Gram-Negative Bacteria: Structure, Examples & Antibiotic Resistance (original) (raw)
These are bacteria that define the opposite of the gram-positive bacteria in relation to the differential staining technique. During gram staining, the gram-negative bacteria will lose the crystal violet dye color after a wash with alcohol and take up the pink/red color of the counterstain, safranin.
The two classes of bacteria are differentiated through gram staining, because of their cell wall composition i.e Gram-positive bacteria have a large layer of peptidoglycan and a thin layer of the lipid layer, and unlike the Gram-negative bacteria which have a thick layer of lipids and they lack the peptidoglycan layer or some have a very thin layer of the peptidoglycan layer. The absence of peptidoglycan makes their cell-wall less strong, and hence the primary stain is easily washed off by alcohol and water.
Gram-negative bacteria are found in a wide range of environments especially those that have life, ranging from normal flora such as Escherichia coli to pathogenic bacteria such as Klebsiella pneumoniae, Chlamydia trichomatis.
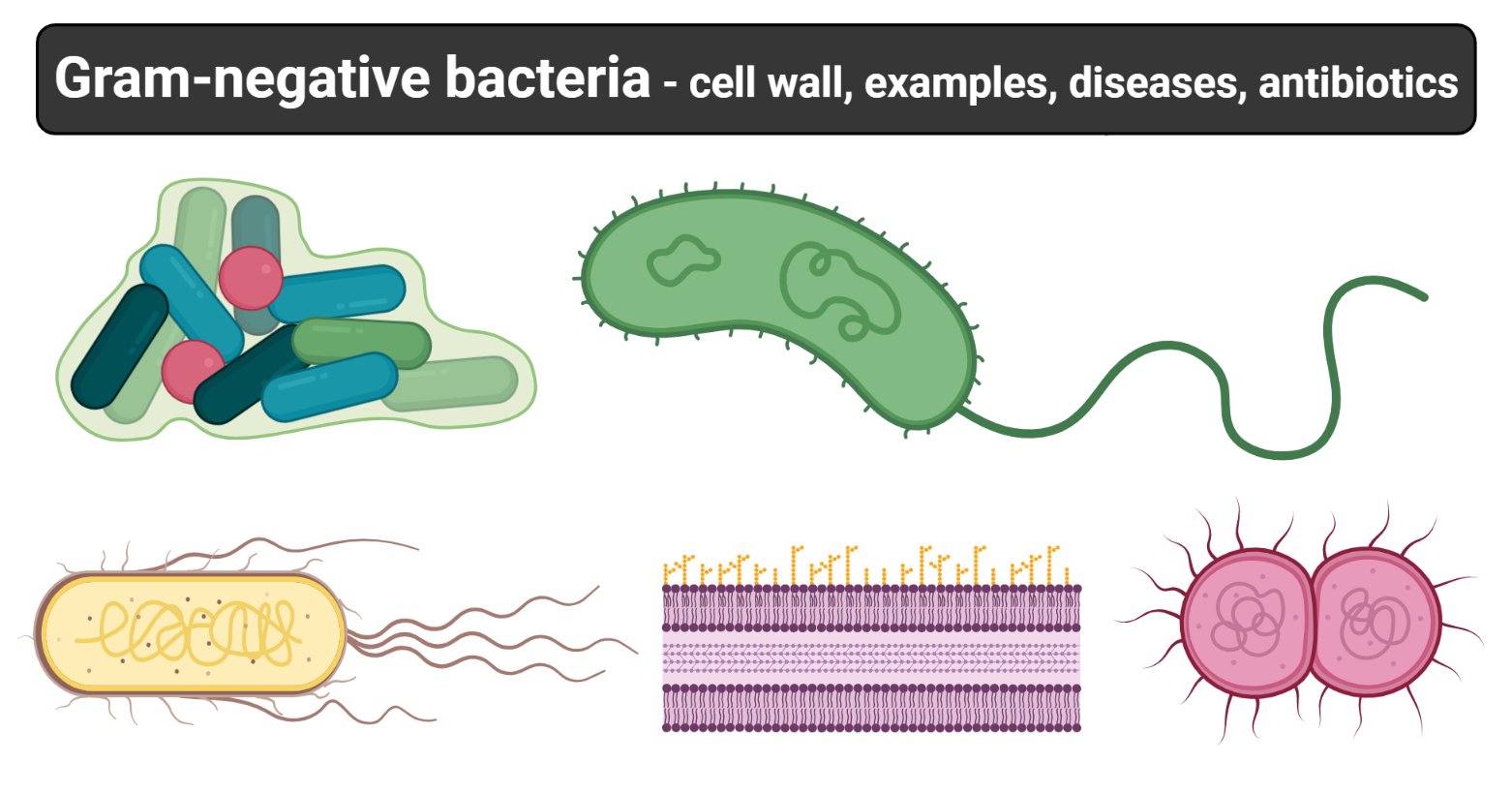
Gram-negative bacteria
- Characteristics of Gram-negative bacteria
- Characterization of Gram-negative bacteria shapes
- Gram-negative bacteria cell wall
- The Periplasmic space
- Peptidoglycan
- The Outer Membrane and the Lipopolysaccharides
- Gram-negative bacteria list and their pathologies and clinical significance
- Gram-negative bacteria antimicrobial agents
- References
- Sources
Characteristics of Gram-negative bacteria
- The gram-negative bacteria have a characteristic cell envelope that differentiates it from the Gram-positive bacteria.
- They have a periplasmic space (Periplasm) which separated the outer membrane from the cytoplasmic layer.
- The periplasmic space has a network of peptidoglycan chains known as the peptidoglycan layer.
- They have a thin peptidoglycan layer.
- They have an outer membrane that is made up of lipopolysaccharides.
Characterization of Gram-negative bacteria shapes
Microscopic observation of Gram-negative bacteria cells ranges from rods to bacillus, to cocci to spiral shapes which are the most commonly known shapes. However some exhibit special shapes such as coccobacillus, tetrads, palisades, trichomes, etc.
For example:
- Rob/bacillus shaped – Escherichia coli.
- Coccobacillus – which is a combination of both cocci and bacilli shapes include Hemophilus influenza.
- Streptobacillus are rod-shapes that are connected together in chains eg Streptobacillus moniliformis.
- Trichome shape is a series of rod-shaped cells that are arranged in a columnar form and it may be enclosed in a sheath.
- Spiral shaped bacteria also called spirochaetes e.g Chlamydia trachomatis, Treponema pallidum.
- Filamentous shaped gram-negative have a filament-like shape eg Norcadia spp.
Gram-negative bacteria cell wall
The Cell wall of the Gram-Negative Bacteria is very complex as compared to that of Gram-Positive Bacteria. Combined with the major role of the outer membrane of the cell, with a layer of peptidoglycan, its functional properties are complex, and here is a description of the cell wall and its functional parts.
- The cell wall of gram-negative bacteria is complex having a thin layer of the peptidoglycan layer of 2-7nm and a thick outer membrane of 7-8nm thick.
- Microscopically, there is a space that is seen between the cell membrane and the cell wall, known as the periplasmic space made up of periplasm. However it is found in both Gram-negative and Gram-positive bacteria, but in gram-negative the periplasmic space is larger.
The Periplasmic space
- The periplasmic space in Gram-negative bacteria is made up of several proteins that assist in acquiring nutrients such as hydrolytic enzymes that attack the nucleic acids and phosphorylated molecules, and the binding proteins which actively assist in the transportation of materials into the bacteria cell. The periplasmic space also has enzymes that synthesize peptidoglycan and modify toxic elements that may cause harm to the cell.
Peptidoglycan
- The Gram-negative bacterial cell wall has a thin peptidoglycan layer that is found above the plasma membrane making about 5-% of the cells dry weight. Some bacteria like E. coli have 2nm thick peptidoglycan (2-3 sheets of peptidoglycan).
The Outer Membrane and the Lipopolysaccharides
- The outer membrane lies above the thin peptidoglycan layer. The membrane is made up of Braun’s lipoprotein which is covalently bound to the peptidoglycan and embedded to the outer membrane by hydrophobic ends. The Braun’s lipoprotein strongly links the outer membrane and the peptidoglycan.
- The gram-negative cell wall is also strengthened by the adhesion sites on the outer membrane which play a role in allowing cell contact and membrane fusion. Substances enter the cell through these adhesion sites.
- The outer membrane is majorly made up of Lipopolysaccacharides (LPSs) which are large complex molecules made up of lipids and carbohydrates. The lipopolysaccharide is made up of 3 units: Lipid A, the core polysaccharides and the O side chain. The most researched gram-negative bacterial lipopolysaccharide is that of Salmonella Typhimurium. The lipid A unit constitutes two glucosamine sugar derivates each containing three fatty acids and pyrophosphate, Any left parts of the lipopolysaccharide project out of the surface of the membrane.
- The O side chain is also known as the O antigen is a chain that extends from the core outwardly. It is made up of sugars that cause variations between bacterial strains. These O antigens are also responsible for bacterial evading antibody responses.
- The Lipopolysaccahrides are also responsible for protecting the cell wall from external attacks.
- The LPSs have a negative charge giving the cell surface a negative charge. Thus this stabilizes the membrane structure.
- Lipid A contributes to the toxic element of the Lipopolysacchaides, hence it acts endotoxins.
- The outer membrane of the gram-negative bacteria and its lipopolysaccharide contribute greatly to preventing the entry of antibiotics, bile salts and other toxic elements from entering and disrupting the cell.
- Consequently, the outer membrane is made up of porin proteins which makes it permeable allowing the entry of small molecules such as glucose.
- Larger molecules like Vitamin B12 are transported across the outer membrane by specific carriers
- The outer membrane also contributes to the prevention of loss of components, especially from the periplasmic space.
Gram-negative bacteria list and their pathologies and clinical significance
Gram-negative bacteria are known to be normal flora apart from some which cause severe human infections which range from community-acquired infections to nosocomial (Hospital-acquired) Infections. They cause severe infections some of which cause death if not detected and treated on time. The table below gives examples of some of the Gram-negative bacteria and the clinical features they exhibit upon causing diseases and infections in the human host.
| Gram-negative bacteria | Pathologies: Clinical feature |
|---|---|
| Neisseria gonorrhoea | Genitourinary tract infections for both male (urethra) and female (vagina and endocervix), associated with purulent urethral discharge and painful urination. The infection may progress to the uterus, causing salpingitis (inflammation of the fallopian tubes), pelvic inflammatory disease (PID), and fibrosis.Infertility may occur for women with salpingitis.Renal infection for men associated with constipation, painful defecation and purulent discharge.Pharyngitis if purulent pharyngeal exudation occurs.Ophthalmia neonatorum in newborns acquired during birth through the cervix.Disseminated infection associated with fever; painful, purulent arthritis; and small, single, scattered pustules on the skin, with an erythematous (red) base due to dilation or congestion of capillaries.Necrosis may develop. |
| Neisseria meningitidis | Meningitis can rapidly spread causing meningococcemia if the bacteria invades the bloodstream, associated with a high fever. It can also spread and invade the brain barrier causing purulent meningitis with fever and severe headaches, joint aches and a petechial and/or purpuric rash.Septicemia occurs within the first 12 hours of infection which can progress to fulminant septicemia and shock especially in children known as Waterhouse-Friderichsen syndrome) |
| Escherichia coli | Intestinal diseases include; enterotoxigenic (ETEC), enteropathogenic (EPEC), enterohemorrhagic (EHEC), enteroinvasive (EIEC), and enteroaggregative (EAEC). They are all associate with diarrhea (watery or/and bloody).Extraintestinal diseases such as Urinary tract infection including cystitis and pyelonephritis, neonatal meningitis and nosocomial-acquired infections such as sepsis/bacteremia, endotoxic shock, and pneumonia. |
| Salmonella spp | Enteric and Typhoid fever characterized by fever, abdominal pain, and severe symptoms include chills, sweats, headache, anorexia, weakness, sore throat, cough, myalgia, and either diarrhea or constipation.Gastroenteritis (salmonellosis) characterized by nausea, vomiting, and non-bloody diarrhea.Bacteremia associated with abdominal infections (of the hepatobiliary tract and spleen); osteomyelitis; septic arthritis |
| Campylobacter jejuni | It causes intestinal and extraintestinal disease with systemic associated with fever, headache, myalgia, and abdominal cramping and diarrhea, which may or may not be bloody.It commonly causes traveler’s diarrhea and pseudoappendicitis with symptoms simulating appendicitis without inflammation of the appendix).Bacteremia (often transient) may occur, most often in infants and older adults. |
| Salmonella dysenterae | Shigellosis (bacillary dysentery) characterized by diarrhea with blood, mucus in stool, and painful abdominal cramping. |
| Vibrio cholerae | Cholera associated with profuse watery diarrhea massive loss of fluid and electrolytes from the body |
| Helicobacter pylori | Acute gastritis with diarrheaSuperficial gastritis associated with epigastric discomfort causing both duodenal ulcers and gastric ulcers.Persistent ulceration may lead to mucosa associated-lymphoid tumors. |
| Klebsiella pneumoniae | It causes UTI and nosocomial acquired bacteremia. |
| Pseudomonas aeruginosa | It causes opportunistic nosocomial infections of wounded patients from surgeries, invading the body through catheters and respirators.Keratitis and endophthalmitis after an injury that formed a wound, associated with necrotic otitis.Skin wound infections.Respiratory tract infections characterized by pneumonia symptoms.Gastrointestinal infections with diarrhea.Necrotic enterocolitis in infants.Systemic infections associated with septicemia, pneumonia, bone and joint infections, Infection of the central nervous system (CNS) and soft tissue infections in hospitalized patients. |
Gram-negative bacteria antimicrobial agents
Antimicrobial agents against Bacteria causative agents are known as antibiotics. These antibiotics against the mechanisms of the bacterial cell blocking or inhibiting certain mechanisms from being initiated to induce bacterial cell multiplication and replication. Examples of antibiotics used against gram-negative bacteria are listed in the table below.
| Antibiotic | Mode of action | Bacterial agent |
|---|---|---|
| Cephalosporin: ceftriaxone | Disruption of the cell by binding to the penicillin-binding proteins and enzymes responsible for the synthesis of peptidoglycan | Neisseria gonorrhea Neisseria meningitidesPseudomonas aeruginosa |
| Tetracycline: Doxycycline | Inhibit protein synthesis by preventing the elongation of polypeptides at 30s ribosomes | Neisseria gonorrheae |
| Streptogramins | Inhibition of protein synthesis by preventing polypeptide elongation of 50s ribosomes | Neisseria gonorrheae |
| Β -lactam: Penicillin G | Inhibition of cell synthesis by disrupting the penicillin-binding proteins and enzymes used for peptidoglycan synthesis | Neisseria meningitidis Pseudomonas aureginosa |
| Rifampin: Rifamycin | Inhibition of nucleic acid synthesis by preventing transcription of binding DNA-dependent RNA polymerase | Neisseria meningitides Escherichia coli |
| Macrolide: Erythromycin, Azithromycin, Clarithromycin | Inhibition of bacterial protein synthesis by preventing the elongation of polypeptides of 50s ribosomes | Neisseria gonorrhea Campylobacter jejuniShigella dysenteraeHelicobacter pyloriPseudomonas aeruginosa |
| Tetracycline: Doxycycline | Inhibition of protein synthesis by preventing the polypeptide elongation of 30s ribosomes | Neisseria gonorrheae Vibrio cholerae |
| Quinolones: Fluoroquinolones, Ciprofloxacin | Inhibition of nucleic acid synthesis by binding to the alpha-subunit of DNA gyrase | Eschericia coli Salmonella typhi/paratyphi (enteric and typhoid fever)Campylobacter jujeniShigella dysenteraePseudomonas aureginosa |
| Aminoglycosides | They inhibit protein synthesis by prematurely producing aberrant peptide chains from 30s ribosomes | Escherichia coli (localized and systemic infections**)** |
| Sulfonamides: sulfamethoxazole | They are antimetabolites that inhibit dihydropteroate synthase and distract folic acid synthesis | _Eschericia coli (_UTIs and systemic diseases) |
| Trimethoprim | They are antimetabolites that inhibit the action of dihydrofolate reductase and disrupts the folic acid synthesis | Escherichia coli(UTIs) |
References
- Jawertz M., Aldenberg., Medical Microbiology: 28th Edition
- Lippincott in Illustrations Reviews Microbiology 3rd Edition
- Prescott M. L., Microbiology 5th Edition
Sources
- 1% – https://www.thoughtco.com/gram-positive-gram-negative-bacteria-4174239
- 1% – https://www.sciencedirect.com/topics/medicine-and-dentistry/salpingitis
- 1% – https://www.ncbi.nlm.nih.gov/pubmed/21208910
- 1% – https://www.answers.com/Q/Why\_gram\_staining\_is\_classified\_as\_differential\_staining
- 1% – https://www.answers.com/Q/Is\_the\_cell\_wall\_of\_gram\_positive\_bacteria
- 1% – https://en.wikipedia.org/wiki/Outer\_mitochondrial\_membrane
- <1% – https://www.youtube.com/watch?v=Didrc3wJ3E8
- <1% – https://www.who.int/water\_sanitation\_health/dwq/GDW11rev1and2.pdf
- <1% – https://www.std.uw.edu/go/pathogen-based/gonorrhea/core-concept/all
- <1% – https://www.slideshare.net/UmeshMaskare/bacteria-bacteria-structure
- <1% – https://www.slideshare.net/drimhotep/bacterial-pneumonia-pharmacology
- <1% – https://www.slideshare.net/bypohemalatha/cholera-and-diarrhoea
- <1% – https://www.sigmaaldrich.com/technical-documents/articles/biology/glycobiology/lipopolysaccharides.html
- <1% – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4635515/
- <1% – https://www.coursehero.com/file/14185100/sc1040-week-5-test-3/
- <1% – https://www.caister.com/highveld/microbiology/gram-negative-bacteria.html
- <1% – https://quizlet.com/215139360/biology-chapter-131-flash-cards/
- <1% – https://quizlet.com/167242502/neisseria-gonnorrhoeae-chlamydia-trachomatis-treponema-pallidum-flash-cards/
- <1% – https://quizlet.com/125172448/the-cell-wall-flash-cards/
- <1% – https://pediaa.com/difference-between-gram-positive-and-gram-negative-bacteria/
- <1% – https://medium.com/the-biochemists/why-are-gram-negative-bacteria-resistant-to-antibiotics-c732fe9afd06
- <1% – https://malariajournal.biomedcentral.com/articles/10.1186/1475-2875-11-275
- <1% – https://en.wikipedia.org/wiki/Protein\_synthesis\_inhibitor
- <1% – https://en.wikipedia.org/wiki/Periplasmic\_space
- <1% – https://en.wikipedia.org/wiki/Braun%27s\_lipoprotein
- <1% – https://en.m.wikipedia.org/wiki/Cefotaxime
- <1% – https://brainly.com/question/4536708
- <1% – https://answers.yahoo.com/question/index?qid=20120117191858AAeid8h
- <1% – https://academic.oup.com/femsre/article/26/1/17/631737
- <1% – http://www.uobabylon.edu.iq/eprints/pubdoc\_12\_2921\_235.doc
- <1% – http://www.scielo.br/scielo.php?script=sci\_arttext&pid=S1984-82502014000100003
- <1% – http://www.microbiologybook.org/mayer/antibiot.htm
- <1% – http://textbookofbacteriology.net/medical\_4.html
About Author
Dr. Faith Mokobi is a passionate scientist and completed her Ph.D. in Nanoengineering (Synthetic Biology specialization) from Joint School of Nanoscience and Nanoengineering, North Carolina A and T State University, North Carolina, USA in 2025. She has a background in Immunology and Microbiology (MSc./BSc.). With extensive higher education teaching and research experience in Biomedical studies, metagenomic studies, and drug resistance, Faith is currently integrating her Biomedical experience in nanotechnology and cancer theranostics.