Management of epistaxis in patients with ventricular assist device: a retrospective review - PubMed (original) (raw)
Management of epistaxis in patients with ventricular assist device: a retrospective review
Clifford Scott Brown et al. J Otolaryngol Head Neck Surg. 2018.
Abstract
Background: Patients with a ventricular assist device (VAD) are at risk for epistaxis due to the need for anticoagulation. Additionally, these patients develop acquired von Willebrand syndrome (AvWS) due to these devices. Management is complicated by the risk of thrombosis if anticoagulation is reversed. This study sought to characterize the clinical features and management of epistaxis in this high-risk population.
Methods: Retrospective review of adults with VAD and epistaxis necessitating inpatient consultation with the otolaryngology service were included.
Results: 49 patients met inclusion criteria. All patients had a presumed diagnosis of AvWS. An elevated INR (> 2.0) was present in 18 patients (36.7%). Anticoagulation was held in 14 (28.6%) patients, though active correction was not necessary. Multiple encounters were required in 16 (32.7%) patients. Spontaneous epistaxis was associated with multiple encounters (p = 0.02). The use of hemostatic material was associated with a lower likelihood of bleeding recurrence (p = 0.05), whereas cauterization with silver nitrate alone was associated with a higher likelihood of re-intervention (p = 0.05). Surgery or embolization was not required urgently for any patient. Endoscopy under general anesthesia was performed for one patient electively. Mean follow up time was 16.6 months (σ = 6.3). At six months, 18 (36.7%) patients were deceased.
Conclusion: While these patients are at risk for recurrent spontaneous epistaxis, nonsurgical treatment without active correction of INR or AvWS was largely successful. Placement of hemostatic material, as opposed to cautery with silver nitrate, should be considered as a first-line treatment in this group. Multidisciplinary collaboration is critical for successful management.
Keywords: Anticoagulation; Epistaxis; Ventricular assist device; von Willebrand syndrome.
Conflict of interest statement
This study was approved by the Institutional Review Board at Duke University (Pro00071269).
not applicable.
The authors declare that they have no competing interests.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Figures
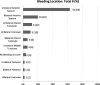
Fig. 1
Bleeding Location: Distribution of bleeding locations by number and percentage. Note that sites are not mutually exclusive
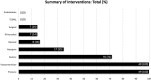
Fig. 2
Summary of Interventions: Distribution of interventions performed by number and percentage. Note that interventions are not mutually exclusive
Similar articles
- Acquired Von Willebrand syndrome is an early-onset problem in ventricular assist device patients.
Heilmann C, Geisen U, Beyersdorf F, Nakamura L, Trummer G, Berchtold-Herz M, Schlensak C, Zieger B. Heilmann C, et al. Eur J Cardiothorac Surg. 2011 Dec;40(6):1328-33; discussion 1233. doi: 10.1016/j.ejcts.2011.03.021. Epub 2011 Apr 22. Eur J Cardiothorac Surg. 2011. PMID: 21515067 - Platelet Secretion Defects and Acquired von Willebrand Syndrome in Patients With Ventricular Assist Devices.
Geisen U, Brehm K, Trummer G, Berchtold-Herz M, Heilmann C, Beyersdorf F, Schelling J, Schlagenhauf A, Zieger B. Geisen U, et al. J Am Heart Assoc. 2018 Jan 13;7(2):e006519. doi: 10.1161/JAHA.117.006519. J Am Heart Assoc. 2018. PMID: 29331958 Free PMC article. - Acquired von Willebrand syndrome in a child following Berlin Heart EXCOR Pediatric Ventricular Assist Device implantation: case report and concise literature review.
Costello JP, Diab YA, Philippe-Auguste M, Jones MB, Shankar V, Friedman KD, Nath DS. Costello JP, et al. World J Pediatr Congenit Heart Surg. 2014 Oct;5(4):592-8. doi: 10.1177/2150135114539521. World J Pediatr Congenit Heart Surg. 2014. PMID: 25324261 Review. - Acquired von Willebrand syndrome in patients with ventricular assist device or total artificial heart.
Heilmann C, Geisen U, Beyersdorf F, Nakamura L, Benk C, Berchtold-Herz M, Trummer G, Schlensak C, Zieger B. Heilmann C, et al. Thromb Haemost. 2010 May;103(5):962-7. doi: 10.1160/TH09-07-0497. Epub 2010 Mar 29. Thromb Haemost. 2010. PMID: 20352153 - Acquired Von Willebrand Syndrome and Blood Pump Design.
Rosenberg G, Siedlecki CA, Jhun CS, Weiss WJ, Manning K, Deutsch S, Pierce W. Rosenberg G, et al. Artif Organs. 2018 Dec;42(12):1119-1124. doi: 10.1111/aor.13291. Epub 2018 Oct 28. Artif Organs. 2018. PMID: 30370640 Review.
Cited by
- Epistaxis Rates and Health Care Utilization in Patients With a Ventricular Assist Device.
Rohe E, Schmoker S, Samson K, Carlson K, Dowdall J. Rohe E, et al. OTO Open. 2024 Apr 12;8(2):e132. doi: 10.1002/oto2.132. eCollection 2024 Apr-Jun. OTO Open. 2024. PMID: 38618289 Free PMC article.
References
- Shrestha I, Pokharel M, Dhakal A, et al. Study of microorganism growth Patten in nasal pack of patients visiting the department of ENT, head and neck surgery. Kathmandu Univ Med J (KUMJ) 2015;13(52):303–307. - PubMed
- Spielmann PM, Barnes ML, White PS. Controversies in the specialist management of adult epistaxis: an evidence-based review. Clin Otolaryngol. 2012 Oct;37(5):382–9. Doi: 10.111/coa.12024. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous