing cultures and varying economic status for patients with heart failure. In contrast, studies of sub-Saharan Africa, where healthcare resources are more limited, have shown poor outcomes in specific populations. [43, 44] For example, in some countries, hypertensive heart failure carries a 25% 1-year mortality, and human immunodeficiency virus (HIV)–associated cardiomyopathy generally progresses to death within 100 days of diagnosis in patients who are not treated with antiretroviral drugs.
Although data regarding developing nations are not as robust as studies of Western society, the following trends in developing nations are apparent:
- Causes tend to be largely nonischemic
- Patients tend to present at a younger age
- Outcomes are largely worse where healthcare resources are limited
- Isolated right heart failure tends to be more prominent, with a variety of causes having been postulated, ranging from tuberculous pericardial disease to lung disease and pollution

Prognosis
In general, the mortality following hospitalization for patients with heart failure is 10.4% at 30 days, 22% at 1 year, and 42.3% at 5 years, despite marked improvement in medical and device therapy. [35, 45, 46, 47, 48, 49]
Mortality is greater than 50% for patients with New York Heart Association (NYHA) class IV, American College of Cardiology/American Heart Association (ACC/AHA) stage D heart failure. Heart failure associated with acute myocardial infarction (MI) has an inpatient mortality of 20-40%; mortality approaches 80% in patients who are also hypotensive (eg, cardiogenic shock). (See Heart Failure Criteria, Classification, and Staging).
Heart failure related to systolic dysfunction has an associated mortality of 50% after 5 years. [24]
Numerous demographic, clinical and biochemical variables have been reported to provide important prognostic value in patients with heart failure, and several predictive models have been developed. [50]
A study by van Diepen et al suggested that patients with heart failure or atrial fibrillation have a significantly higher risk of noncardiac postoperative mortality than patients with coronary artery disease; this risk should be considered even if a minor procedure is planned. [51]
Bursi et al found that among community patients with heart failure, pulmonary artery systolic pressure (PASP), as assessed by Doppler echocardiography, can strongly predict death and can provide incremental and clinically significant prognostic information independent of known outcome predictors. [52]
In the Framingham Offspring Cohort, higher concentrations of galectin-3, a marker of cardiac fibrosis, were associated with an increased risk for incident heart failure (hazard ratio: 1.28 per 1 standard deviation increase in log galectin-3). Galectin-3 was also associated with an increased risk for all-cause mortality (multivariable-adjusted hazard ratio: 1.15). [53]
A more recent, retrospective study that evaluated data from the 2010 Nebraska Hospital Discharge files for 4319 hospitalizations of 3521 heart failure patients admitted to 79 in-state hospitals reported that risk factors for in-hospital mortality in these patients were increasing age, the presence of comordities, and length of hospital day. [54]
In a 2024 prospective, two-center observational study in 350 adults hospitalized for acute heart failure, Espersen et al found four significant independent predictors of the composite of heart failure hospitalization or all-cause mortality in acute heart failure were an admission NT-proBNP (N-terminal pro B-type natriuretic peptide) level of 2000 pg/mL or above, a baseline systolic blood pressure below 120 mmHg, a baseline left atrial volume index of 60 mL/m2 or greater, and 9 or more B-lines on predischarge 4-zone lung ultrasound score (LUS). [55] The investigators noted similar results in a subset of patients (n = 176) with 8-zone LUS data.

Patient Education
To help prevent recurrence of heart failure in patients in whom heart failure was caused by dietary factors or medication noncompliance, counsel and educate such patients about the importance of proper diet and the necessity of medication compliance.
Dunlay et al examined medication use and adherence among community-dwelling patients with heart failure and found that medication adherence was suboptimal in many patients, often because of cost. [56] A randomized controlled trial of 605 patients with heart failure reported that the incidence of all-cause hospitalization or death was not reduced in patients receiving multisession self-care training compared to those receiving a single-session intervention. [57] The optimum method for patient education remains to be established. It appears that more intensive interventions are not necessarily better. [57]

- Ho KK, Pinsky JL, Kannel WB, Levy D. The epidemiology of heart failure: the Framingham Study. J Am Coll Cardiol. 1993 Oct. 22(4 suppl A):6A-13A. [QxMD MEDLINE Link]. [Full Text].
- American Heart Association. Classes of heart failure. Available at https://www.heart.org/HEARTORG/Conditions/HeartFailure/AboutHeartFailure/Classes-of-Heart-Failure_UCM_306328_Article.jsp#.WUcGf-vyuHs. Updated: May 8, 2017; Accessed: June 18, 2017.
- [Guideline] Yancy CW, Jessup M, Bozkurt B, et al, American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation. 2013 Oct 15. 128(16):e240-327. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA Guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Coll Cardiol. 2022 May 3. 79 (17):e263-e421. [QxMD MEDLINE Link]. [Full Text].
- Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA Guideline for the management of heart failure: executive summary: s report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2022 May 3. 145 (18):e876-94. [QxMD MEDLINE Link]. [Full Text].
- Stiles S. New HF guidelines feature 'quad' therapy, tweaked terminology. Medscape Medical News. Available at https://www.medscape.com/viewarticle/971492. April 3, 2022; Accessed: May 6, 2022.
- Pina IL. Key points from the new heart failure guidelines [commentary]. TheHeart.org. Available at https://www.medscape.com/viewarticle/971949. May 4, 2022; Accessed: May 6, 2022.
- [Guideline] Ponikowski P, Voors AA, Anker SD, et al, for the Authors/Task Force Members. 2016 ESC guidelines for the diagnosis and treatment of acute and chronic heart failure: The task force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2016 Jul 14. 37(27):2129-200. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Lindenfeld J, Albert NM, Boehmer JP, et al, for the Heart Failure Society of America. HFSA 2010 comprehensive heart failure practice guideline. J Card Fail. 2010 Jun. 16(6):e1-194. [QxMD MEDLINE Link]. [Full Text].
- Stiles S. FDA approves heart sympathetic activity imaging agent for HF evaluation. Medscape News from WebMD. March 22, 2013. Available at https://www.medscape.com/viewarticle/781309. Accessed: April 5, 2013.
- Braunwald E. The pathogenesis of congestive heart failure: then and now. Medicine. 1991 Jan. 70(1):68-79. [Full Text].
- Braunwald E, Ross J Jr, Sonnenblick EH. Mechanisms of Contraction of the Normal and Failing Heart. 2nd ed. Boston: Little Brown & Co; 1976.
- Greyson CR. Pathophysiology of right ventricular failure. Crit Care Med. 2008 Jan. 36(1 suppl):S57-65. [QxMD MEDLINE Link].
- Haddad F, Doyle R, Murphy DJ, Hunt SA. Right ventricular function in cardiovascular disease, part II: pathophysiology, clinical importance, and management of right ventricular failure. Circulation. 2008 Apr 1. 117(13):1717-31. [QxMD MEDLINE Link].
- Onwuanyi A, Taylor M. Acute decompensated heart failure: pathophysiology and treatment. Am J Cardiol. 2007 Mar 26. 99(6B):25D-30D. [QxMD MEDLINE Link].
- Ross J Jr, Braunwald E. Studies on Starling's law of the heart. IX. The effects of impeding venous return on performance of the normal and failing human left ventricle. Circulation. 1964 Nov. 30:719-27. [QxMD MEDLINE Link]. [Full Text].
- Gheorghiade M, Pang PS. Acute heart failure syndromes. J Am Coll Cardiol. 2009 Feb 17. 53(7):557-73. [QxMD MEDLINE Link]. [Full Text].
- Kajstura J, Leri A, Finato N, Di Loreto C, Beltrami CA, Anversa P. Myocyte proliferation in end-stage cardiac failure in humans. Proc Natl Acad Sci U S A. 1998 Jul 21. 95(15):8801-5. [QxMD MEDLINE Link]. [Full Text].
- Cohn JN. Structural basis for heart failure. Ventricular remodeling and its pharmacological inhibition. Circulation. 1995 May 15. 91(10):2504-7. [QxMD MEDLINE Link]. [Full Text].
- Cody RJ. Hormonal alterations in heart failure. In: Hosenpud JB, Greenberg BH, eds. Congestive Heart Failure: Pathophysiology, Diagnosis and Comprehensive Approach to Management. Philadelphia, PA: Lippincott Williams & Wilkins; 2000. 199-212.
- Anversa P, Nadal-Ginard B. Myocyte renewal and ventricular remodelling. Nature. 2002 Jan 10. 415(6868):240-3. [QxMD MEDLINE Link].
- Leri A, Claudio PP, Li Q, et al. Stretch-mediated release of angiotensin II induces myocyte apoptosis by activating p53 that enhances the local renin-angiotensin system and decreases the Bcl-2-to-Bax protein ratio in the cell. J Clin Invest. 1998 Apr 1. 101(7):1326-42. [QxMD MEDLINE Link]. [Full Text].
- Kajstura J, Leri A, Castaldo C, Nadal-Ginard B, Anversa P. Myocyte growth in the failing heart. Surg Clin North Am. 2004 Feb. 84(1):161-77. [QxMD MEDLINE Link].
- Henes J, Rosenberger P. Systolic heart failure: diagnosis and therapy. Curr Opin Anaesthesiol. 2016 Feb. 29(1):55-60. [QxMD MEDLINE Link].
- Nicoara A, Jones-Haywood M. Diastolic heart failure: diagnosis and therapy. Curr Opin Anaesthesiol. 2016 Feb. 29(1):61-7. [QxMD MEDLINE Link].
- Feldman AM, Combes A, Wagner D, et al. The role of tumor necrosis factor in the pathophysiology of heart failure. J Am Coll Cardiol. 2000 Mar 1. 35(3):537-44. [QxMD MEDLINE Link]. [Full Text].
- Gary R, Davis L. Diastolic heart failure. Heart Lung. 2008 Nov-Dec. 37(6):405-16. [QxMD MEDLINE Link].
- Morris DA, Gailani M, Vaz Perez A, et al. Right ventricular myocardial systolic and diastolic dysfunction in heart failure with normal left ventricular ejection fraction. J Am Soc Echocardiogr. 2011 Aug. 24(8):886-97. [QxMD MEDLINE Link].
- Jousilahti P, Harald K, Jula A, et al, for the National Institute for Health and Welfare-THL - Helsinki - Finland. Salt intake and the risk of heart failure [abstract 1192]. Presented at: European Society of Cardiology 2017 Congress; August 27, 2017; Barcelona, Spain. Eur Heart J. Aug 2017. 38(suppl 1):240. [Full Text].
- Davenport L. High salt intake linked to increased heart-failure risk. Medscape News from WebMD. August 28, 2017. Available at https://www.medscape.com/viewarticle/884824. Accessed: September 1, 2017.
- Lam CS, Lyass A, Kraigher-Krainer E, et al. Cardiac dysfunction and noncardiac dysfunction as precursors of heart failure with reduced and preserved ejection fraction in the community. Circulation. 2011 Jul 5. 124(1):24-30. [QxMD MEDLINE Link]. [Full Text].
- Ho KK, Anderson KM, Kannel WB, Grossman W, Levy D. Survival after the onset of congestive heart failure in Framingham Heart Study subjects. Circulation. 1993 Jul. 88(1):107-15. [QxMD MEDLINE Link]. [Full Text].
- Halley CM, Houghtaling PL, Khalil MK, Thomas JD, Jaber WA. Mortality rate in patients with diastolic dysfunction and normal systolic function. Arch Intern Med. 2011 Jun 27. 171(12):1082-7. [QxMD MEDLINE Link]. [Full Text].
- Murphy RT, Starling RC. Genetics and cardiomyopathy: where are we now?. Cleve Clin J Med. 2005 Jun. 72(6):465-6, 469-70, 472-3 passim. [QxMD MEDLINE Link].
- Benjamin EJ, Blaha MJ, Chiuve SE, et al, for the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics-2017 update: a report from the American Heart Association. Circulation. 2017 Mar 7. 135(10):e146-e603. [QxMD MEDLINE Link]. [Full Text].
- Ni H, Xu J. Recent trends in heart failure-related mortality: United States, 2000–2014. Centers for Disease Control and Prevention. December 31, 2015. Available at https://www.cdc.gov/nchs/data/databriefs/db231.htm. Accessed: January 5, 2016.
- Brauser D. CDC: Heart-failure–related mortality rate climbs after decade-long decrease. Heartwire from Medscape. January 4, 2016. Available at https://www.medscape.com/viewarticle/856704. Accessed: January 5, 2016.
- Chen J, Normand SL, Wang Y, Krumholz HM. National and regional trends in heart failure hospitalization and mortality rates for Medicare beneficiaries, 1998-2008. JAMA. 2011 Oct 19. 306(15):1669-78. [QxMD MEDLINE Link]. [Full Text].
- Kolte D, Abbott JD, Aronow HD. Interventional therapies for heart failure in older adults. Heart Fail Clin. 2017 Jul. 13(3):535-70. [QxMD MEDLINE Link].
- Dharmarajan K, Rich MW. Epidemiology, pathophysiology, and prognosis of heart failure in older adults. Heart Fail Clin. 2017 Jul. 13(3):417-26. [QxMD MEDLINE Link].
- Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009 Apr 2. 360(14):1418-28. [QxMD MEDLINE Link]. [Full Text].
- Stewart S, Wilkinson D, Hansen C, et al. Predominance of heart failure in the Heart of Soweto Study cohort: emerging challenges for urban African communities. Circulation. 2008 Dec 2. 118(23):2360-7. [QxMD MEDLINE Link]. [Full Text].
- Damasceno A, Cotter G, Dzudie A, Sliwa K, Mayosi BM. Heart failure in Sub-Saharan Africa: time for action. J Am Coll Cardiol. 2007 Oct 23. 50(17):1688-93. [QxMD MEDLINE Link]. [Full Text].
- Mbewu A, Mbanya JC. Cardiovascular diseases. In: Jamison DT, Feachem RG, Makgoba MW, et al, eds. Disease and mortality in Sub-Saharan Africa. 2nd ed. Washington, DC: World Bank Publications; 2006. 305-28.
- Dries DL, Exner DV, Domanski MJ, Greenberg B, Stevenson LW. The prognostic implications of renal insufficiency in asymptomatic and symptomatic patients with left ventricular systolic dysfunction. J Am Coll Cardiol. 2000 Mar 1. 35(3):681-9. [QxMD MEDLINE Link]. [Full Text].
- Fonarow GC, Adams KF Jr, Abraham WT, et al, for the ADHERE Scientific Advisory Committee, Study Group and Investigators. Risk stratification for in-hospital mortality in acutely decompensated heart failure: classification and regression tree analysis. JAMA. 2005 Feb 2. 293(5):572-80. [QxMD MEDLINE Link]. [Full Text].
- Levy D, Kenchaiah S, Larson MG, et al. Long-term trends in the incidence of and survival with heart failure. N Engl J Med. 2002 Oct 31. 347 (18):1397-402. [QxMD MEDLINE Link].
- Lucas C, Johnson W, Hamilton MA, et al. Freedom from congestion predicts good survival despite previous class IV symptoms of heart failure. Am Heart J. 2000 Dec. 140(6):840-7. [QxMD MEDLINE Link].
- MacIntyre K, Capewell S, Stewart S, et al. Evidence of improving prognosis in heart failure: trends in case fatality in 66 547 patients hospitalized between 1986 and 1995. Circulation. 2000 Sep 5. 102(10):1126-31. [QxMD MEDLINE Link]. [Full Text].
- Ketchum ES, Levy WC. Establishing prognosis in heart failure: a multimarker approach. Prog Cardiovasc Dis. 2011 Sep-Oct. 54(2):86-96. [QxMD MEDLINE Link].
- van Diepen S, Bakal JA, McAlister FA, Ezekowitz JA. Mortality and readmission of patients with heart failure, atrial fibrillation, or coronary artery disease undergoing noncardiac surgery: an analysis of 38 047 patients. Circulation. 2011 Jul 19. 124(3):289-96. [QxMD MEDLINE Link]. [Full Text].
- Bursi F, McNallan SM, Redfield MM, et al. Pulmonary pressures and death in heart failure: a community study. J Am Coll Cardiol. 2012 Jan 17. 59(3):222-31. [QxMD MEDLINE Link]. [Full Text].
- Ho JE, Liu C, Lyass A, et al. Galectin-3, a marker of cardiac fibrosis, predicts incident heart failure in the community. J Am Coll Cardiol. 2012 Oct 2. 60(14):1249-56. [QxMD MEDLINE Link].
- Nayar P, Yu F, Chandak A, Kan GL, Lowes B, Apenteng BA. Risk factors for in-hospital mortality in heart failure patients: does rurality, payer or admission source matter?. J Rural Health. 2018 Dec. 34(1):103-8. [QxMD MEDLINE Link].
- Espersen C, Campbell RT, Claggett BL, et al. Predictors of heart failure readmission and all-cause mortality in patients with acute heart failure. Int J Cardiol. 2024 Jul 1. 406:132036. [QxMD MEDLINE Link].
- Dunlay SM, Eveleth JM, Shah ND, McNallan SM, Roger VL. Medication adherence among community-dwelling patients with heart failure. Mayo Clin Proc. 2011 Apr. 86(4):273-81. [QxMD MEDLINE Link]. [Full Text].
- DeWalt DA, Schillinger D, Ruo B, et al. Multisite randomized trial of a single-session versus multisession literacy-sensitive self-care intervention for patients with heart failure. Circulation. 2012 Jun 12. 125 (23):2854-62. [QxMD MEDLINE Link].
- Lainscak M, Cleland JG, Lenzen MJ, Follath F, Komajda M, Swedberg K. International variations in the treatment and co-morbidity of left ventricular systolic dysfunction: data from the EuroHeart Failure Survey. Eur J Heart Fail. 2007 Mar. 9(3):292-9. [QxMD MEDLINE Link].
- Panjrath G, Ahmed A. Diagnosis and management of heart failure in older adults. Heart Fail Clin. 2017 Jul. 13(3):427-44. [QxMD MEDLINE Link].
- Stevenson LW, Perloff JK. The limited reliability of physical signs for estimating hemodynamics in chronic heart failure. JAMA. 1989 Feb 10. 261(6):884-8. [QxMD MEDLINE Link].
- Steinhart B, Thorpe KE, Bayoumi AM, Moe G, Januzzi JL Jr, Mazer CD. Improving the diagnosis of acute heart failure using a validated prediction model. J Am Coll Cardiol. 2009 Oct 13. 54(16):1515-21. [QxMD MEDLINE Link].
- [Guideline] Yancy CW, Jessup M, Bozkurt B, et al. 2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of America. Circulation. 2017 Aug 8. 136(6):e137-e161. [QxMD MEDLINE Link]. [Full Text].
- Rich MW, McSherry F, Williford WO, Yusuf S, for the Digitalis Investigation Group. Effect of age on mortality, hospitalizations and response to digoxin in patients with heart failure: the DIG study. J Am Coll Cardiol. 2001 Sep. 38(3):806-13. [QxMD MEDLINE Link].
- [Guideline] Yancy CW, Jessup M, Bozkurt B, et al, for the Writing Committee Members. 2016 ACC/AHA/HFSA focused update on new pharmacological therapy for heart failure: an update of the 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of America. Circulation. 2016 Sep 27. 134(13):e282-93. [QxMD MEDLINE Link]. [Full Text].
- Badve SV, Roberts MA, Hawley CM, et al. Effects of beta-adrenergic antagonists in patients with chronic kidney disease: a systematic review and meta-analysis. J Am Coll Cardiol. 2011 Sep 6. 58(11):1152-61. [QxMD MEDLINE Link].
- Maisel AS, Krishnaswamy P, Nowak RM, et al, for the Breathing Not Properly Multinational Study Investigators. Rapid measurement of B-type natriuretic peptide in the emergency diagnosis of heart failure. N Engl J Med. 2002 Jul 18. 347(3):161-7. [QxMD MEDLINE Link].
- Januzzi JL Jr, Camargo CA, Anwaruddin S, et al. The N-terminal pro-BNP investigation of dyspnea in the emergency department (PRIDE) study. Am J Cardiol. 2005 Apr 15. 95(8):948-54. [QxMD MEDLINE Link].
- Wang CS, FitzGerald JM, Schulzer M, Mak E, Ayas NT. Does this dyspneic patient in the emergency department have congestive heart failure?. JAMA. 2005 Oct 19. 294(15):1944-56. [QxMD MEDLINE Link].
- [Guideline] McDonagh TA, Metra M, Adamo M, et al, for the ESC Scientific Document Group. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J. 2021 Sep 21. 42(36):3599-726. [QxMD MEDLINE Link]. [Full Text].
- Groenveld HF, Januzzi JL, Damman K, et al. Anemia and mortality in heart failure patients a systematic review and meta-analysis. J Am Coll Cardiol. 2008 Sep 2. 52(10):818-27. [QxMD MEDLINE Link].
- Grote Beverborg N, van Veldhuisen DJ, van der Meer P. Anemia in heart failure: still relevant?. JACC Heart Fail. 2018 Mar. 6(3):201-8. [QxMD MEDLINE Link]. [Full Text].
- Beedkar A, Parikh R, Deshmukh P. Heart failure and the iron deficiency. J Assoc Physicians India. 2017 Nov. 65(11):79-80. [QxMD MEDLINE Link].
- Hoes MF, Grote Beverborg N, Kijlstra JD, et al. Iron deficiency impairs contractility of human cardiomyocytes through decreased mitochondrial function. Eur J Heart Fail. 2018 May. 20(5):910-9. [QxMD MEDLINE Link]. [Full Text].
- Rocha BML, Cunha GJL, Menezes Falcao LF. The burden of iron deficiency in heart failure: therapeutic approach. J Am Coll Cardiol. 2018 Feb 20. 71(7):782-93. [QxMD MEDLINE Link].
- Maisel AS, McCord J, Nowak RM, et al, for the Breathing Not Properly Multinational Study Investigators. Bedside B-Type natriuretic peptide in the emergency diagnosis of heart failure with reduced or preserved ejection fraction. Results from the Breathing Not Properly Multinational Study. J Am Coll Cardiol. 2003 Jun 4. 41(11):2010-7. [QxMD MEDLINE Link]. [Full Text].
- Januzzi JL, van Kimmenade R, Lainchbury J, et al. NT-proBNP testing for diagnosis and short-term prognosis in acute destabilized heart failure: an international pooled analysis of 1256 patients: the International Collaborative of NT-proBNP Study. Eur Heart J. 2006 Feb. 27(3):330-7. [QxMD MEDLINE Link].
- Maeda K, Tsutamoto T, Wada A, Hisanaga T, Kinoshita M. Plasma brain natriuretic peptide as a biochemical marker of high left ventricular end-diastolic pressure in patients with symptomatic left ventricular dysfunction. Am Heart J. 1998 May. 135(5 Pt 1):825-32. [QxMD MEDLINE Link].
- Fisher C, Berry C, Blue L, Morton JJ, McMurray J. N-terminal pro B type natriuretic peptide, but not the new putative cardiac hormone relaxin, predicts prognosis in patients with chronic heart failure. Heart. 2003 Aug. 89(8):879-81. [QxMD MEDLINE Link]. [Full Text].
- Hall C, Rouleau JL, Moye L, et al. N-terminal proatrial natriuretic factor. An independent predictor of long-term prognosis after myocardial infarction. Circulation. 1994 May. 89(5):1934-42. [QxMD MEDLINE Link].
- Andersson B, Hall C. N-terminal proatrial natriuretic peptide and prognosis in patients with heart failure and preserved systolic function. J Card Fail. 2000 Sep. 6(3):208-13. [QxMD MEDLINE Link].
- Chen HH, Burnett JC. Natriuretic peptides in the pathophysiology of congestive heart failure. Curr Cardiol Rep. 2000 May. 2(3):198-205. [QxMD MEDLINE Link].
- Cheng V, Kazanagra R, Garcia A, et al. A rapid bedside test for B-type peptide predicts treatment outcomes in patients admitted for decompensated heart failure: a pilot study. J Am Coll Cardiol. 2001 Feb. 37(2):386-91. [QxMD MEDLINE Link].
- Cowie MR, Struthers AD, Wood DA, et al. Value of natriuretic peptides in assessment of patients with possible new heart failure in primary care. Lancet. 1997 Nov 8. 350(9088):1349-53. [QxMD MEDLINE Link].
- Dao Q, Krishnaswamy P, Kazanegra R, et al. Utility of B-type natriuretic peptide in the diagnosis of congestive heart failure in an urgent-care setting. J Am Coll Cardiol. 2001 Feb. 37(2):379-85. [QxMD MEDLINE Link].
- Maeda K, Tsutamoto T, Wada A, Hisanaga T, Kinoshita M. Plasma brain natriuretic peptide as a biochemical marker of high left ventricular end-diastolic pressure in patients with symptomatic left ventricular dysfunction. Am Heart J. 1998 May. 135(5 pt 1):825-32. [QxMD MEDLINE Link].
- Maisel AS, Koon J, Hope J, et al. A rapid bedside test for brain natriuretic peptide accurately predicts cardiac function in patients referred for echocardiography. Am Heart J. 2001. 141:374-9.
- Masson S, Vago T, Baldi G, et al. Comparative measurement of N-terminal pro-brain natriuretic peptide and brain natriuretic peptide in ambulatory patients with heart failure. Clin Chem Lab Med. 2002 Aug. 40(8):761-3. [QxMD MEDLINE Link].
- Song BG, Jeon ES, Kim YH, et al. Correlation between levels of N-terminal pro-B-type natriuretic peptide and degrees of heart failure. Korean J Intern Med. 2005 Mar. 20(1):26-32. [QxMD MEDLINE Link].
- Hobbs FD, Davis RC, Roalfe AK, Hare R, Davies MK, Kenkre JE. Reliability of N-terminal pro-brain natriuretic peptide assay in diagnosis of heart failure: cohort study in representative and high risk community populations. BMJ. 2002 Jun 22. 324(7352):1498. [QxMD MEDLINE Link]. [Full Text].
- Redfield MM, Rodeheffer RJ, Jacobsen SJ, Mahoney DW, Bailey KR, Burnett JC Jr. Plasma brain natriuretic peptide concentration: impact of age and gender. J Am Coll Cardiol. 2002 Sep 4. 40(5):976-82. [QxMD MEDLINE Link].
- St Peter JV, Hartley GG, Murakami MM, Apple FS. B-type natriuretic peptide (BNP) and N-terminal pro-BNP in obese patients without heart failure: relationship to body mass index and gastric bypass surgery. Clin Chem. 2006 Apr. 52 (4):680-5. [QxMD MEDLINE Link].
- Rivera M, Cortes R, Salvador A, et al. Obese subjects with heart failure have lower N-terminal pro-brain natriuretic peptide plasma levels irrespective of aetiology. Eur J Heart Fail. 2005 Dec. 7(7):1168-70. [QxMD MEDLINE Link].
- Hermann-Arnhof KM, Hanusch-Enserer U, Kaestenbauer T, et al. N-terminal pro-B-type natriuretic peptide as an indicator of possible cardiovascular disease in severely obese individuals: comparison with patients in different stages of heart failure. Clin Chem. 2005 Jan. 51(1):138-43. [QxMD MEDLINE Link].
- Seino Y, Ogawa A, Yamashita T, et al. Application of NT-proBNP and BNP measurements in cardiac care: a more discerning marker for the detection and evaluation of heart failure. Eur J Heart Fail. 2004 Mar 15. 6(3):295-300. [QxMD MEDLINE Link].
- Colucci WS, Elkayam U, Horton DP, et al. Intravenous nesiritide, a natriuretic peptide, in the treatment of decompensated congestive heart failure. Nesiritide Study Group. N Engl J Med. 2000 Jul 27. 343(4):246-53. [QxMD MEDLINE Link].
- Ezekowitz JA, Hernandez AF, Starling RC, et al. Standardizing care for acute decompensated heart failure in a large megatrial: the approach for the Acute Studies of Clinical Effectiveness of Nesiritide in Subjects with Decompensated Heart Failure (ASCEND-HF). Am Heart J. 2009 Feb. 157(2):219-28. [QxMD MEDLINE Link].
- Mills RM, LeJemtel TH, Horton DP, et al. Sustained hemodynamic effects of an infusion of nesiritide (human b-type natriuretic peptide) in heart failure: a randomized, double-blind, placebo-controlled clinical trial. Natrecor Study Group. J Am Coll Cardiol. 1999 Jul. 34(1):155-62. [QxMD MEDLINE Link].
- Silver MA, Horton DP, Ghali JK, Elkayam U. Effect of nesiritide versus dobutamine on short-term outcomes in the treatment of patients with acutely decompensated heart failure. J Am Coll Cardiol. 2002 Mar 6. 39(5):798-803. [QxMD MEDLINE Link].
- Miller WL, Hartman KA, Burritt MF, Borgeson DD, Burnett JC Jr, Jaffe AS. Biomarker responses during and after treatment with nesiritide infusion in patients with decompensated chronic heart failure. Clin Chem. 2005 Mar. 51(3):569-77. [QxMD MEDLINE Link].
- Fitzgerald RL, Cremo R, Gardetto N, et al. Effect of nesiritide in combination with standard therapy on serum concentrations of natriuretic peptides in patients admitted for decompensated congestive heart failure. Am Heart J. 2005 Sep. 150(3):471-7. [QxMD MEDLINE Link].
- Michels VV, Moll PP, Miller FA, et al. The frequency of familial dilated cardiomyopathy in a series of patients with idiopathic dilated cardiomyopathy. N Engl J Med. 1992 Jan 9. 326(2):77-82. [QxMD MEDLINE Link].
- Baig MK, Goldman JH, Caforio AL, Coonar AS, Keeling PJ, McKenna WJ. Familial dilated cardiomyopathy: cardiac abnormalities are common in asymptomatic relatives and may represent early disease. J Am Coll Cardiol. 1998 Jan. 31(1):195-201. [QxMD MEDLINE Link].
- Grunig E, Tasman JA, Kucherer H, Franz W, Kubler W, Katus HA. Frequency and phenotypes of familial dilated cardiomyopathy. J Am Coll Cardiol. 1998 Jan. 31 (1):186-94. [QxMD MEDLINE Link].
- McNally E, MacLeod H, Dellefave-Castillo L, et al. Arrhythmogenic right ventricular cardiomyopathy. GeneReviews. 1993. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Cheitlin MD, Alpert JS, Armstrong WF, et al. ACC/AHA guidelines for the clinical application of echocardiography. A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Clinical Application of Echocardiography). Developed in collaboration with the American Society of Echocardiography. Circulation. 1997 Mar 18. 95(6):1686-744. [QxMD MEDLINE Link]. [Full Text].
- Patel AR, Alsheikh-Ali AA, Mukherjee J, et al. 3D echocardiography to evaluate right atrial pressure in acutely decompensated heart failure correlation with invasive hemodynamics. JACC Cardiovasc Imaging. 2011 Sep. 4 (9):938-45. [QxMD MEDLINE Link].
- Prior D, Coller J. Echocardiography in heart failure - a guide for general practice. Aust Fam Physician. 2010 Dec. 39(12):904-9. [QxMD MEDLINE Link].
- Kirkpatrick JN, Wiegers SE, Lang RM. Left ventricular assist devices and other devices for end-stage heart failure: utility of echocardiography. Curr Cardiol Rep. 2010 May. 12(3):257-64. [QxMD MEDLINE Link].
- Abraham J, Abraham TP. The role of echocardiography in hemodynamic assessment in heart failure. Heart Fail Clin. 2009 Apr. 5(2):191-208. [QxMD MEDLINE Link].
- Gupta VA, Nanda NC, Sorrell VL. Role of echocardiography in the diagnostic assessment and etiology of heart failure in older adults: opacify, quantify, and rectify. Heart Fail Clin. 2017 Jul. 13(3):445-66. [QxMD MEDLINE Link].
- Meersch M, Schmidt C, Zarbock A. Echophysiology: the transesophageal echo probe as a noninvasive Swan-Ganz catheter. Curr Opin Anaesthesiol. 2016 Feb. 29(1):36-45. [QxMD MEDLINE Link].
- Kim RJ, Wu E, Rafael A, et al. The use of contrast-enhanced magnetic resonance imaging to identify reversible myocardial dysfunction. N Engl J Med. 2000 Nov 16. 343(20):1445-53. [QxMD MEDLINE Link].
- [Guideline] Ritchie JL, Bateman TM, Bonow RO, et al. Guidelines for clinical use of cardiac radionuclide imaging. Report of the American College of Cardiology/American Heart Association Task Force on Assessment of Diagnostic and Therapeutic Cardiovascular Procedures (Committee on Radionuclide Imaging), developed in collaboration with the American Society of Nuclear Cardiology. J Am Coll Cardiol. 1995 Feb. 25(2):521-47. [QxMD MEDLINE Link].
- Taillefer R, DePuey EG, Udelson JE, Beller GA, Latour Y, Reeves F. Comparative diagnostic accuracy of Tl-201 and Tc-99m sestamibi SPECT imaging (perfusion and ECG-gated SPECT) in detecting coronary artery disease in women. J Am Coll Cardiol. 1997 Jan. 29(1):69-77. [QxMD MEDLINE Link].
- Bonow RO, Maurer G, Lee KL, et al, for the STICH Trial Investigators. Myocardial viability and survival in ischemic left ventricular dysfunction. N Engl J Med. 2011 Apr 28. 364(17):1617-25. [QxMD MEDLINE Link].
- Binanay C, Califf RM, Hasselblad V, et al, for the ESCAPE Investigators and ESCAPE Study Coordinators. Evaluation study of congestive heart failure and pulmonary artery catheterization effectiveness: the ESCAPE trial. JAMA. 2005 Oct 5. 294(13):1625-33. [QxMD MEDLINE Link].
- [Guideline] Dickstein K, Vardas PE, Auricchio A, et al al for the Task Force on Acute Heart Failure of the European Society of Cardiology. 2010 Focused Update of ESC Guidelines on device therapy in heart failure: an update of the 2008 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure and the 2007 ESC guidelines for cardiac and resynchronization therapy. Developed with the special contribution of the Heart Failure Association and the European Heart Rhythm Association. Eur Heart J. 2010 Nov. 31(21):2677-87. [QxMD MEDLINE Link]. [Full Text].
- Bitter T, Westerheide N, Prinz C, et. Cheyne-Stokes respiration and obstructive sleep apnoea are independent risk factors for malignant ventricular arrhythmias requiring appropriate cardioverter-defibrillator therapies in patients with congestive heart failure. Eur Heart J. 2011 Jan. 32(1):61-74. [QxMD MEDLINE Link].
- Ronco C, Haapio M, House AA, Anavekar N, Bellomo R. Cardiorenal syndrome. J Am Coll Cardiol. 2008 Nov 4. 52(19):1527-39. [QxMD MEDLINE Link].
- House AA, Haapio M, Lassus J, Bellomo R, Ronco C. Therapeutic strategies for heart failure in cardiorenal syndromes. Am J Kidney Dis. 2010 Oct. 56(4):759-73. [QxMD MEDLINE Link].
- Giamouzis G, Butler J, Starling RC, et al. Impact of dopamine infusion on renal function in hospitalized heart failure patients: results of the Dopamine in Acute Decompensated Heart Failure (DAD-HF) Trial. J Card Fail. 2010 Dec. 16(12):922-30. [QxMD MEDLINE Link].
- Pleister AP, Baliga RR, Haas GJ. Acute study of clinical effectiveness of nesiritide in decompensated heart failure: nesiritide redux. Curr Heart Fail Rep. 2011 Sep. 8(3):226-32. [QxMD MEDLINE Link].
- O'Connor CM, Starling RC, Hernandez AF, et al. Effect of nesiritide in patients with acute decompensated heart failure. N Engl J Med. 2011 Jul 7. 365(1):32-43. [QxMD MEDLINE Link].
- Konstam MA, Gheorghiade M, Burnett JC Jr, et al, for the Efficacy of Vasopressin Antagonism in Heart Failure Outcome Study With Tolvaptan (EVEREST) Investigators. Effects of oral tolvaptan in patients hospitalized for worsening heart failure: the EVEREST Outcome Trial. JAMA. 2007 Mar 28. 297(12):1319-31. [QxMD MEDLINE Link].
- Massie BM, O'Connor CM, Metra M, et al, for the PROTECT Investigators and Committees. Rolofylline, an adenosine A1-receptor antagonist, in acute heart failure. N Engl J Med. 2010 Oct 7. 363(15):1419-28. [QxMD MEDLINE Link].
- Badve SV, Roberts MA, Hawley CM, et al. Effects of beta-adrenergic antagonists in patients with chronic kidney disease: a systematic review and meta-analysis. J Am Coll Cardiol. 2011 Sep 6. 58(11):1152-61. [QxMD MEDLINE Link].
- Roy D, Talajic M, Nattel S, et al, for the Atrial Fibrillation and Congestive Heart Failure Investigators. Rhythm control versus rate control for atrial fibrillation and heart failure. N Engl J Med. 2008 Jun 19. 358(25):2667-77. [QxMD MEDLINE Link].
- Wilton SB, Fundytus A, Ghali WA, et al. Meta-analysis of the effectiveness and safety of catheter ablation of atrial fibrillation in patients with versus without left ventricular systolic dysfunction. Am J Cardiol. 2010 Nov 1. 106(9):1284-91. [QxMD MEDLINE Link].
- MacDonald MR, Connelly DT, Hawkins NM, et al. Radiofrequency ablation for persistent atrial fibrillation in patients with advanced heart failure and severe left ventricular systolic dysfunction: a randomised controlled trial. Heart. 2011 May. 97(9):740-7. [QxMD MEDLINE Link].
- Chen YM, Li ZB, Zhu M, Cao YM. Effects of exercise training on left ventricular remodelling in heart failure patients: an updated meta-analysis of randomised controlled trials. Int J Clin Pract. 2012 Aug. 66(8):782-91. [QxMD MEDLINE Link].
- Mozaffarian D, Lemaitre RN, King IB, et al. Circulating long-chain omega-3 fatty acids and incidence of congestive heart failure in older adults: the cardiovascular health study: a cohort study. Ann Intern Med. 2011 Aug 2. 155(3):160-70. [QxMD MEDLINE Link].
- Marchioli R, Levantesi G, Silletta MG, et al, for the GISSI-HF Investigators. Effect of n-3 polyunsaturated fatty acids and rosuvastatin in patients with heart failure: results of the GISSI-HF trial. Expert Rev Cardiovasc Ther. 2009 Jul. 7 (7):735-48. [QxMD MEDLINE Link].
- Armstrong PW, Pieske B, Anstrom KJ, et al, for the VICTORIA Study Group. Vericiguat in patients with heart failure and reduced ejection fraction. N Engl J Med. 2020 May 14. 382 (20):1883-93. [QxMD MEDLINE Link]. [Full Text].
- Swedberg K, Komajda M, Böhm M, et al, for the SHIFT Investigators. Ivabradine and outcomes in chronic heart failure (SHIFT): a randomised placebo-controlled study. Lancet. 2010 Sep 11. 376 (9744):875-85. [QxMD MEDLINE Link]. [Full Text].
- Borer JS, Bohm M, Ford I, et al, for the SHIFT Investigators. Effect of ivabradine on recurrent hospitalization for worsening heart failure in patients with chronic systolic heart failure: the SHIFT Study. Eur Heart J. 2012 Nov. 33 (22):2813-20. [QxMD MEDLINE Link]. [Full Text].
- McMurray JJ, Packer M, Desai AS, et al, PARADIGM-HF Investigators and Committees. Angiotensin-neprilysin inhibition versus enalapril in heart failure. N Engl J Med. 2014 Sep 11. 371 (11):993-1004. [QxMD MEDLINE Link]. [Full Text].
- Solomon SD, McMurray JJV, Anand IS, et al, for the PARAGON-HF Investigators and Committees. Angiotensin-neprilysin inhibition in heart failure with preserved ejection fraction. N Engl J Med. 2019 Oct 24. 381 (17):1609-20. [QxMD MEDLINE Link]. [Full Text].
- Solomon SD, Zile M, Pieske B, et al, for the Prospective comparison of ARNI with ARB on Management Of heart failUre with preserved ejectioN fracTion (PARAMOUNT) Investigators. The angiotensin receptor neprilysin inhibitor LCZ696 in heart failure with preserved ejection fraction: a phase 2 double-blind randomised controlled trial. Lancet. 2012 Oct 20. 380 (9851):1387-95. [QxMD MEDLINE Link].
- Entresto (sacubitril/valsartan) [package insert]. East Hanover, NJ: Novartis Pharmaceuticals Corp. October 2019. Available at [Full Text].
- Packer M, Anker SD, Butler J, et al, for the EMPEROR-Reduced Trial Investigators. Cardiovascular and renal outcomes with empagliflozin in heart failure. N Engl J Med. 2020 Oct 8. 383 (15):1413-24. [QxMD MEDLINE Link]. [Full Text].
- McMurray JJV, Solomon SD, Inzucchi SE, et al, for the DAPA-HF Trial Committees and Investigators. Dapagliflozin in patients with heart failure and reduced ejection fraction. N Engl J Med. 2019 Nov 21. 381 (21):1995-2008. [QxMD MEDLINE Link]. [Full Text].
- Anker SD, Butler J, Filippatos G, et al, for the EMPEROR-Preserved Trial Investigators. Empagliflozin in heart failure with a preserved ejection fraction. N Engl J Med. 2021 Oct 14. 385 (16):1451-61. [QxMD MEDLINE Link].
- Solomon SD, McMurray JJV, Claggett B, et al, for the DELIVER Trial Committees and Investigators. Dapagliflozin in heart failure with mildly reduced or preserved ejection fraction. N Engl J Med. 2022 Sep 22. 387(12):1089-98. [QxMD MEDLINE Link]. [Full Text].
- Bhatt DL, Szarek M, Steg PG, et al, for the SOLOIST-WHF Trial Investigators. Sotagliflozin in patients with diabetes and recent worsening heart failure. N Engl J Med. 2021 Jan 14. 384(2):117-28. [QxMD MEDLINE Link]. [Full Text].
- Bhatt DL, Szarek M, Pitt B, et al, for the SCORED Investigators. Sotagliflozin in patients with diabetes and chronic kidney disease. N Engl J Med. 2021 Jan 14. 384(2):129-39. [QxMD MEDLINE Link]. [Full Text].
- Massie BM, Collins JF, Ammon SE, et al, for the WATCH Trial Investigators. Randomized trial of warfarin, aspirin, and clopidogrel in patients with chronic heart failure: the Warfarin and Antiplatelet Therapy in Chronic Heart Failure (WATCH) trial. Circulation. 2009 Mar 31. 119 (12):1616-24. [QxMD MEDLINE Link].
- Freeman JV, Yang J, Sung SH, Hlatky MA, Go AS. Effectiveness and safety of digoxin among contemporary adults with incident systolic heart failure. Circ Cardiovasc Qual Outcomes. 2013 Sep 1. 6 (5):525-33. [QxMD MEDLINE Link].
- Konstantinou DM, Karvounis H, Giannakoulas G. Digoxin in heart failure with a reduced ejection fraction: a risk factor or a risk marker. Cardiology. 2016. 134 (3):311-9. [QxMD MEDLINE Link].
- Owan TE, Hodge DO, Herges RM, Jacobsen SJ, Roger VL, Redfield MM. Trends in prevalence and outcome of heart failure with preserved ejection fraction. N Engl J Med. 2006 Jul 20. 355 (3):251-9. [QxMD MEDLINE Link].
- Hogg K, Swedberg K, McMurray J. Heart failure with preserved left ventricular systolic function; epidemiology, clinical characteristics, and prognosis. J Am Coll Cardiol. 2004 Feb 4. 43 (3):317-27. [QxMD MEDLINE Link].
- Gheorghiade M, Abraham WT, Albert NM, et al, for the OPTIMIZE-HF Investigators and Coordinators. Systolic blood pressure at admission, clinical characteristics, and outcomes in patients hospitalized with acute heart failure. JAMA. 2006 Nov 8. 296 (18):2217-26. [QxMD MEDLINE Link].
- Masip J, Roque M, Sanchez B, Fernandez R, Subirana M, Exposito JA. Noninvasive ventilation in acute cardiogenic pulmonary edema: systematic review and meta-analysis. JAMA. 2005 Dec 28. 294 (24):3124-30. [QxMD MEDLINE Link].
- Peter JV, Moran JL, Phillips-Hughes J, Graham P, Bersten AD. Effect of non-invasive positive pressure ventilation (NIPPV) on mortality in patients with acute cardiogenic pulmonary oedema: a meta-analysis. Lancet. 2006 Apr 8. 367 (9517):1155-63. [QxMD MEDLINE Link].
- Winck JC, Azevedo LF, Costa-Pereira A, Antonelli M, Wyatt JC. Efficacy and safety of non-invasive ventilation in the treatment of acute cardiogenic pulmonary edema--a systematic review and meta-analysis. Crit Care. 2006. 10 (2):R69. [QxMD MEDLINE Link]. [Full Text].
- Vital FM, Saconato H, Ladeira MT, et al. Non-invasive positive pressure ventilation (CPAP or bilevel NPPV) for cardiogenic pulmonary edema. Cochrane Database Syst Rev. 2008 Jul 16. CD005351. [QxMD MEDLINE Link].
- Maeder MT, Kaye DM. Heart failure with normal left ventricular ejection fraction. J Am Coll Cardiol. 2009 Mar 17. 53 (11):905-18. [QxMD MEDLINE Link].
- Gray A, Goodacre S, Newby DE, et al, for the 3CPO Trialists. Noninvasive ventilation in acute cardiogenic pulmonary edema. N Engl J Med. 2008 Jul 10. 359 (2):142-51. [QxMD MEDLINE Link].
- CONSENSUS Trial Study Group. Effects of enalapril on mortality in severe congestive heart failure. Results of the Cooperative North Scandinavian Enalapril Survival Study (CONSENSUS). N Engl J Med. 1987 Jun 4. 316 (23):1429-35. [QxMD MEDLINE Link].
- Yusuf S, Pitt B, Davis CE, Hood WB, Cohn JN, for the SOLVD Investigators. Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N Engl J Med. 1991 Aug 1. 325 (5):293-302. [QxMD MEDLINE Link].
- Zannad F, Alla F, Dousset B, Perez A, Pitt B. Limitation of excessive extracellular matrix turnover may contribute to survival benefit of spironolactone therapy in patients with congestive heart failure: insights from the randomized aldactone evaluation study (RALES). Rales Investigators. Circulation. 2000 Nov 28. 102 (22):2700-6. [QxMD MEDLINE Link].
- Sodhi N, Lasala JM. Mechanical circulatory support in acute decompensated heart failure and shock. Interv Cardiol Clin. 2017 Jul. 6 (3):387-405. [QxMD MEDLINE Link].
- Velazquez EJ, Lee KL, Jones RH, et al, for the STICHES Investigators. Coronary-artery bypass surgery in patients with ischemic cardiomyopathy. N Engl J Med. 2016 Apr 21. 374(16):1511-20. [QxMD MEDLINE Link].
- Busko M. Clevidipine shows promise for acute HF with high BP. Medscape Medical News from WebMD. February 10, 2014. Available at https://www.medscape.com/viewarticle/820377. Accessed: February 18, 2014.
- Felker GM, Lee KL, Bull DA, et al, for the NHLBI Heart Failure Clinical Research Network. Diuretic strategies in patients with acute decompensated heart failure. N Engl J Med. 2011 Mar 3. 364 (9):797-805. [QxMD MEDLINE Link].
- Liu PP. Cardiorenal syndrome in heart failure: a cardiologist's perspective. Can J Cardiol. 2008 Jul. 24 suppl B:25B-9B. [QxMD MEDLINE Link]. [Full Text].
- Kramer BK, Schweda F, Riegger GA. Diuretic treatment and diuretic resistance in heart failure. Am J Med. 1999 Jan. 106 (1):90-6. [QxMD MEDLINE Link].
- Neuberg GW, Miller AB, O'Connor CM, et al, for the PRAISE Investigators. Prospective Randomized Amlodipine Survival Evaluation. Diuretic resistance predicts mortality in patients with advanced heart failure. Am Heart J. 2002 Jul. 144 (1):31-8. [QxMD MEDLINE Link].
- Costanzo MR, Saltzberg M, O'Sullivan J, Sobotka P. Early ultrafiltration in patients with decompensated heart failure and diuretic resistance. J Am Coll Cardiol. 2005 Dec 6. 46 (11):2047-51. [QxMD MEDLINE Link].
- Young JB, Abraham WT, Stevenson LW, et al. Results of the VMAC Trial: vasodilation in the management of acute congestive heart failure. Circ. 2000 Nov 28. 102(22):a2794. [Full Text].
- Publication Committee for the VMAC Investigators (Vasodilatation in the Management of Acute CHF). Intravenous nesiritide vs nitroglycerin for treatment of decompensated congestive heart failure: a randomized controlled trial. JAMA. 2002 Mar 27. 287 (12):1531-40. [QxMD MEDLINE Link].
- Costanzo MR, Jessup M. Treatment of congestion in heart failure with diuretics and extracorporeal therapies: effects on symptoms, renal function, and prognosis. Heart Fail Rev. 2012 Mar. 17 (2):313-24. [QxMD MEDLINE Link].
- Costanzo MR, Guglin ME, Saltzberg MT, et al, for the UNLOAD Trial Investigators. Ultrafiltration versus intravenous diuretics for patients hospitalized for acute decompensated heart failure. J Am Coll Cardiol. 2007 Feb 13. 49 (6):675-83. [QxMD MEDLINE Link].
- CIBIS Investigators and Committees. A randomized trial of beta-blockade in heart failure. The Cardiac Insufficiency Bisoprolol Study (CIBIS). CIBIS Investigators and Committees. Circulation. 1994 Oct. 90 (4):1765-73. [QxMD MEDLINE Link].
- Chaudhry SI, Mattera JA, Curtis JP, et al. Telemonitoring in patients with heart failure. N Engl J Med. 2010 Dec 9. 363 (24):2301-9. [QxMD MEDLINE Link].
- Koehler F, Winkler S, Schieber M, et al, Telemedical Interventional Monitoring in Heart Failure Investigators. Impact of remote telemedical management on mortality and hospitalizations in ambulatory patients with chronic heart failure: the telemedical interventional monitoring in heart failure study. Circulation. 2011 May 3. 123 (17):1873-80. [QxMD MEDLINE Link].
- P&T Community. FDA approves first implantable wireless device with remote monitoring to measure pulmonary artery pressure in certain heart failure patients (news release). Available at https://www.ptcommunity.com/news/20170422/fda-approves-first-implantable-device-remote-monitoring-measure-pa-pressure-heart. May 28, 2014; Accessed: June 2, 2014.
- O'Riordan M. FDA approves first implantable device for remotely monitoring HF patients. Heartwire. Available at https://www.medscape.com/viewarticle/825805. May 28, 2014; Accessed: June 2, 2014.
- Abraham WT, Adamson PB, Bourge RC, et al, for the CHAMPION Trial Study Group. Wireless pulmonary artery haemodynamic monitoring in chronic heart failure: a randomised controlled trial. Lancet. 2011 Feb 19. 377 (9766):658-66. [QxMD MEDLINE Link].
- Eisen HJ, Kobashigawa J, Keogh A, et al, for the Mycophenolate Mofetil Cardiac Study Investigators. Three-year results of a randomized, double-blind, controlled trial of mycophenolate mofetil versus azathioprine in cardiac transplant recipients. J Heart Lung Transplant. 2005 May. 24 (5):517-25. [QxMD MEDLINE Link].
- Yancy CW, Lopatin M, Stevenson LW, De Marco T, Fonarow GC, for the ADHERE Scientific Advisory Committee and Investigators. Clinical presentation, management, and in-hospital outcomes of patients admitted with acute decompensated heart failure with preserved systolic function: a report from the Acute Decompensated Heart Failure National Registry (ADHERE) Database. J Am Coll Cardiol. 2006 Jan 3. 47 (1):76-84. [QxMD MEDLINE Link].
- Cardiac Rhythm News. FDA approves expanded indication for certain pacemakers and defibrillators used to treat heart failure. Available at https://cardiacrhythmnews.com/fda-approves-expanded-indication-for-certain-pacemakers-and-defibrillators-used-to-treat-heart-failure/. April 15, 2014; Accessed: April 15, 2014.
- Stiles S. FDA approves Medtronic CRT sevices for mild HF with AV block. Medscape Medical News. Available at https://www.medscape.com/viewarticle/823485. April 10, 2014; Accessed: April 15, 2014.
- Levy WC, Lee KL, Hellkamp AS, et al. Maximizing survival benefit with primary prevention implantable cardioverter-defibrillator therapy in a heart failure population. Circulation. 2009 Sep 8. 120 (10):835-42. [QxMD MEDLINE Link].
- Santangelo G, Bursi F, Negroni MS, et al. Arrhythmic event prediction in patients with heart failure and reduced ejection fraction. J Cardiovasc Med (Hagerstown). 2021 Feb 1. 22 (2):110-7. [QxMD MEDLINE Link].
- Ojo A, Tariq S, Harikrishnan P, Iwai S, Jacobson JT. Cardiac resynchronization therapy for heart failure. Interv Cardiol Clin. 2017 Jul. 6 (3):417-26. [QxMD MEDLINE Link].
- Rosanio S, Schwarz ER, Ahmad M, et al. Benefits, unresolved questions, and technical issues of cardiac resynchronization therapy for heart failure. Am J Cardiol. 2005 Sep 1. 96 (5):710-7. [QxMD MEDLINE Link].
- Tang AS, Wells GA, Talajic M, et al, for the Resynchronization-Defibrillation for Ambulatory Heart Failure Trial Investigators. Cardiac-resynchronization therapy for mild-to-moderate heart failure. N Engl J Med. 2010 Dec 16. 363 (25):2385-95. [QxMD MEDLINE Link].
- Giraldi F, Cattadori G, Roberto M, et al. Long-term effectiveness of cardiac resynchronization therapy in heart failure patients with unfavorable cardiac veins anatomy comparison of surgical versus hemodynamic procedure. J Am Coll Cardiol. 2011 Jul 26. 58 (5):483-90. [QxMD MEDLINE Link].
- Abraham WT, Fisher WG, Smith AL, et al, for the MIRACLE Study Group. Multicenter InSync Randomized Clinical Evaluation. Cardiac resynchronization in chronic heart failure. N Engl J Med. 2002 Jun 13. 346 (24):1845-53. [QxMD MEDLINE Link].
- Moss AJ, Hall WJ, Cannom DS, et al, for the MADIT-CRT Trial Investigators. Cardiac-resynchronization therapy for the prevention of heart-failure events. N Engl J Med. 2009 Oct 1. 361 (14):1329-38. [QxMD MEDLINE Link].
- Arshad A, Moss AJ, Foster E, et al, for the MADIT-CRT Executive Committee. Cardiac resynchronization therapy is more effective in women than in men: the MADIT-CRT (Multicenter Automatic Defibrillator Implantation Trial with Cardiac Resynchronization Therapy) trial. J Am Coll Cardiol. 2011 Feb 15. 57 (7):813-20. [QxMD MEDLINE Link].
- Ruwald MH, Ruwald AC, Jons C, et al. Effect of metoprolol versus carvedilol on outcomes in MADIT-CRT (multicenter automatic defibrillator implantation trial with cardiac resynchronization therapy). J Am Coll Cardiol. 2013 Apr 9. 61 (14):1518-26. [QxMD MEDLINE Link].
- Cleland JG, Daubert JC, Erdmann E, et al, for the Cardiac Resynchronization-Heart Failure (CARE-HF) Study Investigators. The effect of cardiac resynchronization on morbidity and mortality in heart failure. N Engl J Med. 2005 Apr 14. 352 (15):1539-49. [QxMD MEDLINE Link].
- Bristow MR, Saxon LA, Boehmer J, et al, for the Comparison of Medical Therapy, Pacing, et al. Cardiac-resynchronization therapy with or without an implantable defibrillator in advanced chronic heart failure. N Engl J Med. 2004 May 20. 350 (21):2140-50. [QxMD MEDLINE Link].
- Curtis AB, Worley SJ, Adamson PB, et al, for the Biventricular versus Right Ventricular Pacing in Heart Failure Patients with Atrioventricular Block (BLOCK HF) Trial Investigators. Biventricular pacing for atrioventricular block and systolic dysfunction. N Engl J Med. 2013 Apr 25. 368 (17):1585-93. [QxMD MEDLINE Link].
- Veterans Administration Coronary Artery Bypass Surgery Cooperative Study Group. Eleven-year survival in the Veterans Administration randomized trial of coronary bypass surgery for stable angina. N Engl J Med. 1984 Nov 22. 311 (21):1333-9. [QxMD MEDLINE Link].
- VA Coronary Artery Bypass Surgery Cooperative Study Group. Eighteen-year follow-up in the Veterans Affairs Cooperative Study of Coronary Artery Bypass Surgery for stable angina. Circulation. 1992 Jul. 86 (1):121-30. [QxMD MEDLINE Link].
- Caracciolo EA, Davis KB, Sopko G, et al. Comparison of surgical and medical group survival in patients with left main equivalent coronary artery disease. Long-term CASS experience. Circulation. 1995 May 1. 91 (9):2335-44. [QxMD MEDLINE Link].
- Robinson TN, Morrell TD, Pomerantz BJ, Heimbach JK, Cairns CB, Harken AH. Therapeutically accessible clinical cardiac states. J Am Coll Surg. 2000 Oct. 191 (4):452-63. [QxMD MEDLINE Link].
- Senior R, Lahiri A, Kaul S. Effect of revascularization on left ventricular remodeling in patients with heart failure from severe chronic ischemic left ventricular dysfunction. Am J Cardiol. 2001 Sep 15. 88 (6):624-9. [QxMD MEDLINE Link].
- Velazquez EJ, Lee KL, Deja MA, et al, for the STICH Investigators. Coronary-artery bypass surgery in patients with left ventricular dysfunction. N Engl J Med. 2011 Apr 28. 364 (17):1607-16. [QxMD MEDLINE Link]. [Full Text].
- Elefteriades JA, Morales DL, Gradel C, Tollis G Jr, Levi E, Zaret BL. Results of coronary artery bypass grafting by a single surgeon in patients with left ventricular ejection fractions < or = 30%. Am J Cardiol. 1997 Jun 15. 79 (12):1573-8. [QxMD MEDLINE Link].
- Kron IL, Flanagan TL, Blackbourne LH, Schroeder RA, Nolan SP. Coronary revascularization rather than cardiac transplantation for chronic ischemic cardiomyopathy. Ann Surg. 1989 Sep. 210 (3):348-52; discussion 352-4. [QxMD MEDLINE Link]. [Full Text].
- Doenst T, Velazquez EJ, Beyersdorf F, et al, for the STICH investigators. To STICH or not to STICH: we know the answer, but do we understand the question?. J Thorac Cardiovasc Surg. 2005 Feb. 129 (2):246-9. [QxMD MEDLINE Link].
- Joyce D, Loebe M, Noon GP, et al. Revascularization and ventricular restoration in patients with ischemic heart failure: the STICH trial. Curr Opin Cardiol. 2003 Nov. 18 (6):454-7. [QxMD MEDLINE Link].
- Sharoni E, Song HK, Peterson RJ, Guyton RA, Puskas JD. Off pump coronary artery bypass surgery for significant left ventricular dysfunction: safety, feasibility, and trends in methodology over time--an early experience. Heart. 2006 Apr. 92 (4):499-502. [QxMD MEDLINE Link]. [Full Text].
- Calafiore AM, Di Giammarco G, Teodori G, et al. Late results of first myocardial revascularization in multiple vessel disease: single versus bilateral internal mammary artery with or without saphenous vein grafts. Eur J Cardiothorac Surg. 2004 Sep. 26 (3):542-8. [QxMD MEDLINE Link].
- Nishimura RA, Grantham JA, Connolly HM, Schaff HV, Higano ST, Holmes DR Jr. Low-output, low-gradient aortic stenosis in patients with depressed left ventricular systolic function: the clinical utility of the dobutamine challenge in the catheterization laboratory. Circulation. 2002 Aug 13. 106 (7):809-13. [QxMD MEDLINE Link].
- Carabello BA. Clinical practice. Aortic stenosis. N Engl J Med. 2002 Feb 28. 346 (9):677-82. [QxMD MEDLINE Link].
- Lindblom D, Lindblom U, Qvist J, Lundstrom H. Long-term relative survival rates after heart valve replacement. J Am Coll Cardiol. 1990 Mar 1. 15(3):566-73. [QxMD MEDLINE Link].
- Connolly HM, Oh JK, Schaff HV, et al. Severe aortic stenosis with low transvalvular gradient and severe left ventricular dysfunction:result of aortic valve replacement in 52 patients. Circulation. 2000 Apr 25. 101 (16):1940-6. [QxMD MEDLINE Link].
- deFilippi CR, Willett DL, Brickner ME, et al. Usefulness of dobutamine echocardiography in distinguishing severe from nonsevere valvular aortic stenosis in patients with depressed left ventricular function and low transvalvular gradients. Am J Cardiol. 1995 Jan 15. 75 (2):191-4. [QxMD MEDLINE Link].
- Vaquette B, Corbineau H, Laurent M, et al. Valve replacement in patients with critical aortic stenosis and depressed left ventricular function: predictors of operative risk, left ventricular function recovery, and long term outcome. Heart. 2005 Oct. 91 (10):1324-9. [QxMD MEDLINE Link]. [Full Text].
- Dujardin KS, Enriquez-Sarano M, Schaff HV, Bailey KR, Seward JB, Tajik AJ. Mortality and morbidity of aortic regurgitation in clinical practice. A long-term follow-up study. Circulation. 1999 Apr 13. 99 (14):1851-7. [QxMD MEDLINE Link].
- Chaliki HP, Mohty D, Avierinos JF, et al. Outcomes after aortic valve replacement in patients with severe aortic regurgitation and markedly reduced left ventricular function. Circulation. 2002 Nov 19. 106 (21):2687-93. [QxMD MEDLINE Link].
- Enriquez-Sarano M, Tajik AJ. Clinical practice. Aortic regurgitation. N Engl J Med. 2004 Oct 7. 351 (15):1539-46. [QxMD MEDLINE Link].
- Lancellotti P, Gerard PL, Pierard LA. Long-term outcome of patients with heart failure and dynamic functional mitral regurgitation. Eur Heart J. 2005 Aug. 26 (15):1528-32. [QxMD MEDLINE Link].
- Patel JB, Borgeson DD, Barnes ME, Rihal CS, Daly RC, Redfield MM. Mitral regurgitation in patients with advanced systolic heart failure. J Card Fail. 2004 Aug. 10 (4):285-91. [QxMD MEDLINE Link].
- Bolling SF, Pagani FD, Deeb GM, Bach DS. Intermediate-term outcome of mitral reconstruction in cardiomyopathy. J Thorac Cardiovasc Surg. 1998 Feb. 115 (2):381-6; discussion 387-8. [QxMD MEDLINE Link].
- Akasaka T, Yoshida K, Hozumi T, et al. Restricted coronary flow reserve in patients with mitral regurgitation improves after mitral reconstructive surgery. J Am Coll Cardiol. 1998 Dec. 32 (7):1923-30. [QxMD MEDLINE Link].
- Wu AH, Aaronson KD, Bolling SF, Pagani FD, Welch K, Koelling TM. Impact of mitral valve annuloplasty on mortality risk in patients with mitral regurgitation and left ventricular systolic dysfunction. J Am Coll Cardiol. 2005 Feb 1. 45 (3):381-7. [QxMD MEDLINE Link].
- McGee EC, Gillinov AM, Blackstone EH, et al. Recurrent mitral regurgitation after annuloplasty for functional ischemic mitral regurgitation. J Thorac Cardiovasc Surg. 2004 Dec. 128 (6):916-24. [QxMD MEDLINE Link].
- Srichai MB, Grimm RA, Stillman AE, et al. Ischemic mitral regurgitation: impact of the left ventricle and mitral valve in patients with left ventricular systolic dysfunction. Ann Thorac Surg. 2005 Jul. 80 (1):170-8. [QxMD MEDLINE Link].
- Morishita A, Shimakura T, Nonoyama M, Takasaki T. Mitral valve replacement in ischemic mitral regurgitation. Preservation of both anterior and posterior mitral leaflets. J Cardiovasc Surg (Torino). 2002 Apr. 43 (2):147-52. [QxMD MEDLINE Link].
- Yun KL, Sintek CF, Miller DC, et al. Randomized trial comparing partial versus complete chordal-sparing mitral valve replacement: effects on left ventricular volume and function. J Thorac Cardiovasc Surg. 2002 Apr. 123 (4):707-14. [QxMD MEDLINE Link].
- Gillinov AM, Wierup PN, Blackstone EH, et al. Is repair preferable to replacement for ischemic mitral regurgitation?. J Thorac Cardiovasc Surg. 2001 Dec. 122 (6):1125-41. [QxMD MEDLINE Link].
- Miller DC. Ischemic mitral regurgitation redux--to repair or to replace?. J Thorac Cardiovasc Surg. 2001 Dec. 122 (6):1059-62. [QxMD MEDLINE Link].
- Orban M, Hausleiter J. Edge-to-edge mitral valve repair: solid data and a prosperous future. Heart. 2018 Feb. 104(4):280-1. [QxMD MEDLINE Link].
- Vahanian A, Urena M, Ince H, Nickenig G. Mitral valve: repair/clips/cinching/chordae. EuroIntervention. 2017 Sep 24. 13 (AA):AA22-30. [QxMD MEDLINE Link].
- Feldman T, Kar S, Rinaldi M, et al, for the EVEREST Investigators. Percutaneous mitral repair with the MitraClip system: safety and midterm durability in the initial EVEREST (Endovascular Valve Edge-to-Edge REpair Study) cohort. J Am Coll Cardiol. 2009 Aug 18. 54 (8):686-94. [QxMD MEDLINE Link].
- Chiarito M, Pagnesi M, Martino EA, et al. Outcome after percutaneous edge-to-edge mitral repair for functional and degenerative mitral regurgitation: a systematic review and meta-analysis. Heart. 2018 Feb. 104(4):306-12. [QxMD MEDLINE Link].
- Geis NA, Puls M, Lubos E, et al. Safety and efficacy of MitraClip therapy in patients with severely impaired left ventricular ejection fraction: results from the German transcatheter mitral valve interventions (TRAMI) registry. Eur J Heart Fail. 2018 Mar. 20(3):598-608. [QxMD MEDLINE Link].
- Buckberg GD. Ventricular restoration--a surgical approach to reverse ventricular remodeling. Heart Fail Rev. 2004 Oct. 9 (4):233-9; discussion 347-51. [QxMD MEDLINE Link].
- Yamaguchi A, Ino T, Adachi H, et al. Left ventricular volume predicts postoperative course in patients with ischemic cardiomyopathy. Ann Thorac Surg. 1998 Feb. 65 (2):434-8. [QxMD MEDLINE Link].
- Mickleborough LL, Carson S, Ivanov J. Repair of dyskinetic or akinetic left ventricular aneurysm: results obtained with a modified linear closure. J Thorac Cardiovasc Surg. 2001 Apr. 121 (4):675-82. [QxMD MEDLINE Link].
- Ott DA, Parravacini R, Cooley DA, et al. Improved cardiac function following left ventricular aneurysm resection: pre- and postoperative performance studies in 150 patients. Tex Heart Inst J. 1982 Sep. 9 (3):267-73. [QxMD MEDLINE Link]. [Full Text].
- Athanasuleas CL, Buckberg GD, Stanley AW, et al, for the RESTORE group. Surgical ventricular restoration in the treatment of congestive heart failure due to post-infarction ventricular dilation. J Am Coll Cardiol. 2004 Oct 6. 44 (7):1439-45. [QxMD MEDLINE Link].
- Jones RH, Velazquez EJ, Michler RE, et al, for the STICH Hypothesis 2 Investigators. Coronary bypass surgery with or without surgical ventricular reconstruction. N Engl J Med. 2009 Apr 23. 360 (17):1705-17. [QxMD MEDLINE Link]. [Full Text].
- Imamura T, Chung B, Nguyen A, Sayer G, Uriel N. Clinical implications of hemodynamic assessment during left ventricular assist device therapy. J Cardiol. 2018 Apr. 71 (4):352-8. [QxMD MEDLINE Link].
- Timms D. A review of clinical ventricular assist devices. Med Eng Phys. 2011 Nov. 33 (9):1041-7. [QxMD MEDLINE Link].
- Pamboukian SV, Tallaj JA, Brown RN, et al. Improvement in 2-year survival for ventricular assist device patients after implementation of an intensive surveillance protocol. J Heart Lung Transplant. 2011 Aug. 30 (8):879-87. [QxMD MEDLINE Link].
- Lietz K, Long JW, Kfoury AG, et al. Outcomes of left ventricular assist device implantation as destination therapy in the post-REMATCH era: implications for patient selection. Circulation. 2007 Jul 31. 116 (5):497-505. [QxMD MEDLINE Link].
- Daneshmand MA, Rajagopal K, Lima B, et al. Left ventricular assist device destination therapy versus extended criteria cardiac transplant. Ann Thorac Surg. 2010 Apr. 89 (4):1205-9; discussion 1210. [QxMD MEDLINE Link].
- US Food and Drug Administration. Recently-approved devices: HeartWare HVAD - P100047/S090. Available at https://www.fda.gov/MedicalDevices/ProductsandMedicalProcedures/DeviceApprovalsandClearances/Recently-ApprovedDevices/ucm581473.htm. September 27, 2017 [Updated October 31, 2017]; Accessed: October 31, 2017.
- US National Library of Medicine. Evaluation of the Jarvik 2000 Left Ventricular Assist System with post-auricular connector--destination therapy study. ClinicalTrials.gov. Available at https://clinicaltrials.gov/ct2/show/NCT01627821. Updated: October 16, 2017; Accessed: October 31, 2017.
- Rose EA, Gelijns AC, Moskowitz AJ, et al, for theRandomized Evaluation of Mechanical Assistance for the Treatment of Congestive Heart Failure (REMATCH) Study Group. Long-term use of a left ventricular assist device for end-stage heart failure. N Engl J Med. 2001 Nov 15. 345 (20):1435-43. [QxMD MEDLINE Link].
- Park SJ, Tector A, Piccioni W, et al. Left ventricular assist devices as destination therapy: a new look at survival. J Thorac Cardiovasc Surg. 2005 Jan. 129 (1):9-17. [QxMD MEDLINE Link].
- Starling RC, Naka Y, Boyle AJ, et al. Results of the post-U.S. Food and Drug Administration-approval study with a continuous flow left ventricular assist device as a bridge to heart transplantation: a prospective study using the INTERMACS (Interagency Registry for Mechanically Assisted Circulatory Support). J Am Coll Cardiol. 2011 May 10. 57 (19):1890-8. [QxMD MEDLINE Link].
- Ventura PA, Alharethi R, Budge D, et al. Differential impact on post-transplant outcomes between pulsatile- and continuous-flow left ventricular assist devices. Clin Transplant. 2011 Jul-Aug. 25 (4):E390-5. [QxMD MEDLINE Link].
- Slaughter MS, Pagani FD, Rogers JG, et al, for the HeartMate II Clinical Investigators. Clinical management of continuous-flow left ventricular assist devices in advanced heart failure. J Heart Lung Transplant. 2010 Apr. 29 (4 suppl):S1-39. [QxMD MEDLINE Link].
- Kirklin JK, Naftel DC, Kormos RL, et al. Third INTERMACS Annual Report: the evolution of destination therapy in the United States. J Heart Lung Transplant. 2011 Feb. 30 (2):115-23. [QxMD MEDLINE Link].
- Taylor DO, Edwards LB, Boucek MM, et al. Registry of the International Society for Heart and Lung Transplantation: twenty-second official adult heart transplant report--2005. J Heart Lung Transplant. 2005 Aug. 24 (8):945-55. [QxMD MEDLINE Link].
- Boucek MM, Edwards LB, Keck BM, Trulock EP, Taylor DO, Hertz MI. Registry of the International Society for Heart and Lung Transplantation: eighth official pediatric report--2005. J Heart Lung Transplant. 2005 Aug. 24(8):968-82. [QxMD MEDLINE Link].
- United Network for Organ Sharing (US). National data. UNOS. Available at https://unos.org/data/. October 24, 2017; Accessed: November 1, 2017.
- Stevenson LW, Kormos RL, Bourge RC, et al. Mechanical cardiac support 2000: current applications and future trial design. June 15-16, 2000 Bethesda, Maryland. J Am Coll Cardiol. 2001 Jan. 37 (1):340-70. [QxMD MEDLINE Link].
- Gray NA Jr, Selzman CH. Current status of the total artificial heart. Am Heart J. 2006 Jul. 152 (1):4-10. [QxMD MEDLINE Link].
- Cooley DA, Liotta D, Hallman GL, Bloodwell RD, Leachman RD, Milam JD. Orthotopic cardiac prosthesis for two-staged cardiac replacement. Am J Cardiol. 1969 Nov. 24 (5):723-30. [QxMD MEDLINE Link].
- Platis A, Larson DF. CardioWest temporary total artificial heart. Perfusion. 2009 Sep. 24 (5):341-6. [QxMD MEDLINE Link].
- Roussel JC, Senage T, Baron O, et al. CardioWest (Jarvik) total artificial heart: a single-center experience with 42 patients. Ann Thorac Surg. 2009 Jan. 87 (1):124-9; discussion 130. [QxMD MEDLINE Link].
- Anderson E, Jaroszewski D, Pierce C, DeValeria P, Arabia F. Parallel application of extracorporeal membrane oxygenation and the CardioWest total artificial heart as a bridge to transplant. Ann Thorac Surg. 2009 Nov. 88 (5):1676-8. [QxMD MEDLINE Link].
- Morris RJ. Total artificial heart--concepts and clinical use. Semin Thorac Cardiovasc Surg. 2008 Fall. 20 (3):247-54. [QxMD MEDLINE Link].
- Meyer A, Slaughter M. The total artificial heart. Panminerva Med. 2011 Sep. 53 (3):141-54. [QxMD MEDLINE Link].
- US National Library of Medicine. European clinical evaluation of the Carmat total artificial heart (advance HF). ClinicalTrials.gov. Available at https://clinicaltrials.gov/ct2/show/NCT02962973. Updated: November 25, 2016; Accessed: November 1, 2017.
- [Guideline] Ackerman MJ, Priori SG, Willems S, et al, Heart Rhythm Society (HRS), European Heart Rhythm Association (EHRA). HRS/EHRA expert consensus statement on the state of genetic testing for the channelopathies and cardiomyopathies: this document was developed as a partnership between the Heart Rhythm Society (HRS) and the European Heart Rhythm Association (EHRA). Europace. 2011 Aug. 13 (8):1077-109. [QxMD MEDLINE Link]. [Full Text].
- Marcus FI, McKenna WJ, Sherrill D, et al. Diagnosis of arrhythmogenic right ventricular cardiomyopathy/dysplasia: proposed modification of the Task Force Criteria. Eur Heart J. 2010 Apr. 31 (7):806-14. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] O'Meara E, McDonald M, Chan M, et al. CCS/CHFS heart failure guidelines: clinical trial update on functional mitral regurgitation, SGLT2 inhibitors, ARNI in HFpEF, and tafamidis in amyloidosis. Can J Cardiol. 2020 Feb. 36 (2):159-69. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Tracy CM, Epstein AE, Darbar D,et al. 2012 ACCF/AHA/HRS focused update of the 2008 guidelines for device-based therapy of cardiac rhythm abnormalities: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. [corrected]. Circulation. 2012 Oct 2. 126 (14):1784-800. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Priori SG, Blomstrom-Lundqvist C, Mazzanti A, et al. 2015 ESC guidelines for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: The Task Force for the Management of Patients with Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death of the European Society of Cardiology (ESC). Endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC). Eur Heart J. 2015 Nov 1. 36 (41):2793-867. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Rihal CS, Naidu SS, Givertz MM, et al, Society for Cardiovascular Angiography and Interventions (SCAI), Heart Failure Society of America (HFSA), et al. 2015 SCAI/ACC/HFSA/STS clinical expert consensus statement on the use of percutaneous mechanical circulatory support devices in cardiovascular care: endorsed by the American Heart Association, the Cardiological Society of India, & Sociedad Latino Americana de Cardiologia Intervencion; affirmation of value by the Canadian Association of Interventional Cardiology-Association Canadienne de Cardiologie d'intervention. J Am Coll Cardiol. 2015 May 19. 65 (19):e7-e26. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Feldman D, Pamboukian SV, Teuteberg JJ, et al., International Society for Heart and Lung Transplantation. The 2013 International Society for Heart and Lung Transplantation Guidelines for mechanical circulatory support: executive summary. J Heart Lung Transplant. 2013 Feb. 32 (2):157-87. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Peura JL, Colvin-Adams M, Francis GS, et al. Recommendations for the use of mechanical circulatory support: device strategies and patient selection: a scientific statement from the American Heart Association. Circulation. 2012 Nov 27. 126 (22):2648-67. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Baran DA, Billia F, Randhawa V, et al, for the Consensus Conference participants/collaborators. Consensus statements from the International Society for Heart and Lung Transplantation consensus conference: heart failure-related cardiogenic shock. J Heart Lung Transplant. 2024 Feb. 43 (2):204-16. [QxMD MEDLINE Link]. [Full Text].
- [Guideline] Mullens W, Damman K, Dhont S, et al. Dietary sodium and fluid intake in heart failure. A clinical consensus statement of the Heart Failure Association of the ESC. Eur J Heart Fail. 2024 Apr 12. [QxMD MEDLINE Link]. [Full Text].
- Masini M, Elia E, Vianello PF, et al. Frequency, predictors and prognostic impact of implantable cardioverter defibrillator shocks in a primary prevention population with heart failure and reduced ejection fraction. J Cardiovasc Med (Hagerstown). 2021 Feb 1. 22 (2):118-25. [QxMD MEDLINE Link].
- [Guideline] Lloyd-Jones D, Adams RJ, Brown TM, et al, for the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Executive summary: heart disease and stroke statistics--2010 update: a report from the American Heart Association. Circulation. 2010 Feb 23. 121 (7):948-54. [QxMD MEDLINE Link].
Author
Ioana Dumitru, MD Associate Professor of Medicine, Division of Cardiology, Founder and Medical Director, Heart Failure and Cardiac Transplant Program, University of Nebraska Medical Center; Associate Professor of Medicine, Division of Cardiology, Veterans Affairs Medical Center
Ioana Dumitru, MD is a member of the following medical societies: American College of Cardiology, Heart Failure Society of America, International Society for Heart and Lung Transplantation
Disclosure: Nothing to disclose.
Specialty Editor Board
Mary L Windle, PharmD Adjunct Associate Professor, University of Nebraska Medical Center College of Pharmacy; Editor-in-Chief, Medscape Drug Reference
Disclosure: Nothing to disclose.
Yasmine S Ali, MD, MSCI, FACC, FACP Assistant Clinical Professor of Medicine, Vanderbilt University School of Medicine; President, LastSky Writing, LLC
Yasmine S Ali, MD, MSCI, FACC, FACP is a member of the following medical societies: American College of Cardiology, American College of Physicians, American Heart Association, American Medical Association, American Medical Writers Association, National Lipid Association, Tennessee Medical Association
Disclosure: Serve(d) as a director, officer, partner, employee, advisor, consultant or trustee for: LastSky Writing;Philips Healthcare;M Health;Verywell Health; MedStudy;WellnessVerge;Prose Media; AKH, Inc.; LearnRoll, LLC; Eradigm; RxCe.com; M3 USA; M3 EU; Future US Inc.; Edanz Group; ChesterPA511
Serve(d) as a speaker or a member of a speakers bureau for: RxCe.com.
Chief Editor
Gyanendra K Sharma, MD, FACC, FASE Professor of Medicine and Radiology, Director, Adult Echocardiography Laboratory, Section of Cardiology, Medical College of Georgia at Augusta University
Gyanendra K Sharma, MD, FACC, FASE is a member of the following medical societies: American Association of Cardiologists of Indian Origin, American Association of Physicians of Indian Origin, American College of Cardiology, American Society of Echocardiography, Society for Cardiovascular Magnetic Resonance, Society of Cardiovascular Computed Tomography
Disclosure: Nothing to disclose.
Additional Contributors
Mathue M Baker, MD Cardiologist, BryanLGH Heart Institute and Saint Elizabeth Regional Medical Center
Mathue M Baker, MD is a member of the following medical societies: American College of Cardiology
Disclosure: Nothing to disclose.
Henry H Ooi, MD, MRCPI Director, Advanced Heart Failure and Cardiac Transplant Program, Nashville Veterans Affairs Medical Center; Assistant Professor of Medicine, Vanderbilt University School of Medicine
Disclosure: Nothing to disclose.
Mariclaire Cloutier Freelance editor, Medscape Drugs & Diseases
Disclosure: Nothing to disclose.
Acknowledgements
Barry E Brenner, MD, PhD, FACEP Professor of Emergency Medicine, Professor of Internal Medicine, Program Director, Emergency Medicine, Case Medical Center, University Hospitals, Case Western Reserve University School of Medicine
Barry E Brenner, MD, PhD, FACEP is a member of the following medical societies: Alpha Omega Alpha, American Academy of Emergency Medicine, American College of Chest Physicians, American College of Emergency Physicians, American College of Physicians, American Heart Association, American Thoracic Society, Arkansas Medical Society, New York Academy of Medicine, New York AcademyofSciences,and Society for Academic Emergency Medicine
Disclosure: Nothing to disclose.
David FM Brown, MD Associate Professor, Division of Emergency Medicine, Harvard Medical School; Vice Chair, Department of Emergency Medicine, Massachusetts General Hospital
David FM Brown, MD is a member of the following medical societies: American College of Emergency Physicians and Society for Academic Emergency Medicine
Disclosure: Nothing to disclose.
William K Chiang, MD Associate Professor, Department of Emergency Medicine, New York University School of Medicine; Chief of Service, Department of Emergency Medicine, Bellevue Hospital Center
William K Chiang, MD is a member of the following medical societies: American Academy of Clinical Toxicology, American College of Medical Toxicology, and Society for Academic Emergency Medicine
Disclosure: Nothing to disclose.
Joseph Cornelius Cleveland Jr, MD Associate Professor, Division of Cardiothoracic Surgery, University of Colorado Health Sciences Center
Joseph Cornelius Cleveland Jr, MD is a member of the following medical societies: Alpha Omega Alpha, American Association for the Advancement of Science, American College of Cardiology, American College of Chest Physicians, American College of Surgeons, American Geriatrics Society, American Physiological Society, American Society of Transplant Surgeons, Association for Academic Surgery, Heart Failure Society of America, International Society for Heart and Lung Transplantation, Phi Beta Kappa, Society of Critical Care Medicine, Society of Thoracic Surgeons, and Western Thoracic Surgical Association
Disclosure: Thoratec Heartmate II Pivotal Tria; Grant/research funds Principal Investigator - Colorado; Abbott Vascular E-Valve E-clip Honoraria Consulting; Baxter Healthcare Corp Consulting fee Board membership; Heartware Advance BTT Trial Grant/research funds Principal Investigator- Colorado; Heartware Endurance DT trial Grant/research funds Principal Investigator-Colorado
Shamai Grossman, MD, MS Assistant Professor, Department of Emergency Medicine, Harvard Medical School; Director, The Clinical Decision Unit and Cardiac Emergency Center, Beth Israel Deaconess Medical Center
Shamai Grossman, MD, MS is a member of the following medical societies: American College of Emergency Physicians
Disclosure: Nothing to disclose.
John D Newell Jr, MD Professor of Radiology, Head, Division of Radiology, National Jewish Health; Professor, Department of Radiology, University of Colorado School of Medicine
John D Newell Jr, MD is a member of the following medical societies: American College of Chest Physicians, American College of Radiology, American Roentgen Ray Society, American Thoracic Society, Association of University Radiologists, Radiological Society of North America, and Society of Thoracic Radiology
Disclosure: Siemens Medical Grant/research funds Consulting; Vida Corporation Ownership interest Board membership; TeraRecon Grant/research funds Consulting; Medscape Reference Honoraria Consulting; Humana Press Honoraria Other
Craig H Selzman, MD, FACS Associate Professor of Surgery, Surgical Director, Cardiac Mechanical Support and Heart Transplant, Division of Cardiothoracic Surgery, University of Utah School of Medicine
Craig H Selzman, MD, FACS is a member of the following medical societies: Alpha Omega Alpha, American Association for Thoracic Surgery, American College of Surgeons, American Physiological Society, Association for Academic Surgery, International Society for Heart and Lung Transplantation, Society of Thoracic Surgeons, Southern Thoracic Surgical Association, and Western Thoracic Surgical Association
Disclosure: Nothing to disclose.
Gary Setnik, MD Chair, Department of Emergency Medicine, Mount Auburn Hospital; Assistant Professor, Division of Emergency Medicine, Harvard Medical School
Gary Setnik, MD is a member of the following medical societies: American College of Emergency Physicians, National Association of EMS Physicians, and Society for Academic Emergency Medicine
Disclosure: SironaHealth Salary Management position; South Middlesex EMS Consortium Salary Management position; ProceduresConsult.com Royalty Other
Brett C Sheridan, MD, FACS Associate Professor of Surgery, University of North Carolina at Chapel Hill School of Medicine
Disclosure: Nothing to disclose.
George A Stouffer III, MD Henry A Foscue Distinguished Professor of Medicine and Cardiology, Director of Interventional Cardiology, Cardiac Catheterization Laboratory, Chief of Clinical Cardiology, Division of Cardiology, University of North Carolina Medical Center
George A Stouffer III, MD is a member of the following medical societies: Alpha Omega Alpha, American College of Cardiology, American College of Physicians, American Heart Association, Phi Beta Kappa, and Society for Cardiac Angiography and Interventions
Disclosure: Nothing to disclose.
Francisco Talavera, PharmD, PhD Adjunct Assistant Professor, University of Nebraska Medical Center College of Pharmacy; Editor-in-Chief, Medscape Drug Reference
Disclosure: Medscape Salary Employment