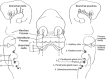Branchial cleft anomalies: a pictorial review of embryological development and spectrum of imaging findings - PubMed (original) (raw)
Branchial cleft anomalies: a pictorial review of embryological development and spectrum of imaging findings
Ashok Adams et al. Insights Imaging. 2016 Feb.
Abstract
The branchial arches are the embryological precursors of the face, neck and pharynx. Anomalies of the branchial arches are the second most common congenital lesions of the head and neck in children, with second branchial arch anomalies by far the most common. Clinically, these congenital anomalies may present as cysts, sinus tracts, fistulae or cartilaginous remnants with typical clinical and radiological findings. We review the normal embryological development of the branchial arches and the anatomical structures of the head and neck that derive from each arch. The typical clinical and radiological appearances of both common and uncommon branchial arch abnormalities are discussed with an emphasis on branchial cleft anomalies.
Key points: • Anomalies of the branchial arches usually present as cysts, sinuses or fistulae. • Second branchial arch anomalies account for approximately 95 % of cases. • There are no pathognomonic imaging features so diagnosis depends on a high index of suspicion and knowledge of typical locations. • Persistent cysts, fistulae or recurrent localised infection may be due to branchial arch anomalies. • Surgical excision of the cyst or tract is the most common curative option.
Keywords: Branchial arch; Branchial cleft; Branchial cleft cyst; Pharyngeal apparatus; Pharyngeal pouch.
Figures
Fig. 1
Frontal schematic representation of a 5-mm human embryo at the fifth week of gestation. Sagittal sections taken through the branchial apparatus demonstrate the anatomic relationship of external clefts and internal pouches as well as the derivation of important head and neck structures. The sixth arch is very small and not visualised as a separate, discrete structure from pouch 4/5 in Fig. 1. [Reproduced with permission from Waldhausen J (2006) Branchial cleft and arch anomalies in children. Seminars in Pediatric Surgery 15:64–69]
Fig. 2
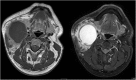
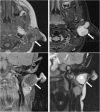
Two-year-old child with axial fat-suppressed T1 post-contrast and sagittal short tau inversion recovery (STIR) images demonstrating a rounded and well-defined T1 isointense, T2 hyperintense lesion with thin peripheral enhancement (thick white arrows). It is located posterior to the right submandibular gland (thin white arrow) and anterior to the sternocleidomastoid muscle and carotid sheath (asterisk). This was confirmed to represent a second branchial cleft cyst following surgical excision
Fig. 3
T1 post-contrast and STIR images demonstrate a T2 hyperintense cystic mass with irregular peripheral enhancement after contrast administration. The abnormality was confirmed to be an infected second branchial cleft cyst in a 54-year-old man who had a history of recurrent infections at the mandibular angle
Fig. 4
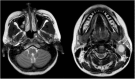
Forty-year-old man presenting with a persistent level II neck lump. Axial T2-weighted imaging demonstrates a complex cystic lesion posterior to the left angle of the mandible (white arrow). Asymmetrical soft tissue was also appreciated in the left fossa of Rosenmüller (asterisk). A second branchial cleft cyst was considered in the differential, but the diagnosis was finally confirmed to be nasopharyngeal carcinoma with cystic metastases
Fig. 5
MR imaging from a child presenting with purulent ear discharge. Axial and coronal T1 post-contrast (left hand images) with axial and coronal STIR images (right hand images) demonstrating a thick-walled sinus tract (white arrows) that extended to the clinically apparent opening in the left external auditory canal. The tract was surgically excised and confirmed to represent a first branchial cleft anomaly
Fig. 6
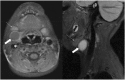
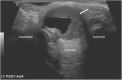
Transverse ultrasound (US) image from the same child as in Fig. 5, confirming the presence of a thick-walled cystic structure that was part of the sinus tract that extended to the left external auditory canal (white arrow)
Fig. 7
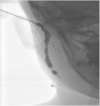
A sinogram performed on a child prior to surgical excision for a presumed first branchial cleft fistula. The opening within the right external auditory canal was cannulated and water-soluble contrast media injected confirmed the presence of a fistulous tract. During the procedure, contrast media was noted to pass via the tract through an external cutaneous opening in the right submandibular region
Fig. 8
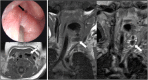
This 18-day-old baby presented with intermittent stridor. On examination, a left-sided oropharyngeal swelling was identified. The baby had initially required continuous positive airway pressure. Microlaryngobronchoscopy identified an internal opening arising from the pyriform sinus apex (black arrow; image courtesy of Mr Y. Bajaj). Axial and coronal T1 with coronal STIR imaging identified a likely air-containing structure (thick white arrows) extending from the pyriform sinus to the level of the left thyroid gland that was abnormally small (thin white arrow). This was surgically confirmed to represent a fourth branchial cleft sinus tract
References
- Schoenwolf G, Bleyl S, Brauer P, Francis-West P (2009) Larsen’s Human Embryology, 4th edn. Churchill Livingston, New York, Edinburgh
- Carlson BM. Human embryology and developmental biology. 4. St. Louis: Mosby; 2009.
- Tewfik T, Yoskovitch A. Congenital malformations of the neck. eMedicine, Medscape. http://emedicine.medscape.com/article/837477-overview. Accessed 14 March 2015
LinkOut - more resources
Full Text Sources
Other Literature Sources